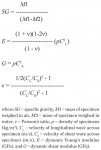Sheila P. Passos, DDS, MSc, PhD; Anderson P. Freitas, DDS, MSc, PhD; Sami Jumaily, DDS; Maria Jacinta M.C. Santos, DDS, MSc, PhD; Amin S. Rizkalla, PhD; and Gildo C. Santos, Jr., DDS, MSc, PhD
Abstract:
OBJECTIVE: This study aimed to evaluate and compare the mechanical properties of five commercial core materials using fracture toughness (FT), Knoop hardness number (KHN), diametral tensile strength (DTS), and dynamic elastic moduli (DEM).
METHODS: Composite material specimens were produced (Rock Core, CosmeCore, ParaCore, MultiCore Flow, and Filtek Supreme Plus). The FT test (n = 15) was performed using notchless triangular prism (NTP) specimens. FT was determined using an Instron testing machine. KHN (n = 3) was evaluated using three indentations applied on each specimen. DTS test (n = 15) was measured using an Instron testing machine. The density of the specimens (n = 3) was determined by water displacement method. Dynamic Young’s, shear moduli, and Poisson’s ratio (n = 3) were measured by an ultrasonic method. Statistical analysis was conducted using ANOVA and a Tukey B rank order test (P = 0.05).
RESULTS: Rock Core presented the lowest FT values. Filtek Supreme Plus and CosmeCore exhibited significantly higher KHN values than the rest of the materials. CosmeCore had the highest DTS value, which was statistically significant only compared to Rock Core. For DEM, Filtek Supreme Plus exhibited significantly higher Young’s and shear moduli than the rest of the materials (P < 0.05).
CONCLUSIONS: Results demonstrated significant differences in the FT, KHN, and DTS values of the core build-up materials tested. According to the elastic behavior of the core composite materials, Rock Core had the lowest Young’s values.
Teeth receiving endodontic treatment are usually severely compromised by decay, previous restorations, or excessive wear; as a result, a significant loss of coronal tooth structure is often observed.1 Core build-up materials can be used to repair the damaged tooth structure prior to crown preparation and stabilize weakened parts of the tooth; as such, they are a key part of the preparation for an indirect restoration consisting of restorative material. Although the long-term clinical success of an indirect restoration is mostly dependent on the amount of remaining tooth structure (which is responsible for the adequate ferrule effect), the core build-up material plays an important role as well. An ideal core build-up material must present excellent mechanical properties in order to resist the stresses that may be produced during function, providing equitable stress distributions of forces and reducing the probability of tensile and compressive failures.
Amalgam, composite resin, and glass-ionomer materials have typically been used as core build-up materials. While these materials were not specifically developed for this purpose, they have found application in core build-up procedures as a consequence of their properties. More recent formulations have incorporated different combinations of materials,2 therefore flow composite core build-up materials have been introduced.3 There are, however, concerns that the mechanical properties of these materials, which incorporate less filler content, could be decreased to allow flowability4 since fillers have been reported to improve the mechanical properties of bis-GMA-based dental resin.5,6 This suggests that flowable materials with less filler content might be mechanically weaker than their more filled counterparts.7
The specific purpose of this study was to evaluate the mechanical properties of five different commercial resin composite core materials using fracture toughness (FT), Knoop hardness number (KHN), and diametral tensile strength (DTS), to experimentally measure Young’s moduli, and to calculate specific gravity, Poisson’s ratio, and shear modulus. The null hypotheses tested were: 1) that there were no differences among the FT, KHN, and DTS of the studied materials; and 2) that there were no differences among the elastic moduli of the materials.
Materials and Methods
Mechanical properties of five resin composite core materials were evaluated in this study—one developed for use as a direct restorative material (control group) and four developed specifically to be used as core build-up materials. Composite core materials, composition, batch numbers, and manufacturers of the products are presented in Table 1.
Fracture Toughness
Fracture toughness is an intrinsic property of a material and is a measure of the energy required to propagate a crack from an existing defect.
For this study, notchless triangular prism (NTP) specimens (6 mm x 6 mm x 6 mm x 12 mm) were made from each core material (n = 15). Each side of the sample was light-cured for 30 seconds, then all samples were polymerized in a visible light-polymerizing (VLP) chamber for 5 minutes. The samples were stored in distilled water at 37ºC for 7 days prior to testing. NTP fracture toughness was determined in a universal testing machine (Instron Model 3345, Instron Corp., www.instron.com).
