Provisional Material Considerations: Creating a Blueprint of the Final Restorations
Gregg A. Helvey, DDS
Abstract:
Indirect restorative dentistry generally requires temporization of prepared teeth during the laboratory fabrication phase. Over the years, the physical properties of newer provisional materials have improved, which has enabled an expansion of the function of provisional restorations. Better strength, surface finish, and color match have increased their acceptability by patients and clinicians. In some clinical situations provisional restorations can provide information that is critical to the overall success of a case. Such information allows the clinician to verify and confirm with the patient the esthetics, phonetics, and function of the proposed anterior restorative treatment. The provisional restorations can also provide valuable information to the laboratory technician regarding design, contour, length, shade, and even correct articulation of the master model. The success of the definitive restoration is dependent on the accurate transfer of this information to the laboratory technician.
Provisional (interim) restorations can be used to provide valuable information in a number of different clinical scenarios. They can be used to maintain positional stability of prepared teeth, assess the occlusal function when altering the occlusion, and evaluate lateral and protrusive guidance.1 Due to the vast amount of other information they provide, such as color, shape, and contour, provisional or interim restorations are no longer referred to as just “temporaries.”2 When selecting a material for provisional restorations there are numerous factors to consider, including handling properties, patient acceptance, and material cost.3
Correct incisal edge position, lingual and facial contour, maxillary cant (dental midline), and shade selection are critical elements in the success of anterior restorative cases. Several techniques and devices can be used to transfer this pertinent information to the laboratory. Traditionally, the facebow transfer apparatus has been used to provide the laboratory technician with the correct orientation of the master cast in a sagittal, frontal, and horizontal plane during the mounting procedure. Esthetically, the horizontal plane is the most critical in terms of producing the correct dental midline cant that would be immediately observable to the patient. Many dentists do not use a facebow routinely because the procedure can be both intricate and time-consuming.4 Instead, other devices are employed—sometimes successfully, sometimes not—such as “stick bites” with horizontal and/or horizontal-vertical cross-pieces, midline aligners with bubble levels, or bite trays with attached cross-pieces. Other techniques used to transfer incisal edge position without a facebow are interchangeable mounted mock-up and master cast models and silicone indexes.
An alternative method of transferring this information is simply to send a duplicate provisional restoration to the laboratory that when placed on a master cast provides the correct orientation of the dental midline. A duplicate provisional sent to the laboratory can also be used as a template for CAD/CAM scanning or when the laboratory incorporates the wax injection technique in conjunction with ceramic pressing.5-7
A provisional material that has a dual-cure component allows for rapid fabrication of a provisional restoration. Provisional restorations should be a blueprint of the final restorations, providing both the clinician and patient the opportunity to evaluate the esthetics, phonetics, and function of the restorations. The functional aspect includes the envelope of function, posterior disclusion, and anterior guidance. There are several dual-cure provisional systems; one of the criteria for selection is how closely the material matches the shade guide used in the office. Having a close match helps the clinician and patient in the shade selection process.
Case Study
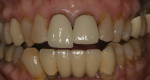
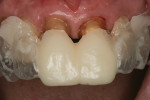
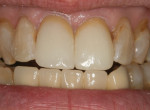
A 52-year-old female patient presented with ceramo-metal crowns on tooth Nos. 8 and 9. Her chief complaints were: that she was unable to bite into certain foods because her front teeth did not touch; the black triangle between the two front teeth; and the difference in the length of her front teeth (Figure 1). She felt that No. 8 was too long and No. 9 was too short. Upon examination, her protrusive position produced an anterior open bite caused by interference of several previously placed posterior crowns. All other aspects of her dental condition were unremarkable. The treatment plan included the equilibration of the posterior occlusal interferences, re-establishing the incisal edge position, and then fabricating new all-ceramic restorations for both central incisors.
