Treatment Planning Materials, ToothReduction, and Margin Placement for Anterior Indirect Esthetic Restorations
Frank M. Spear, DDS, MSD
The restorative dentist on the interdisciplinary team is tasked with determining which teeth need to be restored. This includes treatment planning the restorations, including what materials will be used, how the teeth will be prepared, and where the margins will be placed. Ultimately these decisions impact several other team members and how their respective treatments will be performed. For example, to treat a patient with worn and overerupted anterior teeth, crown lengthening or orthodontic intrusion might be chosen as methods for altering the gingival levels to correct the esthetics.1-3
If the restorative dentist believes that the teeth could be restored with conservative veneers, it might be preferable to use intrusion to move the gingival levels because it would allow the cervical margins of the veneers to be placed on enamel rather than on cementum. However, if the dentist chooses some type of cemented crown as the restorative option, crown lengthening may be a quicker and perfectly acceptable option because the cemented crown would have similar predicta-bility whether the cervical margin was on enamel or cementum.
Another example would be the restoration of a peg-shaped lateral incisor. If the restorative dentist decides a restoration such as a bonded crown might be the best choice, then it is preferable for the orthodontist to position the peg-shaped lateral out of occlusion with lingual clearance so that the restorative dentist does not have to prepare the lingual of a tooth that is already small. If, however, the restorative dentist chooses a conservative veneer that does not cover the lingual surface, then the orthodontist would position the peg-shaped lateral with occlusal contact on the lingual because no restoration will be used to cover the lingual surface. One can see from these examples that how a tooth is restored is critical to how the treatment is planned.
Choosing a method of restoration and a restorative material comes down to evaluating several different parameters. These include the condition of the existing tooth, the color of the existing tooth, the position of the tooth in the mouth (anterior vs posterior), the esthetic desires of the patient, and the skills and preferences of the laboratory technician doing the restoration.4,5 One of the more frequent questions I am asked as an educator is, “What material should I use on a particular patient?” The truth is, there is no one right answer. It very much depends on the variables described above, and even then, several different materials may be acceptable.
Having said that, it is important to impart this author’s basic philosophy of treatment planning: all teeth should be restored with the most conservative restoration that satisfies the patient’s esthetic and functional requirements. That means that although a full crown or an aggressive reverse three quarters crown preparation might be esthetically acceptable, if a conservative veneer would be equally successful it should be the first choice.
Material Options
For the purpose of treatment planning and choosing a material, the author prefers to categorize materials into 2 large groups. One group consists of materials that are homogenous in composition, meaning uniform in structure throughout, and the other group consists of heterogenous ma-terials, meaning they differ structurally from inside to outside Figure 1).
Examples of homogenous materials would be powder and liquid ceramics fabricated on refractory dies or platinum foil, or pressable ceramics. Examples of heterogenous materials would be anything that uses a high-strength core with a different material fired on its surface, such as metal ceramics and a variety of nonmetallic restorations using alumina, zirconia, or lithium disilicate as high-strength core materials. As a general rule, the homogenous vs heterogenous groups have distinctly different properties in several areas. For tooth reduction, the homogenous materials can be used with less reduction than the nonhomogenous materials. Optically, homogenous materials often can be fabricated with greater translucence than can heterogenous materials. This is why homogenous restorations must be bonded to improve their predictability vs the heterogenous restorations that can be cemented in place or bonded without significant differences in performance.6-9
Because of these differences, most heterogenous materials are used as traditional full crowns or bridge restorations, while homogenous restorations can be used as full crowns but are particularly useful for more conservative bonded restorations.
Ultimately the material is chosen based on the needs of the tooth being restored. For the purposes of simplicity, the author likes to think of restorations as fitting into four major categories on anterior teeth: Those that replace primarily enamel, those that replace enamel and dentin but are not full crown, traditional full crowns that have normal-colored dentin, and full crowns with discolored dentin or metal posts that must be covered.
