Low-Shrink Composites
James F. Simon, DDS, MEd; Waldemar G. de Rijk, BA, MS, PhD, DDS, FADM
Resin-based restorative materials shrink when they are cured. The stresses induced by this polymerization shrinkage of dental composites has been well documented.1 Clinicians have devised many ways to circumvent the hazards caused by shrinkage-induced stresses, ranging from incremental placement of the composites to modulating the curing light intensity. Many manufacturers have now started to address this problem by the introduction of new composite formulations that are being advertised as low-shrink composites.
Background
The polymerization shrinkage of composite materials has been implicated as a primary source of interfacial breakdown, resulting in visible white lines or invisible cracks in the enamel and resin at the margins.2 It also has been blamed for the tooth-composite interfacial debonding, cuspal deflection, enamel cracking, and the formation of white lines.3 The bond failure at the interface allows an influx of oral fluids and greatly contributes to the possibility of marginal staining, secondary caries, postoperative sensitivity, and fractures through the enamel along the interface.4
This adverse side effect of the material as the monomer conversion into a polymer results in a closer, tighter arrangement of the molecules leading to a reduction in material volume.5 This volumetric change may vary from as little as 1.5% to as much as 6% for the most common commercial materials, depending on their specific formulation.6 The extent of this shrinkage depends on the volume fraction of the nonshrinking filler and the size of the monomers; that is, the concentration of functional methacrylates per monomer and the extent of the polymerization reaction.3
Clinicians have had to deal with this contraction stress issue since composite materials were first used. Because research has shown that the shrinkage is in the direction of the constrained surfaces7 (composite will shrink away from an unbonded surface toward a bonded surface) during polymerization, placement in incremental layers (horizontal, vertical, or oblique) in small, 2-mm increments has been suggested as one way to overcome this stress on the restoration walls. Therefore, consideration of the C-factor (the ratio of bonded surfaces to unbonded surfaces) should always be an important consideration when placing a composite.
Another suggestion has been the use of a flexible liner, either glass-ionomer, resin-modified glass-ionomer, or a flowable composite. Still another suggestion has been to modify the way the light is applied during the curing process. These methods have included “ramp curing” (increasing the light power from low to high over a period of 10 seconds), “step curing” (a low power used for the first 10 seconds, then full power for the remainder of the curing time), “pulse delay” (a short initial burst of low power followed by a waiting period of several minutes before applying a high power level), or curing through the tooth for the first application of the light.
The shrinkage of present composites varies greatly depending on the chemistry of the composite (the type of monomer, the type and amount of filler material, filler and matrix interactions) and the previously mentioned placement factors. Because it is a direct function of the volume fraction of the polymer matrix in the composite, microfill composites usually show a higher setting contraction (2% to 4%) compared to a fine-particle hybrid.4 It should be noted that shrinkage is only one component in causing stress in composites. The elastic modulus plays an equally important role. Thus, a composite with a lower volumetric shrinkage will not necessarily produce lower stresses in the final restoration.
The approach of manufacturers has been to reduce the residual stress by developing composites that shrink less. Composite shrinkage has been reported from 1.5% to 5.5% by volume.8 The latest attempts have been to produce a composite that will consistently shrink less than 2% by volume. It seems that by tacit agreement, a composite is considered low-shrink if the shrinkage is at or below 2%.
Polymerization Shrinkage
Polymerization shrinkage is an inherent consequence of the chemical process; the volume of two ethene molecules is less than the volume of one butane molecule. This phenomenon is readily seen in the methylmethacrylate (MMA) resins, the monomer used in denture acrylics, which, if polymerized without the powder, will shrink by 26%.9
Manufacturers and researchers of dental composites have for a long time made attempts to reduce polymerization shrinkage. Realistically, there are only two options in reducing the shrinkage of the composites:
- reduce the concentration of the double-bonded carbons; with fewer polymerization steps occurring, the shrink-age will be less.
- change to a different resin matrix using monomers that do not shrink during polymerization.
New monomers have been investigated for some time,10 and recently a patent has been issued for such monomers.11 However, a discussion of these resins is beyond the scope of this article. An additional problem in developing low-shrink composites is that there exist different methods for measuring shrinkage, most not suited to low-volume specimens.
Shrinkage Reduction by Double-Bond Concentration Reduction
The first step taken by manufacturers early in the development of composites was to introduce the dimethacrylates as oligomers, which are large monomer molecules such as BisGMA, UDMA, and TegDMA. Pure TegDMA resin shrinks by 16% (vol) while MMA resin shrinks by 26% (vol).9 The oligomer combinations found in today’s composites (without the fillers) will shrink 10% to 12% by volume, a significant reduction achieved by oligomer application.2 By filling composites with nonshrinking fillers, the shrinkage was further reduced to 4% to 5% by volume.2 The filler fraction by volume for most hybrid composites approaches 70%.2 Each manufacturer has its own proprietary blend of particle sizes that balances the highest filler content while maintaining an acceptable viscosity for the final product.
With the availability of nano-sized silica particles and submicron glass fillers, the filler content of new composites is further increased, with the consequence of further reducing shrinkage. These composites are now marketed as low-shrink composites.
Methods to Determine the Volumetric Shrinkage
There exist different methods of measuring the shrinkage of materials. One method is by determining the density change of the material by Archimedes’s method, using buoyancy and weight in different liquids.12 The pyknometer is based on this method.12 One system that actually measures the volume change is the mercury dilatometer, which records the changes in volume by observing height changes in a capillary column.13 A newer system that measures volume changes is based on optical measurements and pattern recognition. The Acuvol™ (Bisco, Inc, Schaumburg, IL) is a machine that in real time collects and averages images of the specimen, does edge detection on the image, and then calculates the volume of the specimen. The change in volume is reported as a percentage shrinkage.14,15 The system is a noncontact system, as opposed to the mercury dilatometer, avoiding the hazard of air inclusions and is easily calibrated by using standard ceramic spheres of different diameters.