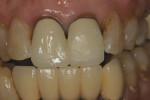
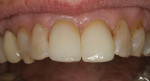
After adjustment of the posterior interferences, the incisal edges of teeth Nos. 8 and 9 were altered by shortening No. 8 and lengthening No. 9 with composite (Figure 2). Phonetic testing included having the patient make “f” and “v” sounds to evaluate the positions of the incisal edges of the upper incisors to the lower lip. She was asked to repeat a series of words that had “f” and “v” sounds. While pronouncing these words, it was noted that the incisal edges were contacting the “wet” inner vermillion border of the lower lip. If the incisal edges were too long then the contact would have been impinging on the outer or dry portion of the lip.8
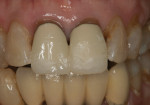
An “s” sound evaluates the maxillary incisor position, mandibular incisor position, and the tongue. The production of a clear “s” sound without a lisp also confirms the correct horizontal position of the incisal edge. The sound is created by how the air is squeezed between the maxillary and mandibular incisors. A lisp will be detected when there is too much space between the maxillary and mandibular incisors. If there is insufficient space then the incisal edges will “bump” into each other.9 Her phonetics were clear and without impingement on the lower lip. Her anterior teeth were able to make contact in protrusive without any posterior interference (Figure 3). The envelope of function was also tested by giving the patient some food to chew. This allowed her to “test drive” the new incisal edge position and ascertain any difficulty or interference during her chewing motion.
After confirmation, an alginate impression was made to record the position and contour of the central incisors and poured into a fast-setting stone (Snap-Stone, Whip Mix Corp., www.whipmix.com).
Preparations
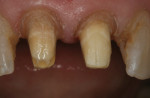
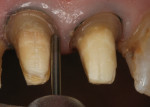
After the existing crowns were removed, secondary decay that remained around the margins was excavated. The facial and interproximal margins were prepared to the height of the gingiva (Figure 4). In order to eliminate the interpapilla black triangles, the crown margins needed to be placed subgingivally. Placing the crown margins below the height of the tissue squeezes the papilla, causing the tissue to move mesially and incisally, thereby filling in the triangular spaces. The preparation margin must be placed at the correct depth in the sulcus so that it does not encroach on the biologic width. Placing the margin too deep can result in chronic inflamed tissue; conversely, placing the margin not deep enough could result in recession with subsequent exposure of the crown margins, which could lead to a reappearance of the black triangles.
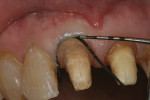
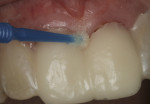
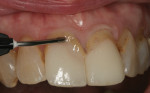
The sulcus depth determines the margin placement.10 The crown margin is placed 0.5 mm to 0.7 mm below the gingival crest when the sulcus depth is 1.5 mm or less. If the sulcus depth is more than 1.5 mm the crown margin should be placed at half of the measured depth below the gingival crest. For this particular case, the sulcus depth measured 1.5 mm on the facial and interproximal areas. A non-impregnated #2-0 surgical suture silk was placed with a periodontal probe exposing 0.5 mm of tooth structure (Figure 5). Due to the tightness of the braided surgical silk, the use of a small tipped periodontal probe easily placed the cord without trauma to the tissue. Traditional retraction cords with loose braids are difficult to place with such a small end instrument because the instrument tip usually perforates the cord while packing. Commercial cord packing instruments with larger tips are needed to pack that type of cord and could possibly traumatize the tissue.
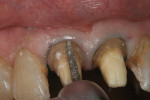
The margins were then prepped to the height of the suture material (Figure 6). An end-cutting diamond bur was used to refine the 90-degree exit angle of the preparation margin (Figure 7).
Although a diode laser may be used to widen and raise the sulcular crevice above the preparation margin, in this author’s experience the placement of the braided surgical suture provides a more concise method of exposing an even amount of tooth structure facially.
A second cord was placed that moved the first cord apically, exposing more of the preparation margin. Wetting the cords with water kept the sulcular epithelium from sticking to the cords when they were removed. This helped to prevent bleeding in the sulcus.
Tray adhesive was applied to the impression tray 10 minutes before the impression was taken. Polyvinyl siloxane (PVS) heavy body was syringed into the tray and inserted. Before reaching the final set time (approximately 30 seconds before the manufacturer’s recommended set time), the tray was partially removed and re-seated. This was repeated several times before the material reached the final set. This maneuver creates relief in the impression to lessen the hydraulic forces generated during a two-step impression technique.11,12 The impression was dried, and interproximal areas were removed. The wash material was then injected into the entire impression and inserted. After setting was complete, the impression was removed and inspected.
Provisionals
With the use of a vacuum-forming machine, a stent was made from the stone model of the mock-up. It is advantageous to scallop the stent around the gingival margins of the prepared teeth; this allows removal of excess uncured provisional material before the setting time is reached and expedites the finishing steps.