Identifying which one of these situations exists will determine what material to choose, how much of the tooth needs to be reduced, and where the margin will be placed.
Enamel Replacement
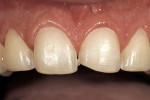
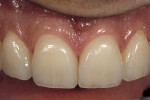
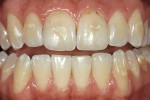
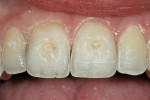
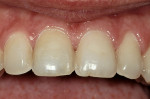
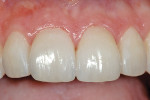
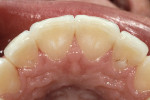
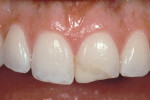
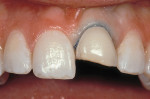
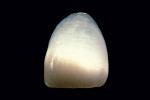
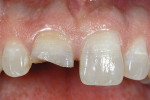
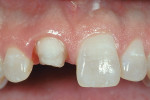
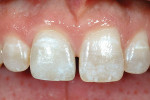
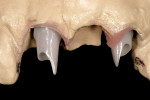
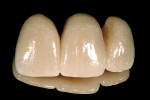
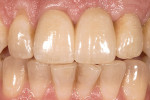
The most conservative of all anterior indirect restorations is the one that essentially replaces enamel with minimal, if any, preparation into dentin. These restorations are useful when the overall tooth color is pleasing and the goal of the restoration is to place a new, more pleasing external surface on the tooth. This type of restoration also can be used to alter tooth shape easily when the need to change the color of the tooth is minimal.10,11 Tooth reduction for enamel replacement is minimal but depends on the skills of the technician and the material chosen. The enamel thickness of a natural tooth varies from 0.4 mm on the facial in the cervical third, to 0.8 mm to 1 mm on the facial in the incisal third. Therefore, true enamel replacement restorations are typically 0.3 mm to 0.5 mm thick and require minimal preparation Figure 2;Figure 3;Figure 4).12
There has been a tremendous amount of marketing recently concerning no-preparation veneers, which fall under the category of enamel replacement, having the same limitation in changing tooth color dependent on the thickness of the porcelain. And while there may be some teeth where true no-preparation veneers are possible, physics is physics and adding material to the external surface of a tooth increases its bulk. If that bulk is acceptable because the tooth was small enough to begin with, then no preparation is possible. But in general, even for enamel replacement restorations, some tooth prep-aration is desirable and even needed to allow for ideal facial contours.13,14
For the thickness of porcelain used for enamel replacement, homogenous materials are the only options, either powder and liquid ceramics or ultrathin pressed restorations. In general, the powder- and liquid-based restorations have the advantage of being able to be fabricated with less thickness, can have variations in color built into the restoration without the necessity of any external stain, and, therefore, can be finished with a bur if necessary without removing any external color. The disadvantages of powder and liquid ceramics are that they are typically harder to fabricate than a pressable restoration, they may not fit as well, and in a laboratory setting they are not as strong.
Pressables have the advantages of easier fabrication, usually have a better fit, and have higher strength in a laboratory setting. Their disadvantages relate to color management. For these reasons, external color usually has to be applied to the ultra-thin pressed restoration to keep it from being monochromatic. The risk is that if any finishing or recontouring is done, this external color can be removed. Suffice it to say that different clinicians and technicians have been able to do enamel replacement using both powder and liquid ceramics and pressable ceramics with excellent results, the choice depending largely on the individual clinician and technician.
Margin placement is one of the big advantages of enamel replacement restorations. The same ultra-thin, highly trans-lucent ceramics that make changing color difficult with these restorations allow them to have supragingival margins placed that are invisible.14,15 It also allows margins to be placed interproximally and incisally without the need to carry the margin through the contact or over the incisal edge and down the lingual surface. In fact, in a clinical study where enamel replacement veneers were used and a comparison was done between covering the incisal edge and preparing the facial half of the incisal edge, leaving the lingual half enamel, there was no differences in the success seen at 3-year recalls.16 This is not to say that the incisal edge cannot be covered with enamel replacement restorations, but if the existing incisal edge position is pleasing, it is not necessary to reduce its length for these types of restorations Figure 5;Figure 6; Figure 7;Figure 8;Figure 9).
