Advanced Immediate Functional Loading: Requirements for Long-Term Success in Modern Implant Dentistry
Abstract: There are benefits to be derived from the use of advanced surgical protocols in conjunction with immediate functional loading using various dental implant designs and implant–abutment connections. Clinical protocols with simultaneous bone grafting, immediate implant placement, and/or sinus augmentations when a shortened treatment period is needed are included in this report, with the aim of providing understanding of the main protocol characteristics and prerequisites for long-term success in implant dentistry. This article presents three clinical cases that illustrate possibilities for advanced immediate loading using different implant designs. It demonstrates treatment of severe bone defects and the facilitation of placing implants in regenerated bone that can be immediately loaded.
The immediate loading (IL) concept in the intraforaminal part of the mandible whereby four primary stable implants are inserted and connected using a bar immediately after placement and loaded with an overdenture has been extensively documented.1,2 The general rule of this treatment concept is to control micromotions at the bone–implant interface when implants are loaded. Implant length, appropriate thread design, surface roughness, and an excellent osteotomy procedure are main factors to maximize primary (mechanical) implant stability. Additional strategies, such as reduction of loading forces and recommendations for soft/liquid diet at the initial stages of healing, have been suggested in order to achieve stability at the bone–implant interface and implant integration.3-7 Moreover, some authors increased the number of implants so as to distribute loading forces4 using rigid immobilization with fixed restorations.4,5,8-13 Transitional (ie, secondary) implants have also been used for immediate loading and temporary rehabilitation and were splinted later with submerged, healed (ie, primary) implants.5,14,15
Recent studies, however, have suggested the use of different types of restorations in the mandible using prefabricated abutments, splinted together utilizing a removable bridge and immediate loading.7,16,17
Primary Implant Stability
Primary (initial) stability (PS) is related to the level of primary bone–implant contacts at the interface during implant placement. Primary stability is an important determinant of implant survival,18,19 especially when implants are loaded immediately after surgery.20 PS is the absence of mobility in the bone bed upon insertion of the implant and depends on the quantity and quality of bone, surgical technique, and implant design.19 There are varying scientific opinions regarding factors that influence PS. For example, some studies demonstrate that length, geometry, and surface area of the implant and bone-to-implant contacts at the histologic level influence PS,21 while others state that implant PS is determined by the bone density, implant design, and surgical technique.22
Implant design and its association with PS has been evaluated by many scientific groups. A study showed results of implants on beagle dogs with no statistically significant differences in bone formation between cylindrical and tapered implant designs when placed using the non-submerged technique.22 Implants with different geometries and similar diameters have shown no differences in strain levels on surrounding bone.23 Improved stability with tapered implant designs versus cylindrical implants was also reported in different studies.24-26
Initial stability seems to be dependent on the bone quality and the surgical technique.27,28 A positive correlation between implant PS and bone density at the osteotomy site was demonstrated in a systematic review.29 However, the use of narrow-diameter drills in poor bone quality may improve the primary implant stability.30
The clinical assessment of implant stability has been evaluated by objective methods, such as the Periotest® device (Medizintechnik Gulden, www.med-gulden.com) with Periotest values (PTV) and the Osstell® device (Osstell, www.ostell.com), which provides a resonance frequency analysis (RFA) with implant stability quotient (ISQ) values. Using RFA, O’Sullivan et al24 demonstrated in a human cadaver study higher PS for tapered designed implants (compared to non-tapered) independent of bone quality. Similarly, Glauser et al31 found significantly higher RFA values and insertion torques for tapered implants than cylindrical. Recent studies using tapered designed implants placed in vitro achieved greater PS than those with a parallel design. Both experienced and inexperienced clinicians consistently achieved PS; however, experienced clinicians achieved higher ISQ values with tapered implants in poor-quality bone.28
Based on the critical analysis of the literature and the author’s own clinical experience, the immobilization of implants and the strength of the implant–abutment connection seem to be significant factors in achieving clinical success using the immediate loading concept.32 This is of special benefit when implants have to be placed in sites with weak bone quality and slight bone volume (eg, soft bone, augmented sites, immediate implant placement, etc) and have to be loaded immediately after their insertion.
