The Art of Denture Relining
Karl F. Leinfelder, DDS, MS; Douglas A. Terry, DDS; and Mark E. Connelly, DDS
Mastering the art of complete or partial dentures requires developing a balance between function, comfort, and esthetics.1 Although the fabrication of complete denture prostheses is somewhat complex, requiring multiple detailed procedures, the result can be generally quite acceptable. Many times after prosthetic completion an imbalance in these three criteria can occur over time. Gradual physiologic changes of the soft tissues as well as resorption of the underlying osseous structure can cause the denture to lose its original stability and retention.2 Assuming that the occlusal and vertical dimensions of the denture are acceptable, it is possible to regain tissue adaptation and retention of the supporting structures by relining the denture base.
This can be achieved through an indirect technique in the laboratory or directly in the patient’s mouth. The indirect technique includes the generation of an impression, stone cast, and then applying new denture base material to the internal aspect of the denture. The direct method of denture relining is accomplished by means of making an intraoral impression within the denture using a chairside lining material that bonds to the inner surface of the denture.3-5
Each of these methods poses potential challenges. The indirect technique is performed in a laboratory with special curing equipment, which means that the patient must go without the denture for a period of time. Other concerns associated with the indirect technique include dimensional change (warping) in the denture base6,7 and potential errors in occlusion. However, conventional laboratory-processed liners exhibit a greater degree of material polymerization from elevated temperatures and pressures that suggest improved physical and mechanical properties of the materials.4 The direct lining method an be more patient-friendly and faster than the laboratory method; however, chairside relining systems in the past were characterized by technical shortcomings of the material. Challenges associated with these materials have included poor bonding of the reline material to the denture base; surface porosities that commonly lead to build-up of food stuffs and bacteria that can result in a bad odor; chemicaburns; heat generation; mucosal irritation; color instability; and an unpleasant taste.6-10 Finally, the intraoral lining method can be characterized by short-term longevity.
Considerations for the Selection of Lining Material
Denture reline materials play a key role in modern removable prosthodontics.8 The criteria for application of a reline material include poor stability and inadequate retention; reduction in vertical dimension; degradation of the denture base; loss of support between the denture and alveolar ridges; improper extension of borders into muccobuccal fold regions; and mucosal irritation.3 The demand for successful treatment with complete and removable partial dentures (RPDs) has provided the clinician and technician with a plethora of simplified “one-visit” lining materials. Therefore, it is understandable that clinicians have uncertainties about the selection of materials and techniques to achieve optimal results for denture relining procedures. The clinical consideration for the selection of a denture lining material becomes a function of the properties of the material and the specific clinical situation. The fundamental properties that provide guidelines for acceptability for a clinical situation include hardness, water sorption, and water solubility.8,11 A high water sorption and solubility of a lining material can reduce mechanical properties such as hardness, fatigue limit, and transverse strength.12-14 An increase in the values of these mechanical properties can result in dimensional change, separation from the denture base, and discoloration.15 An ideal lining material should possess the following characteristics:
- high shear bond strength to denture base materials
- superior resistance to stain
- low water sorption
- no soluble components (low solubility)
- color stability
- optimal hardness for specific lining material
- high fatigue limit
- increased transverse strength
- minimal dimensional change during polymerization (dimensional stability)
- ease of finishing
- abrasion resistance
- tissue compatibility
- absence of taste and odor
- low exothermic temperature release
- absence of free methyl methacrylates.1,2,5,8,16-24
Although the search continues for the ideal lining material, there is no one material that can achieve the requirements of every clinical situation. A review of the clinical considerations for the use of hard and soft liners may provide the clinician with the knowledge required to make the appropriate selection of liner material for each individual clinical situation.
Denture reline materials can be subdivided into two categories: hard and soft liners. A description of the clinical indication for application of each material may provide answers for both clinicians and technicians in their uncertainties about selection of these different liner materials.