One might question why this type of restoration would be chosen over one that does a more aggressive tooth preparation and uses thicker ceramics but is easier to fabricate. There are several reasons to choose the more conservative approach. It is known that as the facial enamel is removed from an anterior tooth, it becomes more flexible under loading, illustrating that the enamel provided the primary rigidity to the tooth.17-19 By leaving as much enamel as possible, a more rigid foundation is maintained to which ceramics can be bonded. This ultimately results in less stress being applied to the bond under function because the stresses of flexion always end up accumulating at the junction between materials of differing rigidities. In addition, enamel is a highly predictable and durable substance to which to bond, so bonds are very technique insensitive. Also, because minimal dentin is exposed, the risk of sensitivity is almost nonexistent. Finally, just as occlusal caries in a posterior tooth is treated with an occlusal restoration, not a mesial-occlusal-distal restoration or a crown, it only makes sense, when possible, to perform the most conservative anterior restorations.
Dentin and Enamel Replacement
As desirable as the conservative nature of enamel replacement restorations may be, many defects of the anterior teeth simply cannot be treated with as minimal a preparation as the enamel replacement previously described. Common situations such as large interproximal Class III composites, malposition, discoloration, wear, or fractures may necessitate a restoration that removes more of the tooth but does not necessitate the preparation of a classic full crown.20 When both dentin and enamel will be replaced but the restoration is not a traditional crown preparation, the homogenous materials are still the materials of choice. The difference being that, unlike enamel replacement restorations, there now will be adequate room to create a brighter, more reflective layer internally with a more translucent layer over the surface.
The actual amount of reduction required will be strongly related to the amount of tooth malposition, the existing restorations present, and the amount of color change desired.12 The more rotated or labially positioned a tooth is, the more it requires heavier reduction. The larger the existing restorations, the greater the need to carry the restoration onto sound tooth structure, and the more color change desired in the final restoration compared to the existing tooth, the greater the facial reduction will need to be made.
In addition, if radical changes in color or tooth position are desired, it may frequently be necessary to carry the restorations through the interproximal, part way down the lingual, or perhaps subgingivally. The reason for not giving specific amounts of reduction is that the presenting clinical situation, material chosen, and demands of the laboratory technician will all impact the amount and location of tooth reduction. In addition, when correcting mal-aligned teeth, it is not uncommon to have varying thicknesses of material on different teeth in the arch because of position.
With regard to the differences between the homogenous materials used for dentin and enamel replacement, powder and liquid ceramics or pressed ceramics, the same issues as described earlier exist concerning fabrication and fit.
There is one clinical situation, however, that highlights the differences in optical properties between the materials. That situation is the Class IV fracture or incisal fracture. The challenge of these types of fractures is to replace the opacity of the missing dentin because if a highly translucent material is used to restore the fracture, typically it will look grey compared to the natural, unfractured portion of the tooth.
When using powder and liquid ceramics, this problem is easily managed. An opacious dentin can be fired first to replace the missing dentin, then a translucent enamel can be fired over the opacious dentin and remaining cervical, resulting in a restoration that is opaque in its incisal portion and translucent cervically to allow the natural tooth color to show through. In fact, it is possible to do an enamel replacement preparation cervically because the opacious dentin is blocking the light incisally Figure 10;Figure 11;Figure 12;Figure 13).
Because pressable ceramics do not offer the ability to place opacity and translucency of such different levels in sections within the same restoration in thin sections, it is generally necessary to use a much heavier cervical reduction for a fractured tooth to provide the space the technician needs to manage the color. That is not to say the pressable would be inferior esthetically, just that it will require greater tooth reduction to accomplish the restoration.