In clinical conditions with bone dehiscences (or fenestrations), where bone grafting is needed, implants with good PS may be used but they cannot be loaded immediately if the implants are not clinically stable when abutments are connected in situ. The high friction of the implant–abutment interface requires less torque for providing a sealing at the connection and, therefore, allows a large variety of clinical options with immediate loading. Immediate functional loading cases in conjunction with simultaneous sinus lift procedures or implant placement in fresh extraction sockets, implant placement with simultaneous bone grafting, immediate loading of implants without direct splinting,17 or implants connected with teeth using a secondary splinting7,33 are some clinical protocols requiring advanced surgical and prosthetic skills but also use of implant designs with excellent PS.
Conical Connections
Morse-tapered (conical) connections seem to be mechanically more stable under loading conditions34 even when implants are splinted together35 and are associated with less crestal bone loss compared to other internal or external butt-joint connections. Biological considerations, such as trauma during surgery (ie, bone planing to create space for the restoration), are associated with crestal bone loss and these are not related to the use of a specific implant design with or without platform-switching.35 In general, it is well known that external hexagons present a microgap associated with bacterial accumulation and inflammatory reactions in the surrounding tissues.36 Even earlier studies showed leakage between different implant–abutment connections in vitro37; recent studies have presented a better sealing at Morse-tapered connections38,39 and these systems have been introduced by different manufacturers today. It should be emphasized that, in general, not every conical connection is a Morse-tapered connection, and the exact angle of the surfaces (abutment–implant interface) should be determined in order to provide excellent sealing and improved abutment stability.
Implants with Morse-tapered connections and concepts of one-abutment at one time40,41 with (or without) subcrestal implant placement41 have been evaluated by different researchers to control crestal bone loss. Other authors do not see advantages of such treatment concepts with platform-switching based on dog studies. Specifically, flap surgery and subcrestal implant placement, implant technology comparing platform shift/switch with standard abutments, surgical approach, and abutment selection seem to have a limited impact on crestal remodeling, associated bone loss, and mucosal profile.42 Also, when immediate implants were placed subcrestally in dogs, the biological width dimension was in a most coronal position, but it did not have any effect on minimizing the marginal bone loss.43
In a recent clinical study using two different implant designs with platform-switching but with different implant–abutment connections (butt-joint and Morse-tapered) in the same patients, a bacterial composition similar to periodontitis and peri-implantitis was found when implant designs had the butt-joint connection even when chlorhexidine for decontamination at the implant–abutment interface was used.44
In a previous clinical study, telescopic abutments were used in the mandible for implant-supported restorations and immediate loading. Four implants were placed and connected with prefabricated telescopic abutments (4-degree angle). The implants were loaded immediately after insertion.16,17 Prefabricated secondary copings were inserted in the prosthesis. Using this treatment concept in the mandible, a high survival rate was reported after 2 years of loading with a maximum of 129 months of loading period.17 A similar clinical concept with immediate loading was used in the maxilla when implants, splinted together with periodontally healthy teeth, using a telescopic-retained prosthesis showed a high success rate for implants and residual teeth with a predictable clinical outcome improving the esthetic result and plaque control.33
Clinical Cases
The present report demonstrates benefits of advanced surgical protocols in conjunction with immediate functional loading using different implant designs and implant–abutment connections. Clinical protocols with simultaneous bone grafting, immediate implant placement, and/or sinus augmentations when the treatment period has to be reduced and that avert biological complications and implant failures are included in this report. The aim is to provide understanding of the main protocol characteristics and discuss prerequisites for long-term success. Further advanced protocols in conjunction with immediate functional loading have been published7 and the role of loading forces around immediately loaded implants to improve wound healing and bone formation was reported in a recent comprehensive paper.45
The three clinical cases presented here illustrate possibilities of advanced immediate loading using different implant designs.
