Immediate Implant Placement and Provisionalization Using a Customized Anatomic Temporary Abutment (CATA) to Achieve Gingival Margin Stability
As advances have progressed in implant dentistry, patient acceptance and long-term success rates have been on the rise. With technology ever improving, clinicians have taken treatment approaches that are aimed at a more immediate timetable as well as esthetics. The immediate implant placement and provisionalization protocol is now being applied to the anterior region. With esthetic concerns being at the forefront of implant dentistry, this case report highlights the importance of five key parameters that are related to the risk of recession following dental implant restoration in maxillary anterior sites.
Recent advances in surgical and restorative techniques in implant dentistry have improved success rates, patient acceptance, and long-term outcomes of tooth replacement. Implant design and surface improvements have helped clinicians direct their treatment approach towards a more immediate timetable as well as a more esthetically driven one. Numerous reports on immediate implant placement and immediate provisionalization, as well as on early and immediate implant placement and loading protocols, have claimed high degrees of success.1-7
The immediate implant placement and provisionalization protocol has now been applied to the anterior esthetic zone with the goal of maintaining and even enhancing the gingival architecture over time. Many authors have reported excellent results with immediate implant placement and provisionalization by maintaining or developing the gingival contours and proper architecture in the anterior esthetic zone in fresh extraction sites.8-14 However, some studies have shown that marginal gingival recession does occur on a significant number of sites over time.15-17 With esthetic concerns being at the forefront, clinicians are now focusing on five key parameters that are related to the risk of recession following dental implant restoration:
• The location of the implant platform should be palatally positioned in the extraction socket.18-21
• The buccal bone should be maintained near the implant platform. When the implant is positioned toward the palate, the implant platform is at a farther distance from the buccal bone, resulting in a larger horizontal defect dimension (HDD). This larger HDD has been shown to better maintain the buccal bone and, thereby, reduce the risk of gingival recession.22-24
• The gingival biotype thickness plays a role in the potential recession that occurs, with a lesser degree of recession associated with a thicker gingival biotype.25-27
• The approach of placement of implants into extraction sites with flapless surgery results in better hard and soft tissue stability, and can minimize marginal gingival recession.28-32 However, despite this focus on reducing surgical manipulation and its correlation on changes in gingival margin heights, recent studies are now reporting that gingival recession can still occur even with a flapless approach.12,13,33-35
• Equally important is the implant–abutment restoration interphase or the immediate abutment and provisional restoration complex.14,34,36-38 The shape and contour of the temporary abutment and provisional restoration complex can influence the development and management of the soft tissue, thus determining the final emergence profile.18,39-42
These five key parameters should be the foundation for the protocol for immediate implant placement and provisionalization in the anterior esthetic zone, with the goal of reducing the risk for future recession.
Case Report
The following case report focuses on a technique that, beyond achieving implant integration, aims to attain proper emergence profile development with the goal of minimizing recession in a fresh extraction site in the anterior esthetic zone.
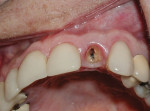
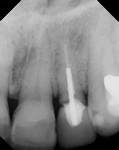
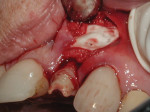
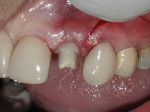
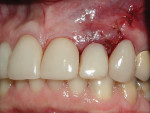
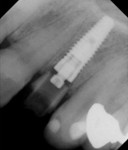
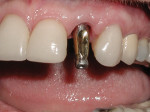
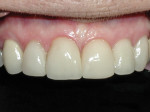
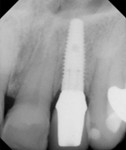
A 56-year-old woman presented to the authors’ office after having fractured off the clinical crown portion and post on tooth No. 10 (Figure 1). The remaining root had an unfavorable prognosis and was nonrestorable, as seen in the radiograph (Figure 2). The adjacent teeth all had full-coverage restorations, leaving the proposed replacement of tooth No. 10 a highly demanding esthetic challenge. The proposed treatment was for extraction of the remaining root followed by immediate implant placement, immediate placement of a customized anatomic temporary abutment (CATA), and fabrication and cementation of an immediate provisional restoration.
