Small Diameter Implants Combined with Laser Therapy—a Case History
Jon Julian, DDS
Dental literature and prominent speakers in the dental industry have suggested that any implant surgery is likely to result in the loss of 0.75 mm to 2 mm in vertical height of soft tissue architecture.1-3 This results in a change of tissue height and a tendency toward show-through of the abutment (a graying at the cervical line). This is because of trauma from surgery and micro-movement of the abutment, resulting in a circumferential loss of bone of 0.75 mm to 1 mm in width, typically down to the first thread of the implant (cratering).4-6 Thus, as the bone is reduced in volume, it does not support the tissue as well over time and esthetics suffer.7-10 While this is not to suggest failure of the implant, it is certainly not desirable.
In the case described in this article, soft tissue grafting was part of the primary treatment plan and yet was not required because of the body’s physiologic response to laser incisions, as well as the bony response to the implant design and function.
CASE PRESENTATION
Pretreatment History
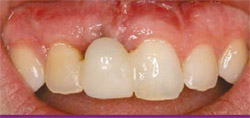
The patient, a healthy 26-year-old woman with a history of tooth loss on tooth No. 8, presented for an initial consultation. She had a previous implant placed at age 16 (4.5-mm x 16-mm straight cylinder). Over the next few years, she noticed that the implant-supported tooth became a different length than the rest of her natural teeth. She was unhappy with the esthetic result and was concerned about the appearance of the gum tissue above the implant-supported crown (Figure 1 and Figure 2).
The diagnosis was a potentially failing implant. The diagnosis of failing in this scenario means that the soft tissue architecture had deteriorated to the extent of total loss of keratinized tissue on the facial aspect, and a fenestration existed in the remaining soft tissue facially. In addition, a deficiency existed in the soft tissue lingually. Hard tissue architecture had deteriorated as well, with almost total loss of osseous tissue on the facial aspect of the implant. Although the implant was still integrated, it indeed was an esthetic failure and was losing osseous support, indicating probable functional failure in the future. Therefore, the decision was made to remove and retreat.
The author’s treatment plan was to remove the existing implant; perform an autogenous block graft to the same site, and, when this graft was stable, replace the previous implant with an implant of smaller diameter (3.5 mm x 11 mm) and length; perform a connective tissue graft to re-establish a healthy zone of keratinized tissue; and place an abutment and crown on tooth No. 8 and ceramic veneers on teeth Nos. 6, 7, and 9 through 11 to fulfill the patient’s desire for an improved esthetic appearance.
Treatment Planning
The treatment sequence began with an initial examination and consultation to interview the patient and discover her existing dental history, health history, and goals for future dental health. The author gathered records during this exam, including study models, panorex, bitewings, photographs, and a dental screening. The author then scheduled a hygiene appointment to do a thorough periodontal examination and, after that, a consultation appointment. During the consultation, the author informed the patient of appropriate treatment choices. She decided to proceed with removing and replacing the implant and, at the same time, undergo a bone-grafting procedure. She also chose to do a soft-tissue grafting procedure and have porcelain veneers placed on her anterior teeth. The author sent the models to a dental laboratory for construction of an idealized wax-up and a surgical stent.
First Surgical Appointment
To begin the next appointment the author delivered 3.6 ml of lidocaine 2% with epinephrine 1: 1000,000 as a mandibular block in the lower right quadrant and another 3.6 ml of lidocaine 2% with epinephrine 1:1,000,000 as infiltration anesthetic facially and lingually to teeth Nos. 6 through 11.
