The Intermediate Layer
Douglas A. Terry; Karl Leinfelder; Hien Ngo
The intermediate layer or “artificial dentin layer” was first identified by John McLean’s “sandwich technique” through the use of glass ionomer and composite resin. Clinicians were searching for a biomaterial that was similar to dentin. With the discovery and introduction of glass ionomers in the early 1970s, Wilson and Kent appeared to have found a restorative material with excellent biocompatibility and the ability to self-adhere to both enamel and dentin, a coefficient of thermal expansion like that of dental hard tissues, and an ability to release fluoride.1,2
The initial formulations were chemically cured by a complex acid-base setting reaction and their use was indicated for the primary and permanent dentition in Classes III and V, provisional restorations, liners and bases, core buildups, occlusal fissure sealing and filling, luting cements, and for those patients with high caries susceptibility.3,4 The early materials were available only in hand-mix form; therefore, early attempts to use these formulations resulted in shortcomings that included low wear resistance, insufficient strength, moisture sensitivity, and color instability.
Significant improvements have been made in the design of conventional glass ionomers and clinical techniques from 1970 to the present. The introduction of a light-curing, resin-modified, glass ionomer cement with a two-setting mechanism (photocure and acid-base reaction) and its further development into a three-curing mechanism (photocure, chemical cure, and acid-base reaction) by Mitra in the late 1980s gave clinicians another useful material in restoring teeth.5-7 Continued development and modification consisted of modifying particle size and distribution of the glass powder, and the addition of a light-curing resin.8 These changes have resulted in improved handling characteristics and some physical properties. These newer formulations of resin-modified glass ionomers demonstrate properties between conventional glass ionomers and composite resins. One significant improvement for conventional and resin-modified glass ionomers is the method of dispensing and mixing. The first was encapsulation, which was introduced in the 1980s, and more recently the paste-paste system.9 Evolution of glass ionomer into an adhesive polymeric material has expanded and created a new dimension in treatment potentials for the progressive dental practice.
Adhesion Versus Polymerization Shrinkage
The integrity of the bond and the marginal adaptation to tooth structure are critical for clinical success in composite restorations.10 In a restorative procedure using composite resins, the polymerization reaction of the resin matrix phase could compromise dimensional stability.11 Conversion of the monomer molecules into a polymer network, along with a closer packing of the molecules, leads to bulk contraction.12 Alternatively, when a curing material is bonded on all sides to rigid structures, bulk contraction cannot occur and shrinkage, therefore, must be compensated for by increased stress, flexure, or gap formation at the adhesive interface.11
Polymerization shrinkage or curing contraction is the amount of volumetric decrease a composite system undergoes because of the curing process.13 During the polymerization reaction, the visco-elastic behavior of the composite changes from viscous to viscous-elastic to elastic. In the viscous state, stress development is essentially nonexistent. However, when present in the visco-elastic phase, the stresses can be partially relieved by flow and elastic strain.14
Shrinkage stresses are transferred to the surrounding tooth structure because the cavity walls restrict the volumetric changes of the composite.14 The factors that influence polymerization shrinkage include: the type of resin,13 the filler content of the composite,13 curing characteristics,15 water sorption,16 cavity configuration,17 and the intensity of the light used to polymerize the composite.14
Shrinkage stress, thought to be caused by polymerization, may be the origin of many clinical challenges encountered with adhesive restorations in clinical dentistry.11 Such challenges include: microleakage, marginal breakdown, fractures, secondary caries, postoperative sensitivity, inadequate marginal adaptation, staining, pulpal irritation, and endodontic therapy.11 Numerous stress-reduction techniques have been described to prevent destructive shrinkage stress. One of those is the development of an intermediate layer of restorative material. Restorative materials recommended for this use include flowable composites and compomers, autopolymerizing composites, and conventional glass ionomer and resin-modified glass ionomer cements.18 Although both the conventional and resin-modified glass ionomers are suitable as a dentin replacement material, this article focuses on the benefits of using resin-modified glass ionomer agents for the development of an intermediate layer.