Surgical Protocol
The patient was given 2 grams of amoxicillin 1 hour prior to surgery and instructed to take 500 mg t.i.d. for 5 days. For postoperative analgesia, Dolobid (500 mg) was utilized two times a day (b.i.d.) for 2 days following completion of surgery. Initially, tooth No. 10 was extracted with a flapless approach under local anesthesia. The extraction socket was then thoroughly curetted and examined with bone sounding. It was determined that a fenestration was present on the labial aspect of the socket. A full-thickness flap was then elevated on the labial aspect for access to thoroughly debride and subsequently perform bone grafting to the fenestrated labial plate. Preparation of the implant site was then completed following Nobel Biocare’s (www.nobelbiocare.com) surgical drilling protocol along with the use of a surgical guide for precise restoratively driven implant placement. The surgical guide was fabricated from an impression taken preoperatively.
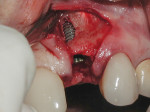
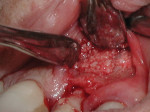
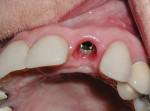
Implant placement location was based on the tri-dimensional implant protocol.14,18,38 The implant platform was placed 1 mm to 2 mm to the palate of the extraction socket and was centered mesial distally and approximately 3-mm apical to the proposed cementoenamel junction (CEJ) of the final restoration as it relates to the existing gingival margin.43 Excellent initial implant stability was achieved (greater than 35 Ncm).44,45 The implant placed was a 4.3-mm x 13-mm NobelReplace® Select™ Tapered Groovy® (Nobel Biocare) with a significant portion of the implant body being exposed due to the fenestration found on the labial (Figure 3). The seven exposed threads of the implant were grafted with a freeze-dried bone allograft (FDBA) (Figure 4) (Puros®, Zimmer Dental, www.zimmer.com), and a collagen resorbable barrier membrane (Ossix® Plus, OraPharma, Inc., www.orapharma.com) was placed (Figure 5).
Restorative Protocol
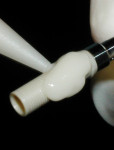
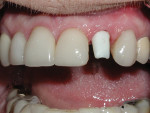
Following the placement of the implant and completion of the surgical phase of the treatment, a stock polyether ether ketone (PEEK) temporary abutment (Nobel Biocare) was used with an auto-cured composite (Systemp®, Ivoclar Vivadent, www.ivoclarvivadent.com) to develop a CATA for a cement-retained provisional restoration (Figure 6). The composite was added to extend over the entire length of the temporary abutment and allowed to auto-cure to a solid state. The CATA was then contoured as it was passively seated into the implant without encroaching on the gingival tissues. With the unfinished CATA seated into the implant, it was then marked for the gingival contour, location of the gingival margin, and desired length, with occlusal clearance and room for a provisional restoration in mind (Figure 7).
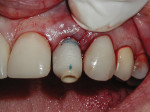
The CATA was then removed and shaped to create the appropriate emergence anatomy, exactly mimicking that of the tooth extracted. In establishing the desired emergence profile, the focus was on not over-contouring the composite and thus compromising the gingival contours, as this could lead to future gingival recession.38,39,41,46 The facial contour of the CATA was either flat or under-contoured. The majority of the contouring was completed out of the mouth (Figure 8). Once properly contoured, the CATA was then hand-tightened to approximately 15 Ncm to the implant. Using either a diamond or a fissure bur with copious water, the final preparation of the CATA was then completed, achieving gingival margin contour on the labial interproximal and lingual for final margin placement. The composite margin was prepared to approximately 0.5-mm supragingival for the provisional crown margin access to ensure total removal of excess cement (Figure 9).
Vinylpolysiloxane (VPS) impression material was then placed into the abutment orifice and covered with a composite material to create a solid abutment complex. A provisional restoration was then fabricated and cemented using routine crown and bridge procedures (Figure 10). Cement was easily accessible, as the abutment margin–provisional interphase was supragingival, allowing excess cement to be readily removed. Special attention was given to verify that no occlusal contact with the opposing teeth existed either in intercuspal position or upon any excursive movements. Then, 5-0 chromic gut sutures were placed to adapt the surgical flap in the desired position. The radiograph of the implant, CATA, and provisional restoration showed a radiolucent space at the implant–abutment connection (Figure 11). This radiolucent space at the implant–abutment interface was due to the lucency of the PEEK material of the temporary cylinder.
