Partial Rehabilitation of the Posterior Edentulous Maxilla Using Axial and Tilted Implants in Immediate Function to Avoid Bone Grafting
Paulo Maló, DDS, PhD; Miguel de Araújo Nobre, RDH
ABSTRACT:There is a need to create rehabilitation solutions for partial edentulism in the posterior maxilla, thereby reducing the need for grafting in these areas. The purpose of this study was to report the results of partial edentulism rehabilitation in the posterior maxilla with a three- to four-unit bridge supported by two implants: anterior implant placed in axial position and posterior implant tilted distally. A theoretical analysis of the concept including a biomechanical discussion is also provided.
MATERIALS AND METHODS:The clinical study included 35 patients (21 women, 14 men) with an age range of 37 to 80 years (mean = 55.5 years), rehabilitated with an implant-supported partial bridge, followed between 4 months and 8 years, with a mean follow-up time of 53 months.
ASSESSMENT DATA:The success criteria included clinical parameters (ie, implant fulfilled its purported function as support for reconstruction; was stable when individually and manually tested; had absence of infection; demonstrated a good esthetic outcome of the rehabilitation; allowed fabrication of the implant-supported fixed prosthesis, which provided patient comfort and hygiene) and radiographic parameters (ie, implant probability of long-term stability, as judged by annual bone loss). The implant survival estimate was computed using the Kaplan-Meier product limit estimator. Data were analyzed with descriptive and inferential analyses.
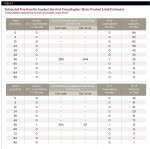
RESULTS: The survival rates were 97.1% and 98.8% at 8 years (Kaplan-Meier), using the patient and implant as units of analysis, respectively. The overall average marginal bone resorption was 1.05 mm (SD = 0.65 mm) at 1-year follow-up, and 1.47 mm (SD = 0.37 mm) at 5-year follow-up, with no significant differences between axial and tilted implants in the 1-year (P = 0.107) and 5-year (P = 0.211) evaluations.
DISCUSSION OF RESULTS:The results indicate that within the limitations of this preliminary study the present protocol is valid for the rehabilitation of partial edentulism in the posterior maxilla. The clinical results confirmed the theoretical analysis on biomechanics and load distribution, with high survival and success rates in the long-term, low implant marginal bone resorption, and low frequencies of complications.
The rehabilitation of posterior areas in the maxilla is challenging. With regard to partial edentulism in the posterior maxilla, the challenge is that the bone in these areas is usually of lower density and inadequate quantity due to the presence of the maxillary sinus. One treatment option is bone onlay grafting and/or sinus lift procedure. This technique, however, has several disadvantages such as poor bone density of the donor site in elderly patients, morbidity, and complications related to the sinus lift procedure such as sinusitis, fistula, osteomielitis, and implant or transplant loss.1 Also, the procedure has lower success rates when compared to implants placed in residual bone,2 and, furthermore, it does not allow the immediate placement of crowns due to the lack of primary anchorage of the implants.
Another treatment alternative is the placement of implants with a reduced size. Despite the results achieved with short implants placed in dense bone,3 their usage is linked to lower success rates4,5that, combined with the poor bone quality and exposure to high occlusal loads, may result in compromised situations from a biomechanical standpoint.6-8 The biomechanical aspects of a partial rehabilitation should be considered. Bending moments lead to higher stress levels in implant components,9,10 and excessive bending moments may lead to failures.11,12 This is especially true for partial rehabilitations, which do not benefit from cross-arch stabilization as complete edentulous rehabilitations do, and, therefore, are more susceptible to bending loads.13 The failures can be either repeated loosening of screw components,8,14 implant fractures,15-17 and/or bone loss as demonstrated in the animal model,18,19 in finite element analysis models20 and in vivo.8,21-25
Load factors such as mechanical strength, implant load, leverages, occlusion, and implant alignment were analyzed in this review of the literature, taking into consideration their potential effect on the bending of the implant and the development of this concept for partial edentulous rehabilitation.
Mechanical strength: The exposure of the implant section below the engagement of the abutment screw to bending load is one of the conditions that can cause implant fracture.11 An implant exposed below this area (two to three threads in the apical direction due to bone loss) may be prone to increased probability of implant fracture.11 Also, a misfit at the implant/abutment or abutment/prosthesis interfaces can make the joint unstable and contribute to an increasing probability of fracture.26
Implant load: Theoretical models and experimental data are available for understanding implant loading as an aid to case planning.27 Parafunctional habits can contribute to bending overload.8 Bending moments occur as a result of functional and parafunctional movement patterns of the mandible,11,28 especially in posterior areas.
Leverages: The deleterious effects of leverages on the biomechanical outcome have been demonstrated.28 Cantilevers are one of the possible leverages. This means that there is a lever arm between the position of force contact and the position of support, which in this case can magnify by a considerable degree the vertical and lateral forces generated at the occlusal contact,11 increasing loads distributed to implants and potentially causing biomechanical complications.8,29 Cantilever size has been related to marginal bone loss around dental implants, as well as mechanical failures of the prosthetic components. Schackelton30 observed that prostheses with less than 15-mm cantilever size survived significantly better than prostheses with more than 15-mm cantilever size.