Benefits of a Resin-Modified Glass Ionomer for an Intermediate Layer
The use of resin-modified glass ionomer as an intermediate dentin layer has been suggested as a method to improve marginal integrity and enhance the internal adaptation of a directly placed, high-viscosity composite resin. To begin with, these biomaterials are multifunctional molecules that can adhere to both tooth structure and composite resin and thus provide an improved sealing ability by chemical or micromechanical adhesion to enamel, dentin, cementum, and composite resin.19 Secondly, resin-modified glass ionomers placed beneath composite resin restorations reduce the interfacial stresses by decreasing the volume of composite necessary to restore the preparation. Thirdly, in certain cavity configurations, there are no free surface areas present. Thus, the ratio between the bonded and unbonded surfaces (C-factor)15 is high, creating shrinkage stresses that are potentially higher than the bond strength.20 This can result in partial delamination from the tooth structures’ interface complex, generating marginal gaps and/or enamel fractures.20,21
The intrinsic porosity of resin-modified glass ionomer can provide inclusions or free surfaces within the cavity, reducing the configuration factor of the restoration. The liner seals the dentin, yet does not adhere to the restoration. Therefore, the gap formation is confined to the internal aspect of the cavity preparation, thereby creating a free surface within the cavity and thus reducing the C-factor. This enables more flow during polymerization, resulting in a more stress-resistant marginal adaptation.22
Next, the strength of these biomaterials is less cohesive than adhesive and thus failure is more likely to occur within the bulk of the glass ionomer than at the dentin interface. This characteristic allows protection to underlying dentin and thus sustains a marginal seal preventing ingress of bacteria. Also, the glass ionomer intermediate layer provides flexibility during functional loading and acts as a stress absorber at the interface of the restoration and the tooth. Furthermore, while resin-modified glass ionomer cements may undergo slight internal fracturing due to polymerization shrinkage, they have an ability to renew broken bonds and reshape to enforced new forms.23 This characteristic provides cavity-sealing properties, internal adaptation, and resistance to microleakage over extended periods of time.24 Finally, although resin-modified glass ionomers have a coefficient of thermal expansion slightly higher than conventional glass ionomers, research has shown no significant clinical difference in microleakage.25 This characteristic in which the materials expand and contract similar to the adjacent tooth structure is the reason for their excellent marginal adaptation that reduces the potential of gap formation and microleakage between the tooth and restoration.26
Using the Sandwich Technique
As compared to glass ionomers, composite resins possess superior fracture toughness, wear resistance, and polishability. Glass ionomers, on the other hand, have lower thermal expansion, setting shrinkage, hydrophilic qualities, and a therapeutic fluoride-release effect.
The “sandwich technique” unites the unique characteristics of both biomaterials to form a monolithic restoration with complete reinforcement of the tooth. This concept, based on the principles of “biomimesis,” was first introduced and advocated by McLean and Wilson.27-29 The procedure involves replacement of the dentin with an intermediate layer of glass ionomer cement while a bonded resin-based composite is used as the enamel substitute;30 this was called the “open-sandwich technique.”21,31,32 This technique allowed the placement of the glass ionomer so that it covered most of the exposed dentin and extended to the external surface of the restoration (ie, the proximal box of a Class II restoration). Such a procedure causes the glass ionomer to be exposed to the oral environment in the gingival region to thereby form the cervical seal (Figure 1).33 The ion exchange on the outer surface of the glass ionomer cement with the tooth structure at the cavity margin provides remineralization of affected dentin while inhibiting the demineralization of tooth structures adjacent to the restoration.34 Concerns regarding the potential for eventual dissolution of the exposed glass ionomer have been offered.35 An alternative procedure, identified as the “closed-sandwich technique” allows the placement of glass ionomer cement so that it replaces and covers the dentin while being completely contained by the overlying composite resin (Figure 2). This technique can be used in moderate-to-large Class I, Class II tunnel preparations,36,37 Class III, and Class V composite restorations.
Developing the Class V Restoration Using the Closed Sandwich Technique
Preoperative Considerations
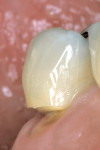
The patient, a 62-year-old man, presented to the office with sensitivity to the mandibular right second bicuspid (Figure 3). The clinical examination revealed numerous cervical defects on posterior teeth in different quadrants of the oral cavity and a high caries index. The occlusal surfaces revealed a wear pattern on the buccal cusp of these posterior teeth. After reviewing the patient’s medical and dental history and considering all of the factors related to tooth substance loss from erosion, attrition, abrasion, abfraction, or a combination of these processes, a differential diagnosis indicated a combination of an abfraction lesion caused from deflective occlusal contact on the buccal cusp and high caries suscepti-bility. Abfracted cervical lesions may be either wedge-shaped or semicircular. The actual morphology depends on the types of force generated by the parafunctioning occlusion. If the cusp is put into a state of tension, the resultant cervical defect is wedge-shaped; conversely, if the cervical region is subjected to compressive stresses, the defect is more concave or saucer-shaped.38
The information acquired during the differential diagnosis will provide a methodical approach for preventive and restorative therapy. Preoperative considerations and procedures may include preventive measures such as fluoride therapy, iontophoresis, brushing with desensitizing dentifrices, provisionalization of lesion with fluoride-releasing glass ionomer, professional application of potassium oxalate or other tubule occluding agents, application of dentin adhesives, occlusal adjustments, dietary instruction, toothbrushing and oral hygiene instruction, discontinuation of poor oral habits, and occlusal guard fabrication.39-44
Restorative Material Selection
There are numerous types of esthetic re-storative materials available for the artificial replacement of cervical tooth structure, examples of which include: the direct placement of glass ionomers,45-54 resin ionomers,45,49,52,54 compomers,40,49,51,53 flowable composites,45,49,54 microfill composites,40,45,49 hybrid composites,45,49 porcelain inlays,55 and indirect composite resin.
