Management of the Compromised Implant Site With Small-Diameter Implants
Paul S. Petrungaro, DDS, MS
The use of dental implants to replace the natural tooth system has become routine when tooth replacement is necessary.1,2 Their use has been well documented in the dental literature,1,2 and for the replacement of anterior teeth (especially in the esthetic zone), implants can offer superior esthetics compared with routine crown-and-bridge procedures.3-6
Some impediments to the use of dental implants do exist. Small edentulous intertooth spaces, advanced bone loss, the patient’s age, and in the incidence of congenitally missing teeth, convergent roots, and/or close proximity of root trunks, can prevent the use of dental implants as a tooth replacement option.
Transitional implants became commercially available in the early 1990s,7-9 and were initially recommended for the immediate loading of a provisional appliance after stage I implant placement and/or advanced bone grafting procedures.7-9 To achieve adequate bone regeneration and/or implant stability, external forces that can cause micro- or macromovement to the bone graft and implants had to be carefully eliminated, and the use of transitional implants aided in this goal.7-10
Eventually, reports11 were published on the use of transitional implants as a permanent solution for patients who were not able to undergo the conventional two-stage implant procedure or advanced grafting protocols before implant placement. Immediate conversion of the patients’ existing denture was a simple, noninvasive technique that allowed these patients to immediately experience the benefits of implant dentistry.11
Expansion of the use of transitional implants has led to design feature changes, offering a nonrotational external hex and a screw-retained restoration option. These design changes have contributed to approval of transitional implants as a permanent implant option by the US Food and Drug Administration.
deally designed for the compromised implant site, these 1.8-mm, 2.2-mm, and 2.4-mm diameter implants offer a fixed permanent tooth replacement option for patients who otherwise would not be able to have implants placed and restored. These small-diameter implants are ideal or a postorthodontic, congenitally missing lateral incisor space < 3.2 mm in width and/or the edentulous space of similar dimension, the early teenaged patient who requires a permanent tooth replacement option for the duration of his or her growth spurt, and for sites in which advanced bone regeneration is necessary but not a treatment option. Their ease of use and atraumatic placement by using a flapless approach with only one coring procedure as well as simplistic abutment transfer and provisional construction make the use of these implants in the aforementioned sites a must for the dental implant practice.
The following case report will demonstrate the use of the Dentatus ANEW™ (Dentatus USA, Ltd., New York, NY) implant for the management of the compromised, congenitally missing lateral space in a 14-year-old adolescent girl.
Case Report
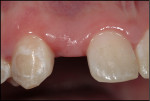
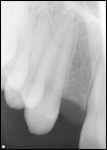
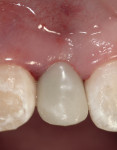
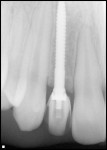
A 14-year-old nonsmoking adolescent girl presented for replacement of the congenitally missing right lateral incisor (tooth No. 7) (Figure 1). The preoperative digital periapical radiograph can be seen in Figure 2. The patient’s orthodontic treatment had resulted in a compromised implant receptor site. Along with her parents, the patient refused any reduction of the virgin natural teeth, and did not accept the option of a resin-bonded bridge. The use of a removable prosthesis was contraindicated because of the significant gag reflex the patient possessed. At the gingival level, the edentulous space measured 4.7 mm from the mesial of tooth No. 6 to the distal of tooth No. 8. Additionally, gingival tissue covered some of the existing clinical crown at teeth Nos. 6 and 8; the decision to crown-lengthen those teeth was postponed until after the patient entered her late adolescence. Conventional implant dimensions were unacceptable to treat this compromised edentulous space. For these reasons, the Dentatus ANEW 2.4-mm x 14-mm implant was selected for placement, and the immediate provisionalization procedure was selected to allow the patient to have a nonremovable tooth option.