Each sample was scorched at the location of tensile forces in order to create a defect. Force was applied until failure of the specimen occurred. The relationships that were used to calculate the FT (KIC) were proposed by Barker8 and adopted by ASTM standard E1304. The equation is as follows:
Pmax
KIC = -------------- Y*min
D √W
where Pmax = the maximum load at fracture, D = the specimen diameter, W = the specimen length, and Y*min = the minimum of the dimensionless stress intensity factor coefficient (= 28).9
Knoop Hardness
The mechanical properties of resin materials depend on the polymer structure and degree of monomer conversion, which are strictly related to effective polymerization. Knoop hardness assessment helps to predict the clinical performance of resin restorative materials and is related to a material’s stiffness.
The specimens of each core material were obtained using the same method of producing the NTP specimens and sliced in 2 mm (6 mm x 6 mm x 6 mm x 2 mm) (n = 3). The specimens’ surfaces were polished under water cooling. The samples were then stored in distilled water at 37ºC for 7 days prior to testing. A Knoop hardness test (Digital Hardness Testing Machine, Buehler, www.buehler.com) of each specimen was performed. Three indentations were obtained for each specimen.
Diametral Tensile Strength
The determination of tensile strength by the direct application of tensile load is suspect given that external stresses are generated by gripping the samples during testing, with the effect that the results may incorporate unacceptable errors. Brittle materials such as glass-ionomer cements and amalgam are liable to fracture at the gripped ends of the specimen. One way to overcome this problem is to use samples of dumb-bell shape and a diametral compression test.
Eighty disc specimens (6 mm x 3 mm) were made from the core materials (n = 15), according to American Dental Association (ADA) specification No. 27,10 and stored in distilled water at 37ºC for 7 days prior to testing. The DTS test was conducted in a universal testing machine. DTS values were calculated according to the following formula11,12:
2P
DTS σx = ---------
πdt
where P = load, d = diameter, and t = thickness.
Dynamic Elastic Moduli
Elastic modulus describes the relative stiffness of the material within the elastic range. Natural hard tissues have a range of intrinsic stiffness or modulus values, and the addition of restorative materials of different moduli can affect the overall stiffness of the restored tooth and the interfacial stresses that are generated. The clinical outcome will be related to the matching of moduli values, and if the modulus mismatch is too great, interfacial stress may result from either thermal, mechanical, or shrinkage strain in the material. Therefore, core build-up material should have high elastic modulus similar to that of tooth structure (dentin) to withstand the forces of mastication and polymerization shrinkage stresses. Consequently, the determination of elastic modulus is valuable in the evaluation of core build-up restorative materials.
The density of the specimens of all core material (n = 3) was determined by water displacement method. The specific gravity,13 dynamic Young’s, shear moduli, and Poisson’s ratio (n = 3) were determined by an ultrasonic method.14 The elastic moduli values were calculated for each specimen using the following formulas:
M1
SG = ----------------
(M1-M2)
(1 +ν)(1-2ν)
E = -------------------- (pC2L)
(1 -ν)
G = pC2S
1/2(CL/CS)2 - 1
ν = --------------------------
(CL/CS)2 - 1
where SG = specific gravity, M1 = mass of specimen weighed in air, M2 = mass of specimen weighed in water, ν = Poisson’s ratio, p = density of specimens (kg/m3), CL = velocity of longitudinal wave across specimen (m/s), CS = velocity of shear wave across specimen (m/s), E = dynamic Young’s modulus (GPa), and G = dynamic shear modulus (GPa).
Statistical Method
The results were analyzed and compared using one-way ANOVA and Tukey B rank order test at the significance level of 0.05.
Results
Fracture Toughness
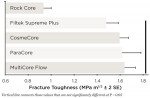
The fracture toughness is presented in Figure 1. Fracture toughness of the core materials ranged from 0.89 to 1.69 MPa m1/2.
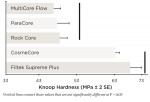
Knoop Hardness
The KHN of Filtek™ Supreme Plus (3M ESPE, www.3MESPE.com) and CosmeCore™ (Cosmedent, Inc., www.cosmedent.com) showed similar values, 69.87 (2.73) and 63.34 (1.18), respectively, and significantly higher than the other groups. KHN values of MultiCore® Flow (Ivoclar Vivadent Inc., www.ivoclarvivadent.com), ParaCore® (Coltène Whaledent Group, www.coltene.com), and Rock Core™ (Danville Materials, www.danvillematerials.com) were 46.74 (2.15), 47.25 (3.18), and 47.56 (2.18), respectively (Figure 2).