Traditional self-curing glass ionomers contain alumino fluorosilicate glass and polyacrylic acid and are set by an acid-base reaction.51 These restorative materials are tooth-colored,56-58 radiopaque,56-58 release fluoride over time,49,56-58 bond to dentin and enamel,56-58 are biocompatable with soft tissue,56-58 inhibit demineralization,56-58 contribute to the remineral-ization of dentin,56-58 and have a similar coefficient of thermal expansion to dentin. However, these materials afford some challenges including: sensitivity to moisture during initial set,49 increased setting time that requires a second appointment for finishing and polishing,56,58-63 rough surface texture,56,58-63 opaqueness, and dehydration.56,58-63
The newer generation of light-curing, resin-modified glass ionomer cements (Vitremer™, 3M ESPE, St. Paul, MN; Fuji II LC, GC America, Alsip, IL; Photac™-Fil Quick, 3M ESPE) are set by an acid-base reaction between an ion-leachable glass and a polyalkenoic acid and a resin polymerization reaction.52,53,64 These light-activated materials offer the following advantages to the self-cure materials in improved physical52 and mechanical properties,56 capability of immediate finishing,52,56 improved shade matching40,52 and translucency,52 improved fluoride release,52 polishability,40,52 and reduced water sensitivity.56
The third category of restorative material that releases fluoride into the saliva after placement is the compomer, although the fluoride release is less than the glass ionomer and the resin-modified glass ionomer. Polyacid-modified composite restorative materials combine the properties of glass ionomers with that of light-activated composite resin. Although manufacturers indicate use without an acid-etch step, the use of an acid-etch technique and a dentin bonding agent appears to create a strong adhesion to the cavity surface.53,65 These materials are sculptable and polishable and have physical properties more similar to those of composite resins than to those of glass ionomers.53,66,67
The final group of restorative agents, composite resin, provides an optimal esthetic result for the carious and noncarious cervical lesion. Composite resin is an excellent restorative choice as a result of the acid-etch technique and the chemical attachment to tooth structure through enamel and dentin bonding systems.40,68 Several materials from this category can be used, including: hybrids, microfills, and flowable composites. The restorative selection for this particular clinical situation with a high caries index was to combine the glass ionomer with a composite resin using the closed sandwich technique.
Clinical Procedure
The following clinical protocol employed two appointments. At the first appointment, a shade selection and photograph comparison was performed before treatment because an elevated value and/or the selection of an improper shade could result from selecting the shade after tooth dehydration. Once anesthesia had been administered, the teeth were isolated with a rubber dam to achieve adequate field control, protect against contamination, and control moisture. A modified technique was used to create an elongated hole that allowed placement of the dam over the retainer.69,70
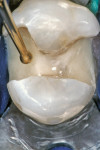
The carious dentin was removed from each tooth with a slow-speed carbide round bur No. 4 (Midwest, Dentsply/Professional, York, PA) and spoon excavators. The preparations were scrubbed with a slurry mixture of disinfectant and pumice (Consepsis®, Ultradent Products Inc, South Jordan, UT) and a surface conditioner (GC Cavity Conditioner, GC America) was applied for 10 seconds, rinsed, and the excess moisture was evacuated, leaving the dentin substrate moist. An encapsulated resin-modified glass ionomer (Fuji II) was mixed and injected into the cavity and light-cured for 20 seconds. A varnish (GC Fuji VARNISH, GC America) was applied with an applicator brush to the surface of the glass ionomer provisional restoration and to the adjacent enamel tooth surfaces. The rubber dam remained in place for 3 minutes to prevent early moisture contamination during the initial set. This initial caries-control procedure provided removal of the infected dentin and a seal in all of the cavities, while remineralizing the affected dentin (Figure 4).