An alternative is to use composite to replace the fractured segment, then do an ideal veneer preparation and final restoration with the veneer being bonded cervically to tooth structures and incisally to composite.21 My preference whenever possible, however, is to not introduce the variable of a restorative material with different flexural properties within the restoration.
The Traditional Full Crown on Normal-colored Dentin
Today one could easily ask the question: When is it appropriate to use a traditional crown on an anterior tooth as opposed to a porcelain bonded restoration? The line between the two is often simply a few millimeters of lingual enamel. In general, the four reasons to use a crown would be: one already exists and you are replacing it; structurally the tooth requires the lingual be prepared; the occlusion requires a significant change so that lingual coverage is necessary; or high-strength materials are being used.
The traditional crown preparation with normal-colored dentin is the one restoration where it may be difficult to decide whether to use the homogenous materials or the heterogenous ones, as both may work equally well. As a general rule, the decision will come down to tooth reduction, laboratory preference, and whether the clinician desires to cement or bond the restoration.
For teeth with normal-colored preparations, the homogenous materials offer the ability to be used with less reduction, typically 0.8 mm to 1 mm, invisible margins when supra- or equi-gingival, and a predictable bond to the restoration itself, because both powder and liquid ceramics and pressable ceramics are easily etched. This can be a particular advantage when an anterior tooth is fractured off significantly enough that a traditional cemented restoration might not have adequate resistance and retention to maintain the restoration in the long term.
This usually becomes a concern when there is less than 3 mm of tooth structure remaining after tooth preparation. In these cases, traditionally a build-up would be done to increase the preparation length and provide adequate resistance and retention form. Instead, by using a predictable bonded homogenous crown, as little as 2 mm of vertical tooth structure is probably adequate without any build-up Figure 14; Figure 15; Figure 16).22,23 That is not to say that one cannot bond to the internal of the heterogenous crown but, in general, etched ceramic is far easier and more predictable to bond to than alumina, zirconia, or metal.
When adequate preparation length exists, however, cementing a heterogenous crown is a simple procedure that often requires less time with little risk of sensitivity. The question, of course, becomes: Which heterogenous system to use?
To answer that it is necessary to describe their differences. Basically all heterogenous restorations are created by first fabricating a high-strength core out of a variety of materials, and then firing a ceramic over it that is matched to the coefficient of thermal expansion of the core. So it is really the differences in core material that is at the heart of the differences in the various heterogenous systems.
The oldest of the heterogenous systems would be metal ceramics, whether cast, electroplated, or formed, such as Captek™ (a division of Precious Chemicals Inc, Altamonte Springs, FL).24-27 These cores have the properties of being the strongest of all the heterogenous systems, but also the most opaque. It is the property of translucency that makes the homogenous materials so attractive to use on normal-colored, full-crown preparations. And, it is the lack of translucency that makes metal ceramics so difficult to use on normal-colored, full-crown preparations. In fact, today, on normal-colored anterior preparations, the author would rarely choose metal ceramics unless he felt that the patient was at a high risk for fracture from severe bruxism.
The next oldest of the currently used heterogenous core systems would be those using alumina to produce the core. Products such as Vita In-Ceram® (Vident™, Brea, CA) or Procera® (Nobel Biocare™ USA, Inc, Yorba Linda, CA) are systems that use alumina.28-30 These restorations have the advantage of being strong enough to be attractive alternatives to the homogenous systems on normal-colored preparations. Most alumina products can be made with varying levels of translucency that allows them to be used on preparations of different shades.31-33 The more ideal the preparation color, the more translucent the core can be made.
The darker the shade of the preparation, the less translucent the core should be. This property of variable translucence allows the alumina-cored system to have a very broad range of anterior applications and margin placement. When used on normal-colored teeth with a translucent core, the margins can be kept supragingival. When used on dark prep-arations and with a more opaque core, the margins generally need to be placed subgingivally to hide them esthetically. The alumina systems, however, cannot be made as translucent as a pure homogenous system.
