“Same-Day” Porcelain Veneers: Fact or Fiction?
Alex Touchstone, DDS
By way of this publication and others, study club meetings, conferences, and the Internet, our profession is fed a steady, albeit “high-calorie,” diet of technique/technology options. While the offerings are as varied as the foods we eat, they all share the promise of improved patient care and enhancement of our delivery of the same.
Alexander Pope’s often-referenced statement, “Be not the first by whom the new is tried, nor yet the last to cast the old aside,”1 though not made in the context of oral healthcare decisions, provides a valid benchmark for integration decisions in dentistry. In fact, from the author’s perspective, the best use of a technique or technology in dental practice is one that supports time-honored principles of complete dentistry while improving the workflow efficiency in the process.
In his latest text, Dr. Peter Dawson defines complete dentistry as “a philosophy that underlies an honest concern for patients.2 Regardless of where one stands in the circle of occlusion debates, there is universal truth to be found in Dawson’s implication that patient experiences and outcomes should remain our primary focus. He expands his definition further by outlining seven associated goals:2
- Freedom from disease in all masticatory system structures;
- Maintainably healthy periodontium;
- Stable temporomandibular joints (TMJs);
- Stable occlusion;
- Maintainably healthy teeth;
- Comfortably healthy function; and
- Optimum esthetics.
It is fair to say that patients today are more discerning—even demanding—than ever regarding the care they receive. Thanks to the Internet, patients often come to ap-pointments equipped with questions in hand. The initial consultation can feel more like an interview of the prospective dentist. Patients also bring expectations that require identification and careful management. It is not uncommon for patients to ask experiential questions and to expect to see photographs of other patients who have received similar care to that proposed. Though not always verbalized, patients have certain goals in mind. In fact, the patients’ goals, if listed, could look something like this:
- Painless procedure;
- Least possible number of visits;
- Genuine empathy by the dental team;
- Maximum longevity;
- Reasonable cost;
- Both short- and long-term comfort; and
- Optimum esthetics as seen through the eyes of the patient.
Interestingly, both Dr. Dawson’s goals for complete dentistry and patients’ goals for treatment outcomes parallel one another in that they are patient-centered, yet they are born of two different perspectives. The ideal treatment outcome is one that harmonizes the patient’s point of view and the dentist’s expertise. The following case report of a patient who received 10 porcelain veneers in a single treatment visit will be used as a springboard for discussion of the techniques and technologies that support the concept of complete dentistry. It is within this context that two seemingly opposing ideals come together for the benefit of the patient—careful, comprehensive treatment planning and a highly compressed time frame for completion.
The First Step: Data Gathering
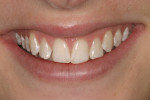
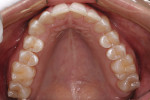
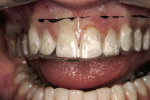
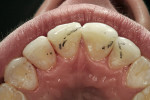
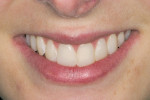
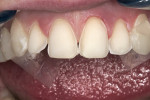
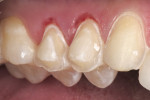
The patient presented with a concern of an unattractive smile. In her words: “I want my smile to be pretty, but also natural-looking.” Objectively, her smile did indeed show evidence of mild fluorosis, undesirable tooth position for teeth Nos. 4, 5, 7, 10, and perhaps 11, and variance in gingival zeniths that detracted from the overall symmetry of her smile (Figure 1; Figure 2; Figure 3). The following steps of data gathering/discovery were accomplished to formulate the treatment plan.
First, comprehensive periodontal and oral cancer screenings were performed. The oral cancer screening was accomplished by observing the tone, texture, and integrity of the soft tissues of her head and neck, intra- and extraorally, and through palpation of these tissues. Further oral cancer screening was performed via radiographic interpretation of a volumetric dental cone-beam scan (CBCT) (Galileos, Sirona Dental Systems, Inc, Charlotte, NC).
