Splints Are Not Just for TMJ Therapy Part II: Fabrication Technique
Greg Vigoren, DDS; and Edward A. McLaren, DDS
Occlusal splints have been generally recommended for temporomandibular disorder (TMD) therapy and to mitigate the occlusal effects of bruxism. During bruxism, if posterior interferences (ie, protrusive, working, and balancing contacts) are present, the maxillary muscles exhibit significantly greater contractile force than when disclusion is guided by a single canine or maxillary central incisors during protrusion, whether it is a normal functional or a parafunctional movement.1 When only the canine or the incisors contact in lateral movement, there is a neurologic feedback mechanism that prevents excessive muscular contraction (the more teeth that contact the greater the possible contractile stress and thus muscular overload). Also, because the anterior teeth are farther from the fulcrum (the temporomandibular joint in this instance), there is a mechanical disadvantage relative to molars. This means the same contractile force in the maxillary muscles exerts proportionally less stress with respect to farther-anterior tooth contact. Combining all of these concepts: (1) fewer teeth in contact during excursions; (2) moving excursive contact farther to the anterior; and (3) creating canine disclusion in lateral movements—because the canine has the longest root and largest cross-sectional area of the anterior teeth which makes it more favorable to absorb lateral stress—has been one of the basic tenents of occlusal theory.2 These excessive uncontrolled forces generated by posterior interferences contribute to a multitude of problems and accelerated failure cycles. Excessive wear and joint problems, muscular issues, and tooth sensitivity all increase as a result of these excess forces. Recessions, fractures of all materials, and early marginal failure all increase under additional loads. Treatment options for malocclusion, including orthodontics with attention to functional occlusion, proper occlusal adjustment, and equilibration can aid in the prevention of these force-flex-failure issues, but a well-fabricated and well-adjusted splint can be an important treatment in preventing future problems.
The first part of this article covered the rationale for and potential uses of a splint and gave the tools necessary for successful patient education and motivation, as patient compliance is a mandatory part of long-term treatment outcomes.2 The objective of the second part of this article is to discuss the fabrication of a hard, durable, repairable, maxillary neutral splint/retainer. In the authors’ experience, this clear composite maxillary splint is very stable and rarely needs adjustment. It can be made in the office in an hour, but there are some important clinical considerations, including:
• Passive fit (no tooth movement or force on teeth) on the maxillary arch.
• Retention through close fit and 1 mm to 2 mm of buccal overhang (cuspid through second-to-the-last tooth).
• Neutral intercuspal (flat contact, no indentations) relationship in solid centric relation; adjust to neurologic/muscular release (free “clomp, clomp, clomp” sound).
• Mild cuspid rise and cuspid protection (posterior contacts are just spots, not slides).
Materials and Equipment
The composite splint featured in this article is fabricated out of a 2-mm thick light-cure composite tray/base material (Triad® TranSheet™ Colorless, DENTSPLY International, York, PA). It is cured in a Triad 2000™ Visible Light Curing Unit (DENTSPLY International) (Figure 1). Triad Model Release Agent (MRA, DENTSPLY Trubyte, York, PA) is the separating agent used for lubricating the cast that does not interfere with future additions or bonding. Add to this list any bonding liquid and brush, pigtail explorer, scalpel, your favorite laboratory acrylic bur, and articulating paper and you have all the necessary materials and equipment (Figure 2).
One of the strengths in this technique is that some of the steps associated with traditional splint techniques are not needed (eg, opposing mandibular impressions and casts, interocclusal jaw registration records, facebow transfer records, a sophisticated articulator or correlator). This is an in-office procedure, thus you do not need to send this out to a laboratory or wait for its return. There is no laboratory bill. This technique was first used in the authors’ practice 15 years ago in an emergency situation involving a patient needing a splint and leaving on an extended trip the next day. This first experimental use of this technique involved less time from start to finish than the normal adjusting time alone of the standard laboratory-processed acrylic splint that had been mounted on an articulator using a facebow and interocclusal records. Thousands have been successfully done using this technique since.
There are several significant differences and advantages between this splint technique and the more traditional laboratory technique. This type of splint is fabricated with no articulator; the patient and in-the-mouth adjustments replace this step. Therefore, no opposing impression, no opposing model, no interocclusal record and no facebow are necessary. The material is easy to use, easy to repair or modify, and, overall, less costly in both time and laboratory expense.
