Space Management: A Technique for Esthetic, Conservative Treatment of Congenitally Missing Teeth
Abstract:
The successful treatment of congenitally missing teeth (CMT)—a common dental anomaly that affects third molars and lateral incisors—requires addressing multiple challenges that frequently accompany the missing teeth. The biggest concern among patients presenting with CMT usually is esthetics. In this case report, an interdisciplinary diagnostic approach is described for conservatively managing the anatomic and esthetic challenges of a 32-year-old woman with this condition, whose main objective was to gain an appealing smile without compromising intact teeth. By utilizing space management techniques, a successful esthetic outcome was achieved without increasing the patient’s risk profile.
Congenitally missing teeth (CMT) is a common dental anomaly that typically affects third molars and lateral incisors,1 with prevalence rates reported to be between 1% and 10%.2-4 The successful treatment of CMT requires addressing multiple challenges that frequently accompany the missing teeth: inadequate bone volume and soft-tissue architecture, tipped and poorly positioned adjacent teeth, and unusual morphology of the existing teeth.5
When presenting for treatment of CMT, dissatisfaction with esthetics is often the primary concern of not only the patients themselves but also of their parents. These patients frequently suffer from low self-esteem and may avoid smiling or engaging in social interactions due to embarrassment about their smile.6 Historically, treatment options were limited; teeth adjacent to the edentulous areas were routinely prepared to be used as abutments for fixed partial dentures. Thus, esthetic success—typically the primary reason for seeking treatment—was achieved at the cost of increased lifetime biomechanical risk for the prepared teeth.7 Therefore, it is essential that the treating clinician place a high priority on the esthetic outcome while adopting a comprehensive interdisciplinary approach to both treatment planning and execution.
This case describes an interdisciplinary diagnostic approach to conservatively manage the anatomic and esthetic challenges of CMT using space management techniques that resulted in a successful esthetic outcome.
Clinical Case Overview
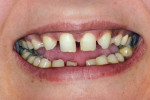
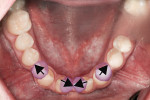
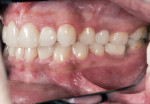
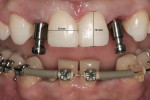
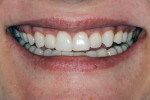
Patient History and Chief Complaint: A healthy 32-year-old woman presented with congenitally missing teeth (Figure 1). While she was self-conscious about her smile (Figure 2), she had been reluctant to proceed with treatment to replace the missing anterior teeth because she did not wish to have her virgin teeth “shaved” to allow for fixed bridge placement. Although she had a limited budget, she was committed to improving the appearance of her smile.
The patient’s medical history was noncontributory, except for smoking approximately 10 cigarettes per day, resulting in a classification of ASA Class II. In addition to expressing a desire to improve her appearance, the patient reported frequent spells of headaches, occasional stiffness of the neck muscles, and a habit of squeezing her teeth together to make all teeth meet.
Diagnostic Findings, Risk Assessment,
and Prognosis
Periodontal: The patient had generalized bleeding with low-to-moderate accumulations of calculus. Generalized mild bone loss was noted, and no periodontal pockets deeper than 4 mm were measured, resulting in a diagnosis of AAP type II, chronic periodontitis.
Risk: Moderate (due to smoking)
Prognosis: Fair
Biomechanical: Teeth Nos. 18 and 30 had overextended restorations; teeth Nos. 3, 4, 14, 21, and 31 had defective restorations; and tooth No. 13 had a cracked root.
Risk: Moderate
Prognosis: The prognosis for individual teeth was as follows: fair for teeth Nos. 18 and 30, poor for teeth Nos. 3, 4, 14, 21, and 31; and hopeless for tooth No. 13.
Functional: The patient’s function was deemed unacceptable due to occlusal dysfunction. She had a bilateral temporomandibular joint (TMJ) click and habitually squeezed her teeth to make them fit. Teeth Nos. 8, 9, 24, and 25 had Class I mobility. Tooth No. 19 had previously been lost due to a crack and fracture.
Risk: Moderate
Prognosis: Fair
Dentofacial: The patient’s smile line was high, revealing 1 mm to 2 mm of gingiva when smiling broadly.
Risk: High
Prognosis: Fair to poor
Treatment Planning Considerations
The patient rejected any removable prosthetic treatment option, and had previously refused to allow her intact teeth to be “shaved,” which precluded consideration of a fixed prosthesis. As there was insufficient space for bonded bridges, implant-retained crowns were the only remaining treatment option.