Perhaps the most translucent of all of the heterogenous systems would be those using a core of lithium disilicate, such asIPS Empress® (Ivoclar Vivadent®, Inc, Amherst, NY) or OPC® 3G (Jeneric/Pentron® Laboratory Technologies, LLC, Wallingford, CT).34,35 These restorations, in fact, can come close to the translucency of the homogenous systems. The trade-off is that the cores are weaker than most of the other heterogenous systems. This requires them to have fairly heavy tooth reduction to create a thick enough core to provide strength. So although they can be produced with similar translucency to a homogenous system, the homogenous restoration can be produced with far less tooth reduction. Because of their high level of translucency, the lithium disilicate systems can be used with supragingival margins on normal-colored preparations. Perhaps the biggest esthetic weakness of the lithium disilicate systems is that when they are used on extremely discolored preparations, their high degree of translucency often is not able to mask the dark preparation.
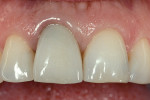
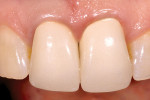
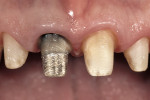
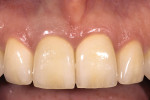
The newest member of the heterogenous family would be those produced from zirconia or zirconium oxide, such as Lava™ All-Ceramic system (3M ESPE, St. Paul, MN) and Cercon® (DENTSPLY Prosthetics, York, PA).36-39 There are large variations in physical and optical properties between the zirconia-based products on the market that are beyond the scope of this article but, in general, all zirconia-based restorations are the strongest of the nonmetallic heterogenous systems. Strength makes zirconia an ideal candidate for implant-supported restorations Figure 17; Figure 18; Figure 19; Figure 20). However, most zirconia frameworks tend to be opaque because of the density of the zirconia cores.
There are some exceptions to this. Lava has the ability to be fabricated with cores that are either quite opaque or moderately translucent, thus it can be used in its more translucent form on normal-colored preparations, or in its in more opaque form on dark preparations.
Most zirconia systems, however, are quite dense and opaque, which makes them far more difficult to use and get excellent anterior esthetics when compared to the homogenous materials or heterogenous restorations fabricated from alumina or lithium disilicate. This density of core also means that, in general, zirconia-based restorations will need to have their margins placed subgingivally for pleasing esthetics. In addition, it is typically necessary to have 0.7 mm to 0.9 mm of ceramic over any opaque core to get the appearance of depth and translucency in the final restoration. If the core also requires a thickness of 0.5 mm, which many do, this means a facial reduction of 1.2 mm to 1.4 mm is necessary to achieve good esthetics.
The other more translucent systems discussed often require 1 mm or less of reduction and have margins that can be placed supragingivally when used on normal-colored preparations. For these reasons most of the zirconia-based systems would not be the author’s first choice when choosing a material for a normal-colored preparation.
The Discolored Full-Crown Preparation
The highly discolored, anterior full-crown preparation presents a difficult esthetic challenge. It will now be necessary to use a restorative technique capable of recreating the normal reflectance of natural dentin and then overlay it with a more translucent material to provide a pleasing final appearance.
To achieve this, several approaches have been advocated.40-43 When using homogenous systems that have the most potential to be adversely affected by the dark preparation, several authors have advocated masking the preparation with an opaque composite and using an opaque cement but still using a relatively translucent restoration.
This can be successful, but it is often the least predictable way to approach the problem, the challenge being that there is no way to see the final color until the restoration is cemented to place. This becomes very difficult for the technician who then must try and guess what impact the preparation color and cement will have on the final color Figure 21 and Figure 22). A far more predictable approach is to use a crown that is more opaque from the beginning and, therefore, less affected by preparation color.44,45 The homogenous materials can be used for this, but the heterogenous materials with more opaque cores are a perfect fit on discolored preparations. This would mean alumina- or zirconia-based systems or even metal ceramics. Now the technician will see the color in the laboratory as it will be seen in the mouth because preparation color will have little to no impact on the seated restoration. Suffice it to say that when these more opaque restorations are used, a facial reduction of 1.2 mm to 1.4 mm will be necessary, and subgingival margins almost have to be used to avoiding having very unesthetic cervical areas. These same materials used to cover discolored preparations also are the materials of choice to cover a metal post and core that cannot be removed Figure 23; Figure 24; Figure 25).