The author began the procedure by making a rectangular incision from the distal aspect of tooth No. 7 to the distal aspect of tooth No. 9 using a DEKA Ultraspeed CO2 laser (DEKA Laser Technologies, Ft. Lauderdale, FL) with a mirrored 100 ml handpiece at 4.5 watts at 80 Hz (Figure 3). After removing the crown from tooth No. 8, the author then reflected a full-thickness flap with blunt dissection to expose the implant. A 5-mm internal diameter trephine bur was used to cut to within 3 mm of the apex of the implant under copious irrigation. The author used surgical forceps to grasp and twist the implant and remove it (Figure 4) and then turned his attention to the mandibular right quadrant. By making a releasing incision anterior to tooth No. 30 and distally along the ramus distal of tooth No. 31, using the same CO2 laser and handpiece at a setting of 4.5 watts at 80 Hz, the author was able to reflect a full-thickness flap with blunt dissection to gain access to the retromolar area of the mandible. A 5.5-mm internal diameter trephine bur was used to cut a cylindrical block of bone from this area of the mandible. The mandibular incisions were closed with five interrupted sutures using 4-0 gut sutures.
The cylinder of autogenous bone was now positioned in the 5.5-mm diameter preparation site and secured with a single 8-mm screw (Figure 5). PepGen P-15 Particulate (DENTSPLY Friadent CeraMed, Lakewood, CO) were overlaid onto the block graft and covered with a barrier membrane, Gore Resolute Adapt (Gore Medical, Flagstaff, AZ). The full-thickness flap was re-approximated and sutured into place with one mattress suture and six interrupted sutures, all 4-0 gut. The author bonded an appropriate denture tooth to teeth Nos. 7 and 9 using composite resin, being careful not to contact the surgical site.
The author gave the patient postoperative instructions and an initial dose of analgesics, 2 tablets of 200 mg of Advil® (Wyeth Consumer Health Care, Madison, NJ) and 2 tablets of 250 mg of Tylenol® (McNeil Consumer Healthcare, Guelph, ON, Canada), with instructions to take further tablets together in a single dose as needed for pain and swelling every 4 to 6 hours. The author scheduled the patient for a postoperation appointment in 10 days.
During the follow-up phone call 24 hours after the procedure, the patient stated that she had little swelling, only took two more doses of the recommended analgesics, and was very comfortable.
At the 10-day follow-up appointment, the patient exhibited no evidence of swelling or inflammation and stated that she stopped taking the analgesics the day after the procedure (she had not taken anything for pain for the past 8 days).
Second Surgical Appointment
The patient returned after 4 months. At this appointment the author administered 3.6 ml of lidocaine 2% with epinephrine 1:100,000 in a facial and palatal infiltration from teeth Nos. 6 through 11. The author made a single vertical-releasing incision distal to tooth No. 7 and a horizontal incision mid-crest from teeth Nos. 7 through 9 (Note: the bonded denture tooth had been removed before this procedure). The same CO2 laser and handpiece were used at the same settings for the incisions.
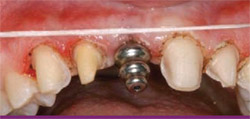
Blunt dissection created and released a triangular flap that exposed the graft site and the stabilizing screw, which was removed. Using the surgical stent, the author prepared the osteotomy site to receive a 3.5-mm x 11-mm ANKYLOS® implant (DENTSPLY Tulsa Dental Specialties, Tulsa, OK), positioned 2 mm to 3 mm below the crest of the bone (Figure 6).
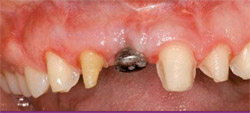
However, because some of the implant collar was visible upon insertion, a second addition of particulate graft material was considered. The author removed the internal sealing screw of the implant with a force of 6 Ncm and placed a balance posterior tissue former 3 mm in height. Then the author placed bone graft material (PepGen crystals combined with autogenous bone from the osteotomy site) over the collar and shoulder of the implant and closed the flap with one mattress suture and four interrupted sutures, all 4-0 gut (Figure 7). Note: due to the 2.5-mm diameter of the tissue former at the insertion site into the 3.5-mm body of the implant, a natural reservoir or retention area is formed that encourages stability of the grafted particles—therefore, no barrier membrane was used.