Space Management in the Maxillary Arch
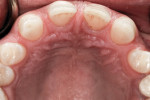
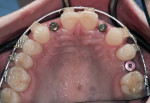
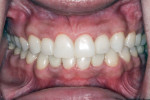
The spacing of the teeth posed a significant obstacle to implant treatment and required detailed measurement to plan for successful implant placement and restoration. A large diastema existed between the central incisors, and the spaces between the centrals and the canines were insufficient for implant placement (Figure 3). The smallest size regular implants available for lateral incisors were 3.3 mm, and each implant needed to be 1.5 mm from the adjacent teeth. Therefore, the space between centrals and canines needed to be at least 6.3 mm. To meet the maxillary esthetic needs, the central incisors and canines needed to be 8 mm wide, and the laterals needed to be 6 mm wide. Therefore, the space needed in the anterior segment was 44 mm, but only 42 mm was available.
Space Management in the Mandibular Arch
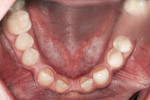
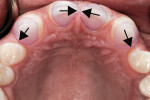
The patient was congenitally missing the lower central incisors. Both the width and height of the alveolar ridge between teeth Nos. 23 and 26 were inadequate for implant placement (Figure 4).8 Excess space was present throughout the arch, and the lateral incisors were aberrant in width at 5.2 mm. The distance between the lower premolars was 36 mm, which was 2 mm more than necessary; this necessitated direct composite augmentation of the natural lateral incisors. To lower the functional risk and allow a proper cusp–fossa relationship, it would be necessary to orthodontically correct the partial Angle Class II molar relationship on the left side as well. This preoperative position of the posterior teeth on the left side precluded correction of the occlusal dysfunction with an occlusal adjustment.
Accepted Treatment Plan
The patient initially claimed that due to her limited budget, she would accept only those procedures absolutely necessary to meet her main objective of creating a pleasing smile without cutting down intact teeth. She was, however, willing to have her bite corrected as a long-term risk management strategy. Her budget precluded the placement of porcelain veneers, therefore an alternative strategy of composite restorations was proposed. After informing her of the potentially limited lifespan and shortcomings of these restorations, she accepted with great enthusiasm the following revised treatment plan.
Orthodontically, the diastema between the upper central incisors would be closed by moving the central incisors mesially and torqueing them buccally so that they would not interfere with chewing patterns (Figure 5). The maxillary canines were to be moved distally to create the necessary room for implant placement and esthetic restoration of the lateral incisors, as well as to provide adequate space to restore the central incisors and canines to their proper width and length.
Due to bone and space limitations, the lower lateral incisors would be moved into the space of the congenitally missing lower central incisors. After the orthodontic movement, they would appear as central incisors and preserve the remaining alveolar bone between the incisors (Figure 6). Placing the implants between the natural incisors and the canines would allow the gingival complex to be managed more predictably with interproximal bone present to support the interdental papilla.
Teeth Nos. 7, 10, 13, 19, 23, and 26 would be replaced with custom abutments and implant-retained all-ceramic crowns. Teeth Nos. 18 and 30 would receive indirect full-coverage restorations, while teeth Nos. 3, 4, 14, 21, and 31 were planned for direct resin restorations.
Treatment Sequence
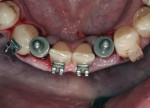
The arches were initially aligned and leveled, then the partial Class II malocclusion was treated by distalizing the left molars and upper left premolars (Figure 7). Orthodontic treatment continued until the teeth were in the optimal position for conservative esthetic restorations. At that time, implants were placed in all four lateral incisor locations as well as in the upper left second premolar and lower left first molar positions (Figure 8 and Figure 9).
The upper posterior brackets were removed and an impression was made for the upper Hawley appliance required to predictably maintain ideal spacing. When the patient returned for the removal of the anterior brackets, the Hawley retainer was delivered immediately.
The maxillary arch was restored before the orthodontic appliances were removed from the mandibular arch.
To achieve proper height-to-width proportions, the clinical crowns of the maxillary centrals and canines had to be lengthened (Figure 10) to be at least 10 mm long, but they could not be extended incisally. After careful sounding of the underlying crestal bone, the gingival height was corrected using a conservative gingivectomy technique,9 which subsequently allowed for proper proximal augmentation.
