Reversing Local Anesthesia
Stanley F. Malamed, DDS
Local anesthesia forms the backbone of pain-control techniques in dentistry. The prevention and elimination of pain during dental treatment has benefited patients, their doctors, and dental hygienists, enabling the dental profession to make tremendous therapeutic advances that would otherwise have been impossible. Introduced in the late 1940s, the amide local anesthetics represent the most used drugs in dentistry. Local anesthetics also represent the safest and most effective drugs in all of medicine for the prevention and management of pain.
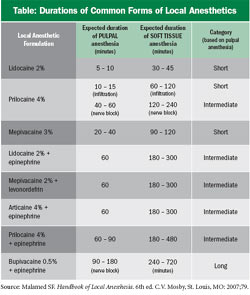
Five local anesthetics are used in dentistry in the United States. The Table presents the currently available formulations. There are three categories of local anesthetics based on the expected duration of pulpal anesthesia: short-, intermediate- and long-acting. The goal in using a specific local anesthetic formulation is to be able to complete the planned dental treatment comfortably. Given an average dental-appointment length of 44 minutes,1 it is no surprise that the intermediate-duration formulations are those most often used. Pulpal anesthesia allows the dental procedure to be performed painlessly.
Anesthesia of the supporting tissues—both bone and soft tissue (lip, tongue, chin, nose, and cheek)—usually persists for several hours after pulpal anesthesia has been lost.2-4 Though normally of minimal concern, residual soft tissue anesthesia (STA) may result in injury, either self-inflicted (eg, biting) or secondary to thermal or chemical burns. This is of particular concern in pediatric patients who may chew a bitten lower lip because it is painless, causing ulceration of the oral mucosa (Figure 1). One recent study measured a 13% incidence of injury after mandibular anesthesia in pediatric patients.5 More commonly, however, residual STA is more of an inconvenience or annoyance to the patient and doctor than a risk. Patients feel that residual STA interferes with their normal daily activities in three areas: perceptual (perception of altered physical appearance), sensory (lack of sensation), and functional (diminished ability to speak, smile, drink, and control drooling).6
In some clinical situations, primary postsurgical, prolonged soft tissue anesthesia is desirable. Dental surgeons have successfully combined oral non-steroidal anti-inflammatory drugs along with the long-acting local anesthetic bupivacaine HCl to successfully manage pain in the postsurgical period.7
The majority of dental procedures, however, are less invasive (eg, routine restorations, non-surgical periodontics) and have little to no associated postoperative pain. Indeed many dental patients complain to their doctors at subsequent appointments that they were unable to eat a meal or to talk normally for many hours after their last dental visit because their lip and/or tongue were still numb. The request of “Doctor, can’t you make the numbness go away faster?” has been uttered by patients to most doctors.
Reversal of soft tissue anesthesia
Attempts have been made to minimize the duration of local anesthesia-induced numbness. As recently as the 1980s, the intraoral use of the medical procedure known as transcutaneous electrical nerve stimulation (TENS) experienced a brief period of popularity as a possible substitute for local anesthetics to provide operative pain control in dentistry.8 As the technique was not consistently reliable, which is an important criterion for clinical acceptance, it ultimately fell short of success and has, with few exceptions, been discarded. However, the technique—known in dentistry as Electronic Dental Anesthesia (EDA)—which produced both a rhythmic skeletal muscle contraction as well as localized vasodilation in the region to which it was applied, was shown to decrease the duration of residual soft tissue anesthesia. This decrease in the duration of postoperative soft tissue anesthesia with EDA was thought to result from (1) its increasing blood flow through the area into which local anesthetic had previously been deposited (as a result of EDA’s vasodilatory action), along with (2) a pumping action produced by the rhythmic contraction of skeletal muscles. The local anesthesia drug would undergo a more rapid redistribution into the capillaries and venules in the area.9,10
At present, no therapeutic modality exists to hasten the return of normal sensation and function after local anesthetic injection. Recently, the search for a pharmacologic means of minimizing postoperative anesthesia has focused on phento-lamine mesylate, which is a nonselective competitive a-adrenergic antagonist that has been demonstrated to reverse vasoconstriction in rats, cats, and dogs resulting from nerve-stimulated release of norepinephrine or locally applied norepinephrine or epinephrine.11-13 Phentolamine antagonizes catecholamine-induced dysrhythmias in the heart14 and has been used clinically in the United States for the prevention of hypertensive episodes, norepinephrine-related dermal necrosis, and for the diagnosis of pheochromocytoma for more than 50 years. As presently used in medicine, phentolamine mesylate is categorized by the United States Food and Drug Administration (FDA) as a Pregnancy category “C” and as “Safety Unknown” for nursing mothers.*
Randomized, controlled phase 2 and phase 3 clinical trials evaluating the safety and efficacy of a proprietary formulation of phentolamine mesylate in both adults and children (aged 4 to 11 years) have been completed and a New Drug Application (NDA) was approved in May 2008 by the FDA for marketing under the name OraVerse (Novalar Pharmaceuticals, Inc, San Diego, CA).