Soft Denture Liners
Soft denture liner materials have become an asset to the technician and clinician because of their viscoelastic properties.25-27 These materials act as shock absorbers and tissue conditioners that can reduce and distribute occlusal forces to the underlying oral structures during function while enhancing patient comfort.4,8,20,25,28-37
These materials may be selected for the treatment of the following conditions:
- atrophic ridges
- bone undercuts
- denture(s) opposing natural teeth
- reduced thickness and viscoelasticity of the mucosa
- pain from gingival irritation
- maxillofacial defects
- traumatic or
- pathologic tissue loss.38-44
Hard Denture Liners
Hard denture liners are generally used in prosthetic dentistry to reline immediate dentures, for selected RPDs, and for interim dentures until a final denture is completed.7 Hard liners can be used when there is an adequate residual ridge, resilient mucosa, and mature and healthy supporting structures. These materials should be selected for the treatment of an unstable and ill-fitting denture.
Components of the System
A better understanding of a specific relining system requires a description and discussion of components of the system. VOCO America, Inc (Sunnyside, NY), as recently as 1997, has introduced both a soft and a hard reline system. The soft system, identified as Ufi Gel SC soft liner, is actually a permanent soft liner. It is based on A-silicone (addition silicone) and is available in safety cartridges (SC). The hard liner material is identified as Ufi Gel hard and is a PMA-based, cold-curing, permanent hard denture liner. It is available in the hand-mix format as well as in the cartridges. Furthermore, the hard liner system is quick and relatively easy to use for both direct and indirect relines. Similar in hardness to denture acrylic, Ufi Gel hard is methyl methacrylate-free but can be trimmed and polished in the same manner as denture acrylic. Also, as compared to acrylic-based resins, there virtually is no increase in temperature during polymerization.
Ufi Gel SC(Soft Relining Agent)
The Ufi Gel SC consists of three basic components. These include the adhesive, the reline materials, and the glaze. The adhesive is composed of a reactive polymer, a special silane, and a commonly used solvent. The adhesive is easily applied to the denture, and after 1 minute the ready-to-use reline material can be applied straight from the cartridge. The reline material is composed of traditional A-silicones and special catalysts. The glaze consists of a two-component A-silicone, which smoothes and seals any trimmed areas of the relining material to prevent bacterial or fungi penetration.
In at least one study conducted by Professor D. Welker at the University of Jena, Ufi Gel SC exhibited considerably better performance in terms of tear resistance and percent elongation when compared to a number of other systems currently on the market.45 Such tests were conducted at body temperature (37° C) at the end of 6 months. The shear bond strength (adhesion) of Ufi Gel SC to polymethyl methacrylate over a 6-month period was also appreciably greater.45 Similar results were also published at the Universities of Hanover and Giessen.46,47 Also, according to the later studies, Ufi Gel SC was shown to be highly resistant to discoloring agents and was relatively property-insensitive in water storage over extended periods of time.45
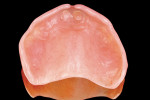
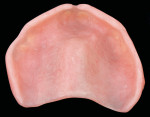
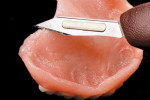
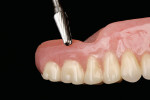