Follow-Up and Final Restorative Protocol
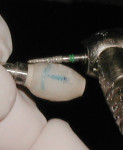
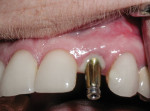
The patient was given oral hygiene instruction and was advised to avoid any function on this implant provisional restoration for approximately 3 to 5 weeks.47 The patient returned to the office for follow-up visits at 1, 3, and 6 weeks, and at 3 months. At the 3-month visit, implant restorative procedures for the final implant crown were initiated. Waiting 3 months enabled the emergence profile to develop and achieve stability, ultimately allowing for excellent soft-tissue contours.48-51 At this time the abutment and provisional crown were removed, revealing excellent soft-tissue development (Figure 12). A fixture level impression technique was used to capture the emergence profile developed with the CATA; this was the first time that the CATA and provisional restoration were removed. This allowed for maximum stability and maturation of the gingival complex and emergence profile. Utilizing a customized fixture level impression technique allows the exact shape of the created emergence profile to be duplicated for the laboratory phase. This technique involved placing a straight profile closed tray impression coping (Nobel Biocare) (Figure 13) and then placing light-cured flowable composite in the gap between the impression coping and the gingival complex (Figure 14). The laboratory was given an impression that exactly matches the developed emergence profile. A patient-specific Procera® Zirconia abutment (Nobel Biocare) was then fabricated to exactly replicate the specific emergence profile. The abutment was then placed and torqued into the implant (35 Ncm) without putting pressure on and compromising the gingival complex (Figure 15). An optimally contoured ceramic crown was fabricated and cemented (Figure 16).
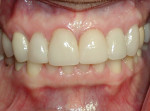
The 5-year follow-up showed excellent stability of the soft-tissue complex with no gingival recession (Figure 17) and excellent bone levels (Figure 18). The immediate functional and esthetic result was extremely satisfactory to the patient.
Conclusion
Success of implant dentistry in the esthetic zone is now judged by the integration of the restoration with the gingival complex, along with the development of the soft-tissue emergence profile and sustaining it over time. Various techniques, both surgically and restoratively, are being developed to accomplish this goal. Strong consideration should be given to the implant–abutment–restoration interphases. This aspect can greatly alter the shape of the emergence profile and ultimately affect the esthetic outcome.
The purpose of this article was to present a novel technique that enhances implant placement by establishing proper subgingival contours in the abutment phase. By doing so, the proper emergence profile can be developed and sustained in the gingival complex. This technique has a significant clinical effect when an implant is immediately placed with an immediate provisional in a fresh extraction site. The exact shape of the pre-existing emergence profile (extraction site), or the proposed emergence profile desired, can be optimally contoured into the CATA, and ultimately the final abutment. By utilizing a properly contoured CATA, accurately copying the developed emergence profile with a custom implant impression technique, and transferring this into the final abutment contour, significant reduction in gingival margin changes can be achieved. This stability of the soft-tissue complex then increases the potential for a more acceptable and desirable esthetic outcome. This technique of utilizing an immediate cement-retained provisional restoration also resembles a more traditional crown and bridge approach, which is user-friendly to most restorative dentists.
The success of this case is not only related to the proposed technique but also proper case selection for immediate placement/provisionalization in the anterior esthetic zone. Some clinical situations, including inadequate primary implant stability, hard or soft tissue deficiencies that could compromise long-term implant survival and esthetics, and when there are concerns about patient compliance, may not be appropriate for this technique and must be recognized during treatment planning.
DISCLOSURE
The authors acknowledge no financial or material support while conducting this study.
ABOUT THE AUTHORS
Scott B. Ross, DDS
Adjunct Professor, Graduate Department of Periodontology, Nova Southeastern University College of Dental Medicine, Fort Lauderdale, Florida; Private Practice in Periodontics, Miami, Florida
Gregory A. Pette, DMD, MS
Adjunct Professor, Graduate Department of Periodontology, Nova Southeastern University College of Dental Medicine, Fort Lauderdale, Florida; Private Practice, Fort Myers, Florida
REFERENCES
1. Mayer TM, Hawley CE, Gunsolley JC, Feldman S. The single-tooth implant: a viable alternative for single-tooth replacement. J Periodontal. 2002;73(7):687-693.
2. Chaushu G, Chaushu S, Tzohar A, Dayan D. Immediate loading of single-tooth implants: immediate versus non-immediate implantation. A clinical report. Int J Oral Maxillofac Implants. 2001;16(2):267-272.
3. Lazzara R, Testori T, Meltzer A, et al. Immediate Occlusal Loading (IOL) of dental implants: predictable results through DIEM guidelines. Pract Proced Aesthet Dent. 2004;16(4):3-15.
4. Cornelini R, Scarano A, Covani U, et al. Immediate one-stage postextraction implant: a human clinical and histologic case report. Int J Oral Maxillofac Implants. 2000;15(3):432-437.