Periodontal bone levels, ligament integrity, and subjective bone quality were assessed using the same CBCT scan. All were found to be normal/healthy. Her periodontal condition was also assessed through a six-point-per-tooth probing and recording of probing depths and bleeding, if present. There were no bleeding points on probing and pocket depths were all less than 4 mm.
Evaluation of her TMJ structures was also performed using the CBCT scan. Both the left and right condyles and eminentia were grossly normal radiographically. She demonstrated clinically normal range of mandibular motion without joint sounds or deviation on opening. Palpation of the muscles of mastication did not elicit any discomfort.
Clinical inspection of her occlusion revealed no abnormal wear facets or evidence of parafunction. She demonstrated canine guidance with posterior disclusion in both left and right lateral excursions. All teeth were assessed for mobility and classified as I or normal. In addition to clinical observation of the patient’s functional pathways, maxillary and mandibular polyvinyl siloxane impressions, an ear-bow transfer, and occlusal records in both maximum and centric relation occlusion were made for further study and diagnostic wax-up. Caries detection followed with the aid of further clinical evaluation and radiographic interpretation of digital posterior bitewing x-rays (XIOS, Sirona Dental Systems, Inc). A full series of digital photographs was made during the visit as well.
A conversation with the patient regarding her esthetic expectations continued throughout the appointment and included review of other patients’ smiles to elicit responses from her that formed the basis for final tooth form and color selection.
Based on the findings of fluorosis, problems with tooth position, length, and color, along with periodontal and TMJ health and normal occlusal function, a provisional treatment plan of mandibular tooth whitening, gingival sculpting, and porcelain veneers for teeth Nos. 4 through 13 was considered and discussed with the patient. The patient agreed to proceed and was appointed for a treatment plan presentation and mandibular tooth whitening.
The Second Step: Treatment Plan Confirmation
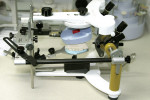
To confirm the proposed treatment plan, the impressions were poured in die stone and mounted in centric-relation occlusion on a semi-adjustable articulator (Stratos® 300, Ivoclar Vivadent, Amherst, NY) (Figure 4). A diagnostic wax-up of the 10 proposed restorations followed with further confirmation that occlusal harmony would be maintained for the patient. A duplicate cast was created of the wax-up and a matrix of that was made with a clear vacuum-formed material. Radiographs and photographs were reviewed again.
The Third Step: Presentation, Esthetic Conversation and Tooth Whitening
During the patient’s second visit, she was asked to evaluate the contours of the teeth as presented in the wax-up and to reiterate her preferences regarding tooth color, shape, and incisal translucency. As the result of these preferences, a target body shade of VITA 3D 0M3 (Vident, Brea, CA) was selected with plans for subtle incisal translucency. She agreed to the proposed treatment plan and received a 1-hour session of in-office tooth whitening (Zoom!, Discus Dental, Culver City, CA) limited to her mandibular teeth. She was told to expect her next appointment to be lengthy, lasting about 6 to 8 hours but that the advantage for her was that she would not have to endure wearing temporary veneers or any associated laboratory delay. She saw the single-visit treatment workflow as a definite benefit and approved.
The Fourth Step: “Single Visit” Veneers
The patient was scheduled for a day-long visit. After administering local anesthesia (4% articane plus 1:200,000 epinephrine, Septodont Inc, New Castle, DE), slight adjustment of the gingival zeniths of teeth Nos. 4, 5, 9, and 10 was accomplished using a diode soft-tissue laser (SIROlaser, Sirona Dental Systems, Inc). Minimal reduction of the labioverted teeth was then performed using a finishing diamond bur to allow for complete seating of the clear matrix of the diagnostic wax-up (Figure 5).
The matrix was filled with flowable composite, seated again, and the composite was light-cured through the matrix. The contours of the composite replicates of the diagnostic wax-up were refined as were the incisal edges, with attention given again to functional harmony (Figure 6).
