Combining Monolithic Zirconia Crowns, Digital Impressioning, and Regenerative Cement for a Predictable Restorative Alternative to PFM
Abstract
Advances in indirect esthetic materials in recent years have provided the dental profession higher levels of strength and esthetics than ever before with products like lithium disilicate and zirconium oxide. Providing excellent fit and versatile performance, and because there is no porcelain to delaminate, chip, or fracture, monolithic zirconia crowns have the potential to outperform other layered restorations such as porcelain-fused-to-metal (PFM). This review of monolithic zirconia highlights a clinical case in which all-zirconia restorations were combined with CAD/CAM technology for a successful esthetic restorative outcome.
The quest for stronger, longer-lasting esthetic restorations has been ongoing since the practice of dentistry began. Today, dentists strive to combine ease in preparation and placement, accepted esthetics, and predictable clinical longevity in a manner that increases practice efficiency and economics. In balancing the functional performance of a material with the heightened esthetic standards of today, it is sometimes necessary for dentists to yield slightly in their pursuit of esthetics in order to gain more strength and durability.1 Along with these philosophical choices, there is often conflicting information on how best to use and handle newer materials and techniques—etch or not etch, sandblast or not, light cure or chemical cure, cement or bond?2
Over the past several years, advances in indirect esthetic materials such as lithium disilicate and zirconium oxide have brought the profession higher levels of strength and esthetics than ever before.3,4 Yttria-stabilized tetragonal zirconia polycrystal (Y-Tzp) has become widely used during this time because of its fracture-resistant flexural strength (> 1,000 MPa), nonmetallic color, kind wear patterns on opposing teeth, easy intraoral polishability, tooth preparation characteristics similar to other all-porcelain crowns, and excellent long-term clinical success.5,6
Monolithic Zirconia: Why and When
Choosing the strongest material that meets the minimum esthetic need of the patient simply makes sense. With its excellent fit, versatile performance, and the widespread popularity of newer-generation ceramics like lithium disilicate, when is the best time to use monolithic zirconia?7 Monolithic zirconia posterior crowns (no layering porcelain) have the potential to outlast other layered restorations, such as porcelain-fused-to-metal (PFM), because there is no porcelain to delaminate, chip, or fracture.8,9 Layering porcelain can be added to a zirconium coping to heighten esthetics, but the weak adherence of the stacked or pressed layer has been a common area of clinical failure when the layering material is in function (just as it has with the traditional PFM crown).10-15
Advances in zirconia have made it less opaque and more esthetically appealing than in previous years. This material may not be as esthetic as a high-quality PFM from a skilled ceramist, but improvements in zirconia esthetics (ie, opacity, hue) have allowed all-zirconia restorations to become a clinically acceptable choice in all but the most esthetically demanding situations.16,17 For patients who have parafunctional habits, for whom a questionable occlusal scheme exists, or who display signs of heavy occlusal loading, full-contour zirconia crowns may be indicated, particularly when moderate esthetics is acceptable.18
Concerns with Zirconia
For those who are less familiar with zirconia, there is concern that its hardness may cause excessive wear on opposing teeth. Although it may seem that zirconia’s high fracture strength and surface hardness would cause a greater degree of wear on opposing enamel, studies have shown that the degree of wear on the opposing tooth is actually several times greater from dental porcelain than from polished, unglazed zirconia. This suggests that not only is monolithic zirconia stronger but also kinder to the opposing natural dentition.19 The fine particle size of zirconia makes intraoral polishing easy with routing porcelain polishing kits such as Dialite® (Brasseler USA, www.brasselerusa.com) or CeraMaster® (Shofu, www.shofu.com); therefore, applying a surface gloss after any needed adjustments is simple.
Another concern is its ability to be cut through for endodontic access or complete removal. Cutting through zirconia can be daunting with traditional burs; therefore, practitioners should maintain a small supply of burs designed for bulk zirconia removal (eg, Great White® Z Diamonds, SS White, www.sswhiteburs.com or TIGER™ Zirconia Diamonds, Dental Burs USA, www.bursusa.com). Used on a high-speed handpiece with light pressure and water, these burs greatly simplify the task.
