Porcelain Laminate Veneer Preparations: The Additive Contour Technique
Gregg A. Helvey, DDS
Preparation techniques for porcelain laminate veneer restorations have multiplied and evolved since the treatment modality was first introduced in the mid-1980s.1,2 Methods of tooth preparation have ranged from very aggressive reduction to no preparation at all. This author has been providing this type of restorative care since its inception and has used various preparation techniques. After all these years, the one technique that has provided the most predictability is the additive contour technique. This article will describe the technique and the rationale behind it.
The term biomimetics was introduced to the dental community in 1999 by Magne et al and refers to restoring a tooth to its original performance as an intact tooth.3,4 A sufficient and uniform thickness of facial enamel is essential to the balance of functional stresses in the anterior dentition.3 Substantial loss of facial enamel is more likely to affect crown rigidity than the interdental reduction of enamel or large class III cavities.5(p48) Peumans et al found in their 10-year clinical trial on porcelain veneers that the failure rate up to 5 years was 4% but increased to 34% between 5 and 10 years. A number of factors were thought to contribute to the increas-ed failure rate, including large amounts of exposed dentin (especially in the cervical area), palatal coverage, and a ceramic-to-luting thickness ratio of less than 3:1.6 Preservation of enamel is vital to the long-term success of porcelain laminate veneer restorations. Studies have shown long-term success of porcelain laminate veneers when they are bonded primarily to enamel.7,8
From a laboratory standpoint, the proper thickness of the porcelain veneer is critical during fabrication and handling during intraoral placement. If the restoration is less than the porcelain manufacturer’s recommended thickness, it becomes more difficult to avoid breakage.
There are two methods of porcelain-laminate veneer fabrication. One method involves constructing the veneers in wax on a multiple-die working model, investing them, burning out the wax in an oven (similar to casting a gold crown) and, finally, pressing melted ceramic into the mold under a vacuum. The other method involves layering feldspathic porcelain that has been placed either on a refractory material representing the master working model or a platinum foil molded over the individual dies. The recommended thickness for porcelain veneers is between 0.3 mm to 0.5 mm in the cervical, 0.7 mm in the midbody, and > 1.5 mm at the incisal edge.5(p242-247),9-11
The Esthetic Mock-Up
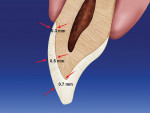
Facial enamel varies in thickness on the gingival, midbody, and incisal areas of the tooth. Measurements can vary from 0.3 mm to 0.5 mm in the gingival third, 0.6 mm to 1 mm in the midbody region, and 1 mm to 2.1 mm in the incisal third12 (Figure 1). Measurements of tooth enamel using electron microscopy showed that the thickness of natural enamel decreases with age. Therefore, it is critical that tooth reduction be as precise as possible and limited to removing only what is absolutely necessary.13 Porcelain veneer therapy should aim at restoring the original tooth volume, rather than the existing tooth volume.14 If tooth preparations are initiated from the enamel present, then the likelihood of sufficient remaining enamel necessary for long-term adhesion is greatly diminished. The bonding of ceramics to natural tooth substrate is reported to be the strongest in the enamel layer.13,15-17
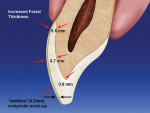
The additive contour technique creates a mock-up of the desired esthetic goal on a preoperative model.18 The esthetic mock-up is obtained by restoring the original enamel volume with composite (whereby the facial thickness of the teeth in question is increased on average of 0.1 mm to 0.3 mm) (Figure 2). The esthetic mock-up is then transferred to the patient by using a vacuum stent and a suitable composite resin of the desired shade. Then, it is fully bonded to the selected teeth. The patient wears the esthetic mockup for a period of time, generally 1 to 2 weeks. During this phase, the patient should be able to deprogram from their existing situation.14 The occlusion, phonetics, and shade are tested. This step serves as an inexpensive trial run. Any changes can easily be made by adding or subtracting composite resin. For example, if the new incisal edge position has been lengthened and impedes on the lower lip during “F” or “V” sounds, it can be easily shortened without affecting the final restoration. After the patient is satisfied with the preview restorations, an accurate impression is made that will accompany all of the materials being sent to the laboratory. (This is necessary only if significant changes were made during the trial period).
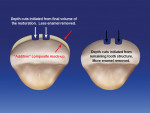
The bonded mock-up represents the final volume of the permanent restorations. Tooth preparations are initiated from the restored facial surface (not the existing enamel surface), which serves as a point of reference (Figure 3). Correct depth cuts are placed using round burs of known dimensions. Reference guides (incisal and labial preparation indexes) made from a polyvinyl silicone material are fabricated from the mock-up model. These indexes will be used to check for the proper amount of reduction.
