An Update on Adhesive Dentistry
State-of-the-art current adhesives—Manufacturers have adopted an etch-and-rinse approach or a self-etch approach in the design of adhesives for bonding restorative materials to tooth structures, which differ in how these adhesives interact with dental hard tissues. Etch-and-rinse adhesives are offered as two- or three-step systems, depending on whether primer and bonding are separate or combined in a single bottle. Likewise, self-etch adhesives are available as one- or two-step systems. Etch-and-rinse adhesives are often preferred when large areas of enamel are still present, while self-etch adhesives provide more predictable bonds to dentin.
Despite current trends toward fewer and simpler application steps, one-step adhesive systems appear to be less predictable than multi-step etch-and-rinse and self-etch systems. Some manufacturers have recently introduced more versatile single-bottle “universal” or “multi-mode” adhesives that encompass self-etch chemistry but also enable the same adhesive to be used with phosphoric acid-etching in the etch-and-rinse mode. Some universal adhesives also incorporate silane primer for chemical bonding to silica-based ceramics, and methacryloyloxydecyl dihydrogen phosphate (MDP) for chemical bonding to zirconia-based ceramics. Because clinical studies on universal adhesives are short-term, they cannot be considered state-of-the-art in the context of evidence-based dentistry. Conversely, two-step mild, self-etch adhesives have been well-tested in clinical trials and represent the current state-of-the-art for bonding to dentin, with reduced incidence of postoperative sensitivity when compared to etch-and-rinse adhesives.
Development of contemporary adhesives from a researcher’s perspective—The current thinking by researchers is that dentin bonding is not as durable as it was originally perceived. This lack of durability is attributed partially to secondary caries around restorative margins that are devoid of enamel and partially to the degradation of the adhesive joint. The latter may be caused by the hydrolysis of ester bonds in the adhesive component by salivary esterases, or by degradation of water-rich, resin-sparse regions of the hybrid layers by endogenous collagen-bound proteases such as matrix metalloproteinases (MMP) and cathepsin K, that are activated from their dormant preforms to active forms by the acidity of contemporary adhesives. These activated enzymes slowly degrade the denuded collagen matrix within hybrid layers, resulting in gradual loss of adhesion.
Much work has been done in developing therapeutic dental adhesives that are able to resist secondary caries and degradation of the adhesive joint. One of the most thoroughly studied antimicrobial resin monomers is the quaternary ammonium methacrylate developed by Kuraray known as methacryloyloxydodecylpyridinium bromide (MDPB). This polymerizable resin monomer is incorporated in the two-step self-etch adhesive Clearfil™ SE Protect. Recent research has demonstrated that MDPB resin is also an effective inhibitor of both MMP and cysteine cathepsins, thereby providing a mechanism to increase the longevity of resin–dentin bonds by preventing collagen degradation. Indeed, an in-vitro and in-vivo study (Donmez, et al. J Dent Res. 2005;84:355-359) showed that resin–dentin bonds created with Clearfil SE Protect (aka, Clearfil Protect Bond) did not degrade after 1 year when compared with a similar self-etch adhesive that did not incorporate the MDPB resin monomer.
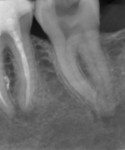
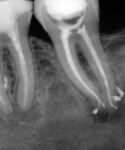
Most common clinical applications of Clearfil SE Protect—As a board-certified endodontist, the author uses Clearfil SE Protect as an antimicrobial adhesive to establish coronal seal after finishing root canal treatment to prevent reinfection of the periradicular tissues via coronal leakage through the filled root canals (Figure 1 and Figure 2). Another common use of Clearfil SE Protect is the restoration of the access cavity prepared through a zirconia-based full-coverage restoration. By taking advantage of the MDP component, the author feels more confident that he can bond to the zirconia with a resin composite without causing leakage along the composite–zirconia interface.
Disclaimer: This article was provided by Dr. Tay.
Kuraray America, Inc.
33 Maiden Lane, Suite 600-D
New York, NY 10038
800-879-1676
dentalaegis.com/go/cced601
Franklin Tay, BDSc (Hons), PhD is Professor and Chair in the Department of Endodontics, College of Dental Medicine, Georgia Regents University, Augusta, Georgia, and a Fellow of the Academy of Dental Materials, as well as a Diplomate of the American Board of Endodontics. With more than 400 papers published in peer-reviewed journals, his research interests include biomineralization of collagen scaffolds with apatite and/or silica, remineralization of resin-dentin bonds, antimicrobial sol-gel chemistry, mesoporous silica, and endodontic materials.