Economic Enhancement with Zirconia
Economy of time equals economy of money. Perhaps often overlooked and seldom discussed is the efficiency and profitability the correct restoration can have on a dental practice. Since monolithic zirconia crowns are milled and no layering porcelain is needed, the time in the laboratory and cost to the dentist can be much less than more labor-intensive restorations. Digital impressions can be e-mailed to the laboratory seconds after the preparation is complete. The laboratory digitally designs, mills, and bakes the restoration in the oven for a few hours, which speeds up the delivery back to the dental office. A fast turnaround time is beneficial for both the laboratory and the patient. Total time in the laboratory is a few hours and there is no reason to delay return to the clinician for weeks as seen with other restorations.
When using traditional putty-type impressions, a model must be made, scanned, and the restoration made as with digital impressions. Less time in a temporary means less microleakage, less sensitivity, and less insertion adjustments from moving adjacent or opposing teeth. There is no reason for the cost of an all-zirconia restoration to come close to that of a PFM or hand-stacked porcelain crown when there is little to no ceramist time involved, no metal cost, and no model work when digital impressions are used.
Reasons to consider monolithic zirconia crowns include: they are more esthetic than metal, they exhibit higher fracture resistance than other tooth-colored materials, they are a conservative tooth preparation similar to gold, and they exhibit sufficient esthetics to decrease the need for layering porcelain. In addition, they can be bonded or cemented, typically have fast turnaround time from the laboratory, and there is less time for the tooth to be adversely influenced by the temporary.
Cementation: Adhesive or Not
Great bonding cannot overcome a poor preparation. A major clinical advantage of zirconia is that it can be cemented or bonded in place depending upon the resistance of the preparation and preference of the dentist. For those cases in which preparation design is retentive in nature, cementation is a viable option because the amount of surface area and the degree of divergence of the prepared walls can provide sufficient micromechanical retention. Resin-reinforced glass-ionomer cements, such as RelyX™ Luting (3M ESPE, www.3MESPE.com) or GC Fuji PLUS™ (GC America Inc., www.gcamerica.com) and newer regenerative cements such as Ceramir® (Doxa AB, www.doxa.se), have been popular choices because of lower reported sensitivity, ease of use, and long-term clinical success on retentive preparations.20,21
When retention is poor, bonding of zirconium-based restorations cannot be done with the same methods of traditional glass-porcelain.22,23 Zirconia is a silica-free, acid-resistant, polycrystalline ceramic, making hydrofluoric acid followed by silane ineffective.24,25 Primers that address the specific needs of nonsilica oxides (eg, zirconia, alumina, and metal) are highly beneficial when traditional retention/resistance form is lacking and, coupled with dual-cure resin cements, give the highest bond strengths.26,27 These primers include Z-PRIME™ PLUS (BISCO, Inc., www.bisco.com), AZ-Primer (Shofu, www.shofu.com), and Metal/Zirconia Primer (Ivoclar Vivadent, www.ivoclarvivadent.com). These primers provide a maximum in adhesion to the restoration, but involve additional steps and cost more than simple cementation. Dual-cure resin cements have been the standard in restoration adhesion, but they, too, involve additional steps and cost more than traditional cementation, in addition to the potential for postoperative complications.
Glass-Ionomer/Calcium-Aluminate Bioactive Cement
Even more efficient would be the use of a cement with adhesive properties that bonds well to enamel and dentin as well as substrates such as zirconia and lithium disilicate without special primers or bonding agents.28 Studies have shown that a newer regenerative material (Ceramir) has performed well in clinical situations after several years with extremely low patient sensitivity and high restoration retention.29 This cement is a calcium-aluminate–based cement with very low microleakage and little acid solubility. In addition, it stimulates hydroxylapatite repair and formation.30 It provides high biocompatibility, rare postoperative sensitivity, slightly alkaline pH, and easy clean-up.31
Cement working time, setting time, film thickness, and mechanical properties are important considerations. With Ceramir, in approximately 2 minutes after placement, the material peels off the tooth in a rubbery consistency that requires very little effort. It has been shown to achieve overall retention at least as good as self-adhesive resin cements with less sensitivity and more bio-acceptability.32 Retention to zirconia and to metals along with its easy clean-up and tissue acceptance have made Ceramir appealing for placing implant crowns when peri-implantitis from cement irritation on soft tissues is a concern.