What have been described here are the possible styles of restoration: enamel replacement, dentin and enamel replacement, full crown with normal color preparations, and full crown with a discolored preparation. It becomes obvious that the requirements for optical properties, tooth reduction, margin placement, and method of placement (bonded vs cemented) will vary for the different situations. Is there a single material that can be used for all of these situations? The closest would be the homogenous systems—powder and liquid ceramics or pressed ceramics. They can be used successfully on all of the restorations described in this article, but they do require bonding and will have the most difficulty when covering extremely discolored teeth.
How is the choice ultimately made? More than any other factor, it is based on what your laboratory does well in each situation. For enamel replacement and dentin and enamel replacement, you will choose from the homogenous family (again, powder and liquid ceramics or pressed ceramics) and then prepare the teeth and place the margin based on the material being used and the technician being used. For normal-colored full crowns the same homogenous material may be used, or if cement is preferred, one of the more translucent heterogenous restorations described could be chosen. Which one? The one with which the technician gets the best result. And for the highly discolored, full-crown preparations, one of the homogenous systems or one of the more opaque-cored heterogenous groups can be used. Again, the choice is made and the tooth is prepared based on the material requirements and the technician being used.
The one area not discussed in this article was using strength as a deciding factor in choosing a restoration for anterior teeth. The reason for that is simple. Although there are definite variations in strength among materials, there are minimal if any variation in their clinical success rates when used on anterior teeth.46-52 And while these variations in strength do show up in clinical studies when used on posterior teeth or bridges, even the weakest materials, the powder and liquid ceramics, have an excellent success rate when used on anterior teeth. In fact, all of the other materials, regardless of the strength of their core, are basically veneered with a material similar in strength to the powder and liquid ceramics materials. For these reasons, in the anterior the author chooses materials for their esthetic properties, while in the posterior he chooses them primarily for their strength, because most clinical studies will show a 7 to 10 times higher failure rate for molar all-ceramic restorations compared to anterior restorations fabricated from the same materials.
Conclusion
There is no one type of universal anterior restoration. It becomes necessary to evaluate each tooth and determine what type of restoration is most appropriate. The material used to complete each restoration should be chosen based on the technical support. And, finally, reduce the tooth and place the margins in the most conservative way that accomplishes the goals of the treatment.
References
1. Kokich VG. Esthetics: The orthodontic-periodontic restorative connection. Semin Orthod. 1996;2(1):21-30.
2. Chiche G, Kokich VG, Caudill R. Diagnosis and treatment planning of esthetic problems. In: Chiche G, Pinault A, eds. Esthetics of Anterior Fixed Prosthodontics. Chicago: Quintessence. 1994:35-52.
3. Rufenacht CR. Principles of Esthetic Integration. Quintessence Publishing Co. Ltd. 2000.
4. Garber D, Adar P, Goldstein R, et al. The quest for the all-ceramic restoration. Quint Dent Tech. 2000;23:27-36.
5. Touati B, Miara P, Nathanson D. Esthetic Dentistry and Ceramic Restorations. Martin Dunitz Ltd. 1999.
6. Pospiech P. All-ceramic crowns: bonding or cementing? Clin Oral Investig. 2002;6(4): 189-197.
7. Sobrinho LC, Cattell MJ, Knowles JC. Fracture strength of all-ceramic crowns. J Mater Sci Mater Med. 1998;9(10):555-559.
8. Malament KA, Socransky SS, Thompson V, et al. Survival of glass-ceramic materials and involved clinical risk: variables affecting long- term survival. Pract Proced Aesthet Dent. 2003;Suppl:5-11.
