Indirect Composite Resin Systems: A Clinical Material Review
Karl F. Leinfelder, DDS, MS, and Douglas A. Terry, DDS
The introduction of composite resin to the profession represents one of the most interesting advances in the field of restorative dental materials. Perhaps even more exciting than the development of amalgam or the introduction of porcelain-fused-to-metal, composite resin has been developed to a level never originally intended or imagined. Currently, it is used by nearly every clinician in Europe and the Americas. In fact, many clinicians have totally substituted composite resin for the traditional amalgam restoration. Not only is it used as a basic restorative material for anterior and posterior teeth, but it also serves as a major component in cements, glass ionomers, denture reliners, endodontic systems, and a wide variety of other restorative systems.
The possibility of inserting a material into a preparation similarly as amalgam but with the appropriate esthetics pushed the imagination to place it into posterior teeth.1 These original posterior materials were very similar to those used for anterior teeth but with a higher compressive strength. It was speculated that increasing the strength of the material would automatically increase wear resistance. Unfortunately, the initial attempts resulted in early clinical failure. Although the clinical restorations suffered from numerous causes, the greatest was that of inadequate wear resistance.2-6 Also of major concern was the higher level of secondary caries, particularly as compared to their amalgam counterpart.
In an effort to resolve both of these problems, it was suggested that the restoration be generated by means of an indirect technique (Figure 1). Such a process should improve substantially the potential for optimizing margin integrity and also provide the means for enhancing the rate of polymerization.7 Improved adaptation of the restoration to the walls of the preparation was expected to decrease the incidence of secondary caries. Post-cure heat treatment (125° C or 275° F) was considered a practical means for increasing the double bond conversion and thereby enhancing wear resistance.8-11
Initial in vitro studies did demonstrate excellent margin integrity as well as a substantial increase in wear resistance.12,13 Unfortunately, however, the follow-up in vivo investigations revealed little or no improvement in occlusal wear.14,15 It is interesting to note, however, that heat treatment in a dry air oven for 15 minutes did appreciably increase the wear resistance in the proximal contact region. Using a postoperative occlusal matrix, it was shown that the wear of the proximal contacts decreased by 30% to 40%, regardless of the year evaluated.16 This heat treatment format should provide a substantial increase in wear resistance not only to the proximal contact areas but also to the occlusal regions as well. This type of heat treatment results in elevating a number of mechanical characteristics through a heightened degree of polymerization, increasing fracture toughness, elastic modulus, compressive strength, flexural and diametral tensile strength, wear resistance, hardness, and color stability.11,17-19
The New Indirect Posterior Composite Resins
Regardless of the positive results as described above, the use of the indirect composite resin restoration was minimal. Undoubtedly, the major contributing factor to this level of disuse was the increased cost to the patient. Because of the laboratory involvement associated with the indirect technique, the fee for the restorative service commonly increased by a factor of 2.5 to 3 times.
More recently, the concept of indirect composite resin restorations has been influenced by the introduction of other forms of processing. Rather than simply applying a post-light–cure heat treatment in a dry heat oven, the entire process of curing was modified. This can be accomplished in three different ways. The first consists of substituting the normal atmospheric conditions in the curing chamber to one without oxygen. This is accomplished by evacuating the oxygen-containing atmosphere and carefully substituting a nitrogen atmosphere. The second method consists of curing at a slow rate (soft-start polymerization). The third and final method for improving wear resistance consists of introducing light and heat simultaneously to the curing chamber. All of these methods, for various reasons, enhance the conversion level of double carbon bonds to single carbon bonds, thereby increasing the degree of polymerization.10,11
Curing Methods
Nitrogen Atmosphere
The inclusion of small air defects (5 µm to 200 µm) within the body of the composite resin has a number of negative effects. First, the air (oxygen) tends to interfere with or inhibit polymerization. Second, as the air inclusions proximate the occlusal surface through the process of attrition, thin layers of resin collapse into the cavity. Third, small amounts of air within the composite restoration tend to absorb light. Eliminating the small air voids actually increases the translucency of the material. Such restorations commonly possess the appearance of defect-free enamel. Only belleGlass™ NG (KerrLab, Orange, CA) employs this method from the beginning to the end of the curing process.7
Soft-Start or Slow Curing
As described by Mehl and his colleagues, this method tends to be a reliable way for combining improved physical properties with increased marginal integrity.20 The concept of slow curing is based upon the concept that a slower rate of curing tends to allow a greater level of polymerization. Faster rates of polymerization tend to prematurely rigidify the newly formed polymerized branches. Such a condition will increase their stiffness, thereby disallowing further propagation of the molecule. Such a concept is incorporated in the curing process for both belleGlass NG and Cristobal+® (Dentsply/Ceramco, York, PA). Incidentally, in the case of Cristobal+, a high level of light intensity is directed to the curing restoration. The combination of a programmed level of low light intensity followed by high intensity produces a restoration that is more wearresistant than the best composite resins on the market that are light-cured only.
