Facial Esthetic Design
Michael Apa, DDS
In today’s world, people are constantly striving to better themselves both mentally and physically. People want to look better, feel better, and live longer. Gym memberships, diet centers, tanning spas, and yoga centers have all become the vogue and are enabling us to live a healthier, even prettier lifestyle. But every now and then dentists have to take a step back and ask, “What am I trying to accomplish?” Technology and science offer another step further in the beautification process. Bleaching centers to get teeth whiter and healthier looking in an hour, Botox or microderm abrasion treatments to erase the signs of aging instantly, and sunless tanning salons to get a perfect tan within minutes are just some of the treatments available to us in obtaining our perfect look. But what does perfection look like? Is there such a thing? Webster’s defines perfect as “complete, excellent; the highest of quality; perfection is the state of being perfect.” Cosmetic dentists frequently hear, “I want my teeth to look perfect.” In the mind of a dentist, symmetrically uniform, straight, white teeth are not perfect. Teeth must have slight angulations, rotations, and other nuances that make a smile look “perfect.”
For teeth to look and feel natural, the surrounding facial features have to be taken into consideration and a plan for the smile needs to be organized. Often, patients will favor either their left or right side when they smile (Figure 1). A lip may rise higher on one side than the other. The favored side is actually the weak side of the facial musculature and the nonfavored side is the strong side of the facial musculature. These facial developments will produce asymmetries that need to be accounted for when the smile is designed. The angulation of the nares, the plane of the eyes, the plane from commisure to commisure, as well as the position of the nose and chin all are in the frame of your “painting.” If they are not all taken into consideration, the art will not look centered in the frame.
This article will focus on the pitfalls of restoring a class II division 2, adhering to this concept of facial esthetic design. Regardless of the position or color of the teeth, certain guidelines should be adhered to, keeping facial structures and tones in mind.
CASE PRESENTATION
Any time a severe class II division 2 is being treatment planned, the first suggestion to the patient should always be orthodontics. Much less preparation will be needed later if the teeth are put into a favorable position early on in the treatment. However, the patient in this case was a model and not allowed to wear braces. At this point, diagnostic models were taken along with a measurement of the central incisors. A series of digital and Polaroid photographs were taken to analyze the smile design and facial esthetic design. It was determined that the lip position at rest is relied on teeth Nos. 7 and 10 to maintain its position. This is where the arch form should be formulated. For example, if the centrals are brought out labially to the laterals, an overly prominent arch form will be created, resulting in a buck tooth. Conversely, if the laterals are brought in too far lingually, the lip position at rest will be lost and a potential pulp exposure on the lateral incisors could be created (Figure 2 and Figure 3). In this case, the author wanted to leave a slight rotation of teeth Nos. 7 and 10 to give the appearance of a class II division 2, yet create a much more favorable arch form. To put the front teeth out further would have pronounced the overjet. The final treatment plan was to place veneers on teeth Nos. 4 through 13, creating a natural arch form with minimal preparation; and to place veneers on teeth Nos. 21 and 28 to gain room cosmetically for the anatomy of the upper canines (Figure 4).
When designing any smile, the first consideration is the surrounding facial features. In Figure 1, note how the patient favors the right side while smiling. In the same way that people are either right- or left-handed, there are dominant and weak sides of facial musculature, as people also favor a side to smile from, speak from, wink from, etc. This leads to an overdevelopment in the musculature and creates asymmetries in facial features. In this case, the interpupillary planes were not parallel to the intercommissural plane, and the nose pointed toward the patient’s left side. All of these factors were taken into consideration when preparing the teeth for the final restorations, and all of these factors were communicated to the ceramist for the diagnostic wax-up. This allows the dentist to be as conservative as possible with preparations through the use of incisal and labial reduction guides that are made directly from the wax-up.
Bulk reduction was done first to the arch form to set the teeth up in the desired position. The centrals were minimally reduced from the labial because they added to this surface. The laterals had a bit more aggressive preparation, although the author still took care not to expose the nerves. Teeth Nos. 7 and 10 were both rolled in from the labial-incisal until they were placed in the correct arch form. The canines and premolars were also minimally prepared because the author was adding to these teeth as well; however, they were prepared to look anatomically light, a smaller version of what the final restorations were to look like. A diode soft tissue laser was used to achieve the correct gingival architecture. The lower first premolars were simply rolled in lingually until enough room (clearance) was available to create a stop on the lingual of the upper teeth.
Provisional restorations were then fabricated using the matrix created from the wax-up. The teeth were coated with glycerine to prevent the temporary material from setting to the teeth. Luxatemp® BL (Zenith/DMG Brand Division, Englewood, NJ) was injected into the matrix, seated for 2 minutes, and then removed. The temporaries were allowed to fully set inside the matrix. Once they set, they were evaluated for sufficient thickness of material, which showed whether the teeth were prepared enough to achieve what was present in the wax-up. After this was determined, upper and lower Impregum™ impressions (3M ESPE, St. Paul, MN) were taken along with a bite registration (Regisil®, DENTSPLY International) and stumpf shade photographs of the preparations.
The provisionals were then cemented in using the spot-bond technique.1 They were trimmed and minimally shaped along with bite adjustments until the patient was comfortable. The patient was instructed to return the following day to evaluate the temporaries while she was not numb (Figure 5). Digital photographs and Polaroids were taken again to evaluate the shape, size, color, and design of the temporaries within the parameters of her facial features, occlusion, and speech. At this point, additional and final reshaping was complete. Photographs, alginate impressions, measurements of the central incisors, and a detailed laboratory prescription were also completed at this time. The goal was to recapture the patient’s at-rest position, showing her two centrals to maintain, yet enhance, her original look. In cases like these, communication is crucial between dentist and ceramist.