Case 1
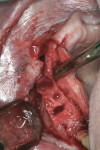
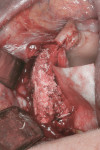
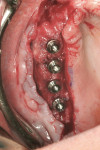
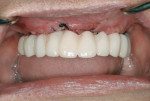
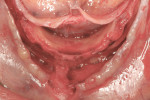
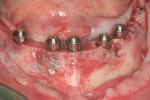
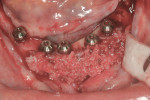
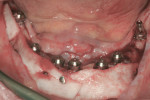
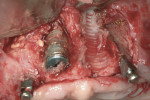
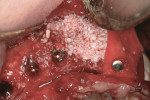
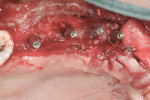
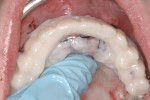
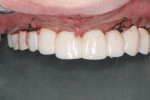
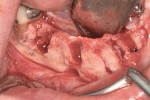
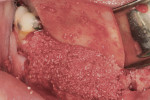
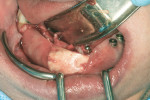
The first case demonstrates bone grafting in the maxilla (Figure 1 through Figure 4) and mandible (Figure 5 through Figure 11) (including sinus augmentation with a lateral window on the left side) and, after 5 months of healing, implant placement (Bone Level®, Straumann, www.straumann.us) with multi-base abutments and a screw-retained provisional restoration for immediate functional loading. In the mandible, the implants were placed with a simultaneous buccal augmentation with cancellous allograft (Puros®, Zimmer Dental, www.zimmerdental.com) and immediate loading. The final screw-retained prostheses were delivered (at the Department of Prosthodontics, Eastman Institute for Oral Health, University of Rochester [NY] Medical Center) 9 months after loading. The final result 2 years after loading showed excellent crestal bone maintenance and a successful clinical outcome.
Case 2
The second clinical case demonstrates removal of clinically stable implants placed in a foreign country in positions difficult to restore prosthetically. Moreover, the implant system that had been used was not FDA approved, and, therefore, the prosthetic components were not available in the United States.
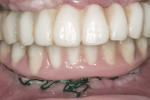
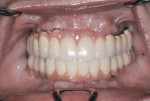
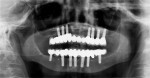
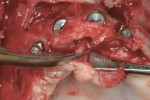
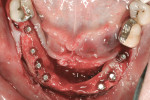
Advanced bone grafting was performed with a combination of autogenous bone and bone mineral (cancellous BioOss®, Geistlich, www.geistlich-na.com) covered by a collagen membrane (BioMend® Extend™, Zimmer Dental), immobilized with titanium tags (Salvin Dental, www.salvin.com). After 4 months of healing, Ankylos® implants (DENTSPLY Implants, www.dentsplyimplants.com) were placed and loaded using standard abutments. The provisional prosthesis (cement-retained) was delivered the day of surgery and fabricated chairside using temporary cement and a vacuum-form machine. In a similar approach, implants were removed in the mandible, and vertical and horizontal bone augmentations with coronal flap advancement for tension-free closure were performed.
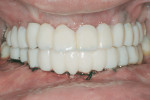
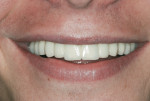
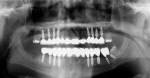
Five months later, implants were placed and connected with their respective abutments for immediate loading. These abutments were never removed and impressions were taken for the final prosthesis using prefabricated impression copings and implant analogues. Fixed prostheses were delivered and cemented with provisional cement material (Temp-Bond®, Kerr Dental, www.kerrdental.com) for follow-up evaluation of the implants. The final clinical and radiographic evaluation showed an excellent result, and the patient was very happy with the outcome. This case is depicted in Figure 12 through Figure 25.
