Minimal Preparation Veneers with a Pressed and Layered Lithium Disilicate Material
Mike Malone, DDS; Mike Bellerino, CDT
When it was introduced almost 4 years ago, the IPS e.max® system (Ivoclar Vivadent, Inc, Amherst, NY) simplified the way dental professionals think about all-ceramic restorations for highly esthetic cases. IPS e.max® Press, in particular, is a lithium disilicate glass ceramic that delivers the fit, form, and function expected from pressable ceramics, but does so with increased strength and optimized optical properties. Additionally, clinicians can use minimal preparation techniques for restorations fabricated with this material because technicians are able to cut back, layer, and thin down the material to achieve dimensions that require minimal tooth reduction.1
Besides its application for highly esthetic veneer restorations, the lithium disilicate material is indicated for anterior and posterior crown substructures and three-unit bridges with the second premolar as the posterior abutment tooth. IPS e.max Press, in particular, demonstrates a flexural strength of 400 MPa and is available in two opacity levels—medium and high—as well as a wide shade range of ingots.
However, to place lithium disilicate restorations with minimal preparation requires treatment planning and communication between the clinician and the laboratory ceramist to ensure esthetic and functional success. This article describes the clinical protocol and communication undertaken between the dentist and patient, and shared between the dentist and ceramist, to promote conservative tooth preparations and patient satisfaction with the anticipated final veneer restorations.
Case Presentation
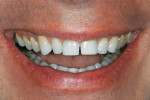
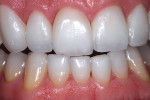
The patient, a 45 year-old man, presented with small, short incisors and diastemas between his teeth. A thorough clinical examination revealed that his teeth were healthy, with the exception of excessive wear. Multiple spaces between the patient’s teeth resulted from the discrepancy between tooth sizes. The esthetic evaluation also revealed a reverse smile line with excessive gingival display on the right side (Figure 1).
As part of the treatment planning process, computer imaging was performed to demonstrate for the patient how his smile could be enhanced. The patient approved the smile design demonstrated by the computer imaging, and this imaging was used as the basis for a laboratory-fabricated wax-up of the proposed restorations.
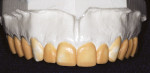
Impressions were made for use in developing study models. A face-bow transfer, centric relation bite registration, and preoperative photographs were also obtained as part of the record-gathering and laboratory-communication processes. This information—along with the patient-approved computer imaging—enabled the laboratory to fully complete the detailed prescription request for a diagnostic wax-up of the anticipated lithium disilicate veneers2 (Figure 2).
The proposed treatment plan included in-office tooth whitening (Zoom!®, Discus Dental, Culver City, CA), replacing the porcelain-fused-to-metal (PFM) restoration on tooth No. 14 with a lithium disilicate full crown, and placing 11 minimal preparation veneers fabricated from a lithium disilicate material (IPS e.max) on teeth Nos. 3 through 13. Additionally, the height of the gingival tissue on teeth Nos. 3 through 5 would be raised.
The patient underwent the in-office bleaching procedure first, after which he was reappointed for evaluation and review of the diagnostic wax-up. At that time, custom shade tabs were used to obtain the shade needed for the durable, light-cured provisional restorations that would be indirectly fabricated on a stone model.
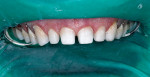
Before initiating tooth preparation, a rubber dam was placed. Minimal tooth reduction was achieved for teeth Nos. 3 through 14, leaving enamel on all surfaces (Figure 3). To ensure the conservative nature of the tooth reduction, a preparation guide made from the wax-up model was used to verify the facial and incisal reduction.3,4
It was during this preparation appointment that the gingival tissue height of teeth Nos. 3 through 5 was raised using an electrosurge unit. The appropriate amount of bone was also removed (after making impressions) to ensure stability of the tissue. Impressions were made (Identic syringable hydrocolloid/Identic alginate, Dux Dental, Oxnard, CA) and a model was poured with an ultra–fast–setting laboratory stone (Snap-Stone, Whip Mix Corp, Louisville, KY), on which the Radica® provisional restorations (DENTSPLY Ceramco, Burlington, NJ) were created (Figure 4).
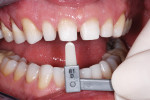
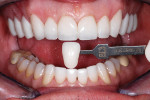
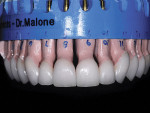
The stumpf shade (Ivoclar Vivadent, Inc) of the preparations was chosen and photographed (Figure 5), and the provisional restorations were bonded in place, except for one central incisor, using a spot-bonding technique and veneer resin cement (Insure Lite, yellow-red, Cosmedent, Inc, Chicago, IL). An impression was then made for developing the trial unit veneer, and the last veneer was spot-bonded in place. Additionally, a photograph of the bonded provisional restorations (Figure 6) was taken, showing the final shade tab in place to facilitate communication with the laboratory.
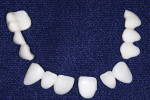
Minor modifications were required to the provisional restorations, after which the patient accepted their shade, texture, and translucency (Figure 7). The patient later approved the trial unit veneer that was created and presented at a subsequent appointment (Figure 8) before the fabrication of all 11 units (Figure 9). The acceptance of the trial unit is very important in eliminating remakes caused by shade miscommunications.
Delivery of the Lithium Disilicate Veneers
Because communication between the dentist and patient, as well as the dentist and laboratory ceramist, was thorough and detailed—encompassing every aspect of the function and esthetics of the proposed lithium disilicate veneers—the cementation appointment went smoothly. The posterior restoration was bonded into place using a dual-cure resin cement (Multilink® Automix, Ivoclar Vivadent, Inc). Then, the veneer restorations were tried in for fit and, after isolating with a rubber dam, adhesively bonded using bonding agents (Clearfil® Liner Bond 2V and Clearfil® Photo Bond, Kuraray America, Inc, New York, NY) and a light-cure resin cement (Insure).
Conclusion
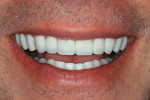
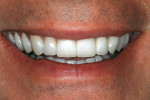
Excellent functional and esthetic results were achieved with minimal preparations that left virtually no exposed dentin. In particular, this case demonstrated the manner in which a lithium disilicate material (IPS e.max Press) can be pressed and layered to produce ideal esthetic and restorative results while maintaining a conservative clinical protocol (Figure 10).
References
1. Javajeri D. Considerations for planning esthetic treatment with veneers involving no or minimal preparation. J Am Dent Assoc. 2007;138(3):331-337.
2. Gürel G. Porcelain laminate veneers: minimal tooth preparation by design. Dent Clin NorthAm. 2007;51(2):419-431.
3. Cho GC, Donovan TE, Chee WWL. Clinical experiences with bonded porcelain laminate veneers. J Calif Dent Assoc. 1998; 26(2):121-127.
4. Trinkner TF, Roberts M. A systematic approach to anterior esthetics. Contemporary Estheticsand Restorative Practice. 2003; 7(1): 42-49.
About the Authors
Mike Malone, DDS
Past President and Accredited Member
American Academy of Cosmetic Dentistry
Private Practice
Lafayette, Louisiana
Mike Bellerino, CDT
Accredited Member
American Academy of Cosmetic Dentistry
Metairie, Louisiana