Maxillofacial Prosthetics: History to Modern Applications. Part 2 – Speech and Swallow Prostheses
Gregory J. Paprocki, DDS
ABSTRACT
Speech and swallow difficulties can arise from a variety of causes. Regardless of etiology, many of the problems can be solved by the fabrication of a speech or swallow prosthesis. Considering the relatively large patient population affected by these disorders, there is limited awareness of maxillofacial prosthetic solutions among the general dental and medical communities. A brief history of speech and swallow prostheses is presented along with recommendations for diagnosis and referral.
Editor’s Note: Part 1 of this series on maxillofacial prosthetics focused on the history and modern applications of obturators.
Problems of speech and swallow can be caused by motor neuron disorders,1 congenital abnormalities,2 surgery,3 and brain injuries.4 Motor neuron disorders include amyotrophic lateral sclerosis (ALS),5 Parkinson’s disease, multiple sclerosis, bulbar poliomyelitis, myasthenia gravis, diabetic neuropathy, and thyroid disease.6 Cleft palate is an example of a congenital abnormality affecting speech and swallow. Surgeries of the soft palate and tongue directly affect speech and swallow, whereas removal of tumors involving the nervous system exert an effect through neuromuscular deficits as do traumatic brain injuries.7 Problems of speech and swallow involving the soft palate are termed velopharyngeal insufficiency, velopharyngeal incompetence,7 or velopharyngeal inadequacy.8 Velopharyngeal insufficiency and velopharyngeal inadequacy describe a condition characterized by a defect in the soft palate such as cleft palate or surgical resection of the soft palate. With velopharyngeal incompetence, the soft palate is anatomically intact but there are neurologic deficits, incoordination, or mislearning.7-9
During normal speech and swallow, the soft palate (velum) moves in a posterosuperior direction, the posterior wall of the pharynx moves anteriorly, and the lateral walls of the pharynx move in an anteromedial direction to contact the velum—hence the term velopharyngeal. This sequence of movements closes the communication between the oral cavity and the nasal cavity to a variable degree. During swallow, velopharyngeal closure should be complete to prevent food or liquid from being ejected through the nose. During speech, velopharyngeal closure controls the degree of hypernasality. Velopharyngeal closure is not necessarily total during speech because certain sounds require a degree of hypernasality.
Regardless of the underlying etiology for velopharyngeal inadequacy or velopharyngeal insufficiency, the prosthodontic treatment involves one of two prostheses. Velopharyngeal insufficiency is managed prosthetically with a speech-aid prosthesis (SAP). The distal extension of the SAP referred to as a “speech bulb” conforms to the movement of the soft palate and oral pharynx during speech and swallow. Velopharyngeal incompetence is treated with a palatal lift prosthesis (PLP). The PLP positions the incompetent soft palate, where it can function with the posterior and lateral pharyngeal walls during speech and swallow.2,7 Surgical resection of the tongue reduces the mass of the tongue and impairs mobility.10 Speech and swallow dysfunction resulting from glossectomy are managed with a palatal augmentation prosthesis.3,11 This prosthesis lowers the palatal vault to a point where the surgically resected tongue can achieve contact during speech and swallow.11
Brief History of Speech and Swallow Prostheses
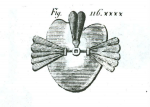
Dentistry offered surprisingly early prosthetic solutions to problems of speech and swallow. In 1776, Verdial made an appliance of Spanish leather, which was lined with sponge intended to seal the edges of the appliance to the teeth. A uvula made of sponge was attached to the appliance with silver wire.12 M. Dubois Foucou in 1780 fabricated an appliance with a spring-loaded metal plate extending distally from the palate. The spring allowed the plate to follow the movements of the residual palate.12 Delabarre in 1820 published a book in which he gave credit to his predecessors and described some of his own designs (Figure 1). He used elastic gum to restore the velum and uvula and is, therefore, considered to be the first to use a soft elastic material for such an appliance.12 James Snell was the first major English author to publish on the subject of cleft palate. During the 18th century, the French had led in culture and science. In 1828, Snell published a book on “obturateurs.” His method used India rubber to restore the missing soft palate.12 Up to this point in time, the authors/developers concentrated on replacing only the missing portion of the soft palate. Because of his medical background, Dr. Stearn, who himself had a cleft palate, had an understanding of the anatomy and physiology of the pharyngeal area but lacked knowledge of prosthetic dentistry. Nonetheless, determined to find a solution, he used molds carved from wood for vulcanizing the prosthetic velum. He demonstrated that a prosthetic extension into the pharynx could be worn comfortably and aid in speech.12 It was Kingsley and Suersen, with their knowledge of prosthodontics, who fabricated an obturator with a pharyngeal component bearing similarities to contemporary prostheses (Figure 2).13