Briefly summarizing these as yet-unpublished clinical trials, overall for both maxillary supraperiosteal and mandibular inferior alveolar nerve block and mental block injections, phentolamine mesylate accelerated the time to return of “normal lip sensation” relative to a “sham” injection by more than 80 minutes (approximately 60 min vs 140 min). This represents a clinically and statistically significant (P < .0001) decrease in the duration of STA.15
These trials demonstrated no significant affect on pain (there was no return of pain after its administration nor was the injection of phentolamine mesylate itself painful (because it was injected into anesthetized tissues). The injection of phentolamine mesylate was not associated with any serious adverse events nor were there any adverse effects on vital signs or patient-reported pain. No clinically observable effects on the oral mucosa were noted. The results of these trials are in press.15
The findings of a pediatric trial of phentolamine mesylate in subjects aged 4 to 11 years were similar to those of the adult trials. Return to normal lip sensation occurred approximately 75 minutes faster compared with sham injection (P < .0001) in children ages 6 to 11. No serious adverse events, effect on vital signs, or patient-reported pain were noted. The article reporting the results of this trial is in press.16
The blood level of local anesthetic was not affected by the local injection of phentolamine in either the adult or pediatric populations.15,16 The only effect the injection of phentolamine had on the blood levels of local anesthetic was to delay the time to peak concentration. This result is consistent with the hypothesis that phentolamine accelerates the rate of recovery by accelerating the rate of redistribution of local anesthetic from the submucosa into the cardiovascular system.17
Clinical trials of phentolamine mesylate have compared the reversal action of the drug with articaine plus epinephrine, lidocaine plus epinephrine; mepivacaine plus levonordefrin; and prilocaine plus epinephrine. Similar results were obtained for each type of anesthetic solution.15
CLINICAL APPLICATION OF PHENTOLAMINE MESYLATE
Phentolamine mesylate (OraVerse) will be packaged in cartridges identical, except for labeling, to traditional local anesthetic cartridges. It may be administered with any dental local anesthetic syringe and dental injection needle. Use of phentolamine mesylate as a reversal agent for dental intraoral local anesthesia would follow the pattern described below.
The patient receives a traditional intraoral injection of local anesthetic, with or without a vasoconstrictor, at the onset of dental treatment. The choice of local anesthetic is determined by the expected duration of pulpal anesthesia required to complete the dental procedure (Table).
At the conclusion of the “traumatic” portion of the dental procedure (eg, the procedure necessitating pulpal anesthesia, such as drilling) phentolamine mesylate is administered. It will be injected into the same site as the local anesthetic was previously deposited (eg, via a right inferior alveolar nerve block injection when treating the mandibular right quadrant). For adults the proposed dosage is 1 to 2 cartridges of phentolamine mesylate (a dose of 0.4 mg to 0.8 mg), while for children the proposed dosage is 0.5 to 1 cartridge (0.2 mg to 0.4 mg).15,16 Phentolamine mesylate produces a localized vasodilation, increasing perfusion at the site of deposition, and likely leads to a more rapid redistribution of the local anesthetic from the injection site into capillaries and venules and away from the oral cavity.17
A clinical example of how the reversal of local anesthetic might benefit a patient is seen in Figure 2. In the present environment, without a local anesthetic reversal agent, the patient arrives for a 1-hour dental appointment in the mid- to late afternoon. As the procedure requires tooth preparation, the dentist elects to administer 2% lidocaine with epinephrine 1:100,000 via inferior alveolar nerve block. Successful anesthesia is achieved. Treatment commences and is completed in approximately 45 minutes. The dentist discharges the patient who leaves the office approximately 1 hour after having received the local anesthetic. The patient’s lip and tongue are still numb. Apart from the fact that the patient feels strange because of this residual numbness (eg “my lip feels fat”), the patient will be unable to eat, or if he does, unable to eat without an increased risk of traumatic soft tissue injury, when dinner is served several hours later.
With the administration of phentolamine mesylate at the conclusion of the traumatic portion of the treatment (tooth preparation) or immediately after the dental procedure, residual soft tissue anesthesia (eg, lip and tongue) has completely resolved by the time dinner is served.
CANDIDATES FOR LOCAL ANESTHETIC REVERSAL
A majority of dental treatments today are not so traumatic in nature that they require a patient to leave the dental office with residual soft tissue anesthesia that lingers for many hours before resolving. These procedures include conservative dental restorations and non-surgical periodontics, such as scaling and root planing. In addition, pediatric patients, whether in the general dentistry or pediatric dentistry office, will benefit from the diminished soft tissue duration associated with phentolamine mesylate administration.
CONCLUSION
Prolonged facial and lingual anesthesia is an often unnecessary and unwanted consequence of intraoral local anesthesia. Many dental patients report that prolonged soft tissue anesthesia interferes with normal oral function. Self-inflicted injuries can occur.
The results of clinical trials with phentolamine mesylate in anesthetized patients demonstrate that its administration after routine dental or periodontal maintenance procedures should yield a significant benefit. Faster recoveries of normal sensation (lip and tongue), as well as a faster return to normal ability to smile, speak, and drink, and to refrain from drooling and inflicting self-injury are highly desirable. The prevention of self-injury resulting from lingering soft tissue anesthesia, particularly in pediatric patients, is an additional important clinical benefit. The high probability that phentolamine mesylate administration would safely accelerate the recovery of both observed and perceived normal sensation and function significantly compared to the current standard of care with minimal risk will likely be perceived as both desirable and beneficial by many dental patients and clinicians.