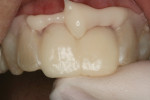
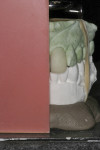
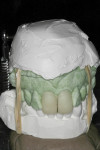
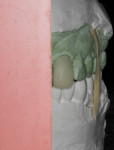
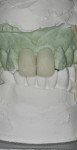
The teeth were lubricated with glycerin. A dual-cure provisional material (SmarTemp® Dual Cure, Parkell Inc., www.parkell.com) was injected into the stent, which was placed over the prepared teeth (Figure 8). Excess material was removed from the margins with a microbrush (Figure 9), and light-curing was then performed for 2 seconds on both the facial and lingual surfaces. The initial set allowed the provisional restoration to be removed and reseated repeatedly as the chemical set phase continued. This tactic blocked out undercuts that could develop between the unparalleled walls of the two adjacent preparations (Figure 10). Additional light-curing was applied to increase the proportion of cured material. The provisional restorations were removed from the stent, trimmed, finished, and returned to the mouth for a final light-curing and verification of occlusion.
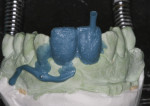
Using the same stent and procedure, a duplicate provisional restoration was fabricated. It was sent to the laboratory and used to correctly orient the master cast (horizontal/vertical cant) on the articulator.
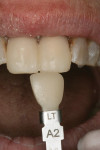
The provisional restorations were cemented in place using a dual-cure temporary cement. The surgical suture retraction cords were removed at this time. Removing the cords earlier could have caused some bleeding, which might have discolored the provisional material. As previously mentioned, the provisional restorations aid in the shade selection (Figure 11).
In the Laboratory: Mounting the Casts
Two master casts were poured: one was used to make a solid model, and the other to make a working multiple die model. The most important step in the laboratory in fabricating the final restorations is ensuring the correct orientation of the mounted models on the articulator.13 If the models are not correctly mounted, achieving success becomes challenging. Without any device, the lab technician must rely on the adjacent teeth to visualize a horizontal cant, which is only an assumption and is unpredictable. Studies have shown that in a large percentage of cases the maxillary cant does not coincide with the horizontal cant.14-16 This is also true for the cusp tips of the canines as well as the gingival heights of contour.17
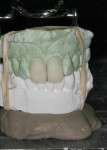
Since the provisional restoration represents the correct cant as observed on the patient, the second provisional restoration that was fabricated and sent to the laboratory represents the same orientation when placed on the master cast. The mounting procedure began by placing the second provisional restoration on the master cast. The midline between the two central incisors was penciled in to accentuate it. The maxillary and mandibular models were hand-articulated and then held together with a rubber band. A thick layer of Silly Putty™ (Crayola, LLC, www.crayola.com) was placed over the lower member of the articulator to hold the model in place (Figure 12). The models were then placed onto the Silly Putty and aligned using a straight edge so the penciled midline was perpendicular to the top of the lab bench and parallel to the straight edge (Figure 13). The consistency of Silly Putty is supportive enough to hold the position of the cast when applying the fast-set mounting plaster (Figure 14). The straight edge is used to verify the correct cant of the mounting (Figure 15).
The Silly Putty was removed from the lower portion of the articulator and the mandibular cast was mounted. The straight edge was used again to verify the correct cant (Figure 16).
In the laboratory the crowns were made using a wax injection technique made from a copy of the provisional restorations. After die spacer was applied to the prepared teeth and lubricated, a silicone matrix of the provisional restorations was placed on the master cast. Melted wax was injected under pressure through strategically placed holes in the silicone matrix. Once the wax cooled, the silicone matrix was removed revealing a duplication of the provisional restoration in wax (Figure 17). The wax crowns were removed, finished on the individual dies, and invested and pressed using IPS e.max® (Ivoclar Vivadent, www.ivoclarvivadent.com) pressable ingots. This technique allows for complete duplication of the provisional restorations that were approved by the patient.
Insertion
The provisional crowns were removed, and the permanent crowns were tried in to verify the fit. The patient was asked to move into an edge-edge position to confirm incisal edge contact of the anterior teeth in protrusive (Figure 18). Phonetic testing was initiated and completed upon the patient’s satisfaction. The patient also approved the esthetics, shape, and color. The crowns were removed and prepared for bonding.
The crowns were inserted using a dual-cure adhesive cement. An oxygen barrier glycerin-based gel was placed over the margins prior to the final light-polymerization18 (Figure 19). Composite polymerization is a continuous reaction induced by free radicals.19 If the surface of the composite comes into contact with oxygen, the polymerization is inhibited by the formation of peroxide radicals, which have a decreased reactivity towards monomers.20 The oxygen stabilizes the excitability of the free radicals, causing an interference with the polymerization reaction. This unreacted layer of free monomers and oligomers is called the oxygen-inhibited layer (OIL) and has a sticky liquid-like surface.19 Depending on the type of composite, the thickness may range from between 10 μm and 200 μm.19 This non-polymerized surface at the restoration-composite-tooth substrate interface is subject to early loss, resulting in a ditched margin within weeks of the insertion.
