Resin-based Composite Margin Repair
Theodore P. Croll, DDS; and Kevin J. Donly, DDS, MS
Wear and tear breaks down teeth and dental materials alike. Just like artificial hips, prosthetic knees, shoulder replacements, and natural human bones, all parts of us, natural and artificial, are subject to degenerative changes resulting from physical forces existing around and within us, over time. Constant and extreme thermal changes, saliva and foodstuffs with varying acidities, and the impact and abrasive forces of occlusion and mastication all take their toll on dental structures and dental materials used in tooth repair. The interface of dentin and enamel and applied tooth repair materials is in a constant dynamic state. Because different substances have different coefficients of thermal expansion, intraoral temperature changes will expand and contract tooth structure to certain dimensions, and restorative materials will deform differently under the same influences.
Resin-based composite dental filling material (RBC), no matter how well adhesively bonded to tooth structure, is subject to these principles. Whether such material is mechanically interlocked, along with being adhesively bonded—such as in the case of a Class I or Class II tooth restoration—or applied and micromechanically retained by the acid-etch method, marginal regions often need repair, as time goes by.
Christensen's essay1 gave a concise and up-to-date view of the subject. Other reports have described methods of repairing RBC restorations, and the bond strengths achieved by such repairs.2-8 This article briefly describes a method of refining and sealing RBC margins that, although not carious, require improvement. Using a self-etching bonding agent and an unfilled clear resin sealant material, cavosurface margins can be smoothed and sealed and tooth appearance improved.
Clinical Technique
Using two typical cases, marginal repair has been documented.
Case One
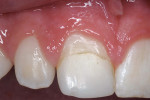
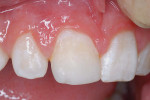
A teenager had a large coronal RBC repair of a fractured central incisor done 6 years previously (Figure 1a). The color match of the restorative material to surrounding tooth structure and other adjacent teeth was acceptable; however, the resin margin was raised and separated from the underlying enamel on the lingual and labial tooth surfaces. Using the Prompt® L-Pop® bonding system (3M ESPE, St. Paul, MN) and Delton brand clear resin sealant (Dentsply, York, PA), the defective margins were repaired as follows:
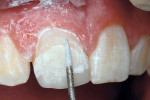
1. Using a medium-grit tapered diamond bur at slow speed, the resin was trimmed flush to the labial enamel surface (Figure 1b and Figure 1c). In addition, surrounding enamel 2 mm to 3 mm beyond the margin was roughened with the diamond bur. Preparation of the adjacent enamel not only removes any aprismatic enamel, but also eliminates the fluoride-rich outer 10 µm.9,10 Such enamel preparation enhances the ability of the self-etching resin bonding agent to etch the freshly ground surface.11
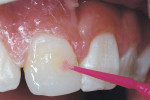
2. The Prompt L-Pop self-etching bonding agent was painted liberally over the trimmed RBC surface and adjacent enamel. It was gently agitated with the applicator tip for 30 seconds (Figure 1d), but not yet polymerized with the light beam. A thin coating of Delton sealant was then painted over the bonding agent (Figure 1d). Exposure to the visible light beam (1,100 mW/cm2) for 15 seconds followed.
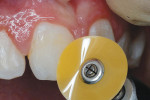
3. The treated surfaces were then finished with a polishing disk at slow speed (Figure 1e).
4. The lingual surface was then repaired in the same manner.
5. The RBC restoration had no perceptible marginal defects 6 months after repair (Figure 1f).
Case Two
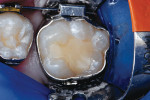
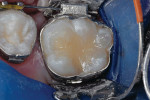
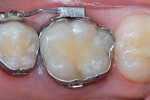
A 13-year-old boy had an occlusal RBC restoration of a mandibular permanent first molar placed 5 years previously. The restorative material was intact, but marginal separation was evident in the entire cavosurface periphery (Figure 2a). After occlusal RBC restoration of his second permanent molar, the rubber dam retainer was repositioned on the first molar, and defective margins repaired as follows:
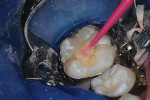
1. Several sizes of round diamond burs were used at slow speed to smooth the raised marginal resin flush to the enamel surface, and also roughen the RBC and enamel that surrounded the cavosurface margin (Figure 2b and Figure 2c). Different sized diamonds that conformed to the varying shapes of the grooves and cuspal slopes were used, in the same way that a sculptor uses instruments to shape different configurations in a sculpture. A minute and insignificant amount of surface resin is removed in this process.