Light and Heat Applied Simultaneously
The combination of these two energy sources increases the thermal energy sufficiently to allow better double-bond conversion. This concept was first used by Heraeus-Kulzer (Armonk, NY) in the development of the first successful indirect composite resin restoration. Identified as Charisma®, wear resistance increased by 35% when compared to those that were cured with light only.16,20
Currently there are three specially processed composite resin restorations on the market that have been shown to be clinically wear resistant and highly esthetic. These include belleGlass NG, Cristobal+, and Sculpture®; Plus (Pentron Clinical Technologies, Wallingford, CT). Each of these systems exhibits a wear rate of around 2 µm to 3 µm more than the adjacent enamel. This can be compared to appreciably higher values for most composite resins presently on the market. Incidentally, some of the compositions actually may be chemically modified to include an activator that allows enhancement of the polymerization process.
Clinical Advantages of the Indirect Composite Resin
In spite of the obvious advantages associated with this new generation of indirect composite resins, some clinicians have been somewhat slow in accepting them as a substitution for the conventional light-cured composite resin restoration. The reason relates not only to an increase in cost to the patient but also the belief that they can fabricate a direct restoration that is as good. While it is probable that some clinicians can fabricate a direct restoration to the same level of excellence as those done in the laboratory, it probably is not the norm. Not only is the properly fabricated indirect restoration more wear resistant and esthetic but it also is less prone to postoperative sensitivity. Although polymerization can be caused by numerous factors, a main contributing factor is polymerization shrinkage stress in direct resin restorations. The polymerization shrinkage pulls the cusps together, placing tension on the odontoblastic processes. In turn, this causes postoperative sensitivity that may range from several days to months or even a year or longer. The postoperative sensitivity under these conditions will continue until there is an equalization of the pressure on the odontoblastic processes. While the direct restoration contains sufficient volume to pull the buccal and lingual cusps toward the long axis of the tooth, the same is not true for the indirect restoration. During final placement, the only polymerization that occurs is that associated with a thin liner of luting agent. Thus, the potential for placing tensile stresses on the odontoblastic processes is considerably less and therefore translates into less potential for postoperative sensitivity. Such information generally is common amongst practitioners. Reports from clinicians and years of clinical studies at such institutions as University of Alabama and University of North Carolina have demonstrated that the postoperative sensitivity of all these restorative materials, regardless of the system, is considerably less with indirect versus direct resin composites.7
The indirect, properly heat-treated composite resin also possesses another advantage. Specifically, as compared to porcelain and porcelain-fused-to-metal restorations, the transfer of masticatory forces is considerably less. There are numerous clinical situations where a highly wear-resistant composite resin is preferable to ceramic agents. For example, the clinician should strongly consider a polymer of the above-mentioned materials when restoring the coronal aspect of a dental implant. Imperfections, such as inclination or angulation of the implant, premature occlusal contacts, and appreciable loss of osseous support, are best dealt with using a material that absorbs the masticatory energy. Porcelain restorations tend to transfer much of the masticatory forces through itself and into the implant and finally into the supporting alveolar structure. The energy transferred to the implant–bone interface may then lead to a higher level of osseous degradation.7 Because certain polymer compositions, when correctly heat treated, absorb much of the energy applied to the occlusal table, it is only common sense to recommend them for full coverage. Composite materials have shown a greater capacity to absorb compressive loading forces and reduce the impact forces by 57% more than porcelain.23Therefore, composite transmits less of the applied load to the underlying implant structure.
Energy transfer through the restorative material can be related to the elastic modulus of the restorative material. By comparison, the modulus of elasticity is considerately greater for porcelain than it is for composite resin polymers.24 As would be expected, the energy transfer associated with ceramic agents is considerably greater than it is for resinous systems. This phenomenon was measured in a clinical study conducted at the University of Alabama. Using a series of monkeys, it was shown that under all circumstances, the masticatory energy associated with ceramic materials was transferred through the dental implant at greater levels as compared to dental polymers.25
Adhesive Surface Preparation
Adhesive bonding of laboratory-processed composite resins increases their resistance to fracture.26 A principal determinate in the long-term success of these restorations relies on the strength and durability of the interface between the resin cement and the bondable surface of the processed resin.27 The surface of these laboratory-processed composite resins have a highly polymerized surface with no unreacted free-end radicals for bonding to the resin cement.