Preparation
The key to the precise reduction of the facial surface is to know the amount of required reduction for the specific type of porcelain laminate veneer fabrication that will be used. Using rotary instruments that will cut at a known depth allows the clinician to adhere to the reduction requirements. There are a number of commercially available laminate veneer depth-cutter diamond rotary instruments but they have limitations in accessing interproximal contours and lack ease in cutting along a radius or cutting different depths at various locations of the facial profile of the tooth.
A round diamond bur easily negotiates the curved pattern of a gingival margin, gains access to the interproximal embrasure and, if the shank of the cutting instrument rests directly on the facial aspect of the tooth, creates a depthlimiting precise reduction. As the bur travels across the facial surface, it follows the existing contour and provides a uniform depth reduction.
For example, a 016 round diamond bur has a head diameter of 1.6 mm. The diameter of the shaft where it connects to the cutting head measures 0.9 mm. Subtract 0.9 mm from 1.6 mm, then cut that number (0.7 mm) in half to account for the head-cutting portion above and below the shaft. This equals a cutting depth of 0.35 mm. Therefore, by keeping the shaft of a 016 round diamond bur in contact with the tooth surface, no matter where it is, a depth cut of 0.35 mm is assured. Table 1 shows the depth cut for a number of different round diamond burs.
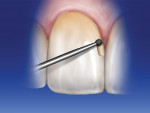
Before preparing the tooth, the clinician must choose which type of porcelain laminate veneer fabrication will be used. This information will provide the reduction measurements needed. The preparation begins with cutting the gingival margin. Using a 016 round diamond bur with its shaft resting against the facial surface and starting at the tip of the gingival papilla, the gingival margin is cut following the gingival contour (Figure 4). This gingival depth cut is repeated on all the teeth that will be prepared. The decision as to where to position the margin in relation to the gingiva (supragingival, equigingival, or subgingival) is based on the amount of shade change that will occur in the restorations. The greater the shade change, the more the margin needs to be hidden. The handpiece should move in a counterclockwise direction. The air flow from the spinning bur pushes the gingival tissue away from the cutting head. If the shaft has been positioned correctly against the composite facial surface, a black scoring line will remain on the surface.
Next, the same round diamond bur is placed at the point where the gingival depth cut was initiated. The bur, with the shaft against the facial surface and perpendicular to the long axis of the tooth, is moved in an incisal direction along the interproximal border. This is repeated for all the teeth to be prepared (Figure 5).
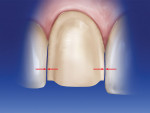
Next, a 021 round diamond bur (depth cut of approximately 0.55 mm) is placed at the junction between the cervical and midbody thirds. The depth cut is placed in a horizontal direction connecting the two interproximal depth cuts on either side of the tooth. This is repeated for all of the teeth. Then, changing the diamond bur to a 023 (depth cut of approximately 0.65 mm) a depth cut is placed at the junction of the midbody and incisal thirds. This depth cut is placed in a horizontal direction connecting the two interproximal depth cuts on either side of the tooth and repeated for all the teeth to be prepared (Figure 6). A pencil line is marked in all of the horizontal depth cuts.
The labial profile of the anterior tooth has three planes. There is an emergence profile in the gingival area, a flatter profile in the midbody area, and an incisal profile that tapers toward the lingual. At this point, there will be three islands of unprepared enamel surrounded by depth cuts. A 018 tapered diamond bur is used to remove each island of enamel, leveling the surface with the surrounding depth cuts. The angle of the bur should be parallel with the plane of the tooth to maintain the natural contour of the tooth (Figure 7). All pencil lines in the horizontal depth cuts should no longer be present. This process ensures a uniform reduction.
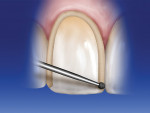
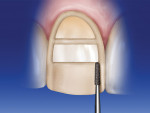
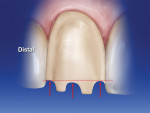
A 018 bur is used to make depth cuts at the incisal edge. This bur is tapered, measuring 1.4 mm at the tip and 1.8 mm at the shank. The depth of the cut depends on what portion of the bur is used. If, for example, a minimum of 1.8 mm of incisal reduction is preferred, then the widest portion of the bur (shank) should be used. The bur is submerged completely in relation to the incisal edge. Three evenly spaced depth cuts are made: one in the middle of the incisal edge, one at the mesial-incisal corner, and one at the distal-incisal corner. The contour of the incisal edge is followed to allow sufficient thickness of ceramic in the final restoration. Because the incisal edge rises in the distal area, this depth cut is positioned toward the gingiva. The mesial corner cut is made slightly lower than that level, and the center depth cut is positioned the lowest toward the incisal edge (Figure 8). If the reduction is on a single plane and less reduction occurs toward the mesial and distal-incisal corners, there will be insufficient room for the appropriate ceramic thickness. After the three depth cuts are placed, the same bur is used to remove the tooth structure between the depth cuts (Figure 9).