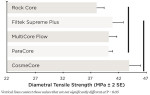
Diametral Tensile Strength
The highest values for DTS were observed for CosmeCore, 44.00 (1.22) MPa; Filtek Supreme Plus, 40.50 (1.98) MPa; ParaCore, 41.07 (0.68) MPa; and MultiCore Flow, 41.07 (1.09) MPa. Rock Core exhibited a significantly lower value (38.62 ± 1.22 MPa) compared to CosmeCore (Figure 3).
Dynamic Elastic Moduli
Specific gravity, Poisson’s ratio, shear moduli, and dynamic Young’s are presented in Figure 4, Figure 5, Figure 6, and Figure 7, respectively. The specific gravity, Poisson’s ratio, shear moduli, and dynamic Young’s ranged from 1.84 to 2.04 GPa, 0.204 to 0.309 GPa, 5.59 to 9.38 GPa, and 14.44 to 22.64 GPa, respectively.
Discussion
Several studies have been undertaken to measure mechanical properties of direct core build-up materials that included: fracture toughness,6-8,15 diametral tensile strength,11,12 elastic modulus,13,14 and shear bond strength.1 Mechanical properties are considered to be a critical indicator of success for restorative materials, because materials are expected to resist masticatory and parafunctional forces.
The mechanical properties of a core material and its clinical performance is affected by many variables. This study evaluated some of these properties, including fracture toughness (FT), Knoop hardness number (KHN), diametral tensile strength (DTS), and dynamic elastic modulus (DEM), in five resin composite materials. The first null hypothesis was not validated since there were differences among the FT, KHN, and DTS of the studied materials. The second hypothesis was partially accepted, in that no difference was observed for only the specific gravity and Poisson’s ratio among the composite materials, and difference was observed for the dynamic Young’s and shear moduli.
Regarding the FT, the notchless triangular prism (NTP) specimen fracture toughness test was used in this study. This technique was introduced by Ruse et al15 and then developed by other researchers.8,14,16 The FT results found in this study are in agreement with the study by Dong and Ruse,17 which used the same method and in which FT of different nanofilled resin composites ranged from 1.08 to 1.47 MPa m1/2; the FT value was 1.08 MPa m1/2 for Filtek Supreme Plus.18 In addition, Watanabe et al6 evaluated FT of six resin composites, and FT values ranged from 0.55 MPa m1/2 to 1.36 MPa m1/2; Filtek Supreme Plus exhibited 1.30 MPa m1/2. Both Filtek Supreme Plus FT values were lower than in the present study (1.53 MPa m1/2) in which Filtek Supreme Plus was the control group (a nanofilled composite). This difference could be related to the differences in the specimen preparation. The specimen configuration and the path of crack propagation may explain the 1.53 MPa m1/2 value obtained for the tested specimens.
Previous studies reported that the higher the filler loading, the higher the FT.6,19,20 The threshold of filler loading for the highest FT values in resin composites was 55% by volume.20 In the present study, all core build-up material evaluated had less than this level. This percent of filler loading is more important than weight percent. MultiCore Flow presented FT values significantly higher than Rock Core FT values, which may be due to other variables once their filler percentage volumes are at a similar level. One of the variable effects on FT values besides filler content is stress transfer from resin matrices to filler particles.6
The results of this study demonstrated that the KHN values varied among the tested resin composites. Previous studies have confirmed that KHN values reflect the degree of polymerization of resin composite,21,22 and many variables can influence the microhardness of resin composite, such as filler size, filler type, filler load, or resin matrix type.5,20,23 The resin materials, filler type, and size of each material are shown in Table 1. Filtek Supreme Plus has nanofillers in its composition and was developed for direct restorative procedures, which explains the highest KHN (40.34 +/- 3.12), although not significantly different from CosmeCore. This finding is in accordance with those of Fujita et al.24 In addition, the core build-up composites developed for this specific purpose presented different KHN,25,26 with CosmeCore presenting the highest KHN among its category.
All the materials investigated reached the minimum DTS value of 34 MPa, required for Type II resin composite materials as specified by ADA specifications.10 The authors’ results are in agreement with another study,27 which evaluated the DTS of the composite materials (which ranged from 35 MPa to 49 MPa).
