Bilateral Maxillary Paramolars in an Adolescent
Preetika Chandna, MDS, MSc; Nikhil Srivastava, MDS, FICD, FDS-RCPS (Glasg); Vivek K. Adlakha, MDS; and Vrinda Sharma
Abstract
Paramolars are relatively uncommon supernumerary molars. Limited cases of bilateral maxillary or mandibular paramolars have been reported. This case report describes bilateral maxillary premolars and their management in a 15-year-old girl, whose chief complaint was food lodgment in these regions. After a diagnosis of bilateral maxillary premolars was made and confirmed by orthopantomogram, both of the paramolars were extracted.
Supernumerary teeth (ST), or hyperdontia, is defined as any tooth or tooth substance in excess of the usual configuration of the normal number of primary or permanent teeth.1 Alternatively, ST may be defined as the teeth that exceed the normal dental formula, independent of their location and form.2,3 Unlike supplemental teeth, ST generally do not resemble the teeth with which they are associated.1
Though ST may occur in either the primary or permanent dentition,4 they are more common in the permanent dentition, with a prevalence of 1.5% to 3.5%.5 In the primary dentition, they show a frequency of 0.3% to 0.8%.5 The prevalence of ST in the molar area ranges from 0.18% to 0.33%.6,7
In the permanent dentition, ST may be located in any area of the maxilla or mandible and are frequently located on the maxillary midline.7 In the primary dentition, ST are commonly located in the maxillary incisor area.8 ST may occur singly, multiply, unilaterally, or bilaterally, and in one or both jaws.6 The prevalence of a single ST is 76% to 86% of cases, two ST is 12% to 23%, and 1% of individuals have multiple (ie, more than 3) ST.9
A number of theories, primarily involving genetic and developmental influences, have been proposed to explain the development of ST. These include atavism (evolutionary throwback), tooth germ dichotomy, genetic and environmental factors, and hyperactivity of the dental lamina.7,10,11 ST may be transmitted as an autosomal dominant or autosomal recessive trait with incomplete penetrance, or may be associated with the X-linked disorders.12 Nonetheless, the specific etiology of ST is still unclear. The most common view is that ST develop as a result of horizontal proliferation or hyperactivity of the dental lamina.7
Paramolars most likely develop because of local, independent, and conditioned hyperactivity of the dental lamina.13 According to this theory, the lingual extension of an additional tooth bud results in the formation of a eumorphic tooth. However, the rudimentary form originates through proliferation of epithelial remnants of the dental lamina that are, in turn, induced by the pressure of the complete dentition.14 The development of ST may also be considered multifactorial.15
ST may be classified on the basis of number, morphology, or topography. On the basis of number, they may be single or multiple.11 Morphologically, ST may be supplemental (eumorphic or normal in appearance) or rudimentary (dysmorphic or variant appearance from normal teeth). Further morphologic classification of the dysmorphic type of ST include conical, tuberculate, and molariform types.16 Topographically, ST occurring in the anterior region, between the maxillary incisors, are called mesiodens.8 ST occurring in the molar area may be categorized as parapremolars, paramolars, or distomolars.8 A paramolar is frequently a small and dysmorphic ST located buccally or palatally/lingually to one of the molar teeth. Paramolars have been reported to occur more often in the mandible than the maxilla.17 Distomolars (sometimes called fourth molars) are positioned distal or disto-lingual to the third molars.16 The orientation of ST may be vertical, inverted, or transverse.1
Paramolars are relatively uncommon supernumerary anomalies occurring in the molar series with a prevalence of 0.09% to 0.29%.18 Paramolars primarily occur singly; bilateral occurrence is rare.18 Very few cases of bilateral paramolars have been reported in the literature.17,19 This case report describes the incidence and management of bilateral paramolars in a 15-year-old girl.
Case Report
With her parents, a 15-year-old girl presented to the department of Pedodontics and Preventive Dentistry, Subharti Dental College and Hospital, Meerut, India with the chief complaint of food lodgment in the bilateral maxillary molar regions. Both her medical and family histories were noncontributory. Written informed consent was obtained from her parents before examination and treatment.
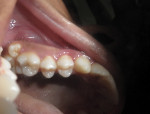
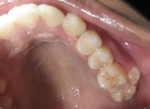
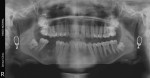
On clinical examination, bilateral supernumerary teeth (Figure 1 and Figure 2) were found in buccal relation to the maxillary first and second molars. The location of the supernumerary teeth suggested a diagnosis of maxillary bilateral paramolars, which was confirmed by an orthopantomogram (OPG) radiograph (Figure 3). Clinical examination of the left and right maxillary first and second molars revealed normal morphology with the expected buccolingual and mesiodistal width of each crown as compared with its contralateral counterpart. This finding suggested lack of fusion with the adjacent paramolars.