Insertion began a week after the preparation appointment. The provisionals were removed, along with any bonding material left behind on the teeth. The veneers were then tried in with water to evaluate marginal fit and color.2 At this point, different cements could be used to brighten or darken the final shade; in this case Vitique® (Zenith/DMG) was used in shade B1 because of its translucent properties. The veneers were then removed, cleaned, and air-dried to check for any remaining etchant.3 Silane was applied for 1 minute and air-thinned, followed by a thin layer of Optibond® Solo Plus™ (Kerr Dental, Orange, CA), and air-thinned. A split rubber-dam technique was used with superoxyl to control gingival bleeding (Figure 6). The teeth were then etched with 37% phosphoric acid for 15 seconds, rinsed, and blotted dry.4 A thin layer of Gluma® (Heraeus Kulzer, Armonk, NY) was applied and air-thinned, followed by a layer of Optibond Solo Plus. This was also air-thinned and light-cured for 10 seconds on each tooth. Vitique B1 was then applied to all of the teeth, beginning from the patient’s right to her left. Excess cement was wiped clean with cotton rolls and brushes, then each tooth was carefully spot-tacked at the gingival margin for 5 seconds. For this the author started at the centrals and moved away from the center. Brasseler strips (Brasseler USA, Savannah, GA) were then placed interproximally, and the cement was wiped clean and cured on both sides for 5 seconds.5 After a final curing of 40 seconds buccally and lingually, the upper veneers were done, and the entire process was repeated for the lower veneers. Polishing and adjustments to the bite were made and the patient was brought back the next day for final adjustments when she was not numb.
CONCLUSION
Figure 7; Figure 8; Figure 9; Figure 10; Figure 11 show the patient 1 year postoperatively. She has had no root canals, no sensitivity, no occlusal problems, and is maintaining her teeth better than she ever did.
The world of esthetic dentistry continues to evolve at an unbelievable rate; it has become much more predictable as a result of dentists and ceramists continually pushing the envelope for a superior result, encouraged by the combination of being able to help people feel better about themselves along with the challenge of creating every look to be as natural-looking and beautiful as possible.
ACKNOWLEDGMENT
The author would like to thank Jason Kim for all of his insight and beautiful porcelain work as well as Dr. Larry Rosenthal for all of his mentoring and patience along the way.
References
1. Christiansen GJ. Veneering of teeth. State of the art dentistry. Dent Clin North America. 1985;29(2): 371-391.2. Christiansen GJ. The changing face of aesthetic dentistry. Signature. 1997;4(2):1.
3. Kanca J 3rd, Bonding to tooth structure: a rational, rationale for a clinical protocol. J Esthet Dent. 1989;1(4):135-138.
4. Bertolotti RL. Total etch—the rational dentin bonding protocol. J Esthet Dent. 1991;3(1):1-6.
5. Kanca J. Resin bonding to wet substrate: 1. Bonding to dentin. Quintessence Int. 1992;23(1):39-41.
 |  | |
| Figure 1 Full face. Note patient favoring right side. | Figure 2 Palatal photo of the upper maxillary arch. | |
 |  | |
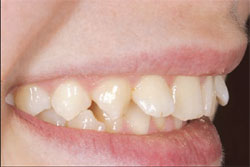
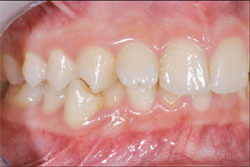
| Figure 3 Sagittal full smile. Note position of lateral incisors. | Figure 4 Maximum intercuspation. Note canine to 1st bicuspid position. | |
 |  | |
| Figure 5 Temporaries. | Figure 6 Upper maxillary arch showing prepared teeth. | |
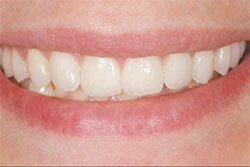 | 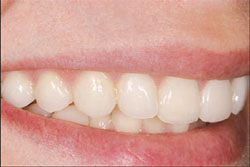 | |
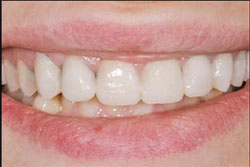
| Figure 7 One year postoperative view of full smile. | Figure 8 One year postoperative lateral right view. | |
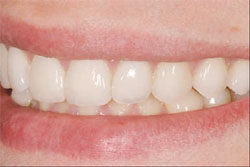 | 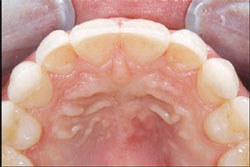 | |
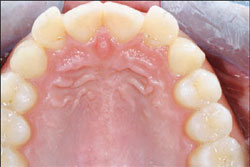
| Figure 9 One year postoperative lateral left view. | Figure 10 Palatal view, one year postoperation. Note simulated Class II Division II recaptured. | |
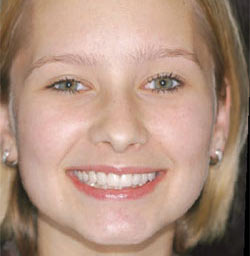 | ||
| Figure 11 One year postoperative view of full smile. Note harmonious facial features in accordance with smile. | ||
| About the Author | ||
 Michael Apa, DDS Michael Apa, DDSThe Rosenthal/Apa Group New York, New York | ||