Elastic moduli of resin composite materials have been measured by many different methods, such as static and dynamic experiments. Some mathematical models have been used for the prediction of the elastic moduli as well. In some dynamic experiments, an ultrasound (resonance) is commonly applied to the materials. In addition, Poisson’s ratio is computed from the velocity or natural frequency of the transverse and longitudinal waves generated.28 Many variables affect the elastic moduli values, including the efficiency of polymerization, the test method, and the strain rate, among others.29
The Poisson’s ratio is a parameter that is affected by the testing procedure, and different values can be obtained with a change of the strain rate. However, the values obtained from the materials in this study are in a reasonable range that was expected for composites and calculated by other researchers.30,31 According to the present results, no difference was observed among the different composite core materials tested. The shear moduli and Young’s moduli of resin composites as found in the present study presented a range similar to a previous study.32 From the findings of this investigation, Filtek Supreme Plus exhibited the highest shear moduli and Young’s moduli; Rock Core had the lowest Young’s moduli. These observations are in agreement with previous studies.33,34
The present study had some limitations, including that it was an in-vitro study and the influence of fatigue in the oral environment was not evaluated. Studies that simulate clinical conditions are necessary for better determination of the properties of the different dental composite materials.
Conclusions
The findings of this study demonstrated that the FT, KHN, and DTS of the core build-up materials tested varied significantly. Rock Core had the lowest FT and Young’s moduli among the materials tested while CosmeCore had the highest KHN values. CosmeCore is expected to present a higher degree of conversion during its dual-cure process (light and chemical cure) when compared to the other dual-cure materials.
Regarding the elastic behavior of the core composite materials, Rock Core had the lowest Young’s values. There was no difference in Poisson’s ratio and specific gravity among the core materials.
Based on these results, respecting the limitations of this study and taking into consideration the convenience of the use of automix systems and dual-cure properties, the authors suggest CosmeCore and MultiCore Flow as core build-up materials of choice.
Disclosure
The authors received a research grant from Clinician's Choice Dental Products, Inc. to complete this study.
References
1. Sadek FT, Monticelli F, Goracci C, et al. Bond strength performance of different resin composites used as core materials around fiber posts. Dent Mater. 2007;23(1):95-99.
2. Bonilla ED, Mardirossian G, Caputo AA. Fracture toughness of various core build-up materials. J Prosthodont. 2000;9(1):14-18.
3. Oberholzer TG, Pameijer CH, Grobler SR, Rossouw RJ. Volumetric polymerisation shrinkage of different dental restorative materials. SADJ. 2004;59(1):8-12.
4. Bayne SC, Thompson JY, Swift EJ Jr, et al. A characterization of first-generation flowable composites. J Am Dent Assoc. 1998;129(5):567-577.
5. Zandinejad AA, Atai M, Pahlevan A. The effect of ceramic and porous fillers on the mechanical properties of experimental dental composites. Dent Mater. 2006;22(4):382-387.
6. Watanabe H, Khera SC, Vargas MA, Qian F. Fracture toughness comparison of six resin composites. Dent Mater. 2008;24(3):418-425.
7. Gu S, Rasimick BJ, Deutsch AS, Musikant BL. In vitro evaluation of five core materials. J Prosthodont. 2007;16(1):25-30.
8. Barker LM. Short bar specimen for KIc measurements. In: Freiman SW, ed. Fracture Mechanics Applied to Brittle Materials. ASTM STP 678. American Society for Testing and Materials; 1979;73-82.
9. Bubsey RT, Munz D, Pierce WS, Shannon JL. Compliance calibration of the short rod chevron-notch specimen for fracture toughness testing of brittle materials. Int J Fracture. 1982;18(2):125-133.
10. American Dental Association Certification Programs of the Council on Dental Materials, Instruments and Equipment. American National Standards Institution/American Dental Association Specification 27 for direct filling resins. Chicago; 1977.
11. Phillips RW. Science of Dental Materials. 9th ed. Philadelphia, PA: Saunders; 1991:404.
12. Canay S, Hersek N, Ciftçi Y, Akça K. Comparison of diametral tensile strength of microwave and oven-dried investment materials. J Prosthet Dent. 1999;82(3):286-290.
13. Puckett AD, Smith R. Method to measure the polymerization shrinkage of light-cured composites. J Prosthet Dent. 1992;68(1):56-58.
14. Babikov OI. Ultrasonics and Its Industrial Applications. New York, NY: Russian Publishers, Consultants Bureau; 1960:123[chap 5].
15. Ruse ND, Troczynski T, MacEntee MI, Feduik D. Novel fracture toughness test using a notchless traingular prism (NTP) specimen. J Biomed Mater Res. 1996;31(4):457-463.