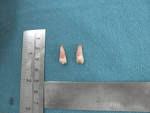
Both bilateral paramolars were then extracted under local anesthesia with vasoconstrictor (lignocaine hydrochloride 21.3 mg with adrenaline 0.005 mg). Extraction was carefully performed with left and right maxillary forceps to prevent damage to the adjacent permanent teeth, which may cause ankylosis and maleruption of these teeth. The possible clinical complications of such extraction include damage to the blood vessels and nerves during manipulation of the paramolar, perforation of the maxillary sinus, the pterygomaxillary space, or the orbit, and fracture of the maxillary tuberosity. The extracted bilateral paramolars (Figure 4) were dysmorphic and conical in morphology and single-rooted with three poorly developed cusps. In conjunction with a periodontist, the sockets were treated with a guided bone regeneration procedure using cancellous bone graft to assure full soft-tissue attachment and avoid postoperative periodontal pocket defects. Soft-tissue closure was achieved with interrupted sutures using 3.0 silk. Oral hygiene instructions were explained carefully to the patient and her family. The healing of the postoperative extraction sockets was uneventful.
An additional radiographic finding was a cystic lesion in the region of the missing mandibular right permanent first molar. This large radiolucency was suspected to be a dentigerous cyst or odontogenic keratocyst. This lesion was subsequently enucleated by an oral and maxillofacial surgeon and was determined by histopathologic diagnosis to be an odontogenic keratocyst.
Discussion
Paramolars are usually small and rudimentary or dysmorphic and located buccal or lingual to a maxillary molar.18 In this patient, the bilateral paramolars were dysmorphic and conical.
Multiple ST may be associated with syndromes such as cleft lip and palate, Gardner syndrome, cleidocranial dysostosis, Fabry disease, Ellis-van Creveld syndrome (chondroectodermal dysplasia), Ehlers-Danlos syndrome, Rubinstein-Taybi syndrome, Nance-Horan syndrome, incontinentia pigmenti, and tricho-rhino-phalangeal syndrome.20,21 More common among these are cleft lip and palate, cleidocranial dysostosis, and Gardner syndrome.20 However, the patient in this case showed nonsyndromic bilateral paramolars. Multiple ST without developmental or syndromic involvement (as in this patient) is rare.18
ST can be found in almost any region of the dental arch, though they have a striking predilection for maxilla over mandible.18 Nonsyndromic multiple ST are more common in the mandible and in the premolar region, however, followed by the molar and anterior regions.20 In the present patient, the bilateral ST were located in the maxillary arch. Although this patient was a girl, males are affected twice as commonly as females.9
ST such as paramolars may be diagnosed during a routine, clinical, or radiographic evaluation and usually do not cause any discernable side effects on neighboring teeth.6 They may sometimes trigger a variety of complications such as delayed eruption, noneruption, crowding, or displacement (including rotations of permanent teeth), as well as, though less frequently, development of odontogenic cysts or resorption of neighboring teeth.6 Delayed eruption is the most common complication of ST.22 In the present case, the patient’s chief complaint was food lodgment in relation to the bilateral paramolars.
Conventionally, 2D radiographs have been used to view paramolars. The OPG is a highly useful radiograph to view ST such as paramolars, along with additional views of the anterior maxilla and mandible in the form of occlusal or periapical radiographs.18 In the present case, an OPG was used to view the bilateral maxillary paramolars. Recent advances in radiography, such as cone-beam computed tomography (CBCT), have also been helpful for viewing ST.23 CBCT allows 3D imaging and may accurately predict the location of ST as well as surrounding structures.
The differential diagnosis of paramolars includes supernumerary structures in maxillary molars, such as fused supernumerary tooth and paramolar tubercle, occurring on buccal surfaces of both maxillary and mandibular molars.17 The paramolar tubercle was first described by Bolk in 1916.24 This structure is commonly present on the buccal surface of the mesiobuccal cusp or paracone and occasionally on the distobuccal cusp or metacone. It is a derivative of the cingulum and must be differentiated from paramolar teeth.18
The management strategy of a paramolar is governed by associated syndromes, position of the tooth, potential effect on adjacent structures and associated malocclusions, caries, and periodontal pathology.8 Clinical cases similar to the present one have been reported previously in the literature.16,17,25 The management options for a paramolar include observation, both clinically and radiographically, if asymptomatic, or extraction.18 If the paramolar is symptomatic, as in the present case in which food lodgment was associated with the bilateral paramolars, extraction is the recommended treatment option. Regular follow-up was required for this patient to ensure no future complications.
Conclusion
Paramolars are a relatively rare type of supernumerary teeth, with their bilateral occurrence even more so. Awareness of paramolars and their management may assist dentists in understanding the potential problems they cause and their management options.