5. Buser D, Chen ST, Weber HP, Belser UC. Early implant placement following single-tooth extraction in the esthetic zone: biologic rationale and surgical procedures. Int J Periodontics Restorative Dent. 2008;28(5):441-451.
6. Lazzara RJ. Immediate implant placement into extraction sites: surgical and restorative advantages. Int J Periodontics Restorative Dent. 1989;9(5):332-343.
7. Cornelini R, Cangini F, Covani U, Wilson TG Jr. Immediate restoration of implants placed into fresh extraction sockets for single-tooth replacement: a prospective clinical study. Int J Periodontics Restorative Dent. 2005;25(5):439-447.
8. Covani U, Barone A, Cornelini R, Crespi R. Soft tissue healing around implants placed immediately after tooth extraction without incision: a clinical report. Int J Oral Maxillofac Implants. 2004;19(4):549-553.
9. Werbitt MJ, Goldberg PV. The immediate implant: bone preservation and bone regeneration. Int J Periodontics Restorative Dent. 1992;12(3):206-217.
10. Fabbri G, Ban G, Mancini R. Immediate loading and flapless, postextraction, single-tooth implant restoration: advantages and indications. Pract Proced Aesthet Dent. 2008;20(10):633-639.
11. Kan JY, Runcharassaeng K, Lozada JL. Immediate placement and provisionalization of maxillary anterior single implants: 1-year prospective study. Int J Oral Maxillofac Implants. 2003;18(1):31-39.
12. Kan JY, Runcharassaeng K, Lozada JL, Zimmerman G. Facial gingival tissue stability following immediate placement and provisionalization of maxillary anterior single implants: a 2- to 8-year follow-up. Int J Oral Maxillofac Implants. 2011;26(1):179-187.
13. Wöhrle PS. Single-tooth replacement in the aesthetic zone with immediate provisionalization: fourteen consecutive cases reports. Pract Periodontics Aesthet Dent. 1998;10(9):1107-1114.
14. Kan JY, Runcharassaeng K, Lozada JL. Immediate placement and provisionalization of maxillary anterior single implants: A surgical and prosthodontic rationale. Pract Periodontics Aesthet Dent. 2000;12(9):817-824.
15. Grunder U. Stability of the mucosal topography around single-tooth implants and adjacent teeth: 1-year results. Int J Periodontics Restorative Dent. 2000;20(1):11-17.
16. Lindeboom JA, Tjiook Y, Kroon FH. Immediate placement of implants in periapical infected sites: a prospective randomized study in 50 patients. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(6):705-710.
17. Norton MR. A short-term clinical evaluation of immediately restored maxillary TiOblast single-tooth implants. Int J Oral Maxillofac Implants. 2004;19(2):274-281.
18. Buser D, Martin W, Belser UC. Optimizing esthetics for implant restorations in the anterior maxilla: anatomic and surgical considerations. Int J Oral Maxillofac Implants. 2004;19(suppl):43-61.
19. Chen ST, Darby IB, Reynolds EC, Clement JG. Immediate implant placement postextraction without flap elevation. J Periodontol. 2009;
80(1):163-172.
20. Chen ST, Darby IB, Reynolds EC. A prospective clinical study of non-submerged immediate implants: clinical outcomes and esthetic results. Clin Oral Implants Res. 2007;18(5):552-562.
21. Evans CD, Chen ST. Esthetic outcomes of immediate implant placements. Clin Oral Implants Res. 2008;19(1):73-80.
22. Grunder U, Gracis S, Capelli M. Influence of the 3-D bone-to-implant relationship on esthetics. Int J Periodontics Restorative Dent. 2005:25(2):113-119.
23. Jemt T, Lekholm U. Single implants and buccal bone grafts in the anterior maxilla: measurements of buccal crestal contours in a 6-year prospective clinical study. Clin Implant Dent Relat Res. 2005;7(3):127-135.
24. Chen ST, Darby IB, Adams GG, Reynolds EC. A prospective clinical study of bone augmentation techniques at immediate implants. Clin Oral Implants Res. 2005;16(2):176-184.
25. Kan JY, Rungcharassaeng K, Umezu K, Kois JC. Dimensions of peri-implant mucosa: an evaluation of maxillary anterior single implants in humans. J Periodontol. 2003;74(4):557-562.
26. Kois JC. Predictable single tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2001;22(3):199-206.
27. Kan JY, Morimoto T, Rungcharassaeng K, et al. Gingival biotype assessment in the esthetic zone: visual versus direct measurement. Int J Periodontics Restorative Dent. 2010:30(3):237-243.