DISCLOSURE
Dr. Malamed is a current consultant for Novalar Pharmaceuticals.
References
1. American Dental Association, 2002 Survey of Dental Practice—Characteristics of Dentists in Private Practice and Their Patients. American Dental Association, Chicago, IL; 2004.2. Hersh EV, Hermann DG, Lamp CJ, et al. Assessing the duration of mandibular soft tissue anesthesia. J Am Dent Assoc. 1995;126(11):1531-1536.
3. Malamed SF: Local anesthetics: Dentistry’s most important drugs. Clinical Update 2006. J Calif Dent Assoc. 2006;34(12):971-976.
4. Yagiela JA. Recent developments in local anesthesia and oral sedation. Compend Contin Educ Dent. 2004;25(9):697-706.
5. College C, Feigal R, Wandera A, Strange M. Bilateral versus unilateral mandibular block anesthesia in a pediatric population. Pediatr Dent. 2000;22(6):453-457.
6. Rafique S, Fiske J, Banerjee A. Clinical trial of an air-abrasion/chemomechanical operative procedure for restorative treatment of dental patients. Caries Res. 2003;37:360-364.
7. Malamed SF. Handbook of Local Anesthesia. 5th ed. C.V. Mosby, St. Louis, MO: 2004;277-278.
8. Smith MJ, Hutchgins RC, Hehenberger D. Transcutaneous neural stimulation use in postoperative knee rehabilitation. Am J Sport Med. 1983;11:75-82.
9. Hochman R. Neurotransmitter modulator (TENS) for control of dental operative pain. J Am Dent Assoc. 1988;116:208-212.
10. Meechan JG, Gowans AJ, Welbury RR. The use of patient-controlled transcutaneous electrical nerve stimulation (TENS) to decrease the discomfort of regional anaesthesia in dentistry. A randomized controlled clinical trial. J Dent. 1998;26(5):417-420.
11. Edwall B, Gazelius B, Fazekas A, et al. Neuropeptide Y (NPY) and sympathetic control of blood flow in oral mucosa and dental pulp in the cat. Acta Physiol Scand. 1985;125:253-264.
12. Koss MC. Differential neural activation of vascular alpha-adrenoreceptors in oral tissues of cats. Eur J Pharmacol. 2002;440: 53-59.
13. Walker HA, Heymans L, Wilson S, Richardson AP. The effect of C-7337 on carotid sinus reflex and on pressor and peripheral vascular actions of epinephrine and nor-epinephrine. J Pharmacol Exp Therap. 1950;98: 33-34.
14. Leimdorfer A. Prevention and abolition of cardiac arrhythmias by Regitine. Society Proceedings. 1952;171: 742-743.
15. Hersh EV, Moore PA, Papas AS, et al. Reversal of soft tissue local anesthesia with phentolamine mesylate. J Am Dent Assoc. In press.
16. Tavares M, Goodson JM, Studen-Pavlovich D, et al. Reversal of soft tissue local anesthesia with phentolamine mesylate in pediatric patients. J Am Dent Assoc. In press.
17. Moore PA, Hersh EV, Papas AS, et al. Pharmacokinetics of lidocaine with epinephrine following local anesthesia reversal with phentolamine mesylate. Anesth Prog. In press.
* Pregnancy category ‘C' - animal studies show adverse fetal effect(s) but no controlled human studies OR no animal or human studies; weigh possible fetal risk vs. maternal benefit. Lactation category ‘Safety Unknown' - Inadequate literature available to assess risk; caution advised.
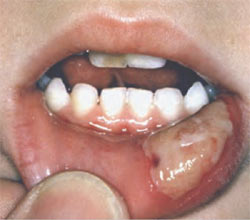 |  | |
| Figure 1 Traumatic injury to lip while soft tissue still anesthetized. Photograph courtesy Dr. John Yagiela. | ||
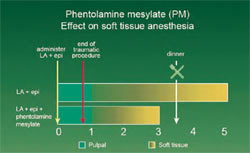 | ||
| Figure 2 The effect of phentolamine mesylate on residual soft tissue anesthesia (STA). The patient receives an injection of a local anesthetic with epinephrine at time ‘0'. In the upper horizontal bar the treatment is completed in 44 minutes and the patient is dismissed. Residual STA persists for about 4 hours, interfering with the patient's ability to eat and increasing the risk of traumatic soft tissue injury. In the bottom horizontal bar, the patient receives an injection of phentolamine mesylate at the conclusion of the traumatic dental procedure. Residual STA lasts only about 2 more hours, enabling the patient to eat a meal without increased risk of traumatic soft tissue injury. | ||
| About the Author | ||
 Stanley F. Malamed, DDS Stanley F. Malamed, DDS Professor of Anesthesia & Medicine School of Dentistry University of Southern California Los Angeles, California | ||



