A Predictable Approach to an All-Ceramic Full-Arch Restoration
Abstract:
This mandibular restoration case using e.max® demonstrates a predictable approach to placing an all-ceramic full-arch restoration. The case also discusses the advantages of using full-contour zirconia (FCZ) for its beauty as well as its resistance to breakage, in light of the current trend towards better tooth morphology and color with FCZ restorations. An additional benefit of FCZ is that the soft-tissue response around units using this highly biocompatible material is much like that at the margins of natural teeth, making it an ideal restorative option, especially when the patient’s bite is being opened.
Dentistry continues to see an increase in the use of full-contour zirconia (FCZ) restorations. Once considered almost exclusively for posterior regions, FCZ restorations have improved in areas such as tooth morphology and color development and have, therefore, become more commonly used in anterior areas. These restorations feature biocompatibility and a natural esthetic appeal, along with increased resistance to breakage. As such, this author has witnessed a significant expansion in the placement of single units of monolithic zirconia.
New Patient Examination
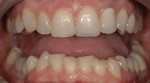
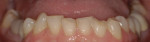
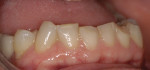
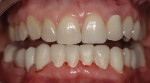
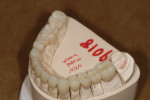
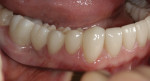
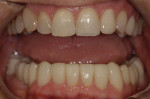
An adult female patient requested cosmetic rehabilitation of a badly dilapidated mandibular dental arch (Figure 1). Her perception was that her lower teeth appeared uneven, worn and old.1 Her medical history was unremarkable. Examination revealed her temporomandibular joints to be supple and moving freely; all were free of clicking and popping noises. She exhibited no deviation on opening or closing and was able to open to 39 mm (Figure 2 and Figure 3).
The mandibular anterior teeth exhibited loss of tooth structure due to abrasion, presently described as dental compression syndrome (DCS). The mandible appeared to be overly closed. In studies of some 500 patients, Henry Shimbashi, DDS, of Edmonton, Alberta, Canada, determined that there was an ideal relationship that existed between the maxilla and mandible. Part of this relationship includes a measurement from the gingival margins of the maxillary central incisors to the gingival margins of the mandibular incisors. Shimbashi concluded that the ideal measurement is 17 mm plus or minus 1 mm.2 As in the present case, the Shimbashi number is often used to aid in the diagnosis of an over-closed mandible when dental compression syndrome is present. DCS has been defined as the sum total of all parafunctional activity that occurs between the mandible and maxilla.3 In this case, the Shimbashi measurement between the gingival margin of tooth No. 8 and the gingival margin of tooth No. 26 was 13 mm.
Restorative Plan
Treatment began with full-arch impressions of the maxillary and mandibular teeth. A facebow transfer and a wax bite were used to mount the study casts. The mounted study casts were used to find the first point of contact between the two arches.
The restoration of the lower arch would begin with the reshaping of the occlusal surfaces of the maxillary teeth. In the condition at presentation, many of the teeth had supererupted and the resulting plane of occlusion had become distorted.4 Enamoplasty would create a more uniform occlusal surface of the maxillary teeth and allow the lower arch to be built with a more ideal occlusal scheme.5 When the enamoplasty was complete, the interference to closure was eliminated, and MIP could be reached without any skid. Using the Dawson-inspired bilateral manipulation, the patient’s occlusion was marked during guided closure.6 Interferences were eliminated and the mandible closed into centric occlusion (CO) without any interference, skid, or movement. The coincidence of CO and centric relation (CR) were verified using the TekScan dental occlusal analysis system (TekScan® Inc., www.tekscan.com). This step was critical because the final restoration would be fabricated 3-mm taller than the pretreatment vertical dimension of occlusion. This would yield a Shimbashi measurement of 17 mm, which is well within the normal range of measurements for anterior teeth.7 As long as the clinicians could mount the final casts using this joint relationship, the case could be opened, built, and inserted into the patient’s mouth without generating any interferences.8 This procedure also would allow the joints to accept the new vertical dimension of occlusion free of pain and discomfort.6
New impressions were taken of both dental arches, along with a facebow transfer and a new bite. A smile design plan was developed to open the bite 3 mm for prosthetic convenience.9 A wax-up would be fabricated at the new vertical dimension of occlusion for the lower arch that would restore natural tooth form, ideal arch form, ideal occlusal plane, and a cusp fossa occlusal scheme.10 A Sil-Tech® (Ivoclar Vivadent, www.ivoclarvivadent.com) putty stent would be fabricated from the wax-up and used in the mouth for fabrication of the provisional restorations.