Duyck et al31 performed a study dealing with the biomechanical aspects of cantilevers, and concluded that the distal implant needs to support compression and bending moments two times more in average when compared to the applied load in normal conditions, due to the cantilever effect. These results were supported by several studies where higher loads were observed in distal implants and bone when the cantilever was loaded.32-38
Occlusion: Occlusion is another factor that must be taken into consideration in a partial rehabilitation, as implants placed in posterior areas are subjected to high occlusal loads.10 Furthermore, overload depends ultimately on the number and location of occlusal contacts, which to a great extent are under the clinician's control.12
Implant alignment: The straighter the alignment, the greater the potential for bending of the implants.39 In these cases, the bending of the implants occurs as a result of lateral occlusal-force components.The use of tilted implants for maxillary rehabilitation is documented in the literature: for complete rehabilitation of the edentulous maxilla, reported success rates are between 93% and 98% after 5 years using a two-stage surgical approach40,41; and for the use of four implants (two anterior implants placed in the axial position and two posterior implants tilted distally) in immediate function, survival rate after 1 year is 97.6%.42 In partial rehabilitations, a survival rate of 100% after 1 year43 and a cumulative success rate of 95.2% after 5 years44 were reported using a two-stage surgical approach; a cumulativesurvival rate of 96.7% after 1 year of follow-up was reported, which added immediate/early function to the protocol.45
Applying the present concept, the partial rehabilitation of the posterior maxilla consisted of a three- to four-unit bridge supported by two implants (the anterior implant in the axial position; the posterior implant tilted distally). The theoretical rationale for this was twofold: 1) biomechanically, supporting both ends of the partial bridge (or at least minimizing the posterior cantilever) reduces the bending moment by up to half when compared with a prosthesis supported by two implants and with a cantilever tooth;10 and 2) the insertion of axial and tilted implants enables use of as much dense bone as possible and decreases the cantilever to a minimum.46
Regarding the technique for placement of tilted implants when rehabilitating patients with partial40 and total40-42 edentulism in the maxilla, the posterior implant placement should be close to and parallel to the anterior wall of the maxillary sinus, angulated 30º to 45º. The tilting of the posterior implants allows the following advantages:
- Longer implants can be placed, enhancing the area of contact between bone and implant, and thus enhancing the primary anchorage.40,42
- The implant support is moved posteriorly.40,42
- The implant follows a dense bone structure (the anterior wall of the maxillary sinus), enhancing the primary stability.40-42
- The desired position of the implants is determined from the prosthetic point of view.41
- A greater distance between implants is achieved, allowing the elimination or decrease of cantilevers in the prosthesis, resulting in better load distribution.46
- A favorable inter-implant distance is gained.42
- Implants can be placed in residual bone, allowing the more complex techniques of bone graft and/or sinus lift to be avoided.42,44
Based on this theoretical analysis, the aim of this study was to report the success of the partial rehabilitation of the posterior maxilla using two implants (one anterior implant placed in the axial position; one posterior implant tilted distally) in immediate function. The research hypothesis was that immediate placement and function using one anterior axial implant and one posterior implant tilted distally for the partial rehabilitation of the posterior maxilla is possible and offers the same level of success as partial rehabilitations using immediate function implants in other areas.47
Materials and Methods
This study was performed at a private dental office (Maló Clinic, Lisbon, Portugal) between January 2002 and April 2010. The study included 35 consecutive patients (21 women and 14 men), with an age range of 37 to 80 years (mean = 55.5 years). The patients were followed between 4 months and 8 years, with a mean follow-up time of 53 months. The patients were included in the study provided they were in need of implant-supported restorations in the posterior maxilla, had good general health, had atrophied jawbone, and were possible candidates for placement of a minimum of two implants, using tilting in distal sites. Patients presenting with the following criteria were excluded: immunodeficiency pathology, stressful social or professional situation, or emotional instability (assessed at the screening appointment through interview). No systemic conditions judged to influence the treatment outcome such as a history of chemotherapy or radiotherapy were present in the study population. The patients provided written consent to participate in the study.
The patients were rehabilitated by using two standard implants (MkIII, MkIV, Brånemark System, Nobel Biocare, www.nobelbiocare.com; and NobelSpeedy™, Nobel Biocare). One implant was placed in the axial position and another implant tilted distally up to 45º. A total of 84 implants were placed, all in immediate function, as part of 42 partial rehabilitations. The implant diameter varied between 3.3 mm and 4 mm, and the length varied between 7 mm and 18 mm. The distribution of the implants and respective opposing dentitions is displayed in Table 1.