Technique
At the first patient visit, make a maxillary alginate impression with attention to lingual, occlusal, and incisal detail. You can use an alginate substitute like Penta™ Quick (3M ESPE, St. Paul, MN) or AlgiNot (Kerr Corporation, Orange, CA). The patient may then either wait for fabrication after the cast sets, return later that day, or come back for a separate appointment.
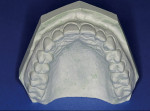
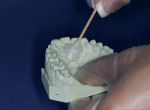
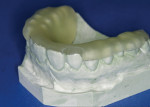
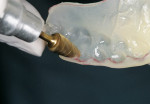
Pour the single maxillary impression in plaster or die stone with or without slurry and trim the cast appropriately (Figure 3). Lubricate the stone cast with MRA (Figure 4), then place a TranSheet on the maxillary cast and outline the final form with excess extending over the anteriors (Figure 5). Double up the anterior area in the TranSheet by folding under (Figure 6). Set the material back on the cast and cut the posterior relief, then cut off any excess material (Figure 7).
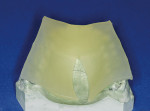
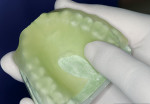
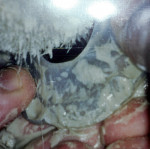
Using your fingers, press down the tray material without thinning it and form it to the cast Figure 8). Cut off any excess material at the incisal of the four anteriors and remove any excess material off the buccal of the most posterior molar, giving a 1-mm to 2-mm overhang on the facial of the cuspid to the first molar and a palatal outline form Figure 9). Light-cure in the oven for 30 seconds, tease the blank up and down, cure for an additional 30 seconds, and then remove from the cast (Figure 10). Light-cure for an additional 5 minutes off the cast (the color will change from a yellow tint to white) (Figure 11). Relieve the interior in the embrasure areas and along the facial flange of retention (facial overhang); this material shrinks lingually into the bulk of the material (Figure 12). Remove rough edges and smooth (Figure 13).
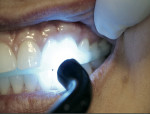
Return the patient to the chair. Fit the splint passively on the upper arch, relieve any tight or pressure points (Figure 14). Using a pencil, mark the mesial and distal of the lower cuspids on the upper splint. This allows you to identify/make a panographic tracing (mild cuspid rise) of the lower cuspids on the splint between these lines (Figure 15). Adjust the interarch occlusion; use articulation paper until even occlusion is achieved (multiple contacts/all teeth, only one per tooth is necessary in centric occlusion) Figure 16).
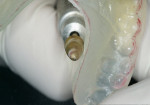
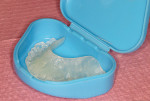
Reline the buccal overhang with a small amount of bonding liquid and a 1-mm roll of splint composite material (this is the only retention feature necessary). Seat the splint and have the patient bite down with force, remove the excess with an explorer, and then set up the reline material with the light source (Figure 17 andFigure 18). Remove the splint from the mouth; trim, smooth, and polish (Figure 19). Return to the mouth and finalize occlusal contacts, make posterior spots as small as possible; remember, they are points on a flat surface, not slides or indentations. Deliver the splint to the patient with instructions, reinforcement, homecare, and in an orthodontic retainer case (Figure 20).
Discussion
This two-part article presented a simplified, in-office splint technique and the associated philosophy of use that addresses many of the concerns over splint use. The verbal skills necessary to motivate patients to use this valuable adjunctive procedure were covered in Part 1. The technique demonstrated in Part 2 makes it simple to fabricate a well-fitting, occlusally well-adjusted appliance that, in the authors’ experience, overcomes most of reasons for lack of acceptance or lack of compliance in using a splint.
References
1. Williamson EH. The role of craniomandibular dysfunction in orthodontic diagnosis and treatment planning. Dent Clin North Am. 1983;27(3):541-560.
2. Vigoren G, McLaren EA. Splints are not just for TMD therapy. Inside Dentistry. 2007;3(10):92-94.
About the Authors
Greg Vigoren, DDS
Private Practice
Newport Beach, California
Adjunct Faculty
UCLA Center for Esthetic Dentistry
Los Angeles, California
Edward A. McLaren, DDS
Director
Center for Esthetic Dentistry
Founder and Director
UCLA Master Dental Ceramist Program
Adjunct Associate Professor
UCLA School of Dentistry
Los Angeles, California
Private Practice limited to Prosthodontics and Esthetic Dentistry