Clinical Case
Indications for Full Zirconia Crowns
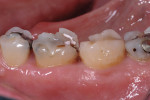
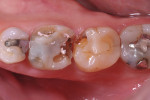
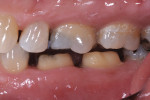
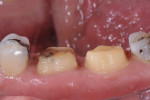
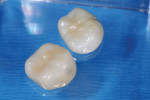
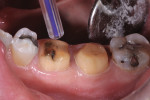
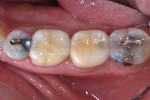
In this case, the patient had a history of nighttime grinding and breaking of molar cusps, including the delamination of two maxillary PFM crowns (Figure 1). Decay, missing tooth structure, and cracking led to the decision to place full crowns instead of conservative inlay/onlay type restorations (Figure 2). The patient had three chipped or partially fractured PFM crowns in other quadrants. The occlusal scheme must always be a factor when choosing restorative materials, preparation, and cementation techniques.
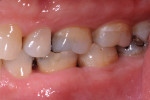
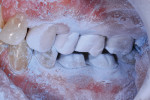
With this patient, the first molars had an edge-to-edge occlusion, and the likelihood of extra stresses on the final restoration encouraged the author to choose restorations and techniques with maximum durability (Figure 3).33 The patient preferred not to use gold if there was a reasonable alternative; therefore, full-contour zirconia restorations were planned for preparation with an insertion appointment the following morning.
Tooth Preparation
Great bonding cannot compensate for poor tooth preparation.34,35 When materials have questionable ability to be bonded, tooth preparation is critical to long-term retention. The preparation of the tooth must fit the characteristics of the restorative material and be designed to aid in the restoration’s resistance to dislodging and fracture. Zirconia bonding may not compensate for preparations designed with walls of excessive taper, a “teepee” preparation, or those with very short axial walls (< 3 mm), which may lead to more restoration debonding.36
Monolithic zirconia crown preparations can be done with preparations similar to gold.37,38 The ideal tooth preparation for monolithic zirconia is 1 mm to 1.5 mm of occlusal clearance, 3 mm to 4 mm axial wall height, and a finish line of 0.5 mm chamfer. Since there is no need for additional reduction to make room for layering porcelain, a more conservative preparation can be done than for PFM crowns or other layered all-porcelain restorations.39 Feather-edge margins are acceptable depending upon laboratory skill but there is more potential for restoration overcontouring. A sound, fundamental preparation done with 4 to 8 degrees of taper and consistent, easily identifiable margins will make design, insertion, and longevity more predictable.
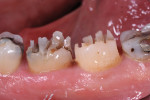
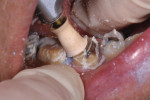
In this case, depth cuts and interproximal slices were made in a single intraoral trip with a 330 bur, which normally has cutting flutes 1.5-mm to 2-mm deep (Figure 4). The axial walls were then reduced with minimal taper to a 0.5-mm to 1-mm chamfer margin using a tapered 0.7-mm-diameter diamond (Figure 5). Preparations were kept supragingival where possible and distinct margins were seen around the entire preparation, making digital impression capture and design much more efficient (Figure 6).
Digital Impression: Accuracy, No Stone, Fast Turnaround
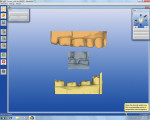
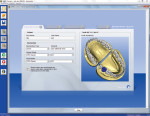
Monolithic zirconia crowns with digital impressions are ideal for office efficiency and restoration success. Laboratories use computer-aided design/computer-aided manufacturing (CAD/CAM) systems to fabricate these restorations and either receive a digital impression from the dentist or digitize a conventional impression sent to them. For this patient, a digital impression of the preparation was captured using CEREC® AC (Sirona, www.cereconline.com) along with the opposing teeth and bite registration (Figure 7). The models were inspected in the software just minutes after final preparation (Figure 8). The CEREC software allowed for accurate virtual articulation of the models without the distortion seen with impression materials, bite trays, and stone (Figure 9).