Case 3
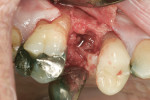
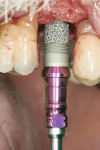
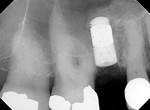
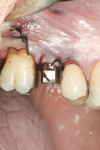
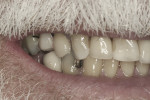
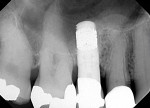
The third case demonstrates a clinical situation after a tooth extraction (tooth No. 4) and, 2 weeks after healing (because the patient could not wait longer due to relocation), implant placement (Ø 4.1 mm/10 mm, Trabecular Metal™ [TM], Zimmer Dental) with a simultaneous osteotome technique (vertical augmentation from the socket) and abutment connection (friction fit) for immediate functional loading. The provisional crown was cemented, and a soft/liquid diet was recommended for a period of 2 to 3 months. The final prosthesis was fabricated outside the mouth to remove the initial abutment using an impression coping and an abutment analogue. A final metalo-ceramic crown was cemented 3 months after loading. The implant presented excellent clinical stability and maintenance of the peri-implant soft and hard tissues at the 1-year follow-up (Figure 26 through Figure 31).
This implant design (slightly tapered) with a tantalum pattern in the middle portion of the implant allows significant improvement of biological stability due to faster bone formation within the porous tantalum-based cylinder.46 However, advanced surgical skills in such cases are required to improve the initial stability, especially when single-tooth implants are placed in fresh extraction sockets.
Conclusion
In conclusion, clinicians who are successfully using the immediate loading concept in their practice may improve the applications of this biological concept, when:
implant systems with great initial implant stability are used
micromotions at the bone–implant interface are avoided
high primary contacts between implant surface and surrounded bone are attempted
implant–abutment connection with high stability (using low torque for sealing) is used, and
soft/liquid diet at the initial stages of healing is recommended
Current developments in implant dentistry with new surfaces and implant designs, platform geometries, and implant–abutment connections may improve crestal bone stability. This may better control biological complications, reduce the entire treatment period, and improve the final esthetic outcome.
ACKNOWLEDGMENTS
The author would like to thank the residents involved in some of the procedures of these cases, including Drs. B. Baig, G. Ciornei, A. Kashi, and M. Palermo (Rochester, New York).
ABOUT THE AUTHOR
Georgios E. Romanos, DDS, PhD, Prof. Dr. med. dent.
Professor, Department of Periodontology, Stony Brook University, School of Dental Medicine, Stony Brook, New York
REFERENCES
1. Ledermann PD. Über 20-jährige erfahrung mit der sofortigen funktionellen belastung von implantatstegen in der Regio interforaminalis. Z Zahnärztl Implantol. 1996;12(3):123-136.
2. Chiapasco M, Gatti C, Rossi E, et al. Implant-retained mandibular overdentures with immediate loading. A retrospective multicenter study on 226 consecutive cases. Clin Oral Implants Res. 1997;8(1):
48-57.
3. Salama H, Rose LF, Salama M, Betts NJ. Immediate loading of bilaterally splinted titanium root-form implants in fixed prosthodontics—a technique reexamined: two case reports. Int J Periodontics Restorative Dent. 1995;15(4):344-361.
4. Balshi TJ, Wolfinger GJ. Two-implant-supported single molar replacement: interdental space requirements and comparison to alternative options. Int J Periodontics Restorative Dent. 1997;17(5):427-435.
5. Tarnow DP, Emtiaz S, Classi A. Immediate loading of threaded implants at stage 1 surgery in edentulous arches: ten consecutive case reports with 1- to 5-year data. Int J Oral Maxillofac Implants. 1997;12(3):319-324.
6. Szmukler-Moncler S, Salama H, Reingewirtz Y, Dubruille JH. Timing of loading and effect of micromotion on bone-dental implant interface: review of experimental literature. J Biomed Mater Res. 1998;43(2):
192-203.
7. Romanos GE. Advanced Immediate Loading. Chicago, IL: Quintessence Publishing Co. Inc.; 2012.
8. Horiuchi K, Uchida H, Yamamoto K, Sugimura M. Immediate loading of Brånemark system implants following placement in edentulous
patients: a clinical report. Int J Oral Maxillofac Implants. 2000;15(6):
824-830.
9. Randow K, Ericsson I, Nilner K, et al. Immediate functional loading of Brånemark dental implants. An 18-month clinical follow-up study. Clin Oral Implants Res. 1999;10(1):8-15.