The planned restorations were IPS e.max® crowns (Ivoclar Vivadent) for teeth Nos. 22 and 27, e.max veneers for teeth Nos. 23 through 26, FCZ bridges for teeth Nos. 19 through 21 and 28 through 30, and a full-coverage FCZ crown for tooth No. 31.
Preparation of Mandibular Arch
Mandibular anesthesia was achieved using two carpules of lidocaine 1/50 in the form of mandibular blocks. The preparation of the teeth began with classic conservative porcelain laminate veneer preparations of teeth Nos. 23 through 26. A bite (SuperDent PVS, Darby Dental Supply LLC, www.darbydental.com) was taken of the prepared teeth in full occlusion. This bite is an important step to maintaining the relationship of the prepared teeth in the mandibular arch with the teeth of the maxillary arch.
The preparation of the mandibular arch continued with the preparation of teeth Nos. 19 through 22. Because the clinicians were opening the bite 3 mm, it was not necessary to reduce an excessive amount of tooth structure from the occlusal aspect of the teeth.11 After the preparations were complete, another bite was taken. First, the bite for teeth Nos. 23 through 26 was carefully placed on the lower anterior teeth. Then the bite registration material was flowed onto the prepared teeth Nos. 19 through 22. The patient was guided to careful closure, making certain the anterior bite (teeth Nos. 23 through 26) was fully seated.
At this point, the clinicians had prepared more than half of the teeth in this restoration, and their careful use of the wax bites taken preserved the joint/fossa relationships for both temporomandibular joints.
Upon completion of the preparation of teeth Nos. 27 through 31, the final bite was taken, with careful attention given to fully seat the bites that were taken of prepared teeth Nos. 19 through 26 before introducing the bite registration material into the prepared teeth Nos. 27 through 31. The finished bite was removed and would be used by the dental laboratory to mount the master cast to the opposing cast. Because the bites captured the dental arches in CO/CR, the dental lab would be able to predictably open the bite 3 mm to create the final restorations.12
When the preparations were complete, the prepared teeth were flushed with water and lightly air-dried using a three-way syringe. Traxodent® Hemodent Paste Retraction System (Premier Dental, www.premusa.com) was introduced into each tooth preparation and placed against the soft tissue in the sulcus. Traxodent was left in contact with the soft tissues for 2 minutes, after which it was thoroughly rinsed away with high-volume water and air from the three-way syringe. The finish margin of the tooth preparations was clean and dry and ready for the final impressions.
Final impressions for the master cast were taken using Cinch™ 90 medium-body material (Parkell, Inc, www.parkell.com) in a full-arch mandibular impression tray. The material was dispensed from a self-mixing syringe. A second syringe containing Cinch 90 light-body flow was equipped with a flow tube to aid in placing the final impression material into the dental sulcus to more easily capture the many finish lines for the master cast.
The Sil-Tech putty stent was filled with LuxaTemp (DMG America, www.dmg-america.com) Vita shade B1, and was seated on the prepared teeth. The stent was left to set on the prepared teeth for 70 seconds and removed. The provisional restorations remained within the Sil-Tech stent for 5 minutes. This allowed the provisional restorative material to reach a complete polymerization. The provisional restorations were then removed from the stent, trimmed, and taken to the mouth for try-in and adjustment. Since the wax-up was done with the opened vertical dimension, the provisional restoration opened the bite by 3 mm. Wearing the provisional restoration for 2 weeks gave the patient an opportunity to evaluate the new occlusal scheme and new vertical height of occlusion.13 The provisional restorations were cemented onto the prepared teeth using TempoCem® NE (DMG America) (Figure 4).
The Restorations
The e.max restorations can be fabricated in two different ways. They may be pressed using a lost-wax technique, or they may be milled using a computer-aided design/computer-aided manufacturing (CAD/CAM) technique. Based on experience, the author asserts that the press technique produces a stronger restoration and shows better marginal adaptation.