After identification of the restoration models, the restorations were uploaded to the laboratory via Sirona Connect (www.cerec-connect.com) (Figure 10). The shade and characterization were typed into the digital prescription, which was sent with the case electronically to the laboratory.
A temporary was made from a preoperative quadrant impression and placed onto the tooth with polyvinyl impression material as the luting “cement.” This provided adequate retention for a short period with none of the potential interferences of temporary materials on the final adhesion to the tooth.40 Even if the restoration is returned after 24 hours and a temporary cement is used, the advantage of minimal time in a temporary can be profound with less time for microleakage, temporary fracture, opposing or adjacent tooth movement, and patient discomfort.41
In this case, the restoration was returned to the office the next morning in a jewel case in an envelope. The fit, both marginally and occlusally, from the digital impressions and CAD/CAM fabrication is at least as good as conventional impressions and usually better.42,43 The greatest paradigm shift for the clinician in this digital revolution is to receive a crown without stone models (Figure 11). While the ability to verify the fit of a restoration on the models is almost a tradition in dentistry, the accuracy of digital systems makes this step avoidable. Nevertheless, it is prudent for the dentist to work with the laboratory so that the restorations are made to the comfort level of the clinician with contacts, occlusion, and contours that will be acceptable.
Cementation with a Bioceramic Cement
In this case, the all-zirconia restorations (BruxZir®, Glidewell Laboratories, www.bruxzir.com) were returned in less than 24 hours from a local laboratory. At the definitive restoration appointment less than 24 hours after preparation, the temporaries were removed and the preparations were cleaned with pumice (Figure 12).44 With the accuracy of the digital impression technique and correct design parameters by the laboratory, interproximal or occlusal adjustments are seldom needed. After try-in, the zirconia restorations were cleaned with a unique cleaning material (Ivoclean, Ivoclar Vivadent) for 20 seconds and then rinsed. The teeth were isolated, rinsed, and lightly dried, leaving the surface slightly moist (Figure 13).
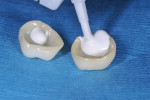
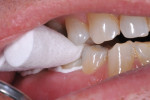
The Ceramir cement requires activation and was mixed in a triturator for 10 seconds to ensure an ideal, “mousselike” consistency with uncompromised physical properties. When activated, the material was placed into the restorations (Figure 14), which were then inserted. The cement has a film thickness of 15 µm and placement is easy with a working time of 1 minute. The patient was instructed to close on cotton roles firmly for approximately 2 minutes (Figure 15). The clean-up was extremely simple because of the material’s rubbery consistency; it easily peeled off the tooth.
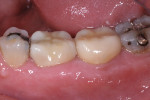
Occlusion was checked with no adjustments needed (Figure 16). Should adjustment of zirconia be needed, it is done with a finishing diamond in a high-speed handpiece, water spray, and light pressure. Polishing is then done with rubber points as with other ceramics. Usually, the fit is exceptional, particularly with digital impressions, and the esthetics are more than acceptable for the majority of posterior restorations. The monolithic zirconia characterization comes from surface staining applied by the laboratory during the firing stage (Figure 17). With little time in a temporary, very little gingival inflammation was observed.
Conclusion
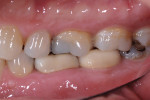
The author has found the ability of this nonlayered zirconia to withstand compromised occlusal forces to be exceptional (Figure 18). The fit is normally excellent and patient reaction is superior to any other restorations placed in this practice. At this point, there is no other procedure and combination of materials that has gained the acceptance of the patients and staff as those described in this article.
Based on research and clinical experience of many cases done in this practice, there is a very high chance of this case lasting for many years with maximum patient satisfaction. Monolithic zirconium, retentive preparations, digital impressions, little time in temporization, and biocompatible cement provides the clinician the highest level of clinical confidence. As developments in bonding, cementation, and materials continue, the future is bright for esthetic dental restorations.
Disclosure
The author declares no financial interest in any of the products mentioned in this article.