At this stage of healing, before making the incision, the author observed that keratinized tissue was reforming without intent or interference; therefore, he decided to postpone that phase of treatment (soft tissue grafting) to a later time if needed (Figure 8). The author prescribed the same analgesics as before and gave the initial dose at the appointment. However, this time the patient did not take any subsequent doses. The author took two periapical radiographs during the procedure (Figure 9) and bonded the denture tooth back into position with the same considerations and care as before (Figure 10).
Third Surgical Appointment
The patient returned after 3 more months. The author observed continued progression and maturation of a substantial zone of keratinized tissue facial and superior to the tissue former. He explained to the patient that his intent was to forgo the tissue-grafting procedure entirely unless the clinical situation deteriorated from its current state.
The author gave 3.6 ml of 2% lidocaine with epinephrine 1:1,000,000 in the same manner as before from teeth Nos. 6 to 11. The author prepared teeth Nos. 6 and 9 through 11 for porcelain veneers and tooth No. 7 for a full-coverage porcelain crown using a Samuri bur and a NEO Diamond round-end taper bur (Microcopy, Kennesaw, GA).
Using a 100-mm handpiece fitted with a perio insert on the same CO2 laser at a power of 3.7 watts at 80 Hz, the author performed tissue troughing around all the gingival margins of the prepared teeth. As CO2 energy is absorbed into water, instead of blood or hemoglobin, the energy leaves a dry field and clearly visible margins without danger of losing tissue height.
Next, the tissue former was removed and a standard ANKYLOS® repositioning post (impression coping) (DENTSPLY Friadent CeraMed, Lakewood, CO) (Figure 11) was placed. Aquasil™ (DENTSPLY Caulk, Milford, DE) light-bodied impression material was syringed around the tooth preparations and Aquasil medium-bodied material was syringed around the repositioning post in a stock tray. Upon completion of a successful impression and replacing of the tissue former, the author constructed temporary crowns combining Charisma® composite resin (Heraeus Kulzer, Armonk, NY) with VOCO Structur 2 QM (VOCO America, Sunnyside, NY). These were trimmed, polished, and seated with Provicol QM temporary cement (VOCO America) after appropriate shade matching was recorded. The author did not give the patient any analgesics for this appointment.
Seating Appointment
Four weeks later, the patient returned for her seating appointment. Again the author administered 3.6 ml lidocaine 2% with epinephrine 1:1,000,000 facially and palatally. The temporaries were removed and the prepared teeth were pumiced (Figure 12). The author removed the tissue former and placed the balance anterior abutment into position with a laboratory-manufactured jig (Arrowhead Dental Lab, Salt Lake City, UT). The author tightened the abutment with a torque wrench to 15 Ncm and cemented the crown on tooth No. 8 at this time using Rely X™ (3M ESPE, St. Paul, MN). The author cleaned the excess cement from tooth No. 8 and placed 35% phosphoric acid etchant (Ultradent, South Jordan, UT) on teeth Nos. 6, 7, and 9 through 11. After thorough rinsing, VOCO primer was placed and air-dried. Then VOCO bond was placed on all prepared teeth, and the crowns (Authentic Elite by Arrowhead Dental Lab) were bonded and light-cured into position. After finishing and polishing, the occlusion was checked and no adjustments were necessary (Figure 13).
At this stage the patient was pleased with her results and ready to be placed into a routine hygiene care program. The author discussed the remarkable resolution of the soft tissue dilemma and advised the patient that there was no further need to consider any type of soft tissue grafting at this time (Figure 14).