At the time of the impression for the maxillary crowns, direct composite (Renamel® Microfill, Cosmedent, www.cosmedent.com) was added to the mesial surfaces of the canines and the distal surfaces of the central incisors to create an ideal height-to-width ratio for an esthetic smile. Final vinylpolysiloxane (VPS) impressions (Take 1® Advanced, Kerr Dental, www.kerrdental.com) were taken and sent to the laboratory, along with bite registration and shade photographs for fabrication of the abutments and crowns. Due to the high smile line, zirconia abutments were selected to keep metal from showing through the free gingiva.
After the upper implant-retained crowns were cemented, the mandibular arch was ready for treatment. Prior to impressioning, the natural incisors were augmented with composite veneers (Renamel Microfill) to allow for better space distribution among the natural and crowned teeth. In a similar manner to the upper arch, a full-arch VPS impression, shade information, and bite registration were sent to the dental laboratory for fabrication of implant-retained crowns for teeth Nos. 19, 23, and 26. The crowns and custom abutments were fitted and cemented using standard protocols. In order to minimize the rebound after the orthodontic treatment, immediately after the cementation of the crowns, a bonded lingual retainer was placed from canine to canine in the lower arch.
The final treatment phase consisted of fabrication of two indirect ceramic restorations, which were bonded on teeth Nos. 18 and 30, as well as the placement of direct resin restorations (Renamel® Microhybrid, Cosmedent) on teeth Nos. 3, 4, 14, 21, and 31 using total-etch technique (OptiBond® Solo Plus, Kerr Dental) (Figure 11). Following the final restoration placement, the occlusion was again checked to ensure that the patient had equal-intensity, simultaneous, bilateral contacts in her maximum intercuspal position (MIP).
The patient was very pleased with the result because in addition to achieving a beautiful smile (Figure 12 and Figure 13), the smile was created without unnecessary tooth structure removal.
Discussion
Despite the need for orthodontics, periodontal surgery, and restorative dentistry, none of the treatments increased the patient’s risk profile or worsened the overall prognosis. In fact, all risks were reduced and the prognosis was improved. Even though she had quit her smoking habit during the treatment, the patient’s bone loss exceeded 2 mm over 3 years. Therefore, her periodontal risk remained moderate, although the prognosis was improved because she was no longer a smoker.
Conclusion
Complex dental rehabilitations do not necessarily have to be a massive undertaking. Although the magnitude of challenges can be overwhelming, careful planning and early involvement of the various specialists can provide a practical template for success.
ACKNOWLEDGMENT
The author would like to acknowledge Marc Pearlstein, DMD, of Swampscott, Massachusetts, for skillful placement of the dental implants and Leon Hermanides of Protea Dental Studio, Redmond, Washington, for the dedication, skill, and artistry needed to fabricate natural-looking restorations.
ABOUT THE AUTHOR
Bozidar “Bole” Kuljic, DDS
Private Practices in Beverly, Massachusetts, and Newburyport, Massachusetts
REFERENCES
1. Behr M, Proff P, Leitzmann M, et al. Survey of congenitally missing teeth in orthodontic patients in Eastern Bavaria. Eur J Orthod. 2011;33(1):32-36.
2. Cantekin K, Dane A, Miloglu O, et al. Prevalence and intra-oral distribution of agenesis of permanent teeth among Eastern Turkish children. Eur J Paediatr Dent. 2012;13(1):53-56.
3. Goya HA, Tanaka S, Maeda T, Akimoto Y. An orthopantomographic study of hypodontia in permanent teeth of Japanese pediatric patients. J Oral Sci. 2008;50(2):143-150.
4. Afify AR, Zawawi KH. The prevalence of dental anomalies in the Western region of Saudi Arabia. ISRN Dent. 2012;2012:837270.
5. Borzabadi-Farahani A. Orthodontic considerations in restorative management of hypodontia patients with endosseous implants. J Oral Implantol. 2012;38(6):779-791.
6. Park JH, Kim A, Tai K. Congenitally missing lateral incisors: treatment. Dent Today. 2011;30(5):81-86.
7. Sabri R. Management of missing maxillary lateral incisors. J Am Dent Assoc. 1999;130(1):80-84.
8. Ishikawa T, Salama M, Funato A, et al. Three-dimensional bone and soft tissue requirements for optimizing esthetic results in compromised cases with multiple implants. Int J Periodontics Restorative Dent. 2010;30(5):503-511.
9. Kois JC. The restorative-periodontal interface: biological parameters. Periodontol 2000. 1996;11:29-38.
Related Content:
A CE article, Managing Congenitally Missing or Microdontic Lateral Incisors, is available at dentalaegis.com/go/cced415