28. Hahn J. Single stage, immediate loading, and flapless surgery. J Oral Implantol. 2000;26(3):193-198.
29. Campelo LD, Camara JR. Flapless implant surgery: a 10-year clinical retrospective analysis. Int J Oral Maxillofac Implants. 2002;17(2):271-276.
30. Rocci A, Martignoni M, Gottlow J. Immediate loading in the maxilla using flapless surgery, implants placed in predetermined positions, and prefabricated provisional restorations: a restrospective 3-year clinical study. Clin Implant Dent Relat Res. 2003;5(suppl 1):29-36.
31. Oh TJ, Shotwell J, Billy E, et al. Flapless implant surgery in the esthetic region: advantages and precautions. Int J Periodontics Restorative Dent. 2007;27(1):27-33.
32. Covani U, Crespi R, Cornelini R, Barone A. Immediate implants supporting single crown restoration: a 4-year prospective study. J Periodontol. 2004;75(7):982-988.
33. Covani U, Cornelini R, Barone A. Bucco-lingual bone remodeling around implants placed into immediate extraction sockets: a case series. J Periodontol. 2003;74(2):268-273.
34. Barone A, Rispoli L, Vozza I, et al. Immediate restoration of single implants placed immediately after tooth extraction. J Periodontol. 2006;77(11):1914-1920.
35. Chen ST, Darby IB, Reynolds EC, Clement JG. Immediate implant placement postextraction without flap elevation. J Periodontol. 2009;80(1):163-172 .
36. Jemt T. Restoring the gingival contour by means of provisional resin crowns after single-implant treatment. Int J Periodontics Restorative Dent. 1999;19(1):20-29.
37. Crespi R, Capparè P, Gherlone E, Romanos GE. Immediate occlusal loading of implants placed in fresh sockets after tooth extraction. Int J Oral Maxillofac Implants. 2007;22(6):955-962.
38. Kois JC, Kan JY. Predictable peri-implant gingival aesthetics: surgical and prosthodontic rationales. Pract Proced Aesthet Dent. 2001;13(9):691-698; quiz 700, 721-722.
39. Priest GF. The esthetic challenge of adjacent implants. J Oral Maxillofac Surg. 2007;65(7 suppl 1):2-12.
40. Touati B. Improving aesthetics of implant-supported restorations. Pract Periodontics Aesthet Dent. 1995;7(9):81-92.
41. Touati B, Guez G, Saadoun A. Aesthetic soft tissue integration and optimized emergence profile: provisionalization and customized impression coping. Pract Periodontics Aesthet Dent. 1999;11(3):305-314.
42. Saadoun AP, LeGall M, Touati B. Selection and ideal tridimensional implant position for soft tissue aesthetics. Pract Periodontics Aesthet Dent. 1999:11(9):1063-1072.
43. Magne P, Gallucci GO, Belser UC. Anatomic crown width/length ratios of unworn and worn maxillary teeth in white subjects. J Prosthet Dent. 2003;89(5):453-461.
44. Neugebauer J, Traini T, Thams U, et al. Peri-implant bone organization under immediate loading state. Circularly polarized light analyses: a minipig study. J Periodontol. 2006;77(2):152-160.
45. Drago CJ, Lazzara RJ. Immediate occlusal loading of Osseotite implants in mandibular edentulous patients: a prospective observational report with 18-month data. J Prosthodont. 2006;15(3):187-194.
46. Touati B. Integration of digital-ceramic restorations. Pract Proced Aesthet Dent. 2004;16(8):546.
47. Barewal RM, Oates TW, Meredith N, Cochran DL. Resonance frequency measurement of implant stability in vivo on implants with a sandblasted and acid-etched surface. Int J Oral Maxillofac Implants. 2003;18(5):641-651.
48. Small PN, Tarnow DP. Gingival recession around implants: a 1-year longitudinal prospective study. Int J Oral Maxillofac Implants. 2000;15(4):527-532 .
49. Grunder U. Stability of the mucosal topography around single-tooth implants and adjacent teeth: 1-year results . Int J Periodontics Restorative Dent. 2000;20(1):11-17.
50. Oates TW, West J, Jones J, et al. Long-term changes in soft tissue height on the facial surface of dental implants. Implant Dent. 2002;11(3):272-279.
51. Priest G. Predictability of soft tissue form around single-tooth implant restorations. Int J Periodontics Restorative Dent. 2003;23(1):19-27.
Related Content: For more information, read The Team Approach to Esthetic Immediate Implant Placement at dentalaegis.com/go/cced389