For teeth Nos. 22 through 27, the e.max restorations were first waxed to full contour and then buried in investment plaster in a casting ring, to ultimately be pressed in an oven using a lost-wax technique. The desired ingot shade of lithium disilicate was heated in a furnace and the units pressed into the prepared form using a specially designed press oven. After the casting ring cooled down, it was divested using glass beads to avoid damaging the restorations.
After divesting and clean-up, each unit was fit back onto the master dies, and adjustments were made for fit. The units were then cut back to allow the placement of custom esthetic porcelains.14 Being more resistant to breakage and fracture than other stacked or pressed ceramic systems, lithium disilicate creates beautiful esthetic veneers and full-coverage restorations for the esthetic zone.
The FCZ restorations were fabricated using a CAD/CAM technique.15 First, the polyvinylsiloxane full-arch impressions were poured in special dental stone that was chosen for its photographic properties. The master casts were scanned into the computer of the CAD/CAM milling machine. Digital images were made from the scans of the stone casts, and these images were stored in the computer.
The digital, working casts were then “waxed up” using a program that produces a virtual wax-up. The virtual wax-up was adjusted to facilitate proper contour and height, and any issues of proportion were addressed at this time. One of the most important issues to be addressed with FCZ bridges is the size of the connectors between the individual units of the bridge. The connectors may be the weakest part of the FCZ bridge; it has been suggested that small connectors could fracture under occlusal load. One dental laboratory has suggested connectors need a load capacity number of at least 27 to resist breakage induced by heavy occlusal forces. This number is the sum of the height of the connector multiplied by the width of the connector, which is then multiplied by the depth of the connector. For example: If the connector is 3-mm wide and 4-mm high and the depth is 3 mm, then 3 X 4 = 12, 12 X 3 = 36; 36 is greater than 27, so the connector would be considered unbreakable in the human mouth under load.16
After the various esthetic issues were addressed, the “waxed case” was ready for fabrication by the milling unit. The milling unit was calibrated to fabricate the FCZ bridges 6% larger than the needed final size.17 The FCZ restorations came out of the milling unit a frosty white color and were somewhat fragile in this unfinished state.
It is during this phase that the final colors are introduced into the dental units. The units were first dipped into a liquid bath that contains the basic color of the restorations, such as Vita B1. Then, any needed color variations such as incisal violet or warm hues at the gingival margin, or any maverick stain or incisal highlight, are hand-painted onto the units with a brush.18
Zirconium (Zr) is easily found in the earth’s crust.19 Zirconia (ZrO2) is formed by the simple addition of oxygen to the pure zirconium metal.20 The addition of yttrium (Y2T2) produces a crystal that is both strong and resists crack generation because of the unique “transformation toughening” that occurs when Zirconia goes from a tetragonal phase to a monolithic phase.21 The FCZ units are then sintered in an oven at 1,650 degrees F for 6.5 hours. It is during this sintering process that the units shrink to the proper size to fit the tooth preparations.22
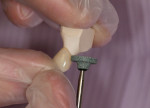
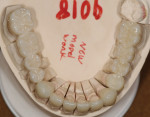
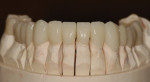
Upon completion of the sintering process, the restorations were ready for final shaping and polishing (Figure 5). Since the individual units had the base color throughout, adjustments were only needed to alter the shape; there was no metal to show through, even on the occlusal. Shaping and polishing was easily accomplished using a slow-speed green stone, GM702HP (Axis Dental, www.axisdental.com), a hard rubber polishing wheel, P0301G (Axis Dental), and a high-shine diamond-impregnated rubber wheel, R17DFHP (Dialite® HP, Brasseler USA, www.brasselerusa.com). The surface of FCZ is very smooth and resistant to bacterial adhesion, which adds to the high degree of its biocompatibility. If any additional surface stains are used, it is important to polish these stains from the surface of the units where they come in contact with the soft tissues.23 Microscopically, surface stains are very rough and are a breeding ground for bacterial colonization, which can cause soft-tissue irritation. The final ceramic units seated on the master cast showed nice proportions, ideal arch form, and a fully developed occlusal form (Figure 6 through Figure 8).