9. Potiket N, Chiche G, Finger IM. In vitro fracture strength of teeth restored with different all-ceramic crown systems. J Prosthet Dent. 2004;92(5):491-495.
10. Belser UC, Magne P, Magne M. Ceramic laminate veneers: continuous evolution of indications. J Esthet Dent. 1997;9(4):197-207.
11. Gurel G. The Science and Art of Porcelain Laminate Veneers. Quintessence Publishing Co. Ltd. 2003.
12. Ferrari M, Patroni S, Balleri P. Measurement of enamel thickness in relation to reduction for etched laminate veneers. Int J Periodontics Restorative Dent. 1992;12(5):407-413.
13. Garber DA. Porcelain laminate veneers-to prepare or not to prepare? Compend Cont Educ Dent. 1991;12(3):178-182.
14. Garber DA. Rational tooth preparation for porcelain laminate veneers. Compend Cont Educ Dent. 1991;12(5):316-320.
15. Materdomini D, Friedman MJ. The contact lens effect: enhancing porcelain veneer esthetics. J Esthet Dent. 1995;7(3):99-103.
16. Magne P, Douglas WH. Additive contour of porcelain veneers: a key element in enamel preservation, adhesion, and esthetics for aging dentition. J Adhes Dent. 1999;1(1):81-92.
17. Karlsson S, Landahl I, Stegersjo G, et al. A clinical evaluation of ceramic laminate veneers. Intl J of Pros. 1992;5(5)447-451:.
18. Magne P, Douglas WH. Porcelain veneers: dentin bonding optimization and biomimetic recovery of the crown. Int J Prosthodont. 1999;12(2): 111-121.
19. Magne P, Douglas WH. Cumulative effects of successive restorative procedures on anterior crown flexure: intact versus veneered incisors. Quintessence Int. 2000;31(1):5-18.
20. Magne P, Versluis A, Douglas WH. Rationalization of incisor shape: experimental-numerical analysis. J Prosthet Dent. 1999;81:345-355.
21. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Quintessence Publishing Co. Inc. 1994;5:97-113.
22. Magne M, Douglas W. Interdental design of porcelain veneers in the presence of composite fillings: finite element analysis of composite shrinkage and thermal stress. Int J Prosthodont. 2000;13(2):117-124.
23. el-Mowafy OM, Fenton AH, Forrester N, et al. Retention of metal ceramic crowns cemented with resin cements: effects of preparation taper and height. J Prosthet Dent. 1996;76(5):524-529.
24. Browning WD, Nelson SK, Cibirka R, et al. Comparison of luting cements for minimally retentive crown preparations. Quintessence Int. 2002;33(2): 95-100.
25. Abbott SJ. Metal-ceramic restorations. J Prosthet Dent. 1978;39(3): 293-294.
26. Loges H, Staegemann G. Metal-ceramic results after a 10-year observation period. Stomatol DDR. 1980;30(6):389-397. In German.
27. Nash RW, Radz GM. An esthetic alternative to conventional porcelain-fused-to-metal crowns. Compend Contin Educ Dent. 1997; 18(12):1160-1163.
28. Shoher I. Vital tooth esthetics in Captek restorations. Dent Clin North Am. 1998; 42(4):713-718.
29. Dickinson AJ, Moore BK, Harris RK, et al. A comparative study of the strength of aluminous porcelain and all-ceramic crowns. J Prosthet Dent. 1989;61(3):297-304.
30. McLean JW, Jeansonne EE, Bruggers H, et al. A new metal-ceramic crown. J Prosthet Dent. 1978;40(3):273-287.
31. Fradeani M, D’Amelio M, Redemagni M, et al. Five-year follow-up with Procera all-ceramic crowns. Quintessence Int. 2005;36(2): 105-113.
32. Koutayas SO, Kakaboura A, Hussein A, et al. Colorimetric evaluation of the influence of five different restorative materials on the color of veneered densely sintered alumina. J Esthet Restor Dent. 2003;15(6):353-360.