10. Ganeles J, Rosenberg MM, Holt RL, Reichman LH. Immediate loading of implants with fixed restorations in the completely edentulous mandible: report of 27 patients from a private practice. Int J Oral Maxillofac Implants. 2001;16(3):418-426.
11. Degidi M, Piattelli A. Immediate functional and non-functional loading of dental implants: a 2- to 60-month follow-up study of 646 titanium implants. J Periodontol. 2003;74(2):225-241.
12. Testori T, Meltzer A, Del Fabbro M, et al. Immediate occlusal loading of Osseotite implants in the lower edentulous jaw. A multicenter prospective study. Clin Oral Implants Res. 2004;15(3):278-284.
13. Romanos GE, Nentwig GH. Immediate functional loading in the maxilla using implants with platform switching: five-year results. Int J Oral Maxillofac Implants. 2009;24(6):1106-1112.
14. Schnitman PA, Wöhrle PS, Rubenstein JE, et al. Ten-year results for Brånemark implants immediately loaded with fixed prostheses at implant placement. Int J Oral Maxillofac Implants. 1997;12:495-503.
15. Froum SJ, Simon H, Cho SC, et al. Histologic evaluation of bone-implant contact of immediately loaded transitional implants after 6 to 27 months. Int J Oral Maxillofac Implants. 2005;20(1):54-60.
16. May D, Romanos GE. Immediate implant-supported mandibular overdentures retained by conical crowns: a new treatment concept. Quintessence Int. 2002;33(1):5-12.
17. Romanos GE, May S, May D. Treatment concept of the edentulous mandible with prefabricated telescopic abutments and immediate functional loading. Int J Oral Maxillofac Implants. 2011;26(3):593-597.
18. Cochran DL, Schenk RK, Lussi A, et al. Bone response to unloaded and loaded titanium implants with a sandblasted and acid-etched surface: a histometric study in the canine mandible. J Biomed Mater Res. 1998;40(1):1-11.
19. Nkenke E, Hahn M, Weinzierl K, et al. Implant stability and histomorphometry: a correlation study in human cadavers using stepped cylinder implants. Clin Oral Implants Res. 2003;14(5):601-609.
20. Javed F, Romanos GE. The role of primary stability for successful immediate loading of dental implants. A literature review. J Dent. 2010;38(8):612-620.
21. Meredith N. Assessment of implant stability as a prognostic determinant. Int J Prosthodont. 1998;11(5):491-501.
22. Glauser R, Sennerby L, Meredith N, et al. Resonance frequency analysis of implants subjected to immediate or early functional occlusal loading. Successful vs. failing implants. Clin Oral Implants Res. 2004;15(4):428-434.
23. del Valle V, Faulkner G, Wolfaardt J. Craniofacial osseointegrated implant-induced strain distribution: a numerical study. Int J Oral Maxillofac Implants. 1997;12(2):200-210.
24. O’Sullivan D, Sennerby L, Meredith N. Measurements comparing the initial stability of five designs of dental implants: a human cadaver study. Clin Implant Dent Relat Res. 2000;2(2):85-92.
25. Sakoh J, Wahlmann U, Stender E, et al. Primary stability of a conical implant and a hybrid, cylindric screw-type implant in vitro. Int J Oral Maxillofac Implants. 2006;21(4):560-566.
26. Romanos GE, Ciornei G, Jucan A, et al. In vitro assessment of primary stability of Straumann® implant designs. Clin Implant Dent Related Res. 2014;16(1):89-95.
27. Wilmes B, Rademacher, C, Olthoff, G, Drescher D. Parameters affecting primary stability of orthodontic mini-implants. J Orofac Orthrop. 2006;67(3):162-174.
28. Romanos GE, Basha-Hijazi A, Gupta B, et al. Role of clinician’s experience and implant design on implant stability. An ex-vivo study in artificial soft bones. Clin Implant Dent Relat Res. 2014;16(2):166-171.