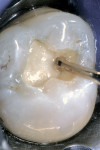
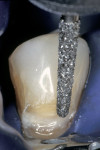
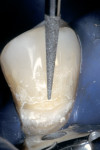
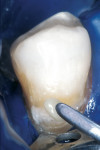
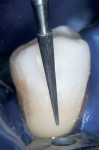
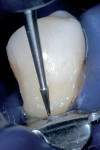
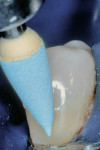
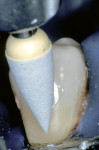
During the second appointment, the external layer of the provisional glass ionomer restoration was removed to develop an ideal Class V adhesive preparation design, while a 2-mm layer of resin-modified glass ionomer remained as the artificial dentin layer. To effect an esthetic result, a chamfer 0.3 mm in depth was placed along the occlusal margin with a long tapered diamond (#6850, Brasseler USA, Savannah, GA). A scalloped bevel was developed 0.5 mm in the enamel in order to interrupt the straight line of the chamfer (Figure 5A and Figure 5B). The bevel was placed on all margins that were in enamel to reduce the potential of microleakage. However, a butt joint would have been prepared if the gingival margin was in cementum/dentin.
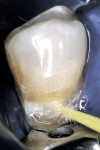
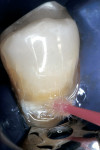
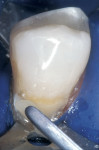
The preparation was polished with rubber cups that contained a premixed slurry of pumice and 2% chlorhexidine (Consepsis). The preparation was rinsed and lightly air-dried. A two-component self-etch system (UniFil® Bond, GC America) was used. The self-etching primer was applied to the preparation and allowed to set for 20 seconds, dried gently for 5 seconds, and the bonding agent was applied to the enamel and dentin surfaces and light-cured for 10 seconds (Figure 6A, Figure 6B, Figure 6C).
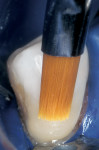
To establish more realistic depth of color, the “artificial enamel” was applied in two composite layers that varied in thickness. The initial enamel layer of A-4 opaceous shaded composite resin (Gradia™ Direct, GC America) was applied to the occlusal one half of the preparation and contoured with a long-bladed composite instrument (TNCVIPC, Hu-Friedy, Chicago, IL) to ensure complete adaptation to the underlying glass ionomer and tooth structure. Each layer was smoothed with an artist’s brush to prevent surface irregularities and to develop the correct anatomical contour (Figure 7A and Figure 7B). Each increment was polymerized with a curing unit for 40 seconds, which allowed placement of subsequent increments without deforming the underlying composite layer. An additional opaceous increment was placed in the gingival one half of the preparation and the previous process was repeated (Figure 8). The final “artificial enamel” was restored with a translucent-shaded hybrid composite (Gradia Direct). The layer was sculpted using the long-bladed composite instrument and smoothed with a sable brush to obtain an anatomical correct emergence profile that encased the underlying matrix cervicoincisally and mesiodistally (Figure 9). This process of careful shaping of the composite resin to those confines before curing facilitates the establishment of anatomic morphology and minimizes the finishing protocol. At least one study reveals that a reduction in finishing results in less damage to the composite and improved wear and clinical performance.71 A thin layer of glycerin was applied to the surface and polymerized for a 2-minute postcure, ensuring complete polymerization of the composite resin at the margins (Figure 10).
Finishing and Polishing
Newer formulations of small-particle hybrids and microhybrids have altered filler components by finer filler size, shape, and orientation and concentration, improving their physical and mechanical characteristics, and allowing the resin composite to be polished to a higher degree.72 The variation in hardness between the inorganic filler and the matrix can result in surface roughness since these two components do not abrade uniformly.72,73 Accordingly, it is imperative that the surface gloss between the restor-ative material and tooth interface are similar because the gloss can influence color perception and shade matching of the restoration and tooth surface.74 The esthetic appearance of the surface of a composite resin restoration is a direct reflection of the instrument system used.75 The surface of the composite can be finished and polished with a variety of techniques. Diamond, multifluted burs, discs, and polishing points and cups have all been used to reproduce the shape, color, and luster of the natural dentition. As Pratten and Johnson have indicated, there is no statistical difference between finishing and polishing anterior and posterior restorative materials;76 the consideration factors for finishing and polishing any restoration are dependent on the instrument shape, the surface shape and texture of the tooth and restorations, the surface of the finishing and polishing instruments, and the sequence of the restorative treatment.76
For finishing the labial surface, a long needle-shaped finishing bur allows the proper anatomical contours of the facial aspect of the anterior tooth to be followed. To replicate natural form and texture, initial contouring and shaping can be achieved with the 30-fluted needle-shaped bur. The ET-9 (Brasseler USA) has sufficient length to overlap the tooth-resin interface and provide a parallel plane to the tooth surface of the maxillary and mandibular anterior teeth. It is important to use a dry protocol77 and closely observe the tooth-resin surface. Dry finishing allows for better visualization of the contour and margins.