33. Devigus A, Lombardi G. Shading Vita In-ceram YZ substructures: influence on value and chroma, part II. Int J Comput Dent. 2004;7(4):379-388.
34. Devigus A, Lombardi G. Shading Vita YZ substructures: influence on value and chroma, part I. Int J Comput Dent. 2004;7(3):293-301.
35. Drummond JL, King TJ, Bapna MS, et al. Mechanical property evaluation of pressable restorative ceramics. Dent Mater. 2000;16(3):226-233.
36. Nagai T, Kawamoto Y, Kakehashi Y, et al. Adhesive bonding of a lithium disilicate ceramic material with resin-based luting agents. J Oral Rehabil. 2005;32(8): 598-605.
37. Blatz MB, Sadan A, Kern M. Ceramic restorations. Compend Contin Educ Dent. 2004;25(6): 412-416.
38. Suttor D. Lava zirconia crowns and bridges. Int J Comput Dent. 2004;7(1): 67-76.
39. Leinfelder KF, Kurdziolek SM. Contemporary CAD/CAM technologies: the evolution of a restorative system. Pract Proced Aesthet Dent. 2004;16(3): 224-231.
40. McLaren EA, Terry DA. CAD/CAM systems, materials, and clinical guidelines for all-ceramic crowns and fixed partial dentures. Compend Contin Educ Dent. 2002;23(7): 637-646.
41. Okuda WH. Using a modified subopaquing technique to treat highly discolored dentition. J Am Dent Assoc. 2000;131(7):945-950.
42. Nixon RL. Masking severely tetracycline-stained teeth with ceramic laminate veneers. Pract Periodontics Aesthet Dent. 1996;8(3): 227-235.
43. Baratieri LN, Coral Neto AC, Monteiro Jr S, et al. The sandwich technique, an alternative treatment for tetracycline-stained teeth: a case report. Quintessence Int. 1991;22(12):929-933.
44. Barath VS, Faber FJ, Westland S, et al. Spectrophotometric analysis of all-ceramic materials and their interaction with luting agents and different backgrounds. Adv Dent Res. 2003;17:55-60.
45. Rasetto FH, Driscoll CF, Prestipino V, et al. Light transmission through all-ceramic dental materials: a pilot study. J Prosthet Dent. 2004;91(5):441-446.
46. Heffernan MJ, Aquilino SA, Diaz-Arnold AM, et al. Relative translucency of six all-ceramic systems. Part II: core and veneer materials. J Prosthet Dent. 2002;88(1):10-15.
47. Haselton DR, Diaz-Arnold AM, Hillis SL. Clinical assessment of high-strength all-ceramic crowns. J Prosthet Dent. 2000; 83(4):396-401.
48. Oden A, Andersson M, Krystek-Ondracek I, et al. Five-year clinical evaluation of Procera AllCeram crowns. J Prosthet Dent. 1998; 80(4):450-456.
49. Probster L. Four year clinical study of glass-infiltrated, sintered alumina crowns. J Oral Rehabil. 1996;23(3):147-151.
50. Probster L. Survival rate of In-Ceram restorations. Int J Prosthodont. 1993;6(3):259-263.
51. Lehner C, Studer S, Brodbeck U. Short-term results of IPS-Empress full-porcelain crowns. J Prosthodont. 1997;6(1):20-30.
52. Segal BS. Retrospective assessment of 546 all-ceramic anterior and posterior crowns in a general practice. J Prosthet Dent. 2001;85(6):544-550.
This article was originally published in Advanced Esthetics and Interdisciplinary Dentistry, Vol 1, No 4, 2005.
About the Author
Frank M. Spear, DDS, MSD
Founder and Director
Seattle Institute for Advanced Dental Education
Seattle,Washington
Affiliate Assistant Professor
University ofWashington School of Dentistry
Seattle,Washington
Private Practice
Seattle,Washington