Tips and Tricks for the Adhesive Cementation of Ceramic Inlays, Onlays, and Veneers
Edward A. McLaren; Jeffrey Hamilton
Bonded-porcelain and glass-ceramic restorations have the advantage of being a conservative treatment option for the esthetic reconstruction of teeth, requiring significantly less tooth structure removal than conventional crown procedures. However, to be successful with bonded-porcelain procedures, exquisite adhesive technique is required. Bonding porcelain restorations can be problematic and time consuming, which has caused many dentists to avoid using bonded-ceramic restorations. This article will cover some clinical tips and tricks that will facilitate the adhesive luting process for inlays, onlays, and veneers.
Tips for Provisionalization Cementation
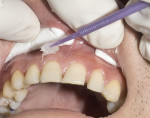
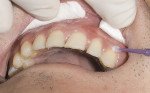
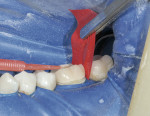
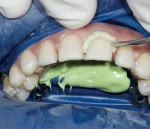
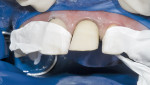
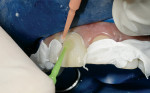
Fabricating and bonding provisional restorations at the preparation appointment and then removing them at the cementation appointment has been problematic for many reasons. Indirect fabrication of prototypes is clearly the best technique but it can be time-prohibitive in the average general dental practice. The direct fabrication of prototypes with bis-Acryl temporary materials has become the standard. Directly curing bis-Acryl materials on prepared teeth can bond the prototypes to the teeth or lock them into undercuts, making their removal difficult and also possibly damaging the preparations upon removal. Many dentists recommend sealing prepared tooth structure at the time of preparation, especially if dentin is exposed. If the tooth has been sealed at the time of preparation it is likely that directly curing bis-Acryl materials on the tooth will bond these materials to the tooth structure. The authors also believe in sealing prepared tooth structure at the time of preparation, by using a thin film thickness primer/adhesive combination to minimize sensitivity, and preventing dentin contamination with temporary cements. Either Adper™ Single Bond Plus Adhesive (3M ESPE, St. Paul, MN) or One-Step® (Bisco, Inc, Schaumburg, IL) can be used for this application. To solve the problem of the materials bonding to the etched and sealed tooth once the adhesive has been cured, a thin coat of Vaseline® (Unilever PLC, London, England) is painted over the sealed tooth to act as a separator. Figure 1 and Figure 2 show examples of this.
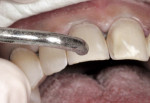
The subsequently directly cured bis-Acryl will not bond to the adhesive layer that has been covered with Vaseline, making it fairly easy to remove at the cementation appointment. A small, circular area in the midfacial of the preparation can be left uncovered with Vaseline; this area will bond to the bis-Acryl, providing some retention of the prototype similar to the spot-etch technique. Water-soluble silicone is not recommended for this purpose; the authors have tried this several times and found removal of the prototypes difficult. Once the prototypes are removed at the cementation appointment, it is ideal to lightly air abrade the surface of the tooth with aluminous oxide. This will effectively remove the oil-based Vaseline and any contamination caused by microleakage. Figure 3 shows a microetcher being used with 50-µm aluminous oxide set at 2 bars (30 psi).
