Techniques to Control or Avoid Cement Around Implant-Retained Restorations
Abstract
As implant dentistry has grown in popularity, many clinicians have attempted to simplify their protocols to more closely resemble conventional crown and bridge procedures. However, a thorough understanding of the biologic differences between natural teeth and dental implants, as well as the types of cements employed, is essential to achieving both short- and long-term success, as these biologic disparities between teeth and implants can lead to residual cement around implant-retained restorations, thus contributing to peri-implant disease. Four techniques are described that either reduce the flow of excessive cement or eliminate it altogether while maintaining proper occlusion without compromising the esthetics of implant-retained restorations.
-----------------------------------------------------------------------------------------------------------------------------
Implant restorative dentistry has become increasingly complicated over the years, yet outcomes have improved significantly. Despite successes, in an effort to simplify protocols, clinicians have attempted to make implant restorative procedures more like conventional crown and bridge restorations. However, due to the biologic and prosthetic differences between teeth and dental implants, this is ill-advised.1 Because the junctional epithelium and connective tissue attachment around natural teeth insert perpendicularly, this tends to limit and compartmentalize the flow of excess cement. This is in contrast to the epithelium and connective tissue around dental implants, where the connective tissue runs parallel and does not insert into the body of the implant. As a result, the flow of cement is not restricted and easily migrates apically.
Consequently, dentistry has seen an increase in the incidence of peri-mucositis and peri-implantitis. In many of these cases, this is a result of not only the difficulty of trying to remove excess cement from around implant-retained restorations, but also of clinicians using the wrong types of cement.2,3
The advantages and disadvantages of screw-retained versus cement-retained implant restorations have been discussed previously.4 In this article, the authors describe various techniques they have been utilizing to better control the flow of cement or eliminate it altogether, thereby reducing the incidence of peri-implant disease and helping to maintain a good long-term prognosis for implant-retained restorations.
Techniques to Eliminate or Control Flow of Cement
Lingual Set-Screw
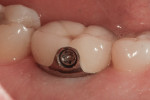
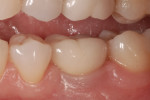
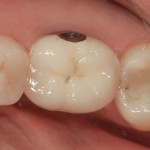
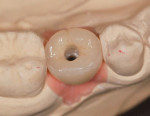
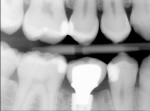
One method for eliminating cement around implant-retained restorations is to use screw retention. Occlusal screw access, however, can present problems with esthetics and make controlling the occlusion difficult. In addition, there is an increased possibility of risk of porcelain chipping. By using a lingual set-screw these concerns can be eliminated. The problems with lingual set-screws, however, are that they are difficult to manage and have a tendency to loosen because of the inability to provide adequate torque.
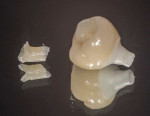
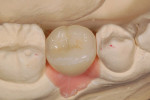
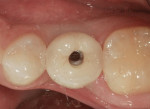
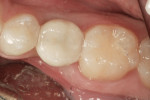
A castable threaded insert has been developed (Zest Anchors LLC, www.zestanchors.com) that utilizes the Straumann SCS® screw (Straumann, www.straumann.us). This system has worked well for the authors. Since the screw is larger than a conventional lingual set-screw, it is easy to handle, and the clinician is able to use a torque wrench to deliver the proper amount of torque required by the manufacturer. However, due to its greater size it can only be used for molars and large premolars.
A case involving this technique is depicted in Figure 1 through Figure 4.
Screw-Retained with Ceramic Insert
An effective means of improving esthetics while maintaining the occlusion is to use a laboratory-processed ceramic plug that is bonded into the screw access opening over Teflon® tape (aka, plumbers or polytetrafluoroethylene [PTFE] tape, available from various manufacturers), thereby protecting the top of the retaining screw.5 The plug can be fabricated out of either a pressed ceramic such as IPS e.max® Press (Ivoclar Vivadent, www.ivoclarvivadent.com) or a laboratory-processed composite such as Cristobal® (DENTSPLY International, www.dentsply.com).
Use of this technique not only maintains the occlusion, but also renders the access opening practically undetectable. Thus, it satisfies the esthetic demands of the patient, adequately maintains the occlusion, and meets the requirements of the clinician regarding cement elimination and retrievability.
The case shown in Figure 5 through Figure 10 utilized a Cristobal-fabricated plug bonded in with Multilink Cement® (Ivoclar Vivadent).
Rubber Dam Technique
If cement is to be used, its flow into the subgingival area must be limited. This can be accomplished with the use of a rubber dam. This technique, however, does not work with tissue-level–type implants.