The gingival contouring was accomplished with a short, tapered, straight-edge, 30-fluted finishing bur (ET-3, Brasseler USA) which conforms to the straight emergence profile as the tooth emerges from the gingival sulcus. It is important to use a dry protocol and retract the gingiva with an 8A instrument, closely observing tooth structure and the gingival margin area. It is important not to overheat the resin by using excessive pressure. Also, it is imperative not to ditch or scar the cementum at the gingival margin (Figure 11A and Figure 11B).
After the initial finishing procedure, the margins and surface defects were sealed. The restoration and all margins are re-etched for 15 seconds with a 37.5% phosphoric acid semi-gel, rinsed for 5 seconds, and dried. Then a layer of composite surface sealant (OptiGuard™, Kerr/Sybron, Orange, CA) is applied over the margins and the restoration. This will prevent leakage and seal any microfractures or microscopic porosities in the material that may have formed during the finishing procedures. The use of a surface sealant has been shown to reduce the wear rate of posterior composite resins,78-80 improve resistance to interfacial staining,81 and decrease microleakage around Class V composite resins.54,82,83 Any excess resin can be removed with a #12 scalpel, retracting the gingiva with an 8A instrument, closely observing tooth structure and the gingival margin area.
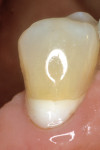
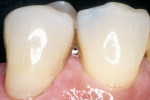
Fine finishing of the facial and gingival regions can be performed with pre-polish and high-shine rubber points and rubber hollow cups (Diacomp, Brasseler USA), which are composed of aluminum oxide particles and silicone that permit surface defects to be effectively eliminated (Figure 12A and Figure 12B). The impregnated cup follows the contour of the gingival neck and reaches into the sulcus to smooth any rough areas. To impart a high luster or surface reflectivity on the tooth and restoration while maintaining the existing texture and surface anatomy, the final polishing can be accomplished with loose abrasive polishing paste and a synthetic foam cup (Enhance® cup, Dentsply, York, PA) applied at conventional speed (Figure 13). These loose abrasive pastes contain aluminum oxide or diamond particles dispersed in a water-soluble vehicle, such as glycerin, and they allow the anatomical details to be maintained while imparting an enamel-like appearance to the restored tooth. An incremental use of water with these loose aluminum oxide abrasives enhances their effectiveness. Diamond abrasive pastes should be used and kept dry because the effectiveness decreases when diluted with saliva. Loose abrasives with aluminum oxide particles include: Prisma-Gloss/Prisma-Gloss ExtraFine (Dentsply/Caulk, York, PA); CompoSite (Shofu, San Marcos, CA); and Enamelize™ (Cosmedent, Chicago, IL). Loose abrasives with diamond particles include: Diamond Polish (Ultradent) and Porcelize (Cosmedent, Chicago, IL). Although clinical evidence of polishability with these new small particle hybrids appears promising, the long-term durability of the polish will need to be evaluated in future clinical trials. The postoperative view of the completed restoration reveals a harmonious integration of resin-modified glass ionomer, composite resin, and tooth structure that can be achieved by using meticulous restorative adhesive concepts with the closed sandwich technique (Figure 14).
Conclusion
The practicality of conventional lining methods with the use of glass ionomers as a restorative material is continually being challenged by new generations of hybrid composite resins and dentin bonding agents. The improved properties of resin-modified glass ionomers have opened a new dimension in preventative and restorative dentistry. This continued evolution of adhesive polymeric restorative materials with resin-modified glass ionomers and composite resins requires the clinician to re-examine and modify their restorative techniques when considering diagnosis, material selection, preparation design, restorative placement techniques, pulp protection, restorative finishing, maintenance, and even individual patient selection.84,85
Although neither restorative material (resin-modified glass ionomer or composite resin) has a monopoly on clinical success, the role of each material is not to replace, but to complement the restorative objectives. As this article has suggested, the combination of resin-modified glass ionomer and composite resin in the treatment of the carious cervical restoration provides a monolithic restoration that simultaneously provides an elastic region capable of relieving restorative-tooth stresses and the potential for gap formation while rendering it caries-resistant.
References
1. McLean, JW. Evolution of glass-ionomer cements: a personal view. J Esthet Dent. 1994;6(5):195-206.
2. Hagge MS, Lindemuth JS, Mason JF, et al. Effect of four intermediate layer treatment on microleakage of Class II composite restorations. Gen Dent. 2001;49(5):489-495.
3. Nicholson JW, Croll TP. Glass-ionomer cements in restorative dentistry. Quintessence Int. 1997;28(11):705-714.
4. Aboush YE. Dentine bond of light-activated glass-ionomer liner/bases. J Ir Dent Assoc. 1994;40(3):63-65.
5. Fruits TJ, Coury TL, Miranda FJ, et al. Uses and properties of current glass ionomer cements: a review. Gen Dent. 1996;44 (5):410-418.