The Shrinkage of 10 Currently Available Composites
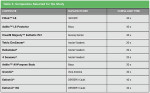
For this study, a total of 10 composites that had been sent by the manufacturers for evaluation for use in the dental school were used; three of which are marketed as low-shrink composites. The composites are listed in Table 1. Because of the ease of use of the Acuvol, it was possible to test this many composite specimens in a relatively short period of time.
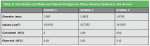
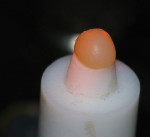
The Acuvol was calibrated using three ceramic spheres by placing the largest sphere first, and replacing it with spheres of decreasing diameter. The calculated volume changes from the spheres and the observed shrinkages are given in Table 2. The Acuvol is seen in Figure 1; a specimen placed on the pedestal is shown in Figure 2, and a computer screen shot of the observed shrinkage is seen in Figure 3. The protocol for the shrinkage measurements was:
• roll the composite into a ball of about 3-mm diameter
• place the specimen on the instrument pedestal
• if the composite slumps, wait 15 seconds then record the volume of the composite
• start the time sequence of volume measurements
• activate the curing light for the time recommended by the manufacturer (Table 1)
• continue to observe the shrinkage for 2.5 minutes after the curing light is turned on
• record the total shrinkage observed
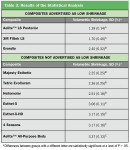
A specimen of each composite was was observed for 5 minutes to make sure that there was no further change from the 2.5-minute observation. For each composite, 10 specimens were measured. Statistical analysis used Tukey-Kramer HSD analysis for differences among the composites. The results are given in Table 3 and shown in Figure 4. The noise in the shrinkage data originates from errors in the continuous edge detection. For these composites, this produced an uncertainty (or detection limit) of 0.02%.
The 10 composites tested in this study fell into three distinct categories; two of the composites were below 2% shrinkage, four composites fell into the 2% to 3% range, and four composites were above 3% shrinkage. The standard deviation did vary for the different products. Optical measurement of the specimen contours appears to be a viable method for determining the volumetric shrinkage. This may lead to a more consistent method of measuring composite shrinkage.
Conclusion
Composite shrinkage will continue to be a concern of dentists as they place these restorations. The manufacturers are attempting to address this issue with the development of new low-shrink composites. Some seem to be making some progress in addressing this composite material shortcoming; however, as they make these changes, they change the handling characteristics of these new composites. Presently, they are only recommended for posterior restorations.
Disclosure
The Acuvol was made available to the University of Tennessee Memphis by Bisco Inc. All products measured in this study were made available by the respective manufacturers. Their support is hereby acknowledged and appreciated.
References
1. Pfeifer CS, Ferracane JL, Sakaguchi RL, Braga RR. Factors affecting photopolymerization stress in dental composites. J Dent Res. 2008;87(11): 1043-1047.
2. Ferrracane JL. Placing dental composites—a stressful experience. Oper Dent. 2008; 33-34,247-257.
3. van Noort R. Introduction to Dental Materials. London: Mosby; 2002.
4. O’Brien WJ. Dental Materials and Their Selection. Chicago, IL: Quintessence Publishing Co, Inc; 2002.
5. Santos MJM, Santos GC, Filho HN, et al. Effect of light curing method on volumetric polymerization shrinkage of resin composites. Oper Dent. 2004;29-32, 157-161.
6. Kleverlaan CJ, Feilzer AJ. Polymerization shrinkage and contraction stress of dental resin composites. Dent Mater. 2005;21(12): 1150-1157.
7. Versluis A, Tantbirojn D, Douglas WH. Do dental composites always shrink toward the light? J Dent Res. 1998;77(6):1435-1445.
8. Ferracane JL. Developing a more complete understanding of stresses produced in dental composites during polymerization, Dent Mater. 2005;21: 36-42.
9. Powers and Sakaguchi. CRAIG’S Restorative Dental Materials. 12th ed. Elsevier Mosby; St. Louis, MO; 2006.
10. Thompson VP, Williams EF, Bailey WJ. Dental resins with reduced shrinkage during hardening. J Dent Res. 1979;58(5): 1522-1532.
11. US Patent 7232852. Chappelow CC, Pinzino CS, Eick JD, Holder AJ, Chen SS, Jeang L. Photopolymerizable compositions that include alicyclic/aromatic dioxiranes and novel dioxiranyl tetraoxaspiro {5.5} undercanes. June 2007.
12. Sargent Welch Co. Selective experiments in physics. Accessed November 26, 2008.
13. Eichmiller F. Mercury dilatometer. Accessed November 26, 2008.
14. Sharp LJ, Choi IB, Lee TE, et al. Volumetric shrinkage of composites using video imaging. J Dent. 2003;31(2): 97-103.
15. Tiba A, Charlton D, Vandewalle K, Ragain J Jr. Comparison of two video-imaging instruments for measuring volumetric shrinkage of dental resin components. J Dent. 2005; 33(9):757-763.
About the Authors
James F. Simon, DDS, MEd
Professor, Department of Restorative Dentistry
Director, Division of Esthetic Dentistry
Director, Division of Clinical Research
University of Tennessee College of Dentistry
Memphis, TN
Waldemar G. de Rijk, BA, MS, PhD, DDS, FADM
Associate Professor, Department of Restorative Dentistry
Director, Division of Biomaterials
University of Tennessee College of Dentistry
Memphis, TN