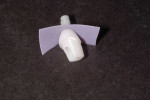
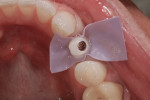
To use this technique, required materials are: scissors, light or medium rubber dam, rubber dam punch, and silicone lubricant (ie, Masque™, Bosworth Co., www.bosworth.com, or equivalent). Begin by cutting a small rectangular piece of the rubber dam, making sure that it fills—but does not overfill—the mesial–distal interdental space. Then, punch a hole in the rubber dam appropriately sized such that it will fit tightly over the abutment, and then place the abutment through the rubber dam (Figure 11).
Next, apply a small amount of lubricant to the transmucosal section of the abutment. In this case, the authors used Corsodyl® 1.0% chlorhexidine gel (GlaxoSmithKline Consumer Healthcare, www.gsk.com). Any excess that gets onto any part of the clinical crown aspect of the abutment must be cleaned off.
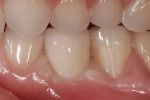
Then, seat the abutment. Rubber dam and torque the abutment into place as recommended by the implant manufacturer (Figure 12). Apply a light coating of cement and place the crown while gently holding the facial and lingual portions of the rubber dam against the gingival mucosa. Finally, clean off any excess cement (the dam will prevent the apical migration of the cement), and remove the dam (Figure 13).
Teflon (PTFE) Tape Technique
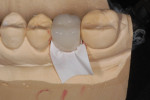
With this next technique, after confirming the intraoral fit of the crown and verifying the patient’s occlusion, the following steps are recommended.6 Start by cutting a small piece of Teflon tape (aka, plumbers or PTFE tape) and placing it in the internal surface of the crown (Figure 14). Seat the crown with the Teflon tape onto the abutment. This will adapt the tape to the internal surface of the crown and will act as a 50-micron spacer for the cement (Figure 15). Then, carefully separate the crown/Teflon tape from the abutment, being careful not to disturb the adaption of the tape from the internal surface of the crown (Figure 16).
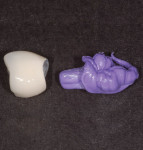
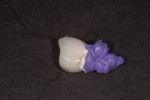
Next, inject quick-setting vinylpolysiloxane (VPS) bite registration material into the crown with the Teflon tape inside, completely filling the crown and creating a handle (Figure 17). Remove the bite registration impression and the Teflon tape from the crown. The result is that an abutment replica has thus been created that is 50 microns smaller than the actual abutment (Figure 18).
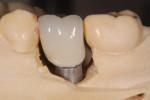
Then, place cement (it is strongly recommended not to use a resin-based cement3,4) into the crown—the authors recommend either zinc oxide eugenol or zinc phosphate—and seat the VPS replica into the crown. Excess cement will be extruded. Remove the replica, clean any excess cement from the external surface of the crown, and seat the crown intraorally. There should then be very little excess cement to remove (Figure 19 and Figure 20).
Discussion
As an increasing number of clinicians have been restoring dental implants, they have tried to simplify their protocols to more closely resemble conventional crown and bridge procedures. However, without a thorough understanding of the biologic differences between natural teeth and dental implants, as well as the types of cements employed, this can lead to both short- and long-term problems for patients.1-4 In his landmark paper, Wilson demonstrated that the timeframe from the initial signs of peri-implant disease post-cementation can range from as short as 3 months to as long as 9 years.2 The current authors have documented a case as little as 6 weeks with signs of peri-mucositis.4 Therefore, it is necessary to monitor all implant cases and be on the alert for any signs of post-delivery peri-implant disease.
For esthetic reasons, many clinicians like to place the margins of their restorations greater than 2-mm subgingival. Linkevicius et al and Agar et al have demonstrated that it is almost impossible to remove excess cement around implant restorations with subgingival margins, especially when the margins are greater than 1.5 mm, and that extensive scratching on the abutment occurs in the attempts to remove the cement. Margins that were placed 1-mm supragingival or at the gingival margin had practically all the cement removed.7,8 The vulnerability of the abutment to scratching in the effort to remove excess cement can lead to increased plaque adherence and possibly an increase in the susceptibility to peri-implant disease.9 In a prospective study by Linkevicius et al involving 53 patients requiring single-tooth implant restorations, it was determined that cement can only be completely removed from visible margins, and the dangers of subgingival cementation line location was emphasized. Additionally, the inability of radiographic examination to reveal remnants of cement was also pointed out.10
Keith et al have demonstrated that the mean marginal discrepancy of screw-retained metal–ceramic crowns on implant abutments is significantly smaller than that of cemented metal–ceramic crowns and that poorly fitted restorations may have long-term adverse effects on the implant–restorative complex within the hard and soft tissues.11 Hebel et al have stated that because the screw-access hole is directly over the implant, vertical loading and biomechanics may be compromised.12 However, with newer techniques, materials, and abutment–implant interface design, this no longer presents a problem. By implementing the techniques described herein, the authors believe that the potential adverse effects cements can present to implant-retained restorations can be reduced and possibly eliminated. However, continuous teamwork and collaboration between the restorative dentist, implant surgeon, and dental laboratory technician in case planning and design is essential to ensuring the best possible outcomes for patients.