As previously stated, early attempts to improve velopharyngeal insufficiency were limited to the replacement of missing soft-palate tissue. The earliest reference to the mechanism of velopharyngeal closure was an article by Hilton in 1836.14 Although subjective, Hilton’s observations were consistent with what is now accepted as the mechanism of velopharyngeal closure. In 1909, Scheier published a report describing the use of a lateral neck radiograph to visualize velopharyngeal closure.15 This lateral view is merely a 2-dimensional view of what is a 3-dimensional (3-D) process. In spite of this shortcoming, this technique was the gold standard for analyzing velopharyngeal insufficiency for 60 years.15 The 3-D nature of velopharyngeal closure was demonstrated by a series of articles by Skolnick dealing with multiview videofluoroscopy.16-18 At the same time, Pigott demonstrated the 3-D nature of velopharyngeal closure using nasendoscopy.19,20 Because nasopharyngoscopy does not require a radiologist or fluoroscopic equipment and can be performed in the office, this procedure became the standard of care.15
Cantor et al described the first use of a palatal augmentation prosthesis to restore function for glossectomy patients, who typically experience difficulty with articulation, resonance, and voice quality.10 Palatal augmentation prostheses have been used to improve speech and swallow following resection of the tongue.3,11,21 Given the relatively recent introduction of the palatal augmentation prosthesis, little change in design has occurred since its introduction in 1969.
Modern-Day Approach to SAPs and PLPs
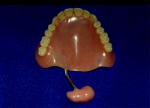
The typical SAP and PLP have an anterior component that supports and retains the posterior velopharyngeal component. In dentate patients, the anterior component is basically a removable partial denture. In edentulous cases, the retentive component is a complete denture base (Figure 3). Retention is an important factor with SAPs and PLPs not only for the final prosthesis but also during fabrication of the prosthesis; therefore, accurate impressions are imperative. The anterior retentive component is the starting point from which the velopharyngeal component is developed.22 The soft palate portion is formed by the addition of thermoplastic material. In the case of the PLP, the material is added to elevate the soft palate to contact the pharyngeal walls during function.23 The soft palate portion of the SAP—in contrast to the PLP—is added to actually contact the pharyngeal walls in function.24 Once developed, the soft palate portion of the SAP and PLP is processed in acrylic.
Modern-Day Approach to Palatal Augmentation Prostheses
Similar to the SAP and the PLP, the basic prosthesis to retain the palatal augmentation prosthesis is either a maxillary denture base or a removable partial denture framework, depending upon whether or not the patient is dentate. The basic prosthesis must be as stable as possible during the development of the palatal augmentation portion, necessitating an accurate impression. Thermoplastic material is used to develop the palatal augmentation. The patient is instructed to articulate “k” and “g” sounds to trace the prosthesis.10 Some authors advocate the use of videofluoroscopy to identify where additional material is needed in the A to P axis of the prosthesis.21 The areas of contact can be checked using pressure-indicating paste, and when satisfied with the results, the prosthesis is processed in acrylic.
On the Horizon
There is currently no way to definitively determine the size and shape of the SAP, PLP, or the palatal augmentation prosthesis using imaging such as computed tomography, laser, digital, etc. To be effective, a diagnostic study would be required to record all the movements of the soft palate (where present), the pharyngeal walls, and the tongue during speech, swallow, and at rest, and to relate the movements in the x, y, and z axes to some reference point on what would be the retentive portion of the prosthesis.
Role of the General Dentist
The procedures involved with developing the SAP are complex and often involve some risk for the patient. These prostheses are best managed by the maxillofacial prosthodontist. The PLP and the palatal augmentation prostheses conversely can be managed by a skilled general dentist, although some review of the literature and coaching by a maxillofacial prosthodontist would be required. Although general dentists may choose not to become involved in the fabrication of these prostheses, their role in follow-up remains essential. These prostheses function optimally when the retentive portion is stable. If the retentive portion is a removable partial denture, modification or loss of the teeth retaining the prosthesis will compromise retention and stability. Patients should be seen for routine maintenance to assure the health of the dentition. Since changes occur over time, the soft tissues should also be monitored for signs of irritation, and recommendations for modification should be made where indicated.
Conclusion
Given the number of conditions that can lead to problems of speech and swallow, the patient population affected by these conditions is large. No special diagnostic test is required to identify patients whose speech is affected because it is obvious due to their hypernasal vocal quality. Problems with swallow associated with loss of a portion of the soft palate or tongue are recognizable with a simple examination of the oral cavity. Problems linked to neurological deficits may not be immediately apparent. Self-reporting by the patient or referral by a physician or speech pathologist is likely to be necessary. Regardless of how the diagnosis is made, recognition that prosthodontic treatment modalities are available is the key to proper management or referral.
