Clinical Use of a Seventh-Generation Bonding Agent
Leonard A. Hess
Quick considerations for treatment success.
One of the most exciting aspects of practicing clinical dentistry is to bear witness to improvements and breakthroughs. Faster, better, stronger, easier, and longer-lasting products are always being developed and demanded. Stagnation seems impossible in most state-of-the-art practices.
Clinicians demand a lot from their bonding agents. Desired qualities include high bond strengths to both dentin and enamel, improved marginal sealing, and a fast and convenient application system. Postoperative sensitivity and technique consistency are two additional issues of long standing contention. Evidence seems to point toward unsealed tubules as a major contributing factor in sensitivity.1 The more steps required to properly bond increases the time and money needed. This can often lead to lack of consistency and failure to follow strict manufacturer protocols. Thankfully, as bonding products have continued to improve, their results have included less clinical steps and better dentinal sealing.
Dentinal bonding started to be feasible in the 1950s and 1960s. Although possible, the clinical realities were failures as bond strengths were nowhere near what would be necessary. Dentin is approximately 50% inorganic by volume against a 98% mineral content of enamel. The remaining 50% of dentin comprises water and collagen. Further complication is produced by the creation of the dentinal smear layer during the preparation. The smear layer leaves a generalized layer of dentin with occluded tubules. The true challenge becomes simultaneous bonding to “wet” dentin and “dry” enamel. Acid-etching allows for the removal of the smear layer exposing fresh denatured collagen. Proper dentinal bonding then becomes dependent upon not over- or under-etching the dentin. Furthermore, it is important not to over-dry the dentin. Loss of the dentinal integrity will hinder the ability of the primer to re-wet (re-expand the collagen) and the bonding agents’ ability to permeate deep into the tubules. When one considers everything that could go wrong and how often clinicians do get it right, the state of modern bonding becomes ever more impressive.
In the 1980s, the science began to catch its stride with the third- and fourth-generation bonding agents and their total-etch techniques. Improvement continued with fifth-generation, single-bottle agents (primer and bonding agent in one solution). Currently, the profession has seventh-generation bonding agents (all-in-one, self-etching) available in clinical armamentariums. These newer bonding agents serve four functions simultaneously as they are contained in a single-application liquid: they etch the tooth, prime the surface, bond, and desensitize. The seventh-generation bonding agents have been shown to be very effective in reducing post-treatment sensitivity.2,3 In addition, studies have shown their bond strength to be equal to or stronger than previous-generation bonding agents.4 The seventh-generation product highlighted in this article is iBOND Self-Etch (Heraeus, Armonk, NY).
The new iBOND Self-Etch has been extensively tested and refined to provide a high-quality product that is very user-friendly. An important factor to evaluate and consider is microtensile bond strengths to dentin and enamel. When compared to competitors’ products and previous-generation bonding agents, it was shown to be equal to and in many cases had stronger bond results.5,6 The same-category leading results were obtained when consideration was given to shear bond strength to dentin.7 When an iBOND Self-Etch restoration was thermocycled and mechanically loaded, the marginal integrity was shown to be stable and almost unchanged.8 When compared against 10 other leading bonding agents, iBOND Self-Etch had the highest average (one-step adhesive) shear bond strength at 14.39 MPa ± 4.5 MPa.9
The indications for the use of iBOND Self-Etch are as follows:
• Light-cured direct placement composite restorations (Figure 1 and Figure 2).
• Bonding of indirect (inlays, onlays, crowns, veneers) restorations in combination with a light-cured luting cement (Figure 3 and Figure 4).
• Treatment of localized hypersensitivity.
The use of iBOND Self-Etch is contraindicated with self-curing composites for luting agents. A significant reduction in bond strength could result in such a pairing. Steps should be taken to ensure that the chemistry of the product is fresh. The precautions would include proper storage (below room temperature), consistent and immediate sealing of the bottle after use, and use of dispensed product in less than 3 minutes. This author prefers single-dose packaging to ensure consistent chemistry upon opening. The bottle application should be briefly shaken before use and dispensing. The single-dose application should be opened immediately before application, and when removing the liquid, rotate the applicator tip or brush briefly in the single dose.