Conclusion
In order to ensure long-term stability and predictability and reduce the incidence of peri-implant disease related to implant-retained restorations, clinicians must have a thorough understanding of the biologic differences between restorations on natural teeth and dental implants. In this article, the authors have described four techniques to either eliminate the need for cement or limit the flow of cement into the subgingival area.
EDITOR’S NOTE
Lingual Set-Screw case (Figure 1 through Figure 4): Robert Levine, DDS (Philadelphia, PA), surgery; Steven Present, DMD (North Wales, PA), prosthetics; Newtech Dental Laboratory (Lansdale, PA), laboratory work.
Screw-Retained with Ceramic Insert case (Figure 5 through Figure 10): Wendy Halpern, DMD (Plymouth Meeting, PA), surgery; Steven Present, DMD, prosthetics; Newtech Dental Laboratory, laboratory work.
Rubber Dam Technique case (Figure 11 through Figure 13): Robert Levine, DDS, surgery; Steven Present, DMD, prosthetics; Newtech Dental Laboratory, laboratory work.
Teflon Tape Technique case (Figure 14 through Figure 20): Robert Levine, DDS, surgery; Steven Present, DMD, prosthetics; Newtech Dental Laboratory, laboratory work.
ABOUT THE AUTHORS
Steven Present, DMD
Clinical Associate Professor, Temple University Kornberg School of Dentistry, Philadelphia, Pennsylvania; Instructor, Manor College, Jenkintown, Pennsylvania; Private Practice, North Wales, Pennsylvania; Fellow, International Team for Implantology
Robert A. Levine, DDS
Clinical Professor, Temple University Kornberg School of Dentistry, Philadelphia, Pennsylvania; Private Practice, Pennsylvania Center for Dental Implants & Periodontics, Philadelphia, Pennsylvania; Fellow, International Team for Implantology
REFERENCES
1. Heitz-Mayfield LJ, Lang NP. Comparative biology of chronic and aggressive periodontitis vs. peri-implantitis. Periodontol 2000. 2010;53:167-181.
2. Wilson TG Jr. The positive relationship between excess cement and peri-implant disease: a prospective clinical endoscopic study. J Periodontol. 2009;80(9):1388-1392.
3. Wadhwani C. Private e-mail correspondence, May 2012, regarding ongoing research at The University of Washington, to be published.
4. Levine R, Present S, Wilson, T. Complications with excess cement and dental implants, Parts 1 and 2: Diagnosis, recommendations and treatment of 7 clinical cases. Implant Realities. In press.
5. Wadhwani C, Piñeyro A, Avots J. An esthetic solution to the screw-retained implant restoration: introduction to the implant crown adhesive plug: clinical report. J Esthet Restor Dent. 2011;23(3):138-143.
6. Wadhwani C, Piñeyro A. Technique for controlling the cement for an implant crown. J Prosthet Dent. 2009;102(1):57-58.
7. Linkevicius T, Vindasiute E, Puisys A, Peciuliene V. The influence of margin location on the amount of undetected cement excess after delivery of cement-retained implant restorations. Clin Oral Implants Res. 2011;22(12):1379-1384.
8. Agar JR, Cameron SM, Hughbanks JC, Parker MH. Cement removal from restorations luted to titanium abutments with simulated subgingival margins. J Prosthet Dent. 1997:78(1);43-47.
9. Augthun M, Conrads G. Microbial findings of deep peri-implant bone defects. Int J Oral Maxillofac Implants. 1997;12(1):106-112.
10. Linkevicius T. Vindasiute E, Puisys A, et al. The influence of the cement margin position on the amount of undetected cement. A prospective clinical study. Clin Oral Implants Res. 2013;24(1):71-76.
11. Keith SE, Miller BH, Woody RD, Higginbottom FL. Marginal discrepancy of screw-retained and cemented metal-ceramic crowns on implant abutments. Int J Maxillofac Implants. 1999;14(3):369-378.
12. Hebel KS, Gaijar RC. Cement-retained versus screw-retained implant restorations: achieving optimal occlusion and esthetics in implant dentistry. J Prosthet Dent. 1997;77(1):28-35.
Related Content:
For more information, read Screw-Access Marking: A Technique to Simplify Retrieval of Cement-Retained Implant Prostheses at dentalaegis.com/go/cced414