Tips for Restoration Try-in and Fitting
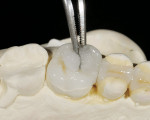
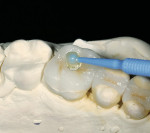
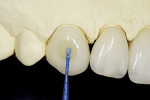
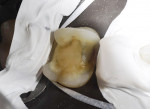
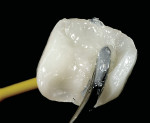
Trying-in and fitting inlays, onlays, and veneers can be a tricky process. Because of the small and fragile nature of these types of restorations, they can easily chip or fracture if too much force is applied. Also, it is very difficult to try-in and cement them without some sort of special carrying device. The authors have come up with two simple methods to attach a “handle” to the restoration that allows the easy seating and withdrawal of the restoration. In the first method, isopropyl alcohol is wiped over the surface to which the holder will be attached. For a veneer, it is the facial surface; for an inlay or onlay, it is the occlusal surface (Figure 4). A nylon primer adhesive brush is used as the handle. An unfilled adhesive is used to attach the handle to the restoration. It is important to note that a primer/adhesive combination material does not work well for this purpose. Instead, a first-generation unfilled resin or a bonding agent for etched enamel should be used, because a viscous unfilled resin will not flow all over the ceramic surface and potentially run over to the internal surface that is about to be bonded to the tooth. Examples of good materials for this are the dual-etch bonding agent from the All-Bond® 2 kit (Bisco, Inc) or the modeling resin from the belleGlass™ kit (Kerr Corporation, Orange, CA), which actually works better because of the higher viscosity (Figure 5). A drop of the resin is placed on the surface of the ceramic and the tip of the brush is wetted with the adhesive. The brush is placed in contact with the drop of resin on the ceramic (Figure 6) and then light-curing of the adhesive is accomplished (Figure 7). The brush must be attached in such a way that when carrying the restoration to place, the restoration is oriented correctly to the preparation, ie, the distal aspect of the restoration lines up with the distal aspect of the preparation (Figure 8). To remove the handle and the resin after final cementation, a sickle-shaped curette is used.
The second technique uses a plastic handle with sticky wax on the end. The problem with these devices is that they do not stick very well to porcelain. To remedy this, first wipe the porcelain surface with isopropyl alcohol as in the previous technique. Then, with a bunson burner or electronic waxer, place sticky wax on the porcelain surface to which the holder should stick (Figure 9). The sticky wax on the holder will now stick very well to the porcelain restoration (Figure 10). After final cementation, spray water on the wax and it will easily flip off with an instrument.
Marking with articulator paper and adjusting interproximal contacts is done using the same handle technique. The authors use Parkell, Inc’s (Edgewood, NY) double-sided articulating film. A small piece is cut and held in small hemostats. This is held in the contact area while gentle seating pressure is applied to the restoration (Figure 11). One of the instruments the authors like to use to adjust contacts is the knife-edge pink CeramiPro™ Dialite® disc from Brasseler USA® (Savannah, GA) (Figure 12). Once the contact gets close, a fine metal finishing strip is used to a broad, even contact inciso-gingivally (Figure 13). Once adjusted, the final polishing is done with the knife-edge gray Dialite disc.
Tips for Cementcolor Verification and Modification
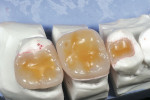
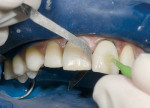
When trying-in veneers, a try-in paste should be used to verify shade. The authors start with a clear try-in paste to see if the bonded veneer will have the desired value (Figure 14). If the veneer is not bright enough, the authors recommend adding opaque to the clear try-in paste in 5% increments until the desired value is obtained (Figure 15). More than about 25% opaque white will tend to make the veneer look artificial. The amount of opaque white is noted and this ratio of opaque to clear is used in the final bonding procedure.
Tips for Gingival Retraction
If the margins are at or below the gingival margin, gingival retraction must be accomplished. Traditionally, retraction cord is used for this. If only minor retraction is necessary, an injectable retraction material called Expasyl™ (Kerr Corporation) is useful for this process (Figure 16). It is significantly faster to place than conventional cord and gives adequate retraction for this procedure. It is absolutely critical to remove the Expasyl by copious water irrigation of at least 15 seconds before starting the adhesive procedure.
Tips for Isolation During Bonding Procedures
If etchant and bonding materials get on adjacent teeth during the bonding process, the teeth can literally end up splinted together. Separating the teeth can be quite difficult and may damage the restoration and adjacent teeth. Thus, when bonding inlays, onlays, and veneers, it is important to isolate the tooth receiving the restoration. Thin matrices have been recommended but even thin matrices can prevent the seating of the restoration. The authors have found a technique for interproximal isolation that was introduced by Dr. William Liebenberg. The technique uses “plumbers” tape (Figure 17), which is a very thin Teflon® material (EI du Pont de Nemours and Company, Wilmington, DE) that comes in rolls and is used by plumbers to seal water pipes wherever there is a joint. Plumbers tape can be purchased at any hardware store. A short piece of the tape is cut and stretched over the contact of the adjacent teeth where the restoration is going to be seated (Figure 18 and Figure 19). The tape can be pulled so thin that it can be seen through. The tape is left in for the etching, priming, adhesive, and restoration placement steps. Most times the restoration will seat fully with the tape in place. If the restoration does not appear to seat fully and the excess cement is removed as normal, then the tape can be easily removed, allowing complete seating. Because no etchant, primer, adhesive, or resin cement has been allowed to contact the adjacent teeth, there will be no problem of splinting adjacent teeth. One trick that can be used for cementing inlays and onlays to help remove the excess cement before polymerization is to place a piece of dental tape or floss below the preparation margin (Figure 19). Once the onlay is seated the tape is pulled out, bringing much of the excess cement with it. This is done before polymerization.