Cementation Process
On the day of final cementation, the patient was first anesthetized using one carpule of lidocaine 1/50 in the form of infiltration at the mental foramen, bilaterally. The provisional restorations were evaluated for both comfort and wear and were removed. The preparations were thoroughly cleaned to remove any remnants of the temporary cement. The e.max restorations were tried on the preparations and checked with dental floss to assess the contact areas. After adjusting the contacts to allow full seating of all of the e.max units, the posterior FCZ bridges were tried in for marginal fit and contact with the e.max units. After adjustments were made, the occlusion was checked using a thin blue paper. Interferences were adjusted and polished, and the final units were ready for cementation. The patient then had her first opportunity to see the final restorations in her mouth.
The FCZ bridges were cemented first using Fuji® PLUS™ Capsules (GC America, www.gcamerica.com). The cement was allowed to reach a final set and the flash was removed and cleaned. The anterior e.max units were tried in to make sure the final cementation of the FCZ bridges had not caused any interference to the complete seating of the anterior units. The e.max units were removed and cleaned and made ready for cementation with MultiLink® (Ivoclar Vivadent).
The prepared teeth were pretreated with MultiLink self-etching primer. The e.max units were primed with a silane coupling agent, air-dried, and carefully loaded with the MultiLink final cement. All six units were placed on the preparations at the same time, the excess cement was brushed away, and dental floss was used to clean between the units. The units were then cured for the recommended time with an optimized curing light. Cement flash was removed and the units were cleaned and polished in the mouth.
The occlusion was then checked using thin marking paper. Any obvious interferences were gently polished, and the bite was checked using the Dawson bilateral manipulation technique, using the marking paper to record the contacts. The TekScan unit was then used to detect and eliminate any interferences to full closure and any deviations of the mandible as it closed to MIP.
Upon completion of occlusal adjustment, the patient was able to see the final restorations in a full-face mirror as well as talk and evaluate the changes the new restorations provided.
Conclusions
This was a straightforward mandibular restoration case that lent itself to any of a number of restorative possibilities, including dental implants and conventional porcelain-fused-to-metal (PFM) restorations, pressed-to-zirconia (P2Z) bridges, anterior crowns, or the latest in restorative care—FCZ bridges and e.max veneers and crowns. The natural beauty of e.max, along with its increased resistance to breakage, makes it an ideal restorative material, especially when the bite is being opened. The restorations in this case exhibited nice proportions and natural form and coloration; the anterior units enhanced the patient’s smile.
Over the past 2 years, this author has placed more than 400 single units of FCZ. Initially, they were boxy, poorly colored units that were most suitable for placement in the posterior segments of central nervous system (CNS) bruxxers/clenchers, where broken teeth and/or broken restorations are commonplace. With each new case received, however, better tooth morphology and improved color development have become increasingly evident.
The author has begun to use FCZ in selected anterior restorations. Any deficiencies in form or proportion can be easily and quickly corrected, and the increased resistance to breakage afforded by FCZ crowns makes them a logical choice for the restorative dentist. FCZ restorations are also highly biocompatible. The soft-tissue response around these units is similar to the soft-tissue response at the margins of natural teeth; the tissue stays pink and healthy.
The FCZ posterior bridges in this case were fabricated from monolithic zirconia. The colors for the FCZ bridges were developed from the inside out. No surface stain was used on this case to create the final esthetic appearance of the bridges.
Color development, along with more consistent morphology has improved to the point that clinicians can now use FCZ crowns anywhere in the mouth where the added strength of FCZ will provide long-term reliability. Moreover, these bridges have no esthetic porcelain that could be subject to possible fracture in the future.
The contours of the individual units of the bridge in this case appear natural and flow from anterior to posterior. The occlusal morphology of these units fit snuggly into the occlusal tables of the opposing dentition. Pontic development was also very accurate. The ovate pontics were very smooth in all dimensions and easy to clean using a simple toothbrush and dental floss (Figure 9). The cementation process for FCZ bridges is the same as for cementing a classic PFM restoration; no special cementing techniques or unusual cements are required to finish FCZ restorations.
This case finished very nicely and easily (Figure 10) and will likely provide many years of trouble-free use for this patient.
