Bioactive and Therapeutic Preventive Approach to Dental Pit and Fissure Sealants
Key Take-Aways
• Dental pit and fissure sealants have long been considered an important part of preventive and minimally invasive dental care; however, their complete adoption by the dental profession has not been as fully integrated as anticipated.
• Drawbacks of conventional hydrophobic resin materials can be overcome with the adoption of a hydrophilic resin sealant material.
• The hydrophilic properties of Embrace WetBond sealant enable improved adaption to pits and fissures, making this sealant less technique-sensitive and easier to place than traditional materials.
-----------------------------------------------------------------------------------------------------------------
The current economic environment and federal mandates concerning healthcare are causing an increasing number of businesses and state government agencies to reduce funding for dental care. This circumstance will likely make preventive services for dental patients more critical than ever since their cost can be significantly lower than restorative procedures.
The American Dental Association has long been an advocate of minimally invasive and preventive care and has urged the profession to embrace pit and fissure sealants as one of the important mechanisms in preventive care.1 The ADA has stated:
• Dental sealants are effective at preventing dental decay (primary prevention).
• Both children and adults can benefit from the use of sealants.
• Sealants can stop non-cavitated (incipient) lesions from progressing (secondary prevention).
• To be effective, sealants must be properly applied, monitored, and replaced when needed.
The dental profession, however, has not fully adopted this vital preventive procedure.2,3 Some of the reasons often stated for not advocating the routine use of pit and fissure sealants are the perceived lack of long-term effectiveness, poor retention, technique failure attributable to traditional hydrophobic materials,4,5 and the perception that if the sealant fails, the sealed-in bacteria can continue to penetrate deeper into the tooth structure.6,7
Having an understanding of the physiology and science of the oral cavity can shed some light on potential solutions that make the use of pit and fissure sealant materials more universally acceptable to the dental profession. For example, it is now known that enamel is a “semi-permeable membrane” that has a constant flow of fluids outward from the pulp.8 It is also known that the cyclic action of demineralization and remineralization is continuously occurring in the oral cavity. The outer surface of the enamel is being constantly attacked by acids from food, beverages, and pathogenic bacteria, lowering the pH and making the mouth quite the battleground.
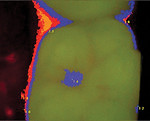
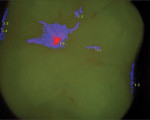
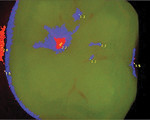
When the protective mechanism of the oral cavity is able to combat this attack, equilibrium is established by the influx of calcium, phosphate, and fluoride ions into the tooth structure. These minerals precipitate onto the tooth and become part of a complex system in which enamel-building proteins interact with hydroxyapatite to form protective fluorapatite and tooth enamel. If conditions in the oral cavity impede this mineral transfer, then the healthy formation of the enamel rods and crystalline enamel structure is impaired, the tooth becomes less resistant to the constant acid attack, and the condition of the tooth degrades.9 Figure 1 through Figure 3 are images obtained using the Spectra® Caries Detection Aid system (Air Techniques Inc., www.airtechniques.com) that demonstrate the progression of a carious lesion over a period of 14 months.
Traditional Pit And Fissure Sealants
Traditional pit and fissure sealants and composite restorative materials are hydrophobic and essentially inert in nature. Predominantly passive materials, they do not contribute to the healing process of the dentition or the replenishment of ions and minerals necessary to help neutralize the cyclic acid attack on the dentition. This neutral existence is intended to be biocompatible and cause no harm. However, due to their passive nature, these sealants fail to contribute to the overall protective process that can be achieved with dynamic, bioactive materials that are capable of combating the constant environmental attacks from the acids and bacteria found in the oral cavity.10-13
When traditional pit and fissure products are used, the bond to the enamel is critical for the procedure to succeed. Yet, there are several factors that can lead to the failure of traditional hydrophobic sealants. First, deep fissures will invariably retain moisture, preventing full penetration of the hydrophobic sealant into the depth of the fissure.14-16 Second, it is impossible to have a totally dry environment in the mouth; breathing produces moisture, and eliminating this moisture requires the use of rubber dam for complete isolation. However, rubber dam is not routinely used by the majority of clinicians placing sealants.17,18 Additionally, the trend is to delegate treatment and have the sealants placed by dental auxiliaries, many of whom are not highly trained in rubber dam placement. An intraoral isolation device may be used as an alternative to aid in reducing moisture contamination; however, while such a device may be effective, some dental offices may hesitate to incorporate it due to the initial cost of purchase.