Tips for Etching and Primer/Adhesive Application
The authors still believe in the total-etch technique for the adhesive cementation of bonded porcelain and glass ceramic restorations. Either 32% or 37% phosphoric acid is placed on the prepared tooth structure and left for 20 seconds, then rinsed with water for 10 seconds. Instead of drying with compressed air, nitrogen is used to dry for 1 to 2 seconds. A slight sheen should be visible on the tooth, with no pooling of water. A primer/adhesive bonding agent is then applied (eg, OptiBond® Solo Plus™, Kerr Corporation) and thinned with a nitrogen spray at 3 bars. The compressed nitrogen does not introduce oxygen bubbles, which can create problems with the cure. The nitrogen is also clean, as many compressed air lines contain moisture and contaminants. Precuring the adhesive can prevent complete seating of the final restoration. This is especially true for inlays and onlays. If curing is a concern, then the activator from the OptiBond Solo Plus is added to make it dual-cure.
Tips for Resin Cementing and Cement Removal
One fundamental decision that needs to be made is how many restorations are to be adhesively bonded at a time. The authors have tried every technique on one, two, or multiple restorations at once. Cementing multiple restorations at once, while very fast during the cementation process, was found to be moderately time consuming in removing the set cement and polishing. Also, the isolation technique previously discussed cannot be used with simultaneous multi-unit cementation. The authors prefer to bond one restoration at a time using medium-viscosity resin cement. All of the excess cement can be removed before light polymerization. Because there is minimal clean-up with this technique, the total treatment time to bond restorations in this manner was found to be the same as the multi-unit technique, considering cement removal time.
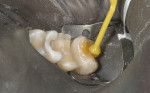
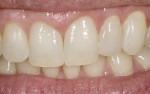
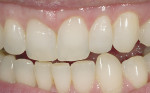
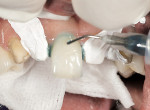
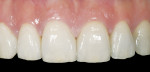
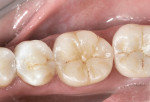
In the following examples, the restoration was filled with cement (Figure 20) and then seated intraorally. Excess cement was removed with a composite brush (Figure 21). The restoration was tacked to place with a 5-second cure in the center of the tooth. Any excess cement was easily removed before final polymerization. An air-barrier coating needed to be applied to the cement margin area to cure the air-inhibited layer. A good material for this is Liquid Lens™ (Danville Innovative Dental Products, San Ramon, CA) (Figure 22). After application, the resin cement was completely photo-polymerized. Because there was very little cement left, it was easy to remove with a micro periodontal curette or a #12 Bard-Parker™ blade (BD Medical, Franklin Lakes, NJ). Ideally, the margins of your restorations should never be touched with a bur as it will be virtually impossible to achieve the same level of finish that was obtained by proper glazing and polishing in the laboratory. Figure 23 and Figure 24 show the examples of finished veneer and inlay/onlay cases.
About the Authors
Edward A. McLaren, DDS
Director, UCLA Center for Esthetic Dentistry
Founder and Director, UCLA Master Dental Ceramist Program
Adjunct Associate Professor, UCLA School of Dentistry
Los Angeles, California
Master Dental Ceramist
Private Practice, Limited to Prosthodontics and Esthetic Dentistry
Los Angeles, California
Jeffrey Hamilton, DDS
Private Practice
Olympia, Washington
Adjunct Faculty, UCLA Center for Esthetic Dentistry
UCLA School of Dentistry
Los Angeles, California