While microleakage has been reported to occur at this interface between the internal surface of the inlay and the resin cement without the use of composite softening agents,28 several surface treatments have been advocated to promote adhesion between the resin cement and the indirect composite restoration. Mechanical roughening of the internal surface of the inlay can be accomplished with diamond burs, microetching with 50-µm AO particles or 30-µm silanized silica-coated AO particles (CoJet™Sand, 3M™ESPE™, St. Paul, MN) which creates a micromechanical retention bond at a microscopic level between the restorative material and the resin cement. In addition to mechanical roughening, an application of proprietary softening agents, wetting agents, or silane have been reported to enhance the bond strength between the restoration and the resin cement.29
Various pre-cementation protocols have been recommended by the manufacturers of indirect resin systems. This author’s standard cementation protocol for laboratory-processed composite resins includes microetching with CoJet Sand, followed by a silane application to restore any coating on the original fillers that may have been removed by sandblasting. As a bifunctional molecule, the silane acts as a coupling agent between the filler particles on the indirect resin surface and the resin cement. Microetching of aged composite resin with CoJet Sand resulted in increased bond strengths compared to other surface treatments for intraoral repair of composites. CoJet is designed to create a chemical bond between composite and all types of restorations.30 The mechanism of action allows the silicate particles to become embedded in the surface of the restoration during sandblasting which then reacts with the silane to improve bond strengths.31 However, reports indicate that etching or rinsing after CoJet surface treatment significantly reduced shear bond strengths (Figure 2A and Figure 2B).29,32
Conclusion
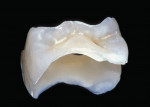
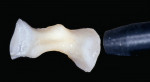
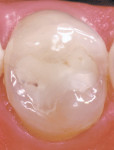
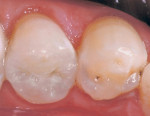
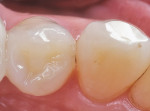
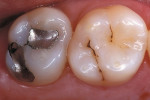
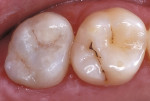
Using composite resin for a restorative procedure requires more than a rudimentary understanding of the material. Progress in adhesive technology and composite materials (ie, direct and indirect systems) allows for the preservation and reinforcement of tooth structure, while improving natural esthetics and wear resistance. These indirect composite systems complement and broaden the scope of restorative alternatives that are available to assist the patient, technician, and dentist in making an informed selection for different clinical situations. The following illustrations are provided to demonstratethe clinical application of these materials for intracoronal restorations (Figure 3A and Figure 3B; Figure 4A and Figure 4B; Figure 5A and Figure 5B).
References
1. Terry DA. Optimal esthetic results with indirect posterior composite resins. Compend Contin Educ Dent. 2001;22(2)160-166.
2. Jackson RD, Morgan M. The new posterior resins and a simplified placement technique. J Am Dent Assoc.2000;131(3):375-383.
3. Dietschi D, Scampa U, Campanile G, Holz J. Marginal adaptation and seal of direct and indirect Class II composite resin restorations: An in vitro evaluation. Quintessence Int.1995;26(2):127-138.
4. Full CA, Hollander WR. The composite resin restoration: a literature review. Part I. Proper cavity preparation and placement techniques ASDC J Dent Child. 1993;60(1):48-51.
5. Dietschi D, De Siebenthal G, Neveu-Rosenstand L, Holz J. Influence of the restorative technique and new adhesives on the dentin marginal seal and adaptation of resin composite Class II restorations: an in vitro evaluation. Quintessence Int. 1995;26(10):717-727.
6. Eames WB, Strain JD, Weitman RT, Williams AK. Clinical comparison of composite, amalgam, and silicate restorations. J Am Dent Assoc.1974;89(5):1111-1117.
7. Leinfelder KF. New developments in resin restorative systems. J Am Dent Assoc. 1997;128(5):573-581.
8. Touati B. The evolution of aesthetic restorative materials for inlays and onlays: a review. Pract Periodontics Aesthet Dent.1996;8(7):657-666.
9. Touati B, Aidan N. Second generation laboratory composites for indirect restorations. J Esthet Dent.1997;9(3):108-118.
10. Miara P. Aesthetic guidelines for second-generation indirect inlay and onlay composite restorations. Pract Periodont Aesthet Dent.1998;10(4):423-431.