In situations where a majority of the bonding surface of a restoration has a limited visibility to the curing-light source, finishing should be delayed for a period of time since the chemical-curing phase is slower to complete than the light-curing phase.
The crowns were light-polymerized for 20 seconds per surface. The transparency of the oxygen-barrier glycerin gel allowed the light source unabated to the crown margin. A final view of the crowns in place is shown in Figure 20.
Conclusion
Using the duplicate provisional restoration to mount the master model ensured that the mounting would be correct because it gave the technician the opportunity to observe exactly what the patient was wearing. After the midline was penciled in and the provisional was placed on the working model, it was obvious that the position of the master cast was correctly oriented on the articulator. Duplicating the anatomical contours and tooth positions with either a wax-injection technique or a copy-scan-mill (CAD/CAM) technique by copying an “already approved” provisional afforded the clinician confidence for the success and acceptance of the final restorations.
About the Author
Gregg A. Helvey, DDS
Adjunct Associate Professor, Virginia Commonwealth University School of Dentistry, Richmond, Virginia; Private Practice, Middelburg, Virginia
References
1. Burke FJ, Murray MC, Shortall AC. Trends in indirect dentistry: 6. Provisional restorations, more than just a temporary. Dent Update. 2005;32(8):443-444, 447-448, 450-452.
2. Lodding DW. Long-term esthetic provisional restorations in dentistry. Curr Opin Cosmet Dent. 1997;4:16-21.
3. Gratton DG, Aquilino SA. Interim restorations. Dent Clin North Am. 2004;48(2):vii, 487-497.
4. Samet N, Smidt A, Samet N, Weiss EI. A clinical and cost-benefit evaluation of five facebows. Quintessence Int. 2002;33(7):511-515.
5. Helvey GA. Press-to-zirconia: a case study utilizing CAD/CAM technology and the wax injection method. Pract Proced Aesthet Dent. 2006;18(9):547-553.
6. Helvey GA. Fabrication of porcelain laminate veneers from provisional restorations: the wax injection method. Pract Proced Aesthet Dent. 2003;15(7):538-542.
7. Helvey GA. The wax injection method of replication teeth. Pract Proced Aesth Dent. 2003;15(5):361-363.
8. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Hanover Park, IL: Quintessence Publishing; 1994:21.
9. Dawson PE. Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2006:181.
10. Shenoy A, Shenoy N, Babannavar R. Periodontal considerations determining the design and location of margins in restorative dentistry. J Interdiscip Dent. 2012;2(1):3-10.
11. Caputi S, Varvara G. Dimensional accuracy of resultant casts made by a monophase, one-step and two-step, and a novel two-step putty/light-body impression technique: an in vitro study. J Prosthet Dent. 2008;99(4):274-281.
12. Franco EB, da Cunha LF, Herrera FS, Benetti AR. Accuracy of Single-Step versus 2-Step Double-Mix Impression Technique. ISRN Dent. 2011;2011:341546.
13. Bhuvaneswaran M. Principles of smile design. J Conserv Dent. 2010;13(4):225-232.
14. Bjorndal AM, Henderson WG, Skidmore AE, Kellner FH. Anatomic measurements of human teeth extracted from males between the ages of 17 and 21 years. Oral Surg Oral Med Oral Pathol. 1974;38(5):791-803.
15. Shillingburg HT Jr, Kaplan MJ, Grace SC. Tooth dimensions—a comparative study. J South Calif Dent Assoc. 1972;40(9):830-839.
16. Magne P, Gallucci GO, Belser UC. Anatomic crown width/length ratios of unworn and worn maxillary teeth in white subjects. J Prosthet Dent. 2003;89(5):453-461.
17. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Hanover Park, IL: Quintessence Publishing; 1994:26.
18. Hoofard S, Lowe E. Matching crown restorations in the esthetic zone. Inside Dental Technology. 2010;1(2):34-38.
19. Park HH, Lee IB. Effect of glycerin on the surface hardness of composites after curing. J Korean Acad Conserv Dent. 2011;36(6):483-489.
20. Ghivari S, Chandak M, Manvar N. Role of oxygen inhibited layer on shear bond strength of composites. J Conserv Dent. 2010;13(1):39-41.