Achieving Clinical Success with Provisionals
Douglas A. Terry, DDS
The provisional restoration has become an integral component in the development and management of the design of definitive prosthetic restorations. Unfortunately, many clinicians still utilize yesterday’s temporary restoration techniques with today’s newer provisional materials and wonder why they achieve less than ideal final results. Continuing esthetic and restorative demands by the public and the profession have resulted in new developments in provisional materials and cements with improved mechanical, physical, and optical properties. To meet these demands, the following considerations for selecting the proper provisional cement should be reviewed.
Optimal Retention During Function
The unseating (i.e., dislodgement) of provisional restorations can be an inconvenience for the patient and the clinician. The dilemma in cementing a provisional restoration becomes one of ensuring not too much retention upon its removal for final cementation of the definitive restoration, as well as not too little, which could lead to an early dislodgement. Furthermore, early dislodgement of the provisional can result in micromovement, sensitivity, bacterial infiltration, gingival inflammation with bleeding, gingival recession and fracture of the abutment. These manifestations can be the origin and cause of many prosthetic challenges encountered during the cementation of the permanent restoration.
Favorable Esthetics
When esthetics is of primary concern, the selection of the appropriate shade becomes an important consideration. Therefore, when creating optimal esthetic harmony with the surrounding dentition, the color of the underlying substrate and restorative cement can directly influence the final restoration. In addition, the degree of translucency/opacity and the thickness of the provisional material can influence esthetics. When the provisional material is translucent and/or has a thin dimension, an opaque provisional cement can negatively influence the value. Utilizing a translucent provisional cement (although limited in number) with a high chromatic substrate and/or a provisional material that is translucent or thin in dimension can have the same negative effect on esthetics.
Ease of Removal and Cleanup
The primary objective of the provisional cementation procedure is to achieve a durable bond and good marginal adaptation of the luting material to the provisional restoration and the tooth between the time of tooth preparation and the placement of the final restoration. The variables that influence provisional retention and/or removal include: preparation design, provisional fabrication technique and material, provisional cement, and removal technique. The provisional should be able to be removed without excess force or pressure applied to the tooth or restoration. In addition, the cement should be easy to remove from the internal surfaces of the provisional, as well as the tooth surface, if recementation is required.
Adequate Extraoral Working Time
There are several factors that can influence the required working time for cementation of provisionals: the number of provisionals to cement, utilization of automix or hand-mix materials, film thickness, or whether or not an auxiliary is used. The time required for mixing the provisional cement and lining and seating the provisional is influenced by these factors. Multiple provisionalizations may benefit from utilizing both an automix material that has a longer working time and low film thickness and an auxiliary. One in vitro study indicates that provisional cements with a lower percentage of increase between immediate film thickness and film thickness at the end of working time would benefit the single operator with multiple provisionals.1
Effect on Bond Strength
Adhesive cementation of an indirect restoration is the final process in a sequence of precisely orchestrated and repeated manipulations of instruments and restorative materials.2 This is the most complex, multifaceted procedure in dentistry due to the number of variables that can affect the success and long-term outcome of the restoration when selecting a luting cement. One of those variables is the selection of the provisional cement; studies indicate that bond strengths of resin luting cements for indirect restorations can be influenced by the provisional cement used.1 The influence of provisional cements on resinous materials and the difficulty in obtaining good bond strength to dentin under these circumstances has been reported in numerous studies.3-7 In addition, various studies suggest that the effects of the provisional cement on dentin bond strength is specific to the dentin bonding system used, and that most of the 2- and 3-step dentin bonding agents provide an increase in bond strength.8, 9
There are 2 additional procedures that have been proposed for managing dental tissues in between the preparation and final cementation of the restoration. The first is the prehybridization technique, which allows the development of a hybrid layer on vital teeth immediately after cavity preparation. This procedure provides an acid-resistant envelope that seals the dentin and prevents microleakage, protects the pulp from mechanical trauma, thermal stimuli and bacterial invasion, and, therefore, prevents hypersensitivity10 during impression taking, provisional fabrication, and final cementation. Additional clinical benefits include: improved marginal and interfacial adaptation, with reduced gap formation at the internal tooth-restorative interface; reduction of internal stress by relieving polymerization contraction stress; prevention of desiccation of the dentin that may improve the bond strength of resin cement to dentin with certain provisional cements;7 easier removal of the provisional cement; and possible prevention of hydraulic intratubular loading pressure during cementation of the restoration.