The composite replicates serve three very useful purposes. First, they allow for intraoral verification of occlusal harmony by virtue of having the patient go through border movements on the composites before copying them into the software. Second, the patient and dentist are afforded a preview of the intended result and further feedback is gained from the patient, thus making approval of the final restorations more likely (Figure 7). If the patient or the dentist feels that a trial period is appropriate before creating the final restorations, then the composite replicates may serve in that capacity as well. Because the composites are bonded to the teeth in a conventional fashion, if a trial period is desirable, then the patient simply leaves the office to return on a later date after an agreed upon timeframe for the creation of the restorations. Third, and somewhat unique to the single-visit CAD/CAM workflow, the replicates are scanned directly into the software and used as a virtual diagnostic wax-up in the creation of the final restorations.
At this point, segments of the arch are chosen for convenience and maximum efficiency when working with a chairside CAD/CAM imaging, design, and milling system (CEREC® 3D, Sirona Dental Systems, Inc). In this case, they were the following: incisors in one segment; left canine and premolars in the second and right canine; and premolars in the third.
The composite replicates of the wax-up for teeth Nos. 7 through 10 were then imaged with an infrared scanning camera that is part of the CEREC system. These images form the basis from which a virtual diagnostic wax-up is created in the software. Next, the four incisors were prepared, again using the clear matrix as a reduction guide. Care was taken to arrive at a uniform reduction for all teeth relative to the final tooth contours. The prepared incisors were then scanned in an identical manner to the previous scans. This resulted in a preparation model and virtual diagnostic wax-up model that were precisely superimposed over one another within the CEREC software.
The four incisors were then simply designed to fit to the contours of the diagnostic wax-up and milled from one of a variety of materials, which in this case was VITA Mark II 0M1 shade glass ceramic (Vident). Once milled, glass ceramics lend themselves well to surface texturing and either staining and glazing or polishing. In this case, polishing the veneers was accomplished using only a diamond polishing paste and a stiff laboratory rotary bristle brush (Diashine, VH Technologies Ltd, Bellevue, WA).
Interestingly, the author has observed through electron microscopy studies3 that both milled leucite and feldspathic glass ceramics seem to possess enhanced polishability over those that have been processed via more traditional stacking and firing or pressing techniques. For example, Figure 8 is a scanning electron micrograph (SEM) made at 500 magnification of the polished surface of a sample of VITABLOCS Mark II® (Sirona Dental Systems, Inc) milled ceramic. Figure 9 is a SEM at 500 magnification of a sample of Vitadur Alpha (Vident) veneering porcelain, which was polished with the same procedure as the Mark II. These two materials are virtually identical chemically but they are processed in different ways, which results in the milled ceramic having more density and fewer inclusions. As these two figures illustrate, a polished milled ceramic, because of its increased density, will have a smoother surface than its laboratory-fired counterpart, thus giving the milled/polished material more favorable wear characteristics.
The choice was made to bond the incisors before preparation of segments two and three to prevent undue patient sensitivity or continued need for local anesthetic. The veneers were prepared for bonding by hydrofluoric acid-etching, rinsing, drying, silane application, and drying again without rinsing. The incisor teeth were isolated, etched for 30 seconds with phosphoric acid (Figure 10) and the veneers were bonded with a standard bonding protocol using a combination of a bonding agent/composite resin cement (Futurabond and Gradio Veneer, VOCO America, Sunnyside, NY).
After delivery of the incisor veneers, the other two segments were completed in a similar manner. The preparations for the canines and premolars, however, were more aggressive in the incisal/occlusal regions to allow for adequate material thickness in areas that would endure heavier functional occlusal loads (Figure 11). The remaining veneers were treated and bonded in the same fashion as the incisors. They were then adjusted to harmonize with the opposing teeth in the envelope of function.