About the Authors
Preetika Chandna, MDS, MSc
Professor
Department of Pedodontics and Preventive Dentistry
Subharti Dental College
Swami Vivekanand Subharti University
Meerut, Uttar Pradesh, India
Nikhil Srivastava, MDS, FICD, FDS-RCPS (Glasg)
Professor and Head
Department of Pedodontics and Preventive Dentistry
Principal and Dean
Subharti Dental College
Swami Vivekanand Subharti University
Meerut, Uttar Pradesh, India
Vivek K. Adlakha, MDS
Professor
Department of Pedodontics and Preventive Dentistry
Subharti Dental College
Swami Vivekanand Subharti University
Meerut, Uttar Pradesh, India
Vrinda Sharma
Third-year Postgraduate Resident
Department of Pedodontics and Preventive Dentistry
Subharti Dental College
Swami Vivekanand Subharti University
Meerut, Uttar Pradesh, India
References
1. Rajab LD, Hamdan MA. Supernumerary teeth: review of the literature and a survey of 152 cases. Int J Paediatr Dent. 2002;12(4):244-254.
2. Hattab FN, Yassin OM, Rawashedeh MA. Supernumerary teeth: report of three cases and review of the literature. ASDC J Dent Child. 1994;61(5-6):382-393.
3. Zhu JF, Marcushamer M, King D, Henry RJ. Supernumerary and congenitally absent teeth: a literature review. J Clin Pediatr Dent. 1996;20(2):87-95.
4. Ata-Ali F, Ata-Ali J, Peñarrocha-Oltra D, Peñarrocha-Diago M. Prevalence, etiology, diagnosis, treatment and complications of supernumerary teeth. J Clin Exp Dent. 2014;1;6(4):e414-e418.
5. Mason C, Azam N, Holt RD, Rule DC. A retrospective study of unerupted maxillary incisors associated with supernumerary teeth. Br J Oral Maxillofac Surg. 2000;38(1):62-65.
6. Kara Mİ, Aktan AM, Ay S, et al. Characteristics of 351 supernumerary molar teeth in Turkish population. Med Oral Patol Oral Cir Bucal. 2012;17(3):e395-e400.
7. Cassetta M, Altieri F, Giansanti M, et al. Morphological and topographical characteristics of posterior supernumerary molar teeth: an epidemiological study on 25,186 subjects. Med Oral Patol Oral Cir Bucal. 2014;19(6):e545-e549.
8. Solares R, Romero MI. Supernumerary premolars: a literature review. Pediatr Dent. 2004;26(5):450-458.
9. Fernández Montenegro P, Valmaseda Castellón E, Berini Aytés L, Gay Escoda C. Retrospective study of 145 supernumerary teeth. Med Oral Patol Oral Cir Bucal. 2006;11(4):e339-e344.
10. De Oliveira Gomes C, Drummond SN, Jham BC, et al. A survey of 460 supernumerary teeth in Brazilian children and adolescents. Int J Paediatr Dent. 2008;18(2):98-106.
11. Garvey MT, Barry HJ, Blake M. Supernumerary teeth – an overview of classification, diagnosis and management. J Can Dent Assoc. 1999;65(11):612-616.
12. Marya CM, Kumar BR. Familial occurrence of mesiodentes with unusual findings: case reports. Quintessence Int. 1998;29(1):49-51.
13. Primosch RE. Anterior supernumerary teeth—assessment and surgical intervention in children. Pediatr Dent. 1981;3(2):204-215.
14. Sykaras SN. Mesiodens in primary and permanent dentitions. Report of a case. Oral Surg Oral Med Oral Pathol. 1975;39(6):870-874.
15. Rao PV, Chidzonga MM. Supernumerary teeth: literature review. Cent Afr J Med. 2001;47(1):22-26.
16. Parolia A, Kundabala M. Bilateral maxillary paramolars and endodontic therapy: a rare case report. J Dent (Tehran). 2010;7(2):107-111.
17. Nagaveni NB, Umashankara KV, Radhika NB, et al. Maxillary paramolar: report of a case and literature review. Arch Orofac Sci. 2010;5(1):24-28.
18. Nayak G, Shetty S, Singh I, Pitalia D. Paramolar - A supernumerary molar: a case report and an overview. Dent Res J (Isfahan). 2012;9(6):797-803.
19. Sulabha AN, Sameer C. Unusual bilateral paramolars associated with clinical complications. Case Rep Dent. 2015;2015:851765.
20. Açikgöz A, Açikgöz G, Tunga U, Otan F. Characteristics and prevalence of non-syndrome multiple supernumerary teeth: a retrospective study. Dentomaxillofac Radiol. 2006;35(3):185-190.
21. Subasioglu A, Savas S, Kucukyilmaz E, et al. Genetic background of supernumerary teeth. Eur J Dent. 2015;9(1):153-158.
22. Seddon RP, Johnstone SC, Smith PB. Mesiodentes in twins: a case report and a review of the literature. Int J Paediatr Dent. 1997;7(3):177-184.
23. Liu DG, Zhang WL, Zhang ZY, et al. Three-dimensional evaluations of supernumerary teeth using cone-beam computed tomography for 487 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;103(3):403-411.
24. Bolk L. Problems of human dentition. Am J Anat. 1916;19(1):91-148.
25. Omal PM, Jacob V, Lonapan J, Kurian A. Bilateral fourth molars with paramolars in maxilla. Kerala Dental Journal. 2011;34(2):277-279.