To ensure the proper amount of reduction, the incisal index is positioned onto the teeth. A measuring device, such as a FlexTab™ (Kerr Corp, Orange, CA) or a periodontal probe, is used to measure the amount of reduction. The FlexTabs come in thicknesses of 1 mm, 1.5 mm, and 2 mm. Depending on the desired amount of incisal reduction, the appropriate FlexTab can be used to measure the amount of reduction with the incisal index in place.
After the proper amount of incisal reduction is confirmed, the labial index is positioned in the mouth. Observing from an incisal view, the amount of labial reduction can be evaluated in the incisal area. Any areas of insufficient reduction are marked with a pencil. Using a surgical blade in a horizontal direction, a portion of the labial index is removed. This allows the labial index in the midbody portion of the prepared tooth to be viewed. Again, any areas of insufficient reduction are marked. This step is then repeated to check the gingival areas of the teeth.
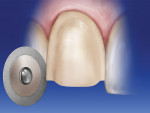
There are two schools of thought on whether to break the contact in porcelain laminate veneer preparations. This author prefers to break the contact between the teeth using a double-sided diamond disk (911H, Brasseler USA, Savannah, GA) (Figure 10). Breaking the contact with a diamond disk enhances the proximal margin definition. It also allows the technician to easily fabricate a multiple-die working model. If the contact is not broken, the technician will have to use a surgical blade to separate the dies. This step can alter the margins in the proximal areas (Figure 11).
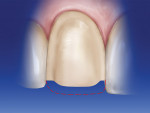
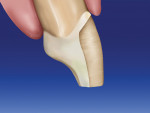
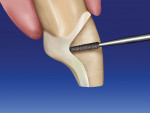
After the contacts are separated (Figure 12), the proximal margin is placed toward the lingual because the ceramic restoration will reestablish the proximal contacts. The area of the proximal margin between the contact area and the gingival papilla is placed even further to the lingual. This preparation design helps to hide the margin when the restorations are viewed from an angle, especially when there is a significant shade change. This design is often referred to as the “gull-wing” or “dog-leg” effect. A 018 tapered diamond bur or a 014 round diamond bur is used to extend the margin lingually (Figure 13). The clinician should view the margin from a 45° angle to be sure that it is hidden (Figure 14).
The last step is to eliminate all sharp angles. These angles can be very easily overlooked. An alginate impression can be made and poured using a quick-setting gypsum (Snap-Stone, Whip Mix Corp, Louisville, KY). After 5 minutes, the model can be separated and examined. Problems with the preparations can be more readily seen on this three-dimensional model than directly in the mouth. This step may take a few minutes, but eliminates the call from the technician complaining of problems with the preparations.
Inevitably, some dentin may be exposed during the preparations of teeth that may have been out of the arch form. Any areas of exposed dentin must be sealed before making an impression. This procedure is referred to as immediate dentin sealing, prehybridization, dual-bonding, or resincoating. Studies show improved bond strength when the exposed dentin is sealed using a three-step, etch-and-rinse, filled dentin bonding agent before making the impression.19-23 Sealing the exposed dentin also eliminates postoperative sensitivity by decreasing bacterial leakage24,25 and causing fewer gap formations.4,22
Conclusion
Ceramic restorations have a greater chance of long-term success when they are bonded primarily to enamel. Therefore, preservation of the enamel is paramount when preparing teeth for porcelain laminate veneers. The traditional approach begins the preparations on the existing enamel surface without consideration of previous enamel wear. This approach has led to excessive enamel reduction and dentin exposure. The additive contour technique considers the enamel wear and also provides a slight increase in the labial profile of the teeth. This change is tested before beginning the preparations, which allows the clinician and the patient to preview the final outcome and make any alterations that fulfill phonetic, esthetic, and functional parameters. The laboratory technician needs only to replicate the contours of the provisional restorations for a predictable result.