Acknowledgment
The author would like to thank Dan Becker, CDT, at Becker Dental Lab, Herculaneum, MO (www.beckerdentallab.com), for his fine work and commitment to current trends in dentistry.
References
1. Larsson C. Zirconium dioxide based dental restorations. Studies on clinical performance and fracture behaviour. Swed Dent J Suppl. 2011;213:9-84.
2. Rosentritt M, Ries S, Kolbeck C, et al. Fracture characteristics of anterior resin-bonded zirconia-fixed partial dentures. Clin Oral Investig. 2009;13(4):453-457.
3. Christensen GJ. The ceramic crown dilemma. J Am Dent Assoc. 2010;141(8):1019-1022.
4. Quinn GD, Studart AR, Hebert C, et al. Fatigue of zirconia and dental bridge geometry: Design implications. Dent Mater. 2010:26(12):1133-1136.
5. Fisher H, Weber M, Marx R. Lifetime prediction of all-ceramic bridges by computational methods. J Dent Res. 2003;82(3):238-242.
6. Quinn JB, Cheng D, Rusin R, et al. Fractographic analysis and material properties of a dental zirconia. ADA Foundation IADR Meeting. 2005.
7. Silva NR, Thompson VP, Valverde GB, et al. Comparative reliability analyses of zirconium oxide and lithium disilicate restorations in vitro and in vivo. J Am Dent Assoc. 2011;142(suppl 2):4S-9S.
8. Burke FJ, Ali A, Palin WM. Zirconia-based all-ceramic crowns and bridges: three case reports. Dent Update. 2006;33(7):401-410.
9. Kugel G, Perry RD, Aboushala A. Restoring anterior maxillary dentition using alumina- and zirconia-based CAD/CAM restorations. Compend Contin Educ Dent. 2003;24(8):569-576.
10. Ishibe M, Raigrodski AJ, Flinn BD, et al. Shear bond strengths of pressed and layered veneering ceramics to high-noble alloy and zirconia cores. J Prosthet Dent. 2011;106(1):29-37.
11. Ozkurt Z, Kazazoglu E, Unal A. In vitro evaluation of shear bond strength of veneering ceramics to zirconia. Dent Mater J. 2010;29(2):138-146.
12. Donovan TE. Factors essential for successful all-ceramic restorations. J Amer Dent Assoc. 2008;139(suppl):14S-18S.
13. White SN, Miklus VG, McLaren EA, et al. Flexural strength of a layered zirconia and porcelain dental all-ceramic system. J Prosth Dent. 2005;94(2):125-131.
14. Donovan TE. Porcelain fused to metal (PFM) alternatives. J Esthet Restor Dent. 2009;21(1):4-6.
15. Christensen RP, Ploeger BJ. A clinical comparison of zirconia, metal and alumina fixed prostheses frameworks veneered with layered or pressed ceramic: a three-year clinical report. J Am Dent Assoc. 2010;141(11):1317-1329.
16. Beuer F, Stimmelmayr M, Gernet W, et al. Prospective study of zirconia-based restorations: 3-year clinical results. Quintessence Int. 2010;41(8):631-637.
17. Guess PC, Zavanelli RA, Silva NR, et al. Monolithic CAD/CAM lithium disilicate versus veneered Y-TZP crowns: comparison of failure modes and reliability after fatigue. Int J Prosthodont. 2010;23(5):434-442.
18. Wall JG, Cipra DL. Alternative crown systems. Is the metal-ceramic crown always the restoration of choice? Dent Clin North Am. 1992;36(3):765-782.
19. Jung YS, Lee JW, Choi YJ, et al. A study on the in-vitro wear of the natural tooth structure by opposing zirconia or dental porcelain. J Adv Prosthodont. 2010;2(3):111-115.
20. Vargas MA, Bergeron C, Diaz-Arnold A. Cementing all-ceramic restorations: recommendations for success. J Am Dent Assoc. 2011;142(suppl 2):20s-24s.
21. Thompson JY, Stoner BR, Piascik JR, et al. Adhesion/cementation to zirconia and other non-silicate ceramics: where are we now? Dent Mater. 2011;27(1):71-82.
