The Photoshop Smile Design Technique (Part 1): Digital Dental Photography
Abstract:
The proliferation of digital photography and imaging devices is enhancing clinicians’ ability to visually document patients’ intraoral conditions. By understanding the elements of esthetics and learning how to incorporate technology applications into clinical dentistry, clinicians can predictably plan smile design and communicate anticipated results to patients and ceramists alike. This article discusses camera, lens, and flash selection and setup, and how to execute specific types of images using the Adobe® Photoshop Smile Design (PSD) technique.
Increasingly, patients are seeking dental and medical treatments for esthetic purposes.1,2 The advent of digital photography and intraoral imaging devices has dramatically improved clinicians’ ability to quickly and easily document patients’ intraoral conditions through photographs or video, using a monitor or printer to clearly demonstrate to patients the problems diagnosed. Historically, dentists have verbally explained the possibilities for treatment and may have shown images of patients treated in similar cases. Another classic mode of communicating potential treatment options has been to show the patient a design wax-up. (The authors use the term “design” instead of “diagnostic” because the wax-up is a potential design and does not actually serve to diagnose.)
In recent years, however, the computer design software that has developed and evolved has become a powerful tool for showing patients the possibilities for enhancing their smiles. By understanding the elements of esthetics and learning how to incorporate technology applications into clinical dentistry, clinicians can predictably plan smile design and communicate anticipated results to patients and ceramists alike.3
This article will discuss camera, lens, and flash selection and setup, and how to take very specific types of images using the Adobe® Photoshop Smile Design (PSD) technique. It will also cover techniques for taking high-quality macro images of teeth to best visualize the color and texture detail present in a tooth. [Editor’s Note: In 2014 Compendium is planning to publish more on this subject by these authors. Topics tentatively scheduled will include: specific Photoshop settings used for the smile design technique; basic Photoshop techniques for initial importing and image manipulation; simple smile design techniques using imported “stock” smiles from a smile design library; simple alterations of teeth to improve smiles using Photoshop; and sophisticated techniques of digitally measuring patients’ existing smiles and using smile design principles to create and apply tooth grids with known proportions, then re-design teeth using special tools in Photoshop to create more ideal esthetic relationships.]
Cameras, Lenses, Lighting, Camera Settings
Distortion-free, repeatable, and calibrated images with known magnification ratios are essential for accurate diagnosis, digital design, and, ultimately, credible communication. Point-and-shoot cameras are not ideal; due to the fixed focal length and aperture of these types of cameras, there are distortions and depth-of-focus issues with the images that do not lend themselves well to digital alteration. Therefore, it is important to use a digital single-lens reflex (SLR) camera (Figure 1) with a lens with the proper focal length.
The lens used is also important. Short focal lenses (wide angle) distort aspects of the image, making elements closer to the lens appear larger and those farther away from the lens appear smaller than in reality (Figure 2). Images made with a long focal length lens make all elements of the image look flat, and farther away elements in the image appear larger than they are. An 80 mm to 105 mm macro lens that focuses from 1:1 magnification to infinity creates the least distortion at all magnification ratios. Thus, a retracted full-arch (second molar to second molar) image and a full-face image made with this lens will maintain undistorted intra-element relationships within the image. Dual- (or multi-) point flash systems that allow quick repositioning for both normal dental and smile design images are ideal for use.
Camera Selection
There are literally hundreds of digital SLR cameras on the market at any given time. The authors recommend either Nikon (www.nikon.com) or Canon (www.canon.com) mid-price range or above digital SLR cameras, as these have much better white balance control than less expensive versions,4 and Nikon and Canon both have flash systems that are ideally suited to dental macro-photography. Mid-range digital SLR cameras feature a control that allows the white balance to be set at color temperatures in 100-degree kelvin increments, compared with less expensive versions that only allow presets. The mid-range cameras have higher resolutions for digital images and have full high-definition (HD) video capacity. They also have user settings that allow stored information of specific camera settings to be set in a one-touch fashion versus having to set camera variables individually. Compared to the higher-end cameras available, their flexibility, durability, and performance (eg, speed) is less than that needed by professional photographers, however mid-range cameras tend to be ideal for most dental uses.
Although there are more expensive cameras available, the crop-sensors on the following recommended camera bodies provide an ideal balance between resolution, noise, and depth of field, and all have HD video capacity. These recommendations are Nikon’s D7000 and D7100 and Canon’s 70D and 60D.