The use of prophylaxis pumice as a routine procedure to remove plaque prior to placing pit and fissure sealant must also be examined. The intent is to remove debris and contaminants from the tooth surface and enhance the adhesion of the pit and fissure sealant. However, it has been reported that the bottom of the fissure still remains filled with plaque and moisture,19 contributing to the ultimate failure of the sealant.13
Another available cleaning method is an air polisher with sodium bicarbonate in a water slurry. The sodium bicarbonate raises the pH of the tooth, making it imperative to etch and rinse twice in order to neutralize the higher pH and effectively etch the tooth; otherwise, the etching of the tooth surface will be inadequate, which will challenge the retention of the sealant material.
The use of 4th- and 5th-generation dental adhesives has also been recommended to improve the adhesion and adaptation of sealants to the morphology of molars.20 These hydrophilic primers are used after etching and have a water chaser, such as ethanol or acetone, which enables them to better penetrate the depth of the pits and fissures before application of the sealant. However, this procedure adds an additional step, which takes time, adds cost, is technique-sensitive, and introduces another avenue for moisture contamination.21,22
Hydrophilic Sealants
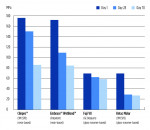
While hydrophobic monomers have demonstrated good sealing characteristics compared to self-etching materials,23 many of the aforementioned issues can be resolved by using hydrophilic sealants. With these materials, preparing the surface of the tooth structure to remove debris remains important, however moisture is not an issue. An example of a currently available hydrophilic pit and fissure sealant is Embrace™ WetBond™ (Pulpdent Corp., www.pulpdent.com), a resin-based hydrophilic sealant that readily penetrates down into and adapts to the pits and fissures.24 Glass-ionomer-based hydrophilic pit and fissure sealant materials are also available; however, the resin-based Embrace WetBond material has greater strength and durability than the glass ionomers, and a superior retention rate has been demonstrated for resin-based sealants over that found with glass-ionomer-based sealant materials.25 Figure 4 shows mean values and standard deviation of compressive strength of four different materials: two were glass-ionomer-based, and two were resin-based (Embrace WetBond and Clinpro™ [3M ESPE, www.3MESPE.com]).26
An important characteristic of hydrophilic sealant materials that needs to be further emphasized is their ability to transport ions from the oral environment onto the tooth surface. This process requires water, and materials that contain water and are moisture-friendly are advantageous in this respect. Although this transport mechanism is passive and dependent on the concentration gradients of the ions and the permeability of the resin matrix, it is constant and never ending, and it results in remineralization and the restoration of the tooth’s physical and mechanical properties.
Embrace WetBond materials are ionic resins that contain a small amount of water and are moisture-tolerant and water-miscible. They are designed to behave favorably in the moist oral environment and take advantage of the water that is ever-present in the mouth.27 In the presence of moisture, the uncured material is acidic and simultaneously ionizes, etches, and adheres to the tooth structure. The cured Embrace WetBond material has a neutral pH and very low solubility (0.06%), but it is not a static material, rather it is a dynamic system. The water content of the hydrophilic resin enables increased and continuous ionic exchange in the cured material and allows calcium, phosphate, and fluoride ions to precipitate onto and bind to minerals in the tooth, forming a strong resin–hydroxyapatite complex and a positive seal against microleakage. This bioactive process is inherent in the Embrace WetBond ionic resin, which mimics nature and provides the ionic components required for remineralization. Furthermore, research has shown that Embrace WetBond can be recharged by fluoride28 in the same way as glass-ionomer materials, thereby providing continued benefit to tooth structure (Figure 5).
This ionic exchange process was recently reported in research involving the atraumatic or alternative restorative technique (ART). Carious lesions with an intact dental matrix can be reversed, and the tooth structure can remineralize. Research at Northwestern University (Evanston, Illinois) in collaboration with UNESP (Aracatuba, São Paulo, Brazil) conducted at the Argonne National Laboratory (Argonne, Illinois) tested pit and fissure sealants to determine their effect on remineralization.29-31 These research studies demonstrated that certain sealant materials can actually remineralize the surface of the tooth. Another recent in-situ study on pit and fissure sealant remineralization also reported that bioactive or therapeutic sealant materials demonstrated remineralization capabilities on artificial caries lesions.32
Among the constituents that have the potential to remineralize carious lesions or minimize caries development are calcium and phosphate ions from saliva or other sources (dentifrices, chewing gums, beverages, remineralizing solutions, and restorative materials) and fluoride from topical (toothpaste and mouth rinses) or systemic sources (water and diet). The calcium and phosphate in saliva are the natural defense against mineral tooth loss. However, if only salivary calcium and phosphate are available, this remineralization occurs only in the most superficial part of the lesion, and demineralization in the rest of the lesion is only arrested.33
Fluoride present in the oral environment plays an important role in reducing demineralization and potentiating remineralization. However, fluoride ion activity is dependent upon the availability of calcium and phosphate ions at the site of a lesion or in the saliva.34,35 If a supplementary concentration of calcium and phosphate ions is supplied by paste, varnish, tablet, gum, or rinse, the efficiency of the remineralization process will increase. When one considers the complex nature of this dynamic system, the continuous ionic exchange, the demineralization–remineralization process, and the multiple sources of the ionic components, it is clear that hydrophilic sealants that both allow and increase transport of ions for the remineralization of tooth structure are a significant positive development in the evolution of preventive dentistry.