ABOUT THE AUTHOR
Gregory J. Paprocki, DDS
Course Director, Staff Instructor, University of Tennessee, College of Dentistry, Memphis, Tennessee
REFERENCES
1. Kelly SW, McLean CC, Manley MC. Assessment in the treatment of hypernasal speech with motor neuron disease: a clinical report. J Prosthet Dent. 1996;75(5):479-482.
2. Tuna SH, Pekkan G, Gumus HO, Aktas A. Prosthetic rehabilitation of velopharyngeal insufficiency: pharyngeal obturator prostheses with different retention mechanisms. Eur J Dent. 2010;4(1):81-87.
3. Davis JW, Lazarus C, Logemann J, Hurst PS. Effect of maxillary glossectomy prosthesis on articulation and swallow. J Prosthet Dent. 1987;57(6):715-719.
4. Winstein CJ. Neurogenic dysphagia. Frequency, progression, and outcome in adults following head injury. Phys Ther. 1983;63(12):1992-1997.
5. Esposito SJ, Mitsumoto H, Shanks M. Use of palatal lift and palatal augmentation prostheses to improve dysarthria in patients with amyotrophic lateral sclerosis: a case series. J Prosthet Dent. 2000;83(1):90-98.
6. Wolf DC. Dysphagia. In: Walker HK, Hall DH, Hurst JW, eds. Clinical Methods. 3rd ed. Boston, MA: Butterworths; 1990:432.
7. Shifman A, Finkelstein Y, Nachmani A, Ophir D. Speech-aid prostheses for neurogenic velopharyngeal incompetence. J Prosthet Dent. 2000;83(1):99-106.
8. Kipfmueller LJ, Lang BB. Treating velopharyngeal inadequacies with a palatal lift prosthesis. J Prosthet Dent. 1972;27(1):63-72.
9. The glossary of prosthodontic terms. J Prosthet Dent. 2005;94(1):10-92.
10. Cantor R, Curtis TA, Shipp T, et al. Maxillary speech prostheses for mandibular surgical defects. J Prosthet Dent. 1969;22(2):253-260.
11. Shimodaira K, Yoshida H, Yusa H, Kanazawa T. Palatal augmentation prosthesis with alternative palatal vaults for speech and swallowing: a clinical report. J Prosthet Dent. 1998;80(1):1-3.
12. Aramany M. A history of prosthetic management of cleft palate: Pare′ to Suersen. Cleft Palate J. 1971;8:415-430.
13. Suersen W. A new system of artificial palates. Am J Dent Sci. 1867;1:373-379.
14. Hilton W. Case of a large bony tumor in the face completely removed by spontaneous separation. Guys Hosp Rep. 1836;1:493-506.
15. Shprintzen RJ, Marrinan E. Velopharyngeal insufficiency: diagnosis and management. Curr Opin Otolaryngol Head Neck Surg. 2009;17(4):302-307.
16. Skolnick ML. Video velopharyngography in patients with nasal speech, with emphasis on lateral pharyngeal motion in velopharyngeal closure. Radiology. 1969;93(4):747-755.
17. Skolnick ML. Videofluoroscopic examination of the velopharyngeal portal during phonation in lateral and base projections—a new technique for studying the mechanics. Cleft Palate J. 1970;7:803-816.
18. Skolnick ML, McCall GN, Barnes M. The sphincteric mechanisms of velopharyngeal closure. Cleft Palate J. 1973;10:286-305.
19. Pigott RW. The nasendoscopic appearance of the normal palato-pharyngeal valve. Plast Reconstr Surg. 1969;43(1):19-24.
20. Pigott RW, Bensen JF, White FD. Nasendoscopy in the diagnosis of the velopharyngeal incompetence. Plast Reconstr Surg. 1969;43(2):141-147.
21. Wheeler RL, Logemann JA, Rosen MS. Maxillary reshaping prostheses: effectiveness in improving speech and swallowing of postsurgical oral cancer patients. J Prosthet Dent. 1980;43(3):313-319.
22. Lang BR. Modification of the palatal lift speech aid. J Prosthet Dent. 1967;17(6):620-626.
23. La Velle WE, Hardy JC. Palatal lift prostheses for treatment of palatopharyngeal incompetence. J Prosthet Dent. 1979;42(3):308-315.
24. Hofstede TM, Jacob RF. Diagnostic considerations and prosthetic rehabilitation of a cocaine-induced midline destructive lesion: a clinical report. J Prosthet Dent. 2010;103(1):1-5