Lens Selection
The lens required for most dental photography is a macro- (or micro- per Nikon) specific lens of approximately 100 mm focal length with a maximum f/stop of approximately 2.8. This type of lens is well suited to manipulating images for digital smile design. Higher-quality lenses generally include ease-of-use features such as image stabilization, fixed lens length, better image quality, and faster autofocus (when needed). It is recommended that consistency be maintained between lens and camera manufacturer—ie, use a Nikon lens for a Nikon camera and a Canon lens for a Canon camera—although there are after-market lenses that work for each camera as long as the focal length is in the recommended range. The authors’ lens choices for Nikon are AF-S VR Micro-Nikkor 105 mm f/2.8G IF-ED and AF-S DX Micro-Nikkor 85 mm f/3.5G ED VR; for Canon, they are Canon EF 100 mm f2.8L USM IS Macro and Canon EF 100 mm f2.8 USM Macro.
Flash Selection
Of all the camera components, the flash and light control have the greatest effect on image quality. The authors have found that a dual-point flash system with a specialized bracket that allows quick positioning of the flash units offers the best image results for a small portable package (Figure 3). Such brackets are available from several manufacturers, although the authors strongly prefer the Photomed R2 Dual Point Flash Bracket (Photomed, www.photomed.net).
Camera Settings
Though SLR cameras may initially seem to offer a vast array of settings, there is a strong case to be made for uniform settings in dental photography.5 The following settings will give the dental photographer a strong baseline from which to work. For smile design images, the authors recommend recording images in RAW file format. Images recorded in RAW will allow the greatest flexibility in postprocessing and fine-tuning of exposure, using the following guidelines: The photographer should set the ISO to 200. For intraoral images, the aperture should be set to f/32, although f/22 to f/45 will work nearly as well. For full-face images, the aperture should be set to f/8, although f/5.6 to f/11 will also suffice. The exposure mode should be set to aperture priority (often denoted as Av).
With certain camera models, however, the manual exposure mode (M) is preferable, and as the user further develops camera knowledge and expertise, manual mode gives the photographer the greatest control. If using manual settings, the authors recommend setting the shutter speed to approximately 1/250. Note that setting the shutter speed as high as possible will also negate most of the ambient lighting.
The white balance is often a subject of much debate.6 The camera should be set to 5500K in the white balance camera setting. If the camera does not allow “dialing in” the white balance to a specific number, the flash’s pre-set white balance should suffice. For ultimate white balance control, the camera can be set to a custom white balance, using the camera instructions for this technique.
For exposure control (ie, the lightness and darkness of the image) the easiest thing to change is the exposure value (EV) setting on the flash (Figure 4), but it can also be changed on the camera (Figure 5). To expose the image more—ie, make it brighter—the EV setting should be changed to the “+” (plus); conversely, to expose the image less—thereby making it darker—the EV setting should be changed to “-” (minus).
Smile Design Images and Video
Images for Photoshop smile design should be taken in a consistent manner from one patient to the next—ie, camera settings, magnification ratio, lighting, and composition should be standardized for each type of image. Among the images needed to analyze and digitally design a smile are full-face, lower one-third face, and retracted full-face views.7
Full-Face Images
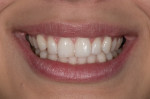
Full-face images can be thought of as preoperative portraits. Smile design image #1 is a full-face image from above the hairline to below the chin (Figure 6), with the patient in the repose lips-relaxed position and the camera vertical to enable closer focus. The magnification is between 1:8 and 1:10, F-stop 8. Some academies require the image to be shot with the camera in a horizontal position. The important point is the composition, not so much the camera orientation. Image #2 is done with the exact same camera settings and camera position; the only difference is that the patient shows a full/normal smile (Figure 7). An optional photograph, though very helpful with digital calibration of image rotations, is a full-face image with the same settings and magnification ratios, but done with the patient holding cheek retractors (Figure 8). The authors suggest shooting this image with the patient seated on the assistant’s stool and the photographer seated on the doctor’s stool so the patient is more likely to be in an upright position (Figure 9).
Intraoral Full-Arch Images
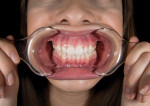
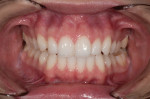
The primary image used in the PSD technique is the retracted full-arch view (Figure 10).3 The teeth should be slightly separated—about 2 mm, roughly the same amount they are separated while smiling. The aperture adjustment on the camera is set to f/32 or higher, and the magnification is set at 3:1; the flashes are placed next to the lens, and the cheek retractors are held by the patient (Figure 11). Two or three images should be taken as backups. This image should be taken just before the next image of the lower one-third face smiling. After these images are taken, the patient is asked to remove the cheek retractors and smile (Figure 12). This will minimize movement of the subject (patient) and enable the photographer to take the next image at the same position and same magnification ratio, thus making it easier to superimpose the images in Photoshop at a later time.