Conclusion
Pit and fissure sealants should be part of a total, minimally invasive dental care approach that emphasizes preventive maintenance and includes home adjunctive care with remineralization products. Coupled with routine use of the caries risk assessment tools for determining the caries risk for each individual patient, sealants can provide profound benefit to patients.
With today’s resin-based hydrophilic sealant products such as Embrace WetBond, the routine use of pit and fissure sealants is a viable and predictable preventive procedure. Hydrophilic properties provide improved adaption to pits and fissures and a better seal, making these sealants less technique-sensitive and easier to place than traditional materials. The bioactive properties produce greater ionic activity and encourage remineralization of tooth structure. Because these sealant materials thrive in the moist oral environment, the drawbacks and challenges of traditional hydrophobic materials are eliminated. As such, these products can be considered a bioactive, therapeutic sealant with properties that encourage the repair of early carious lesions.
DISCLOSURE
The authors have no affiliation with any of the companies mentioned in this article.
ACKNOWLEDGMENT
The images in Figure 1 through Figure 3 are courtesy of John Flucke, DDS, Lee’s Summit, Missouri.
About the Authors
Mark L. Cannon, DDS, MS
Associate Professor, Northwestern University, Chicago, Illinois; Associate Professor of Clinical Otolaryngology-Dental Surgery, Feinberg School of Medicine, Research Director and Attending, Division of Dentistry, Ann and Robert Lurie Children’s Hospital of Chicago, Chicago, Illinois
John C. Comisi, DDS, MAGD
Private Practice, Ithaca, New York
REFERENCES
1. Beauchamp J, Caufield PW, Crall JJ, et al. Evidence-based clinical recommendations for the use of pit-and-fissure sealants: a report of the American Dental Association Council on Scientific Affairs. J Am Dent Assoc. 2008;139(3):257-268.
2. Workshop on guidelines for sealant use: recommendations. J Public Health Dent. 1995;55(5 spec iss):263-273.
3. Tellez M, Gray SL, Lim S, Ismail AI. Sealants and dental caries: dentists’ perspectives on evidence-based recommendations. J Am Dent Assoc. 2011;142(9):1033-1040.
4. Kaste LM, Selwitz RH, Oldakowski RJ, et al. Coronal caries in the primary and permanent dentition of children and adolescents 1-17 years of age: United States, 1988-1991. J Dent Res. 1996;75(spec iss):631-641.
5. Elfrink ME, Veerkamp JS, Kalsbeek H. Caries pattern in primary molars in Dutch 5-year-old children. Eur Arch Paediatr Dent. 2006;7(4):236-240.
6. Bakhshandeh A, Qvist V, Ekstrand KR. Sealing occlusal caries lesions in adults referred for restorative treatment: 2-3 years of follow-up. Clin Oral Investig. 2012;16(2):521-529.
7. Soto-Rojas AE, Escoffié-Ramírez M, Pérez-Ferrera G, et al. Retention of dental sealants placed on sound teeth and incipient caries lesions as part of a service-learning programme in rural areas in Mexico. Int J Paediatr Dent. 2012;22(6):451-458.
8. Chow LC, Vogel GL. Enhancing remineralization. Oper Dent. 2001;6:27-38.
9. Marsh PD. Dental plaque as a biofilm: the significance of pH in health and caries. Compend Contin Educ Dent. 2009;30(2):76-87.
10. McCabe JF, Yan Z, Al Naimi OT, et al. Smart materials in dentistry. Aust Dent J. 2011;56(suppl 1):3-10.
11. Van Duinen RN, Davidson CL, De Gee AJ, Feilzer AJ. In situ transformation of glass-ionomer into an enamel-like material. Am J Dent. 2004;17(4):223-227.
12. Davidson CL. Advances in glass-ionomer cements. J Appl Oral Sci. 2006;14 suppl:3-9.
13. Antonson SA, Antonson DE, Brener S, et al. Twenty-four month clinical evaluation of fissure sealants on partially erupted permanent first molars: glass ionomer versus resin-based sealant. J Am Dent Assoc. 2012;143(2):115-122.