Acknowledgment
The author would like to thank Mr. Bob Spallino and the FCZ team at Great White Dental Lab in Santa Maria, California, for their help and guidance creating this mandibular restoration. His work with developing color techniques for use with monolithic zirconia and his dedication to developing better morphology for crowns and bridges will help lead to a bright future for monolithic zirconia restorations.
References
1. Jørnung J, Fardal Ø. Perception of patients’ smiles: a comparison of patients’ and dentists’ opinions. J Am Dent Assoc. 2007;138(12):1544-1553.
2. Arnold JH. Giving back a smile…and a life. J Cosmetic Dentistry. 2008;24(2):26-33.
3. McCoy G. Occlusion confusion. Gen Dent. 2013;61(1);71-75.
4. Jacobson N, Hagan MB. The use of porcelain repair technique to improve the plane of occlusion of an existing restoration. Gen Dent. 2011;59(3):207-209.
5. Milnar F. Sequencing three conservative, minimally invasive treatments. Contemporary Esthetics and Restorative Practice. 2007;11(10):24-29.
6. Dawson PE. Functional harmony. Functional Occlusion: From TMJ to Smile Design. St Louis, MO: Mosby; 2007:75-101.
7. Arnold JH. Weatherman gets a new smile. Dental Tribune. 2010;5(15):32-33.
8. Neff A. Doctor, my veneer just broke. How and why does porcelain fracture? J Cosmetic Dentistry. 2010;26(2):90-96.
9. LeSage BP, Dalloca L. Approaches to smile design. J Cosmetic Dentistry. 2012;28(1):126-147.
10. Kahng LS. Patient–dentist–technician communication within the dental team: using a colored treatment plan wax-up. J Esthet Restor Dent. 2006;18(4):185-195.
11. Wells D. Low-risk dentistry using additive-only (“no prep”) porcelain veneers. Compend Contin Educ Dent. 2011;32(5):50-55.
12. Lerner J. A systematic approach to full-mouth reconstruction of the severely worn dentition. Pract Proced Aesthet Dent. 2008;20(2):81-87.
13. Spear F. Candid advice regarding the complexities of occlusion. J Cosmetic Dentistry. 2012;28(3):14-21.
14. Tinschert J, Natt G, Mautsch W, et al. Fracture resistance of lithium disilicate-, alumina-, and zirconia-based three-unit fixed partial dentures: a laboratory study. Int J Prosthodont. 2001;14(3):231-238.
15. Moving to monolithic. Inside Dental Technology. 2011;2(1):70-71.
16. Glidewell Laboratories. Technical Update: Do Not Use Discs To Finish Full-Contour Zirconia. Bruxzir® Blog. https://blog.bruxzir.com/search.aspx?q=do%20not%20use%20discs%20to%20finish&sc=tcon&dt=a&al=. Published December 20, 2010. Accessed February 20, 2013.
17. Bok SD, Lee HH, Bae JY, et al. Factors affect fracture resistance of three-unit zirconia posterior bridge [abstract]. J Dent Res. 2011;90(spec iss A). Abstract 3218.
18. Tauro V. Bench mastery: Step-by-step Zenotec Color ZR—Evolution to revolution. Dental Lab Products. 2011;36(5):28-31.
19. Wolf C, Rüssel C. Sol-gel formation of zirconia: preparation, structure and rheology of sols. Journal of Materials Science. 1992;27(14):3749-3755.
20. McLaren EA, Giordano RA II. Zirconia-based ceramics: Material properties, esthetics, and layering techniques of a new veneering porcelain, VM9. Quintessence Dent Technol. 2005;28:99-111.
21. Wachtman JB, Cannon WR, Matthewson MJ. Mechanical Properties of Ceramics. 2nd ed. Hoboken, NJ: Wiley and Sons; 2009:228.
22. Curran DJ, Fleming TJ, Towler MR, Hampshire S. Mechanical properties of hydroxyapatite-zirconia compacts sintered by two different sintering methods. J Mater Sci Mater Med. 2010;21(4):1109-1120.
23. Long HA. Monolithic zirconia crowns and bridges. Inside Dentistry. 2012;8(1):60-66.
About the Author
Harry A. Long, DMD
Private Practice
Sparta, New Jersey