Lower One-Third Face Images
For lower one-third face images, the camera settings, lens aperture and magnification, and flash positions are exactly the same as the previous intraoral full-arch retracted view image. The difference is that the patient is asked to remove the cheek retractors and smile normally (Figure 12). The photographer then takes at least two images of this composition (Figure 13). The full-arch retracted and lower one-third smiling images will now be superimposed—positional adjusting in Photoshop may be needed—to design new teeth using the retracted view. The image with the lips is placed on top of the new design so that the patient can visualize the new teeth with the lips. The same new design can be taken to the full-face image to show the patient the effect of the new design on the full face.
Close-Up Dental Images
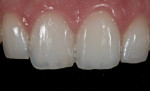
While not required for smile design, a 1:1 magnification view of the central incisors with a black background is a useful source of information for the ceramist (Figure 14). This type of image best highlights the translucency and color detail of teeth that may be desirable to reproduce. To achieve this, the camera is set to f/32 or higher, and the flashes are positioned about 3 inches away and 2 inches behind the lens (Figure 15). Close-up images can be further optimized by reducing glare by using a polarizer on the flash. Chroma gradations can be seen and glare eliminated altogether (Figure 16) by also polarizing the lens (Figure 17). Sheet polarizers for the flash and lens polarizers can be purchased separately from a knowledgeable photography resource; Figure 17 shows a system specifically designed for dentistry (Polar Eyes, Photomed).
Video
All of the cameras recommended have an HD video capture capacity (Figure 18). Recording the dynamic movement of the lips from a relaxed position, to talking, to a full smile is a valuable adjunct to still images for helping with the smile analysis and ultimate smile design. Though the flash cannot be used for video (video light sources are available), the authors have found the ambient operatory lighting to be sufficient with the following settings: ISO 800, f/8, shutter speed 1/30-1/60, monochrome, magnification 1:3. Image stabilization (vibration reduction) is invaluable for video recording; use of a tripod is a viable alternative. The color temperature of the ambient operatory light is distracting in video captures and is best resolved through the use of a monochrome setting. In the authors’ opinions, dentists and technicians alike will be significantly better equipped to make diagnostic decisions based on the video capture of the dynamic lip movements versus static image capture.8
Summary
Digital dental photography is an exceptional tool for communication, diagnosis, and documentation. Much of what is possible today with dental treatment hinges strongly upon dentists’ ability to fully capture the necessary diagnostic information and properly educate their patients. With the proper training, techniques, equipment, and implementation, dental photography can support the making of an accurate diagnosis and enhance communication regarding treatment recommendations.
ABOUT THE AUTHORS
Edward A. McLaren, DDS, MDC
Professor, Founder, and Director, UCLA Post Graduate Esthetics; Director, UCLA Center for Esthetic Dentistry; Founder and Director, UCLA Master Dental Ceramist Program, UCLA School of Dentistry, Los Angeles, California; Private Practice, Prosthodontics and Esthetic Dentistry, Los Angeles, California
David A. Garber, DMD
Clinical Professor, Department of Periodontics, Georgia Health Sciences University School of Dentistry, Augusta, Georgia; Private Practice, Atlanta, Georgia
Johan Figueira, DDS
Private Practice, Caracas and Isla de Margarita, Venezuela, and Los Angeles, California
REFERENCES
1. Samorodnitzky-Naveh GR, Geiger SB, Levin L. Patients’ satisfaction with dental esthetics. J Am Dent Assoc. 2007;138(6):805-808.
2. Demand for Botox, fillers drives US cosmetic surgery growth. Published February 20, 2013; Reuters. https://www.foxnews.com/health/2013/02/20/demand-for-botox-fillers-drives-us-cosmetic-surgery-growth/. Accessed October 11, 2013.
3. McLaren EA, Schoenbaum T. Digital photography enhances diagnostics, communication, and documentation. Compend Contin Educ Dent. 2011;32 spec no 4:36-38.
4. McLaren EA, Terry DA. Photography in dentistry. J Calif Dent Assoc. 2001;29(10):735-742.
5. Devigus A. A picture is worth… A three-step process for taking better photographs. Journal of Cosmetic Dentistry. 2012;28(1):82-88.
6. Lowe E. Digital photography: the AACD series—part one. Journal of Cosmetic Dentistry. 2010;26(1):25-30.
7. Snow SR. Assessing and achieving accuracy in digital dental photography. J Calif Dent Assoc. 2009;37(3):185-191.
8. Van der Geld P, Oosterveld P, Schols J, Kuijpers-Jagtman AM. Smile line assessment comparing quantitative measurement and visual estimation. Am J Orthod Dentofacial Orthop. 2011;139(2):174-180.