14. Jasmin JR, van Waes H, Vijayaraghavan TV. Scanning electron microscopy study of the fitting surface of fissure sealants. Pediatr Dent. 1991;13(6):370-372.
15. Irinoda Y, Matsumura Y, Kito H, et al. Effect of sealant viscosity on the penetration of resin into etched human enamel. Oper Dent. 2000;25(4):274-282.
16. Choi JW, Drummond JL, Dooley R, et al. The efficacy of primer on sealant shear bond strength. Pediatr Dent. 1997;19(4):286-288.
17. Lynch CD, McConnell RJ. Attitudes and use of rubber dam by Irish general dental practitioners. Int Endod J. 2007;40(6):427-432.
18. Soldani F, Foley J. An assessment of rubber dam usage amongst specialists in paediatric dentistry practising within the UK. Int J Paediatr Dent. 2007;17(1):50-56.
19. Hitt JC, Feigal RJ. Use of a bonding agent to reduce sealant sensitivity to moisture contamination: an in vitro study. Pediatr Dent. 1992;14(1):41-46.
20. Feigal RJ, Musherure P, Gillespie B, et al. Improved sealant retention with bonding agents: a clinical study of two-bottle and single-bottle systems. J Dent Res. 2000;79(11):1850-1856.
21. Cehreli ZC, Gungor HC. Quantitative microleakage evaluation of fissure sealants applied with or without a bonding agent: results after four-year water storage in vitro. J Adhes Dent. 2008;10(5):379-384.
22. Asselin ME, Fortin D, Sitbon Y, Rompré PH. Marginal microleakage of a sealant applied to permanent enamel: evaluation of 3 application protocols. Pediatr Dent. 2008;30(1):29-33.
23. Eliades A, Birpou E, Eliades T, Eliades G. Self-adhesive restoratives as pit and fissure sealants: A comparative laboratory study. Dent Mater. 2013;29(7):752-762.
24. Kane B, Karren J, Garcia-Godoy C, Garcia-Godoy F. Sealant adaptation and penetration into occlusal fissures. Am J Dent. 2009;22(2):89-91.
25. de Oliveira DC, Cunha RF. Comparison of the caries-preventive effect of a glass ionomer sealant and fluoride varnish on newly erupted first permanent molars of children with and without dental caries experience. Acta Odontol Scand. 2013;71(3-4):972-977.
26. Kavaloglu Cildir S, Sandalli N. Compressive strength, surface roughness, fluoride release and recharge of four new fluoride-releasing fissure sealants. Dent Mater J. 2007;26(3):335-341.
27. Prabhakar AR, Murthy SA, Sugandhan S. Comparative evaluation of the length of resin tags, viscosity and microleakage of pit and fissure sealants - an in vitro scanning electron microscope study. Contemp Clin Dent. 2011;2(4):324-330.
28. Cannon M, Powell A, Kuttab J, Jurado R. Pilot study to measure fluoride ion penetration of hydrophilic sealant. Paper presented at: AADR Annual Meeting; March 6, 2010; Washington, DC. Abstract 1345.
29. Featherstone JD, ten Cate JM, Shariati M, Arends J. Comparison of artificial caries-like lesions by quantitative microradiography and microhardness profiles. Caries Res. 1983;17(5):385-391.
30. Vieira AE, Delbem A, Cannon M, Stock S. Remineralization and Demineralization Protocols, Use of Laboratory Micro CT. Organization for Caries Research, July 2005.
31. Cannon M, Vieira AEM, Danelon M, et al. Effect of Ions Released From Sealants on Demineralization of Enamel. Academy of Dental Materials, October 2007.
32. Silva KG, Pedrini D, Delbem AC, et al. In situ evaluation of the remineralizing capacity of pit and fissure sealants containing amorphous calcium phosphate and/or fluoride. Acta Odontol Scand. 2010;68(1):11-18.
33. Kardos S, Shi B, Sipos T. The in vitro demineralization potential of a sodium fluoride, calcium and phosphate ion-containing dentifrice under various experimental conditions. J Clin Dent. 1999;10(1 spec iss):22-25.
34. Schemehorn BR, Orban JC, Wood GD, et al. Remineralization by fluoride enhanced with calcium and phosphate ingredients. J Clin Dent. 1999;10(1 spec iss):13-16.
35. Cochrane NJ, Cai F, Huq NL, et al. New approaches to enhanced remineralization of tooth enamel. J Dent Res. 2010;89(11):1187-1197.