DISCUSSION
Many elements combined to make this a satisfying case that exceeded the patient’s expectations. First of all, by eliminating or significantly reducing inflammation and swelling, the patient experienced a more comfortable and positive outcome and the tissue healed without stressing the sutures. In using the CO2 lasers over the past 3 years, the author has observed little or no scaring of tissue postoperatively. The actual cut from a 100-mm mirrored handpiece is 30 µm in width, but appears wider as dehydration affects approximately another 60 µm, making the average incision appear to be 90 µm in width. Laser energy sterilizes as it cuts and seals off lymphatics, blood vessels, and nerves. Thus, there is no histamine release to trigger an inflammatory response and the pain associated is significantly reduced or elimin-ated. The energy is readily absorbed into the water component of tissue. Because the energy can be delivered in pulses of millionths of a second at energy levels of 0.2 watts to more than 6 watts, soft tissue can be effectively treated for apthous lesions at low levels. As the energy settings are raised, dentists can treat periodontal pockets, trough around crown preparations, and create incisions safely and rapidly through any tissue type. These are just a few of the practical uses. When the laser energy comes into contact with bone, it forms a char on the 0.1-mm surface of the bone (ie, the heat does not penetrate nor cause bone necrosis). As implants have no water in their surface, this laser energy is completely safe when it comes into contact with an implant body or abutment.
Even though this case was a complex, multi-surgery clinical situation, the patient did not experience any pain or swelling that could not be managed by over-the-counter medications. Suture lines were never stressed because of the minimized swelling. The author has experienced a dramatic reduction in prescription analgesics and/or steroid usage postsurgically in a majority of clinical cases. Finally, vision for the clinician during the surgeries is greatly enhanced because of the hemostatic effect of the laser energy. Reduced bleeding makes the clinician’s job simpler because the area being worked on can be seen more clearly.
In the author’s opinion, the second major success of this case was the use of an unusually engineered implant design. The ANKYLOS implant has an internal morse taper connection. At 5.8º of taper, and being perfectly round without any geometric shape to align the abutment (such as a triangle or hex, etc), the fit of the abutment is very intimate. This gives the effect of a strong friction-fit and symmetrical cone. It is anti-rotational and requires only 15 Ncm of force to torque the stabilizing screw. This creates a rigid-sealed connector that exhibits no micro-gap with the stability gained from the medullary bone. The implant body is ideally positioned 1 mm to 2 mm below the crest of the bone (and below the cortical plate). The progressive threading is more pronounced in the apical half of the implant, thus engaging the medullary bone for support.
Combining the strength of the conical connector and no apparent micro-gap with the stability gained from the medullary bone (which has good blood supply and therefore high reparative qualities) and placement below the cortical plate results in greater stability of the circumferential bone (ie, no cratering). Therefore, there is more support for the peri-implant soft tissue architecture. With this type of implant, the author was able to replace the 4.5-mm x 16-mm implant originally placed with a 3.5-mm x 11-mm implant and have greater strength in the connector, while removing a smaller volume of bone to accommodate the new implant and maintaining a greater volume of stable bone supporting a greater volume of soft tissue. This not only enhances the esthetic result but, in the author’s opinion, and in this particular case, it allowed the body to normalize the tissue type and health without surgical intervention. The 2.5-mm diameter that all abutments exhibit (no matter what diameter of implant is used, the abutment is 2.5 mm at the insertion point) encourages a greater volume of tissue to envelop the abutment crown complex. This biologic seal maintains tissue health and provides great esthetics by masking the abutment–crown interface.
CONCLUSION
This clinician feels that his skills in no way influenced this case because he has performed similar surgical procedures with cold steel and other implant systems, only to witness eventual, if not immediate, loss of tissue height. These surgical procedures also resulted in gray showing through at the cervical line, which does not necessarily mean failure, but does significantly affect the esthetic outcome. The clinician’s clinical judgment and skills certainly are important; his experience helped the bone grafting procedure to be successful. However, better tools and innovative engineering concepts converted this case from a salvaging situation to an ideal outcome.
DISCLOSURE
The author has received honoraria from Arrowhead Dental Lab and Deka Laser Technologies.
References
1. Berglundh T, Lindhe J. Dimension of the peri-implant mucosa. Biologic width revisited. J Clin Periodontol. 1996;23(10):971-973.2. Small PN, Tarnow DP. Gingival recession around implants: a 1-year longitudinal prospective study. Int J Oral Maxillofac Implants. 2000;15(4): 527-532.
3. Oates TW, West J, Jones J, et al. Long-term changes in soft tissue height on the facial surface of dental implants. Implant Dent. 2002;11(3): 272-279.