22. Denry I, Kelly JR. State of the art of zirconia for dental applications. Dent Mater. 2008;24(3):299-307.
23. Conrad HJ, Seong WF, Pesun IJ. Current ceramic material and systems with clinical recommendations: a systematic review. J Prosthet Dent. 2007;98(5):389-404.
24. Blatz MB, Sadan A, Kern M. Resin-ceramic bonding: a review of the literature. J Prosthet Dent. 2003;89(3):268-274.
25. Dérand P, Dérand T. Bond strength of luting cements to zirconium oxide ceramics. Int J Prosthodont. 2000;13(2):131-135.
26. Griffin J, Suh B, Chen L, Brown D. Surface treatments for zirconia bonding: A clinical perspective. Canadian J of Restorative Dentistry and Prosthodontics. Winter 2010:23-29.
27. Tanaka R, Fujishima A, Shibata Y, et al. Cooperation of phosphate monomer and silica modification on zirconia. J Dent Res. 2008;87(7):666-670.
28. Jefferies SR, Pameijer CH, Appleby DC, et al. Prospective observation of a new bioactive luting cement: 2-year follow-up. J Prosthodont. 2011;21(1):33-41.
29. Jefferies SR, Appleby D, Boston D, et al. Clinical performance of a bioactive dental luting cement–a prospective clinical pilot study. J Clin Dent. 2009;20(7):231-237.
30. Loof J, Svahn F, Jarmar T, et al. A comparative study of the bioactivity of three materials for dental applications. Dent Mater. 2008;24(5):653-659.
31. Pameijer CH, Jefferies S, Lööf J, Hermansson L. Microleakage evaluation of XeraCem in cemented crowns. J Dent Res. 2008;87(B):3098.
32. Jefferies SR, Lööf J, Pameijer CH, et al. Physical properties of XeraCem. J Dent Res. 2008;87(B):3100.
33. Bachhav VC, Aras MA. Zirconia-based fixed partial dentures: a clinical review. Quintessence Int. 2011;42(2):173-182.
34. Beuer F, Aggstaller H, Richter J, et al. Influence of preparation angle on marginal and internal fit of CAD/CAM-fabricated zirconia crown copings. Quintessence Int. 2009;40(3):243-250.
35. Abou-Madina MM, Özcan M, Abdelaziz KM. Influence of resin cements and aging on the fracture resistance of IPS e.max press posterior crowns. Int J Prosthodont. 2012;25(1):33-35.
36. Baltzer A. All-ceramic single-tooth restorations: choosing the material to match the preparation--preparing the tooth to match the material. Int J Comput Dent. 2008;11(3-4):241-256.
37. BruxZir preparation guide. BruxZir Web site. www.bruxzir.com/science-bruxzir-zirconia-dental-crown. Accessed January 25, 2013.
38. BruxZir technical notes. Glidewell Laboratories Web site. www.glidewelldental.com/bruxzir-zirconia-crowns/features. Accessed January 25, 2013.
39. Tooth Preparation Guidelines for Zirconia Crowns. The Dental Advisor. July 2009;(3).
40. Ribeiro JC, Coelho PG, Janal MN, et al. The influence of temporary cements on dental adhesive systems for luting cementation. J Dent. 2011;39(3):255-262.
41. Mayer T, Eickholz P. Microleakage of temporary restorations after thermocycling and mechanical loading. J Endod. 1997;23(5):320-322.
42. Scotti R, Cardelli P, Baldissara P, Monaco C. Clinical fitting of CAD/CAM zirconia single crowns generated from digital intraoral impressions based on active wavefront sampling. J Dent. 2011 Oct 17. [Epub ahead of print]
43. Ender A, Mehl A. Full arch scans: conventional versus digital impressions—an in-vitro study. Int J Comput Dent. 2011;14(1):11-21.
44. Dillenburg AL, Soares CG, Paranhos MP, et al. Microtensile bond strength of prehybridized dentin: storage time and surface treatment effects. J Adhes Dent. 2009;11(3):231-237.
About the Author
Jack D. Griffin, Jr., DMD
Private Practice
Eureka, Missouri