Finally, Ufi Gel SC has been shown to be a dimensionally stable and permanently soft material. A permanent set value of 12.1% demonstrates its high elasticity. In addition, its elastic recovery of 99.76% indicates that it will always return to its original dimension or shape when deformed. The Shore A hardness value of 26 is within the ideal range for soft lining materials and indicates that it does remain permanently soft. Incidentally, the amount of water sorption after 9 months in storage was only 0.1%. This value can be compared to other commercial agents, which were as high as 3.5% after only 1 day in water storage.45 This agent, by VOCO, is a new type of hard reline material in direct application cartridges, which is used directly in the oral cavity. The material is methyl-methacrylate?free and adhesively bonds to the denture base firmly and permanently. Furthermore, no exothermic heat characterizes the system during polymerization. Consequently, the curing process can occur entirely in the patient’s mouth, which in turn assures an accurate fit. The range of indications includes hard, permanent relining of all denture base and denture-bearing tissues, inaccuracies in partial and full dentures as well as functional peripheral extensions. The extensions can be carried out without the necessity of building up large peripheral sections of the denture. Furthermore, layer-by-layer adjustments are possible over many years of service. Ufi Gel hard is a cold-curing, permanently hard denture reline material based on polymethacrylate. The hand-mixed version consists of a powder/liquid system. In addition to the usual reline components, the liquid is based almost entirely on dimethacrylate. The powder component consists of bead polymers. Because of the volatility of the solvent base, the conditioner permeates the denture resin and generates additional retention between the denture and the reline material. The availability of Ufi Gel hard in direct-application cartridges (Ufi Gel hard C) offers the advantages of fast and relatively easy application, homogeneity, and bubble-free consistency. Ufi Gel hard is a methyl methacrylate-free material. Furthermore, it contains extremely little monomethacrylate (< 3% by weight). As a result, it ensures no mucosal irritation or allergenic responses. It is completely tasteless and odorless. The bond strength to denture acrylic after immersion for 24 hours is 15 MPa; in conjunction with thermal cycling, this value ranges between 12 MPa and 13 MPa.48 Its resistance to discoloration when immersed in coffee for 1 week is very low. Specifically, the b-value, which is part of the AE-value (defined as the difference in color between the material and the body), is 3.2 or nearly half that of others against which it was tested.48 Lastly, the polymerization temperature of the hard line material is the same or less than that of body temperature (37° C or 98.6° F); other systems may reach nearly 55° C (138° F).48 This relining system can be carried out chairside and completed in one appointment. It is biocompatible, easy and quick to complete, and is tasteless and odorless. Because it is methyl methacrylate-free, there is no associated mucosal irritation or allergenic responses. It generates a permanently strong bond with the base and can be trimmed and cleaned upon finishing. Lastly, it is color stable and esthetic. The following clinical procedure demonstrates the art of relining a maxillary overdenture using this new type of hard reline material through direct application. A 74-year-old woman presented with an ill-fitting overdenture 6 months after immediate placement. A soft liner had been repeatedly placed for several months to condition the tissue. This material not only improves denture stability and retention but also absorbs and uniformly distributes the applied functional forces while the supporting soft and hard tissues mature from surgery.25 The maxillary right central had an existing gold post that was contoured and polished while the remaining abutment teeth were restored with a hybrid composite resin (Aelite™ LS, Bisco, Inc, Schaumburg, IL), contoured, finished, and polished. The clinical procedure illustrates the authors’ relining procedure (Figure 1; Figure 2; Figure 3; Figure 4; Figure 5; Figure 6; Figure 7; Figure 8; Figure 9; Figure 10; Figure 11; Figure 12; Figure 13; Figure 14; Figure 15; Figure 16; Figure 17). Knowledge