6. Mitra SB. Proceedings of the Second International Symposium on Glass Ionomer Cements (ed. Peter Hunt). International Symposia in Dentistry. Philadelphia, PA. 1994;13-23.
7. Mitra SB. Eur Patent application, 0323120A2, 1989; Antonucci JM, Mckinney JE, Stansburry JW, US Patent application, 160,856,1988.
8. Sidhu SK, Watson TF. Resin-modified glass-ionomer materials. A status report for the American Journal of Dentistry. Am J Dent. 1995;8(1):59-67.
9. Mount GJ. Glass ionomers: A review of their current status. Oper Dent. 1999; 24(2):115-124.
10. Bouschlicher MR, Cobb DS, Boyer DB. Radiopacity of compomers, flowable and conventional resin composites for posterior res-torations. Oper Dent. 1999;24(1):20- 25.
11. Davidson CL, Feilzer AJ. Polymerization shrinkage and polymerization shrinkage stress in polmer-based restoratives. J Dent. 1997;25(6):435-440.
12. Loshaek S, Fox TG. Cross-linked polymers I. Factors influencing the efficiency of cross-linking in copolymers of methyl methacrylates and glycol methacrylates. J Amer Chem Soc. 1953;75:3544-3550.
13. Quellet D. Considerations and techniques for multiple bulk-fill direct posterior composites. Compend Contin Educ Dent. 1995;16(12):1212-1226.
14. Feilzer AJ, Dooren LH, de Gee AJ, et al. Influence of light intensity on polymerization shrinkage and integrity of restoration-cavity interface. Euro J Oral Sci. 1995;103(5):322-326.
15. Krejci I, Lutz F. Marginal adaptation of Class V restorations using different restorative techniques. J Dent. 1991;19(1):24-32.
16. Soltesz U, Bath P, Klaiber B. Dimensional behavior of dental composites due to polymerization shrinkage and water sorption. In: Christel P, Meunier A, Lee AJC, eds. Biological and Biomechanical Performance of Biomaterials. Amsterdam: Elsevier Science Publishers 1986:123-128.
17. Feilzer AJ, de Gee AJ, Davidson CL. Setting stress in composite resin in relation to configuration of the restoration. J Dent Res. 1987;66(11):1636-1639.
18. Farrah JW, Powers JM, eds. Condensable composites. Dent Advisor. 1998;15:2-4.
19. Wakefield CW, Kofford KR. Advances in restorative materials. Dent Clin North Am. 2001;45(1):7-29.
20. Prager MC. Using flowable composites in direct posterior restorations. Dent Today. 1997;16(7):62-69.
21. Davidson CL, de Gee AJ, Feilzer AJ. The competition between the composite- dentin bond strength and the polymerization contraction stress. J Dent Res. 1984;63(12):1396-1399.
22. Baratieri LN, Ritter AV, Perdigão J, et al. Direct posterior composite resin restorations: current concepts for the technique. Pract Periodontics Aesthet Dent. 1998;10(7):875-886.
23. Davidson CL. Glass-ionomer bases under posterior composites. J Esthet Dent. 1994;6(5):223-224.
24. McLean JW. Dentinal bonding agents versus glass-ionomer cements. Quintessence Int. 1996;27(10):659-667.
25. Sidhu SK. Sealing effectiveness of light-cured glass ionomer cement liners. J Prosthet Dent. 1992;68(6):891-894.
26. Bullard RH, Leinfelder KF, Russell CM. Effect of coefficient of thermal expansion on microleakage. J Am Dent Assoc. 1988;116(7):871-874.
27. Douglas WH, Lin CP. Strength of the new systems. In Hunt PR, ed. Glass Ionomers: The Next Generation. Proceedings of the Second International Symposium on Glass Ionomers. Philadelphia, PA: International Symposia in Dentistry, PC. 1994:209-216.
28. Mount GJ. Clinical requirements for successful “sandwich”—dentine to glass ionomer cement to composites resin. Aust Dent J. 1989;34(3):259-265.
29. McLean JW, Powis DR, Prosser HJ, et al. The use of glass-ionomer cements in bonding composites resins to dentine. Br Dent J. 1985;158(11):410-414.
30. Croll TP, Nicholson JW. Glass ionomer cements in pediatric dentistry: review of the literature. Pediat Dent. 2002;24(5):423-429.
31. Knibbs P. The clinical performance of a glass polyalkenate (glass ionomer) cement used in a “sandwich” technique with a composite resin to restore Class II cavities. Br Dent J. 1992;172(3):103-107.