Conclusion
At first glance, the prospect of milling CAD/CAM porcelain veneers and placing them in one day may seem novel and/or unproven. In considering this argument, it is useful to break the procedure down to the categories of restorative material used (feldspathic porcelain), fabrication technique (chairside milling), finishing technique (polishing), and bonding technique (total-etch and light-curing with composite-resin luting agents).
The reader can appreciate that the material, feldspathic porcelain, used to fabricate these veneers is certainly not new to dentistry, having been generally accepted for restorations placed in low-stress situations for decades.4 What may be less apparent is that the excellent longevity of veneers created via a chairside milled technique is confirmed.5 Marginal integrity is also well-established as on par with or superior to laboratory-fabricated restorations when created from the same class of materials.6-10 Polishing results in a surface that wears opposing enamel minimally and compares favorably to that of gold.11-13 Total-etch bonding, especially to enamel, is widely accepted as resulting in a tenacious and long-lasting interface.14 The evidence clearly supports the technique of chairside milling of CAD/CAM restorations, including veneers.
It is both possible and, with proper planning, entirely practical to provide patients with as many as 10 to 12 porcelain veneers—or other milled restoration types for that matter—in a single chairside visit. With the compressed workflow, however, comes the heightened necessity to carefully and comprehensively plan the case, with attention given to both the technical concepts of complete dentistry and to the patient’s goals as to desired outcome. In addition to the fact that she was able to receive her veneers in a single treatment day, this patient also received optimum care that resulted in restorations whose appearance meets her expectations (Figure 12, Figure 13 and Figure 14) and very good long-term prognosis.
References
1. Pope A. “An Essay on Criticism.” 1711.
2. Dawson P. Functional Occlusion, From TMJ to Smile Design. St. Louis, MO: Mosby; 2006: 4-5.
3. Touchstone A. SEM comparison of surface texture after polishing of milled versus veneering porcelains. Non-published data, August 2005.
4. Johnston WM, O’Brien WJ. The shear strength of dental porcelain. J Dent Res. 1980;59(8):1409-1411.
5. Wiedhahn, K. CEREC veneers. In: Mörmann WH (ed). State of the Art of CAD/CAM Restorations, 20 Years of CEREC. Berlin: Quintessence, 2006:65-72.
6. Fasbinder DJ. Margin fit. In: Mörmann WH (ed). State of the Art of CAD/CAM Restorations, 20 Years of CEREC. Berlin: Quintessence, 2006: Poster.
7. Sturdevant JR, Bayne SC, Heymann HO. Margin gap size of ceramic inlays using second-generation CAD/CAM equipment. J Esthet Dent. 1999;11(4): 206-214.
8. Denissen H, Doziç A, van der Zel J, van Waas M. Marginal fit and short-term clinical performance of porcelain-veneered CICERO, CEREC, and Procera onlays. J Prosthet Dent. 2000;84(5):506-513.
9. Suh PS, Johnson R, White SN. Fit of veneers made by CAD-CAM and platinum foil methods. Oper Dent. 1997;22(3):121-127.
10. White SN, Suh PS, Yu Z, Johnson R. Effect of fit adjustment on CEREC CAD/CAM veneers. Am J Dent. 1997;10(1):46-51.
11. Kelly R. Mach Cer. In: Mörmann WH (ed.). State of the Art of CAD/CAM Restorations, 20 Years of CEREC. Berlin: Quintessence, 2006:29-38.
12. Krejci I: Wear of CEREC and other restorative materials. In: First International Symposium on Computer Restorations. Berlin: Quintessence, 1991:245-251.
13. al-Hiyasat AS, Saunders WP, Sharkey SW, et al. The abrasive effect of glazed, unglazed, and polished porcelain on the wear of human enamel, and the influence of carbonated soft drinks on the rate of wear. Int J Prosthodont. 1997;10(3):269-282.
14. Strassler HE. Applications of total-etch adhesive bonding. Compend Contin Educ Dent. 2003;24(6):427-441.
About the Author
Alex Touchstone, DDS
Private Practice
Charlotte, North Carolina