and a desire to create are limited by the products clinicians have available to them for restorative procedures, and knowledge must be integrated with the proper selection of material and technique for each clinical situation. Maintaining the balance between function, comfort, and esthetics with removable and complete dentures requires periodic clinical evaluation and long-term maintenance. There are a myriad of reline materials available to the restorative dentist and a wide variety of applications. This article has attempted to provide an overview of one relining system. Although this clinical procedure has provided excellent clinical results in specific cases, clearly these direct reline materials and techniques require peer research to determine their long-term effectiveness. As with most procedures, clinical experience and judgment based on scientific evidence must dictate the final decision for application. 1. Dootz ER, Koran A, Craig RG. Comparison of the physical properties of 11 soft denture liners. J Prosthet Dent. 1992;67(5): 707-712. 2. Arena CA, Evans DB, Hilton TJ. A comparison of bond strengths among chairside hard reline materials. J Prosthet Dent.1993;70(2):126-131. 3. Christensen, GJ. Relining, rebasing partial and complete dentures. J Am Dent Assoc. 1995;126(4):503-506. 4. Parr GR, Rueggeberg FA. Physical-property comparison of a chairside- or laboratory-polymerized permanent soft-liner during 1 year. J Prosthodont. 1999;8(2):92-99. 5. Hayakawa I, Akiba, N, Keh E, et al. Physical properties of a new denture lining material containing a fluoroalkyl methacrylate polymer. J Prosthet Dent. 2006;96(1):53-58. 6. Craig RG. Restorative Dental Materials, 7th ed. St Louis, Mo: The CV Mosby Co, 1985:495. 7. Bunch J, Johnson GH, Brudvik JS. Evaluation of hard direct reline resins. J Prosthet Dent. 1987;57(4):512-519. 8. Yilmaz H, Aydin C, Bal BT, Ocak F. Effects of different disinfectants on physical properties of four temporary soft denture-liner materials. Quintessence Int. 2004;35(10):826-834. 9. Hickey JC, Zarb GA. Boucher’s Prosthodontic Treatment for Edentulous Patients, 8th ed. St Louis, Mo: The CV Mosby Co,1980:560. 10. Smith DC. Recent developments and prospects in dental polymers. J Prosthet Dent. 1962;12:1066. 11. Waters M, Jagger R. Mechanical properties of an experimental denture soft lining material. J Dent. 1999;27(3):197-202. 12. Dixon DL, Ekstrand KG, Breeding LC. The transverse strengths of three denture base resins. J Prosthet Dent. 1991;66(4):510-513. 13. Fujii K. Fatigue properties of acrylic denture base resins. Dent Mater J. 1989;8(2):243-259. 14. Kalachandra S, Turner DT. Water sorption of plasticized denture acrylic lining materials. Dent Mater. 1989;5(3):161-164. 15. Massler M, Emslie RD, Bolden TE. Fetor ex ore; a review. Oral Surg Oral Med Oral Pathol. 1951;4(1):110-125. 16. Craig RG. Restorative Dental Materials, 8th ed. St Louis, Mo: The CV Mosby Co, 1989:509-559. 17. Wright PS. Composition and properties of soft lining materials for acrylic dentures. J Dent. 1981;9(3):210-223. 18. Arima T, Murata H, Hamada T. Properties of highly cross-linked autopolymerizing reline acrylic resins. J Prosthet Dent. 1995;73(1):55-59. 19. Water MG, Jagger RG, Winter RW. Water absorption of (RTV) silicone denture soft lining material. J Dent. 1996;24(1-2):105-108. 20. Emmer TJ Jr, Emmer TJ Sr, Vaidyanathan J, et al. Bond strength of permanent soft denture liners bonded to the denture base. J Prosthet Dent. 1995;74(6):595-601. 21. Kawano F, Dootz ER, Koran A, et al. Sorption and solubility of 12 soft denture liners. J Prosthet Dent. 1994;72(4):393-398. 22. Kawano F, Dootz ER, Koran A, Craig RG. Comparison of bond strength of six soft denture liners to denture base resin. J Prosthet Dent. 1992;68(2):368-371. 23. Council on Dental Materials and Devices. Revised American Dental Association specification No. 12 denture base polymers. J Am Dent Assoc. 1975;90:451-458. 