32. van Dijken JW. A 6-year evaluation of a direct composite resin inlay/onlay system and glass-ionomer cement-composite resin sandwich restorations. Acta Odontol Scand. 1994;52(6):368-376.
33. Davidson CL. Glass-ionomer bases under posterior composites. In: Hunt P (ed). Glass Ionomers: The Next Generation. Proceedings of the Second International Symposium on Glass Ionomers. Philadelphia, PA: International Symposia in Dentistry, PC. 1994.
34. Serra MC, Cury JA. The in vitro effect of glass-ionomer cement restoration on enamel subjected to dimeneralisation and remineralisation models. Quintessence Int. 1992;23(2):143-147.
35. van Dijken JW, Kieri C, Carlen M. Longevity of extensive class II open-sandwich restorations with a resin-modified glass-ionomer cement. J Dent Res. 1999;78(7):1319-1325.
36. Strand GV, Nordbo H, Tveit AB, et al. A 3-year clinical study of tunnel restorations. Eur J Oral Sci. 1996;104(4[Pt 1]):384-389.
37. Jones SE. The theory and practice of internal ‘tunnel’ restorations: a review of the literature and observations on clinical performance over eight years in practice. Prim Dent Care. 1999;6(3):93-100.
38. Grippo JO. Abfractions: a new classification of hard tissue lesions of teeth. J Esthet Dent. 1991;3(1):14-19.
39. Eccles JD. Tooth surface loss from abrasion, attrition, and erosion. Dent Update. 1982:9(7):373-381.
40. Lambrechts P, van Meerbeek B, Perdigão J, et al. Restorative therapy for erosive lesions. Eur J Oral Sci. 1996;104(2[Part2]):229-240.
41. Leinfelder KF. Restoration of abfracted lesions. Compend Contin Educ Dent. 1994;15(11):1396-1400.
42. Gillam DG, Newman HN, Bulman JS, et al. Dentifrice abrasivity and cervical dentinal hypersensitivity. Results 12 weeks following cessation of 8 weeks’ supervised use. J Periodontol. 1992;63(1):7-12.
43. Xhonga FA, Sognnaes RF. Dental erosion: progress of erosion measured clinically after various fluoride applicationsJ Am Dent Assoc. 1973;87(6):1223-1228.
44. Markowitz K. Tooth sensitivity: mechanisms and managements. Compendium 1993;14(8):1032.
45. Grippo JO. Noncarious cervical lesions: the decision to ignore or restore. J Esthet Dent. 1992;4 Suppl:55-64.
46. Mount GJ. Restorations of eroded areas. J Am Dent Assoc. 1990;120(1):31-35.
47. Galan D. Clinical application of Geristore glass-ionomer restorative in older dentitions. J Esthet Dent. 1991;3(6):221-226.
48. Matis BA, Carlson T, Cochran M, et al. How finishing affects glass ionomers. Results of a five-year evaluation. J Am Dent Assoc. 1991;122(7):43-46.
49. Miller MB. Restoring Class V lesions Part 1: Carious lesions. Pract Periodontics Aesthet Dent. 1997;9(4):441-442.
50. Meyers IA. Efficiency of glass ionomer cement linings in preventing microleakage under Class V composite resin restorations. Aust Prosthodont J. 1990;4:17-22.
51. Estafan D, Pines MS, Erakin C, et al. Microleakage of Class V restorations using two different compomer systems: An in vitro study. J Clin Dent. 1999;10(4):124-126.
52. Tyas MJ. The Class V lesion-aetiology and restoration. Aust Dent J. 1995;40(3):167-170.
53. Folwaczny M, Loher C, Mehl A, et al. Class V lesions restored with four different tooth-colored materials-3 year results. Clin Oral Investig. 2001;5(1):31-39.
54. Estafan D, Dussetschleger FL, Miuo LE, et al. Class V lesions restored with flowable composite and added surface sealing resin. Gen Dent. 2000;48(1):78-80.
55. Cox CF. Etiology and treatment of root hypersensitivity. Am J Dent. 1994;7(5):266-270.
56. Koprulu H, Gurgan S, Onen A. Marginal seal of a resin-modified glass-ionomer restorative material: an investigation of placement techniques. Quintessence Int. 1995;26(10):729-732.
57. Wilson AD, McLean JW. Glass-Ionomer Cement. Chicago: Quintessence, 1988: 151-152.
58. Mount GJ. Buonocore Memorial Lecture. Glass-ionomer cements: Past, present, and future. Oper Dent. 1994;19(3):82-90.
59. Mount GJ. Esthetics with glass-ionomer cements and the “sandwich” technique. Quintessence Int. 1990;21(2):93-101.
60. Gordon M, Plasschaert AJ, Soelberg KB, et al. Microlaeakage of four composite resin over a glass ionomer cement base in Class V restorations. Quintessence Int. 1985;16(12):817-820.