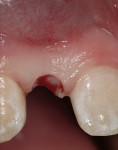
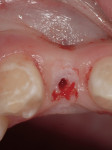
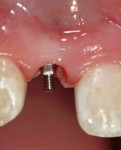
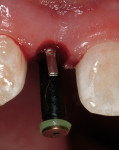
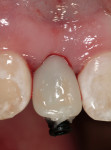
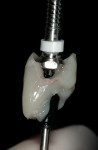
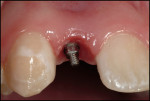
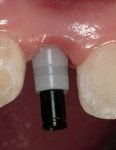
After administration of a local anesthetic, the planned tissue emergence profile was created in the edentulous ridge with a round #8 diamond (Figure 3). Placement of a TempStent™ (Contemporary Periodontics and Implantology, Lake Elmo, MN) surgical guide allowed for creation of an osteotomy site in the appropriate position in the ridge (Figure 4). After completion of the osteotomysite preparation, a 2.4-mm-diameter x 14-mm-long Dentatus ANEW implant was seated within the housing of the sculpted tissue emergence profile (Figure 5). Conversion of the TempStent surgical guide into the esthetic provisional wasinitiated by placement of the coping/silicone retention screw system (Figure 6). Placement of the TempStent over thecoping mechanism was preceded by retrofitting to the silicone screw using 3M™ ESPE™ Filtek™ (3M ESPE, St. Paul, MN) flowable composite (Figure 7). Once the composite was cured, the provisional was removed by unscrewing the retention screw and was placed on a Dentatus ANEW implant analog to correct the marginal integrity of the prosthesis (Figure 8). The final provisional restoration and the case-completed digital periapical radiograph can be seen in Figure 9 and Figure 10.
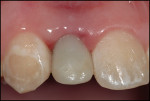
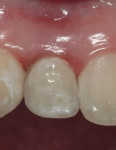
The 2-week postoperative view can be seen in Figure 11. Note the natural soft tissue contours obtained in the papillary regions at this time. At the 6-week postoperative visit, the provisional was removed, and impressions were taken for the final prosthesis (Figure 12). Insertion of an impression coping (Figure 13) preceded the appropriate impression techniques and bite registrations. The final ceramic restoration and the case-completed digital periapical radiograph can be seen in Figure 14 and Figure 15.
Conclusion
The use of the ANEW titanium alloy implant for the treatment of compromised tooth-tooth spaces is a viable treatment option to provide the patient with a fixed, permanent tooth replacement solution. For young individuals (either pre- or postorthodontic treatment) the use of a removable prosthesis can be eliminated, and the creation of esthetic tissue contours can be established. These contours can support the natural symmetry of the gingival complex in the esthetic zone, leading to esthetic tooth replacement procedures at the time of treatment, and if necessary, future treatment as well. This can lead to a successful treatment outcome with dental implants for patients who would otherwise be limited to a removable tooth replacement option or one requiring tooth preparation.
Disclosure
The author is a consultant to Dentatus, USA, Ltd.
References
1. Branemark P-I, Zarb GA, Albrektson T, eds. Tissue-Integrated Prosthesis: Osseointegration in Clinical Dentistry. Carol Stream, IL: Quintessence Publishing; 1985:11-81.
2. Adell R, Lekholm U, Rockler B, et al. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981;10(6):387-416.
3. Saadoun AP, LeGall MG. Periodontal implications in implant treatment planning for aesthetic results. Pract Periodontics Aesthet Dent. 1998;10(5):655-664.
4. Salama H, Salama M. The role of orthodontic extrusive remodeling in the enhancement of soft and hard tissue profiles prior to implant placement: a systematic approach to the management of extraction site defects. Int J Periodontics Restorative Dent. 1993;13(4):312-333.
5. Petrungaro PS. Immediate restoration of implants utilizing a flapless approach to preserve interdental tissue contours. Pract Proced Aesthet Dent. 2005;17(2):151-158.
6. Kan JY, Rungcharassaeng K. Immediate placement and provisionalization ofmaxillary anterior single implants: a surgical and prosthodontic rationale. Pract Periodontics Aesthet Dent. 2000;12(9):817-824.
7. Petrungaro PS. Fixed temporization and bone-augmented ridge stabilization with transitional implants. Pract Periodontics Aesthet Dent. 1997;9(9):1071-1078.
8. Petrungaro PS, Smilanich MD, Adams T. Altering the concepts of implantology for the 21st century. Contemporary Esthetics and Restorative Practice. 1999;3:30-37.
9. Froum S, Emtiaz S, Bloom MJ, et al. The use of transitional implants for immediate fixed temporary prosthesis in cases of implant restorations. Pract Periodontics Aesthet Dent. 1998;10(6):737-746.
10. Petrungaro PS. Reconstruction of severely resorbed atrophic maxillae and management with transitional implants. Implant Dent. 2000;9(3):271-276.
11. Babbush CA. Dental Implants: The Art and Science. Philadelphia, PA: WB Saunders Co.; 2001:201-216.
About the Author
Paul S. Petrungaro, DDS, MS
Director, The Institute for Advanced Dental Education, Inc.
Lake Elmo, Minnesota
Private Practice
Chicago, Illinois and Lake Elmo, Minnesota