4. Hermann JS, Schoolfield JD, Schenk RK, et al. Influence of the size of the microgap on crestal bone changes around titanium implants. A histometric evaluation of unloaded non-submerged implants in the canine mandible. J Periodontol. 2001;72(10):1372-1383.
5. King GN, Hermann JS, Schoolfield JD, et al. Influence of the size of the microgap on crestal bone levels in non-submerged dental implants: a radiographic study in the canine mandible. J Periodontol. 2002;73(10):1111-1117.
6. Elian N, Jalbout ZN, Cho SC, et al. Realities and limitations in the management of the interdental papilla between implants: three case reports. Pract Proced Aesthet Dent. 2003;15(10):737-744.
7. Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol. 2000;71(4):546-549.
8. Choquet V, Hermans M, Adriaenssens P, et al. Clinical and radiographic evaluation of the papilla level adjacent to single-tooth dental implants. A retrospective study in the maxillary anterior region. J Periodontol. 2001;72(10):1364-1371.
9. Grunder U, Gracis S, Capelli M. Influence of the 3-D bone-to-implant relationship on esthetics. Int J Periodontics Restorative Dent. 2005;25(2):113-119.
10. Zetu L, Wang HL. Mangement of inter-dental/inter-implant papilla. J Clin Periodontol. 2005;32(7):831-839.
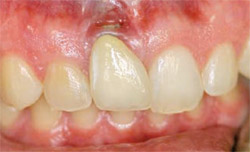 |  | |
| Figure 1 Patient at presentation and initial exam. | Figure 2 Radiograph of patient at presentation and initial exam. | |
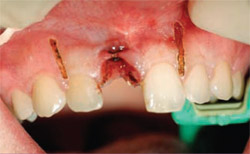 | 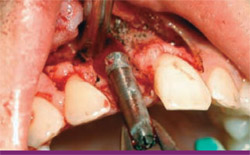 | |
| Figure 3 The CO2 laser incision gained access. | Figure 4 Removal of the implant body with forceps and trephine bur. | |
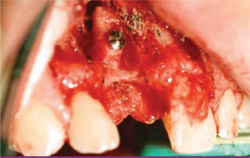 | 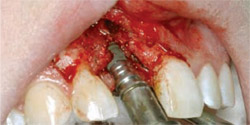 | |
| Figure 5 The cylindrical block graft intimately fits; it was secured with a single screw. | Figure 6 Placement of the ANKYLOS implant in a subcrestal position with slight exposure of facial collar. | |
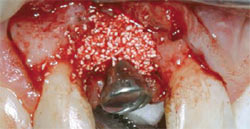 | 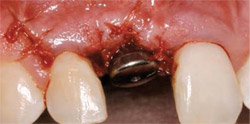 | |
| Figure 7 Tissue former in place with secondary tissue graft. | Figure 8 Note the zone of keratinized tissue developing above the surgical site. | |
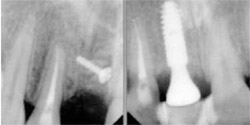 |  | |
| Figure 9 Pre- and posttreatment radiographs of the osteotomy site. | Figure 10 Temporization. | |
 |  | |
| Figure 11 Prepared teeth; laser trophing the implant impression post. | Figure 12 Preparing teeth for bonding. | |
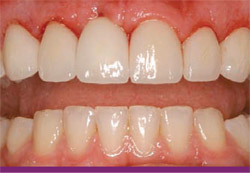 | 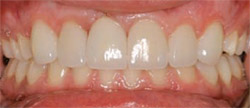 | |
| Figure 13 Immediate post insertion of Elite by Arrowhead Dental Lab. | Figure 14 Ninety-day follow-up shows complete resolution of tissue. The patient was very pleased with the outcome. | |
| About the Author | ||
 Jon Julian, DDS Jon Julian, DDSPrivate Practice McPherson, Kansas The Dr. Dick Barnes Group Sandy, Utah | ||