Upon completion of the preparation, verify that it is free of debris and other contaminates. Dispense a copious amount of iBOND Self-Etch to the preparation and marginal area and verify complete coverage of the area. The adhesive should be agitated over the surface area for 20 seconds to aid in demineralization and diffusion of the product. Air-dry the area for 5 to 10 seconds to evaporate the solvent. What should be left is an even and highly glossy surface which indicates complete cross-linking of the adhesive with the tooth surface (Figure 5 and Figure 6). If this has not been accomplished or isolated dull spots are visible, repeat the application process. The sealed preparation should then be light-cured for approximately 20 seconds. The area is then ready for direct placement of the light-cured restorative material. Indirect restorations would be bonded in a like fashion, being sure that the luting agent is a light-cured product. Always take steps to prevent contamination of the bonding zone from blood and saliva.
CONCLUSION
There is no replacement for sound clinical judgment and attention to details. No dental product, regardless of quality, can pardon errors created as a result of improper use or poor planning. Successful treatment is never an accident. Properly bonded restorations must start with the correct environment and healthy remaining tooth structure. Having scientific and quality-driven materials in your armamentarium will only make successful outcomes less stressful and more consistent.
DISCLOSURE
The author has received financial support from Heraeus Kulzer.
1. Christensen GJ. Self-etching primers are here. J Am Dent Assoc. 2001;132(7):1041-1043.
2. Turkun LE. The clinical performance of one and two step self-etching adhesive systems at one year. J Am Dent Assoc. 2005;136(5): 656-664.
3. Kaurani M, Bhagwat SV. Clinical evaluation of postoperative sensitivity in composite resin restorations using various liners. N Y State Dent J. 2007;73(2):23-29.
4. Kiremitci A, Yalcin F, Gokalp S. Bonding to enamel and dentin using self etching adhesive systems. Quintessence Int. 2004;35(5):367-370.
5. Frankenberger R, Nikolaenko S. Microtensile bond strength to dentin. University of Erlangen, Germany. Manufacturer in vitro study.
6. Van Meerbeek B. Microtensile bond strength on enamel and dentin. University of Leuven, Belgium. Manufacturer in vitro study.
7. Shear bond strength and marginal adaptation to dentin. Research and development in vitro study. Heraeus Kulzer. Wehrheim, Germany.
8. Haller B. Marginal integrity at the enamel and dentin. University Hospital Ulm, Germany. Manufacturer in vitro study.
9. Degrange M. Battle of the bond shear bond strength. Biomaterials Laboratory, University of Paris, France. Manufacturer in vitro study.
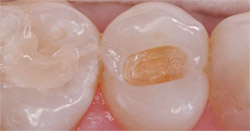 | 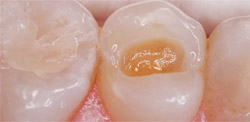 |
| Figure 1 Preoperative view of a direct resin preparation. | Figure 2 Direct resin preparation after application of iBOND Self-Etch bonding agent. Note the glossy appearance of the dentin. |
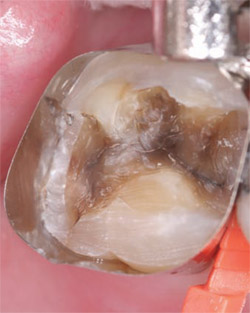 | 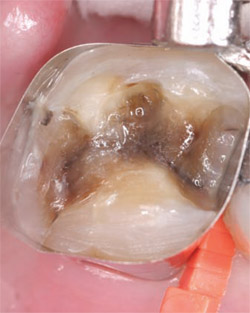 |
| Figure 3 A typical restorative situation involving a needed core build-up after alloy and decay removal. | Figure 4 iBOND Self-Etch has been applied to the area for 20 seconds. Notice the highly glossy surface indicating complete cross-linking of adhesive with the tooth surface. |
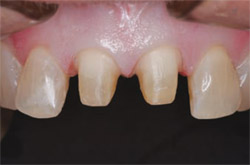 | 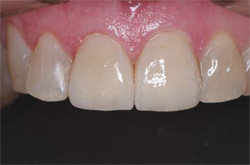 |
| Figure 5 Indirect restorative preparations that have been properly cleaned with an oil- and fluoride- free cleaning agent before the application of iBOND Self-Etch. | Figure 6 Indirect porcelain crowns immediately following bonding with iBOND Self-Etch and a light-cured luting resin. |
| About the Author | |
 | Leonard A. Hess, DDS Private Practice Monroe, North Carolina |