16. Barker LM. A simplified method for measuring plane strain fracture toughness. Eng Fracture Mech. 1977;9(2):361-369.
17. Dong XD, Ruse ND. Fatigue crack propagation path across the dentinoenamel junction complex in human teeth. J Biomed Mater Res A. 2003;66(1):103-109.
18. Cho SD, Bulpakdi P, Matis BA, Platt JA. Effect of bleaching on fracture toughness of resin composites. Oper Dent. 2009;34(6):703-708.
19. Kim KH, Kim YB, Okuno O. Microfracture mechanisms of composite resins containing prepolymerized particle fillers. Dent Mater J. 2000;19(1):22-33.
20. Kim KH, Ong JL, Okuno O. The effect of filler loading and morphology on the mechanical properties of contemporary composites. J Prosthet Dent. 2002;87(6):642-649.
21. Ferracane JL. Correlation between hardness and degree of conversion during the setting reaction of unfilled dental restorative resins. Dent Mater. 1985;1(1):11-14.
22. Rueggeberg FA, Ergle JW, Mettenburg DJ. Polymerization depths of contemporary light-curing units using microhardness. J Esthet Dent. 2000;12(6):340-349.
23. Yamaga T, Sato Y, Akagawa Y, et al. Hardness and fracture toughness of four commercial visible light-cured composite resin veneering materials. J Oral Rehabil. 1995;22(12):857-863.
24. Fujita K, Ikemi T, Nishiyama N. Effects of particle size of silica filler on polymerization conversion in a light-curing resin composite. Dent Mater. 2011;27(11):1079-1085.
25. Schmage P, Nergiz I, Sito F, et al. Wear and hardness of different core build-up materials. J Biomed Mater Res B Appl Biomater. 2009;91(1):71-79.
26. Polydorou O, Mönting JS, Hellwig E, Auschill TM. Effect of in-office tooth bleaching on the microhardness of six dental esthetic restorative materials. Dent Mater. 2007;23(2):153-158.
27. Lu H, Lee YK, Oguri M, Powers JM. Properties of a dental resin composite with a spherical inorganic filler. Oper Dent. 2006;31(6):734-740.
28. Chung SM, Yap AU, Koh WK, et al. Measurement of Poisson’s ratio of dental composite restorative materials. Biomaterials. 2004;25(13):2455-2460.
29. Dauvillier BS, Aarnts MP, Feilzer AJ. Modeling of the viscoelastic behavior of dental light-activated resin composites during curing. Dent Mater. 2003;19(4):277-285.
30. Hübsch PF, Middleton J, Knox J. A finite element analysis of the stress at the restoration-tooth interface, comparing inlays and bulk fillings. Biomaterials. 2000;21(10):1015-1019.
31. Borkowski K, Kotousov A, Kahler B. Effect of material properties of composite restoration on the strength of the restoration-dentine interface due to polymerization shrinkage, thermal and occlusal loading. Med Eng Phys. 2007;29(6):671-676.
32. Papadogiannis DY, Lakes RS, Papadogiannis Y, et al. The effect of temperature on the viscoelastic properties of nano-hybrid composites. Dent Mater. 2008;24(2):257-266.
33. Ikejima I, Nomoto R, McCabe JF. Shear punch strength and flexural strength of model composites with varying filler volume fraction, particle size and silanation. Dent Mater. 2003;19(3):206-211.
34. Braem M, Lambrechts P, Van Doren V, Vanherle G. The impact of composite structure on its elastic response. J Dent Res. 1986;65(5):648-653.
About the Authors
Sheila P. Passos, DDS, MSc, PhD
Research Assistant
Department of Dentistry
University of Alberta
Edmonton, Alberta, Canada
Anderson P. Freitas, DDS, MSc, PhD
Associate Professor
Department of Restorative Dentistry
Federal University of Bahia
Salvador, Bahia, Brazil
Sami Jumaily, DDS
Private Practice
London, Ontario, Canada
Maria Jacinta M.C. Santos, DDS, MSc, PhD
Assistant Professor
Department of Restorative Dentistry
Schulich School of Medicine and Dentistry
University of Western Ontario
London, Ontario, Canada
Amin S. Rizkalla, PhD
Associate Professor
Department of Biomaterials Science
Schulich School of Medicine and Dentistry
University of Western Ontario
London, Ontario, Canada
Gildo C. Santos, Jr., DDS, MSc, PhD
Associate Professor
Department of Restorative Dentistry
Schulich School of Medicine and Dentistry
University of Western Ontario
London, Ontario, Canada