29. Marquezan M, Osório A, Sant’Anna E, et al. Does bone mineral density influence the primary stability of dental implants? A systematic review. Clin Oral Implants Res. 2012;23(7):767-774.
30. Turkyilmaz I, Aksoy U, McGlumphy EA. Two alternative surgical techniques for enhancing primary implant stability in the posterior maxilla: a clinical study including bone density, insertion torque, and resonance frequency analysis data. Clin Implant Dent Relat Res. 2008;10(4):231-237.
31. Glauser R, Lundgren AK, Gottlow J, et al. Immediate occlusal loading of Brånemark TiUnite implants placed predominantly in soft bone: 1-year results of a prospective clinical study. Clin Implant Dent Relat Res. 2003;5(suppl 1):47-56.
32. Romanos GE. Bone quality and the immediate loading of implants-critical aspects based on literature, research, and clinical experience. Implant Dent. 2009;18(3):203-209.
33. Romanos GE, May S, May D. Implant-supporting telescopic maxillary prostheses and immediate loading [published online ahead of print September 21, 2012]. Clin Implant Dent Relat Res. 2012. doi: 10.111/cid.12003.
34. Zipprich H, Weigl P, Lange B, Lauer HC. Erfassung, Ursachen und Folgen von Mikrobewegungen am Implantat-Abutment-Interface. Implantologie. 2007;15(1):31-46.
35. Romanos GE, Malmstrom H, Feng C, et al. Immediately loaded platform-switched implants in the anterior mandible with fixed prostheses: a randomized, split-mouth, masked prospective trial [published online ahead of print March 28, 2013]. Clin Implant Dent Relat Res. 2013. doi: 10.1111/cid.12065.
36. Ericsson I, Persson LG, Berglundh T, et al. Different types of inflammatory reactions in peri-implant soft tissues. J Clin Periodontol. 1995;22(3):255-261.
37. Coelho PG, Sudack P, Suzuki M, et al. In vitro evaluation of the implant abutment connection sealing capability of different implant systems. J Oral Rehabil. 2008;35(12):917-924.
38. Jaworski ME, Melo AC, Picheth CM, Sartori IA. Analysis of the bacterial seal at the implant-abutment interface in external-hexagon and Morse taper-connection implants: an in vitro study using a new methodology. Int J Oral Maxillofac Implants. 2012;27(5):1091-1095.
39. Dʼercole S, Tripodi D, Ravera L, et al. Bacterial leakage in morse cone internal connection implants using different torque values: an in vitro study. Implant Dent. 2014;23(2):175-179.
40. Degidi M, Nardi D, Piattelli A. One abutment at one time: non-removal of an immediate abutment and its effect on bone healing around subcrestal tapered implants. Clin Oral Implants Res. 2011;22(11):1303-1307.
41. Romanos GE, Aydin E, Gärtner K, Nentwig GH. Long-term results after subcrestal or crestal placement of delayed loaded implants [published online ahead of print May 15, 2013]. Clin Implant Dent Relat Res. 2013. doi: 10.1111/cid.12084.
42. Wenzel BA, Gamborena I, Lee J, et al. Effect of platform shift on crestal bone levels and mucosal profile following flap surgery and subcrestal implant placement in presence/absence of gap defects. Clin Implant Dent Relat Res. 2014. doi: 10.1111/cid.12216.
43. Negri B, López Marí M, Maté Sánchez de Val JE, et al. Biological width formation to immediate implants placed at different level in relation to the crestal bone: an experimental study in dogs [published online ahead of print February 6, 2014]. Clin Oral Implants Res. 2014.doi: 10.1111/clr.12345.
44. Romanos GE, Biltucci MT, Kokaras A, Paster B. Bacterial composition at the implant-abutment connection under loading in vivo. Clin Implant Dent Related Res. (submitted).
45. Romanos GE. Wound healing in immediately loaded implants. Periodontol 2000. In press.
46. Lee JW, Battula S, Wen HB, et al. Faster bone formation within Tantalum-based porous engineered dental implant. Poster presented at: Academy of Osseointegration Annual Meeting; March 6-8, 2014; Seattle, WA.