11. Terry DA, Touati B. Clinical considerations for aesthetic laboratory-fabricated inlay/onlay restorations: a review. Pract Proced Aesthet Dent.2001;13(1):51-58.
12. Wendt SL Jr. The effect of heat used as secondary cure upon the physical properties of three composite resins. II. Wear, hardness, and color stability. Quintessence Int.1987;18(5):351-356.
13. Wendt SL Jr. The effect of heat used as a secondary cure upon the physical properties of three composite resins. I. Diametral tensile strength, compressive strength, and marginal dimensional stability. Quintessence Int.1987;18(4):265-271.
14. Wendt SL Jr, Leinfelder KF. The clinical evaluation of heat-treated composite resin inlays. J Am Dent Assoc.1990;120(2):177-181.
15. Wendt SL Jr, Leinfelder KF. Clinical evaluation of a heat-treated resin composite inlay: 3-year results. Am J Dent. 1992;5(5):258-262.
16. Mazer RF, Leinfelder KF. Klinische Beuteilung von Charisma als direktes and indirektes Restauration-smaterial. Der Freie Zahnartzt. 1994;6:26-29 [In German].
17. Leinfelder KF. Indirect posterior composite resins. Compend Contin Educ Dent. 2005;26(7):495-503.
18. Cook WD, Johannson M. The influence of postcuring on the fracture properties of photo-cured dimethacrylate based dental composite resin. J Biomed Mater Res. 1987;21(8):979-989.
19. Bausch JR, de Lange C, Davidson CL. The influence of temperature on some physical properties of dental composites. J Oral Rehabil.1981;8(4):309-317.
20. Mehl A, Hickel R, Kunzelmann KH. Physical properties and gap formation of light-cured composites with and without ‘softstart-polymerization.’ J Dent. 1997;25(3-4):321-330.
21. Lovell LG, Newman SM, Donaldson MM, Bowman CN. The effect of light intensity on double bond conversion and flexural strength of a model, unfilled dental resin. Dent Mater. 2003;19(6):458-465.
22. Al-Malik MS. An investigation of the dynamic mechanical properties of dental root form implants[master thesis]. Birmingham, Al:Department of Prosthodontics, University of Alabama; 1991.
23. Gracias SE, Nicholis JI, Chalupnik JD, et al. Shock-absorbing behavior of five restorative materials used on implants. Int J Prosthodont.1991;4(3):282-291.
24. Roberson TM, Heymann HO, Swift EJ Jr. Sturdevant’s Art Science of Operative Dentistry.4th ed. St Louis, MO;2002:141.
25. Al-Malik MS. An investigation of the dynamic mechanical properties of dental root form implants. [Master of Science degree thesis] Department of Prosthodontics, University of Alabama at Birmingham; 1991.
26. Rosenstiel SF, Gupta PK, Van der Sluys RA, Zimmerman MH. Strength of a dental glass-ceramic after surface coating. Dent Mater. 1993;9(4):274-279.
27. Dietschi D, Magne P, Holz J. Recent trends in esthetic restorations for posterior teeth. Quintessence Int. 1994;25(10):659-677.
28. Jordan RE. Esthetic Composite Bonding: Techniques and Materials, 2nd Ed. St. Louis, MO: Mosby Year Book, Inc; 1993.
29. Sun R, Suansuwan N, Kilpatrick N, Swain M. Characterization of tribochemically assisted bonding of composite resin to porcelain and metal. J Dent. 2000;28(6):441-445.
30. Bouchlicher MR, Cobb DS, Vargas MA. Effect of two abrasive systems on resin bonding to laboratory-processed indirect resin composite restorations. J Esthet Dent. 1999;11(4):185-196.
31. Miller MB. Miscellaneous. In: Reality 2000. 14th ed. Houston, TX: Reality Publishing; 408.
32. Bouschlicher MR, Reinhardt JW, Vargas MA. Surface treatment techniques for resin composites repair. Am J Dent. 1997;10(6):279-283.
About the Authors
Karl F. Leinfelder, DDS, MS
Adjunct Professor, Biomaterials Clinical Research
University of North Carolina at Chapel Hill
Chapel Hill, North Carolina
Professor Emeritus
University of Alabama School of Dentistry
Birmingham, Alabama
Douglas A. Terry, DDS
Assistant Professor, Department of Restorative Dentistry and Biomaterials
University of Texas Health Science Center at Houston
Houston, Texas
Private Practice, Esthetic and Restorative Dentistry
Houston, Texas