Acknowledgment
The author wishes to extend special thanks to Ruth Egli for her editorial contribution.
References
1. Clamia J R. Etched porcelain facial veneers: a new treatment modality based on scientific and clinical evidence. NY J Dent. 1983; 53(6):255-259.
2. Horn HR. A new lamination, porcelain bonded to enamel. NY State Dent J. 1983;49(6): 401-403.
3. Magne P, Versluis A, Douglas WH. Rationalization of incisor shape: experimental-numerical analysis. J Prosth Dent. 1999; 81(3):345-355.
4. Magne P, Douglas WH. Porcelain veneers: dentin bonding optimization and biomimetic recovery of the crown. Int J Prosthodont. 1999;12(2):111-121.
5. Magne P, Belser U. Bonded porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Chicago, IL: Quintessence Publishing Co Inc; 2002.
6. Peumans M, Munck JD, Fieuws S, et al. A prospective ten-year clinical trial of porcelain veneers. J Adhes Dent. 2004;6(1):65-76.
7. Fradeani M, Redemagni M, Corrado M. Porcelain laminate veneers: 6 to 12-year clinical evaluation—a retrospective study. Int J Periodontics Restorative Dent. 2005;25(1): 9-17.
8. Friedman MJ. A 15-year review of porcelain veneer failure: a clinician’s observation. Compend Contin Educ Dent. 1998;19(6): 625-636.
9. Highton R, Caputo AA, Mátyás J. A photoelastic study of stresses on porcelain laminate preparations. J Prosthet Dent. 1987; 58(2):157-161.
10. Christensen GJ, Christensen RP. Clinical observations of porcelain veneers: a three-year report. J Esthet Dent. 1991;3(5): 174-179.
11. Magne P, Kwon KR, Belser U, et al. Crack propensity of porcelain laminate veneers: a simulated operatory evaluation. J Prosthet Dent. 1999;81(3):327-334.
12. Ferrari M, Patroni S, Balleri P. Measurement of enamel thickness in relation to reduction for etched laminate veneers. Int J Periodontics Restorative Dent. 1992;2(5): 407-413.
13. Atsu SS, Aka PS, Kuculesmen HC, et al. Age-related changes in tooth enamel as measured by electron microscopy: implications for porcelain laminated veneers. J Prosthet Dent. 2005;94(4):336-341.
14. Magne P, Magne M. Use of additive waxup and direct intraoral mock-up for enamel preservation with porcelain laminate veneers. Euro J Esthet Dent. 2006;1(1): 10-19.
15. Christensen GJ. Has tooth structure been replaced? J Am Dent Assoc. 2002;133(1): 103-105.
16. Kedici PS, Kalipcilar B, Bilir OG. Effect of glass ionomer liners on bonding strength of laminate veneers. J Prosthet Dent. 1992;68(1): 29-32.
17. Peumans M, Van Meerbeek B, Lambrechts P, et al. Porcelain veneers: a review of the literature. J Dent. 2000;28(3):163-177.
18. Gürel G. The Science and Art of Porcelain Laminate Veneers. Chicago, IL: Quintessence Publishing Co Inc; 2003 247-248.
19. Magne P, Kim TH, Cascione D, et al. Immediate dentin sealing improves bond strength of indirect restorations. J Prosthet Dent. 2005;94(6):511-519.
20. Ozturk N, Aykent F. Dentin bond strengths of two ceramic inlay systems after cementation with three different techniques and one bonding system. J Prosthet Dent. 2003; 89:275-281.
21. Jayasooriya PR, Pereira PN, Nikaido T, et al. Efficacy of resin coating on bond strengths of resin cement to dentin. J Esthet Restor Dent. 2003;15(2):105-113.
22. Jayasooriya PR, Pereira PN, Nikado T, et al. The effect of a “resin coating” on the interfacial adaptation of composite inlays. Oper Dent. 2003;28(1):28-35.
23. Terry DA. Prehybridization of indirect restorative preparations. Pract Proced Aesthet Dent. 2004;16(9): 661-662.
24. Pashley EL, Comer RW, Simpson MD, et al. Dentin permeability: sealing the dentin in crown preparations. Oper Dent. 1992;17(1): 13-20.
25. Cagidiaco MC, Ferrari M, Garberoglio R, et al. Dentin contamination protection after mechanical preparation for veneering. Am J Dent. 1996;9(2):57-60.
About the Author
Gregg A. Helvey, DDS
Adjunct Associate Professor
Virginia Commonwealth University School of Dentistry
Richmond, Virginia
Private Practice
Middleburg, Virginia