24. Ogle RE, Sorensen SE, Lewis EA. A new visible light-cured resin system applied to removable prosthodontics. J Prosthet Dent. 1986;56(4):497-506. 25. Kawano F, Tada N, Nagao K, et al. The influence of soft lining materials on pressure distribution. J Prosthet Dent. 1991;65(4):567-575. 26. Hayakawa I, Kawae M, Tsuji Y, et al. Soft denture liner of fluoroethylene copolymer and its clinical evaluation. J Prosthet Dent. 1984;51(3):310-313. 27. Craig RG, Gibbons P. Properties of resilient denture liners. J Am Dent Assoc. 1961;63:382-390. 28. Lytle RB. The management of abused oral tissue in complete denture construction. J Prosthet Dent. 1957;7:27-42. 29. Lytle RB. Complete denture construction based on a study of the deformation of the underlying soft tissue. J Prosthet Dent.1959;9:539-551. 30. Kawano F, Kon M, Koran A, et al. Shock-absorbing behavior of four processed soft denture liners. J Prosthet Dent. 1994;72(6):599-605. 31. Crum RJ, Loisselle RJ, Rooney RE Jr. Clinical use of a resilient mandibular denture. J Am Dent Assoc. 1971;83(5):1093-1096. 32. Kawano F, Ohguri T, Koran III A, et al. Influence of lining design of the processed soft denture liners on cushioning effect. J Oral Rehab. 1999;26(12):962-968. 33. Parker HM. Impact reduction in complete and partial dentures, a pilot study. J Prosthet Dent. 1966;16(2):227-245. 34. Plotnick IJ. Stress regulator for complete and partial dentures. J Prosthet Dent. 1967;17(2):166-171. 35. Calikkocaoglu S. Tam Protezler. 2. cilt, Protez Akademisi ve Gnatoloji Dernegi 2. Bilimsel yayni, 1998. 36. Qudah S, Harrison A, Huggett R. Soft lining materials in prosthetic dentistry: a review. Int J Prosthodont. 1990;3(5):477-483. 37. Jepson NJ, McCabe JF, Storer R. Evaluation of the viscoelastic properties of denture soft lining materials. J Dent. 1993;21(3):163-170. 38. Boucher Co, Hickey JC, Zarb GA, eds. Prosthodontic Treatment for the Edentulous Patient. St Louis, Mo: The CV Mosby Co, 1989:542-544. 39. Yano K. Changes in elastic and creep properties of denture soft lining materials. J Kyushu Dent Soc. 1990;44:874-889. 40. Moriya N. Study on viscoelastic properties of soft lining materials. J Hiroshima Univ Dent Soc. 1993;25:186-199. 41. Hayakawa I, Hirano S, Kobayashi S, et al. The creep behavior of denture supporting tissues and soft lining materials. Int J Prosthodont. 1994;7(4):339-347. 42. Hayakawa I. Principles and practices of complete denture. Tokyo: Quintessence 1999:231-248. 43. Hayakawa I, Hirano S, Takahashi Y, et al. Changes in the masticatory function of complete denture wearers after relining the mandibular denture with a soft denture liner. Int J Prosthodont. 2000;13(3):227-231. 44. Shim JS, Watts DC. An examination of the stress distribution in a soft-lined acrylic resin mandibular complete denture by finite element analysis. Int J Prosthodont. 2000;13(1):19-24. 45. Welker D, et al. Werkstoffkndlich-vergleichende untersuchungen des weichen Kunststoffs Ufi Gel SC; Klinikum dere Freidrich-Schiller-Universitat Jena: marz 1998. 46. Kraft A. Mechanical properties of silicone-based soft lining materials. J Dent Res. 1999;78(Spec Issue):2727. 47. Borchers L. Bond strength of silicone lining materials to PMMA. J Dent Res. 1999;(Spec Issue):335. 48. Hartmann J. Scientific Product Information Ufi Gel- Relining System, VOCO America, Inc: Sunnyside, NY; 2000. Karl F. Leinfelder, DDS, MS Douglas A. Terry, DDS Mark E. Connelly, DDSUfi Gel Hard
Clinical Procedure
Conclusion
References
About the Authors
Adjunct Professor, Biomaterials Clinical Research
University of North Carolina
Chapel Hill, North Carolina
Professor Emeritus
University of Alabama School of Dentistry
Birmingham, Alabama
Adjunct Assistant Professor, Department of Restorative Dentistry and Biomaterial
University of Texas Health Science Center at Houston
Private Practice
Houston, Texas
Past Chairman of the Department of Removable Prosthodontics,
University of Texas Health Science Center at Houston
Houston, Texas Faculty
University of Alabama School of Dentistry
Birmingham, Alabama
Private Practice
Houston, Texas