61. Ngo H, Earl A, Mount GJ. Glass-ionomer cements: A 12-month evaluation. J Prosthet Dent. 1986;55(2):203-205.
62. Lim KC. The microleakage of a glass ionomer cement using two methods of moisture protection. Quintessence Int. 1987;18(12):835-839.
63. Craig RG. Restorative Dental Materials. 8th ed. St. Louis, MO: Mosby, 1989:284-286.
64. Fritz UB, Finger WJ, Uno S. Resin-modified glass ionomer cements: bonding to enamel and dentin. Dent Mater. 1996;12(6):161-166.
65. Triana R, Prado C, Garro J, et al. Dentin bond strength of fluoride-releasing material. Am J Dent. 1994;7(5):252-254.
66. Uno S, Finger WJ, Fritz U. Long-term mechanical characteristics of resin-modified glass ionomer restorative materials. Dent Mater. 1996;12(1):64-69.
67. Hansen EK. Five-year study of cervical erosions restored with resin and dentin-bonding agent. Scand J Dent Res. 1992;100(4):244-247.
68. Fahl N, Denehy GE, Jackson RD. Protocol for predictable restoration of anterior teeth with composite resins. Pract Periodontics Aesthet Dent. 1995;7(8):13-21.
69. Croll TP. Alternative methods for use of the rubber dam. Quintessence Int. 1985;16(6):387-392.
70. Duke ES. Direct posterior composites. J Indiana Dent Assoc. 1993;72(5):35-39.
71. Chung KH. Effects of finishing and polishing procedures on the surface texture of resin composites. Dent Mater. 1994;10(5):325-330.
72. Chen RC, Chan DC, Chan KC. A quantitative study of finishing and polishing techniques for a composite. J Prosthet Dent. 1988;59(3):292-297.
73. Vanini L. Light and color in anterior composite restorations. Pract Periodontics Aesthet Dent. 1996;8(7):673-682.
74. Northeast SE, van Noort R. Surface characteristics of finished posterior composite resins. Dent Mater. 1988;4(5):278-288.
75. Pratten DH, Johnson GH. An evaluation of finishing instruments for an anterior and a posterior composite. J Prosthet Dent. 1988; 60(2):154-158.
76. Dodge WW, Dale RA, Cooley RL, et al. Comparison of wet and dry finishing resin composite with aluminum oxide discs. Dent Mater. 1991;7(1):18-20.
77. Dickinson GL, Leinfielder KF. Assessing the long-term effect of a surface penetrating sealant. J Am Dent Assoc. 1993;124(7):68-72.
78. Torstenson B, Brannstrom M, Lambrechts P, et al. Clinical investigation of dental adhesive systems. Part I. In vivo study. J Prosthet Dent. 1986;55(2):157-163.
79. Kawai K, Leinfelder KF. Effect of surface-penetrating sealant on composite wear. Dent Mater. 1993;9(2):108-113.
80. Ramos RP, Chimello DT, Chinelatti MA, et al. Effect of three surface sealants on marginal sealing of Class V composite resin restorations. Oper Dent. 2000;25(5):448-453.
81. Kemp-Scholte CM, Davidson CL. Marginal sealing of curing contraction gaps in Class V composite resin restorations. J Dent Res. 1988;67(5):841-845.
82. Barone-Smith CE, Dickens SH. Effect of surface sealing on the microleakage of bonded restorations. J Dent Res. 1999;Abstract #394.
83. Leinfelder KF. Using composite resin as a posterior restorative material. J Am Dent Assoc. 1991;122(4):65-70.
84. Ferracane JL. Using posterior composites appropriately. J Am Dent Assoc. 1992; 123(7):53-58.
85. Liebenberg WH. Posterior composite resin restorations: operative innovations. Pract Periodontics Aesthet Dent. 1996;8(8):769-778.
About the Author
Douglas A. Terry, DDS
Adjunct Assistant Professor, Department of Restorative Dentistry and Biomaterial
University of Texas Health Science Center at Houston Private Practice
Houston, Texas
Karl Leinfelder, DDS, MS
Adjunct Professor
Biomaterials Clinical Research
University of North Carolina
Chapel Hill, North Carolina
Professor Emeritus
University of Alabama
School of Dentistry
Birmingham, Alabama
Hien Ngo, BDS, MDS
Associate Professor
Biomaterials and Minimal Intervention
University of Adelaide
School of Dentistry
Adelaide, Australia