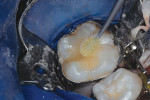
2. In the same manner as in Case One, the self-etching bonding agent was applied and gently agitated for 30 seconds. The clear sealant was then applied, without first exposing the bonding agent to the polymerizing light (Figure 2d and Figure 2e).
3. The light beam (1,100 mW/cm2) was then applied for 15 seconds (Figure 2f).
4. The repaired surface showed improvement immediately after treatment (Figure 2g) and 16 months afterwards (Figure 2h).
Discussion
Based on the concept of "smooth surface sealing"12 we have repaired marginal defects in RBC material using slow-speed, diamond-bur smoothing followed by the standard acid-etch technique (etch/rinse/dry) and Delton sealant since the 1980s. The method has been simplified with the availability of self-etching bonding agents. Although, in our experience, both ap-proaches have yielded sure and lasting improvement in marginal adaptation and appearance, the exact nature of the bond to both the roughened RBC material and surrounding enamel has not been evaluated microscopically. Questions to be answered when using the self-etching bonding agent with clear resin sealant include:
• How much sealant is taken up in the "microgap" that exists in the cavosurface interface?
• How deep do the resin tags penetrate into the etched enamel and how is that affected over time?
• What microscopic or clinical differences would there be if other self-etching bonding agents, other resin sealant materials, or if the standard etch/rinse/dry acid-etch procedure were to be substituted in the above protocol?
• Is there any significant bonding between the old RBC and freshly applied unfilled sealant?
• Would more or less etching time improve or decrease how the sealant attaches to either the old filling material or enamel?
Disclosure
The authors have no financial interest in any product or company mentioned in this article.
References
1. Christensen GJ. When and how to repair a failing restoration. J Am Dent Assoc. 2007;138:1605-1607.
2. Boyer DB, Chan KC, Torney DL. The strength of multilayer and repaired composite resin. J Prosth Dent. 1978;39:63-67.
3. Chan KC, Boyer DB. Repair of conventional and microfilled composite resins. J Prosth Dent. 1983;50:345-350.
4. Meeker HG, Hirsch SM, Kaim JM. Repairing voids at cavosurface-composite resin margins. J Prosth Dent. 1983;50: 636-638.
5. Boyer DB, Chan KC, Reinhardt JW. Build-up and repair of light-cured composites: bond strength. J Dent Res. 1984;63: 1241-1244.
6. Pounder B, Gregory WA, Powers JM. Bond strengths of repaired composite resins. Oper Dent. 1987;12:127-131.
7. Croll TP. Repair of defective class I composite resin restoration. Quintessence Int. 1990;21:695-698.
8. Croll TP. Repair of class I resin-composite restoration. ASDC J Dent Child. 1997;64:22-27.
9. Duschner H, Uchtmann H. Depth profiles of fluoride interactions in hyperfine subsurface layers of dental enamel. Fresenius Z Anal Chem. 1987;327:484-490.
10. Garcia-Godoy F, Gwinnett AJ. Effect of etching times and mechanical pretreatment on the enamel of primary teeth: An SEM study. Am J Dent. 1991;14:115-118.
11. Ripa LW, Gwinnett AJ, Buonocore MG. The "prismless" outer layer of deciduous and permanent enamel. Arch Oral Biol. 1966;11:41-48.
12. Croll TP. Bonded resin sealant for smooth enamel defects: New concepts in "microrestorative" dentistry. Quintessence Int. 1987;18:5-10.
About the Author
Theodore P. Croll, DDS
Private Practice, Pediatric Dentistry
Doylestown, Pennsylvania
Affiliate Professor
Department of Pediatric Dentistry
University of Washington School of Dentistry
Adjunct Professor
Department of Pediatric Dentistry
University of Texas Health Science Center at San Antonio, Dental School
Kevin J. Donly, DDS, MS
Professor and Chair
Department of Pediatric Dentistry
University of Texas Health Science Center at San Antonio, Dental School