The second procedure that may reduce the effects of the provisional cement is surface preparation of the tooth substrate by microabrasion prior to the adhesive procedure. This procedure may reduce any contaminating effect from any provisional material and oral contamination that could provoke chemical interference with the polymerization of adhesive materials.
Clinical Procedure
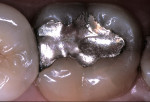
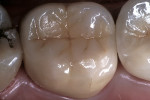
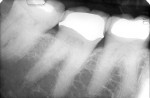
A 41-year-old male presented with a defective amalgam restoration on the mandibular left first molar with recurrent decay (Figure 1). He requested treatment with the most durable and esthetic restoration available. Preoperative considerations included radiographic analysis, preoperative diagnostic models, diagnostic wax-up, custom shade selection, and a hand-drawn occlusal and shade diagram.
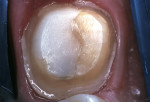
Occlusal analysis of the anatomy was performed, and the preoperative occlusal stops and excursive guiding contacts were recorded with bodyiculation paper and transferred to a hand-drawn occlusal diagram. This initial registration is valuable in the preparation design and development of the provisional and the final restoration. After removal of the existing amalgam restoration and recurrent caries, a composite build-up was developed, and the crown preparation was performed (Figure 2). The preparation was prehybridized prior to impression taking.
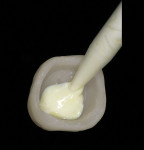
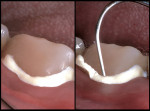
The provisional restoration was fabricated from the diagnostic wax-up utilizing a custom acrylic matrix technique and an auto-curing acrylic resin. The provisional cement selected for this procedure (Zone, Dux Dental/Cadco, Oxnard, CA) provided all of the previously discussed consideration factors (Figures 3 and 4). The specific shade tabs, comparative photographs and diagrams, and diagnostic wax-up, along with the impression of the provisional restoration, were provided to the laboratory technician so that an exact duplication could be developed (Figures 5a and 5b).
Conclusion
In light of the plethora of different restorative materials, luting cements, and dentin bonding systems available and their various clinical applications, it is understandable that clinicians are uncertain about the proper selection and critical clinical requirements involved for their use. Because each material possesses unique characteristics, proper material selection requires integrating a knowledge of each with the aforementioned consideration factors and techniques in order to create a new dimension in treatment possibilities for a wider range of clinical situations.
References
1. Miller MB. The ratings. Reality. 18th ed. Houston: Reality Publishing; 2004:771.
2. Donovan TE, Cho GC. Contemporary evaluation of dental cements. Compend Contin Educ Dent. 1999;20(3):197-220.
3. Duke ES, Phillips RW, Blumershine R. Effects of various agents in cleaning cut dentine. J Oral Rehabil. 1985;12(4):295-302.
4. Hansen EK, Asmussen E. Influence of temporary filling materials on effect of dentin-bonding agents. Scand J Dent Res. 1987; 95(6):516-20.
5. Woody TL, Davis RD. The effect of eugenol-containing and eugenol-free temporary cements on microleakage in resin bonded restorations. Oper Dent. 1992;17(5):175-80.
6. Millstein PL, Nathanson D. Effects of temporary cementation on permanent cement retention to composite resin cores. J Prosthet Dent. 1992;67(6):856-9.
7. Paul SJ, Schärer P. Effect of provisional cements on the bond strength of various adhesive bonding systems on dentine. J Oral Rehabil. 1997;24(1):8-14.
8. Bertschinger C, Paul SJ, Luthy H, et al. Dual application of dentin bonding agents: effect on bond strength. Am J Dent. 1996; 9(3):115-9.
9. Mbodyin R, Paul SJ, Luthy H, et al. Dentin bond strength of Dyract Cem. Am J Dent. 1997;10(1):27-31.
10. Nakabayashi N, Kojima K, Masuhara E. The promotion of adhesion by the infiltration of monomers into tooth substrates. J Biomed Mater Res. 1982;16(3):265-73
About the Authors
Douglas A. Terry, DDS
Assistant Professor
Depbodyment of Restorative Dentistry and Biomaterials
University of Texas Health Science Center, Dental Branch
Houston, Texas
Adjunct Faculty
University of California, Los Angeles, Center for Esthetic Dentistry
Private Practice-Esthetic and Restorative Dentistry
Houston, Texas