The surgical procedures were performed under local anesthesia with mepivacaine chlorhydrate with epinephrine 1:100,000 (Scandinibsa 2%®, Inibsa Laboratory, www.inibsa.com). All patients were sedated with diazepam (Valium® 10 mg, Roche, www.roche.com) prior to surgery. Antibiotics (amoxicillin 875 mg + clavulanic acid 125 mg, Labesfal Genericos, www.labesfalgenericos.pt) were given 1 hour prior to surgery and daily for 6 days thereafter. Cortisone medication (prednisone 5 mg [Meticorten®], Schering-Plough Farma, Lda, www.merck.com) was given daily in a regression mode (15 mg to 5 mg) from the day of surgery until 4 days postoperatively. Anti-inflammatory medication (ibuprofen 600 mg, Ratiopharm, Lda, www.ratiopharm.com) was administered for 4 days postoperatively starting on day 4. Analgesics (clonixine 300 mg, [Clonix®], Janssen-Cilag Farmaceutica, Lda, www.janssen-emea.com) were given on the day of surgery and postoperatively for the first 3 days if needed. Antacid medication (omeprazole, 20 mg) was given on the day of surgery and daily for 6 days postoperatively. Teeth were extracted, when needed, at the time of surgery before implant placement. A mucoperiosteal flap was raised at the ridge crest with relieving incisions on the buccal aspect in the molar area. A small window was opened to the sinus using a round bur for identification of the exact position of the anterior sinus wall.42
The insertion of the implants followed standard procedures, except that under-preparation was employed to achieve an insertion torque of at least 30 Ncm before final seating. The implant neck was aimed to be positioned 0.5 mm to 1 mm below the bone level, and bicortical anchorage was established whenever possible.
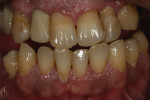
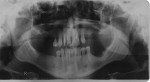
A clinical situation is illustrated in Figure 1 , Figure 2, Figure 3, Figure 4, Figure 5, Figure 6, Figure 7, and Figure 8.
Tilting the posterior implant made it possible to position the implant head in the second premolar/first molar region instead of in the canine/first premolar region in the case of a vertically placed posterior implant. The anterior implants were positioned vertically by means of a guide pin. Care was taken to avoid conflict between the apices of the anterior and the tilted posterior implants. The anterior implants were most often either 4 or 3.75 mm in diameter and were typically placed in the canine or first premolar positions.
This implant arrangement resulted in supports at both ends of the partial bridge, avoiding cantilevers. After closing and suturing the flap with 3-0 nonresorbable suture, the impression copings were placed and an impression was taken.
Provisional partial all-acrylic prostheses were delivered on the day of surgery (n = 42). A premade impression tray was used. Small volumes of silicon were placed around the copings, followed by complete filling with soft putty. After removal of the copings, protection caps were placed to support the peri-implant mucosa during the manufacturing of the prosthesis. Based on the impression, high-density baked all-acrylic prostheses with titanium cylinders were manufactured at the laboratory and most often delivered to the patients within 2.5 hours (Figure 3).
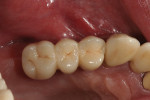
Final prostheses were delivered 4 to 6 months after surgery, consisting of ceramic/metal-ceramic bridges (Figure 4 , Figure 5, and Figure 6). If an adjustment of the angulated abutment was needed for better positioning of the screw access hole, the impression for the final prosthesis was taken at implant level. The abutment position was then determined at the laboratory and adjusted in the patient's mouth.
Assessment/Data
All patients were included in a prospective follow-up protocol and evaluated clinically (at 10 days, 2 months, 4 months, and 6 months, and every 6 months thereafter) and radiologically (at 10 days, 6 months, 1 year and 5 years follow-up visits). The prostheses were removed at each follow-up appointment to perform the clinical assessments. The following clinical data was recorded: clinical mobility (Mob) and suppuration (Sup). Mob was evaluated using manual movement to assess individual implant mobility and registered as present or absent;48 Sup was evaluated by applying finger pressure to the peri-implant complex and registered as present or absent.48
For the radiological evaluation through intraoral technique, a conventional radiograph holder was used, the position of which was adjusted manually to ensure orthogonal film positioning. The lower corner of the implant head was radiographed as a reference point for the bone level measurements.
An implant was classified as a success according to the following criteria adopted by the authors: 1) it fulfilled its purported function as support for reconstruction; 2) it was stable when individually and manually tested; 3) no signs of infection were observed; 4) it demonstrated a good esthetic outcome of the rehabilitation; 5) it allowed fabrication of the implant-supported fixed prosthesis, which provided patient comfort and hygiene; and 6) it had a high probability of long-term stability, as judged by the annual bone loss (< 2 mm in the first year 43; less than 0.2 mm/year from thereafter49).
The following complication parameters were assessed: 1) mechanical complications: fracture or loosening of mechanical and prosthetic components, and wear marks in the prosthesis (as indicators of overload); 2) biological complications: soft-tissue inflammation, fistula formation, pain, or maxillary sinus infections; 3) esthetic complications: esthetic complaints from the patient or dentist; 4) functional complications: phonetic, masticatory, and comfort complaints; and 5) oral hygiene complications: poor oral hygiene.
Descriptive statistics were used to classify the variables of interest. Survival estimates were computed using the Kaplan-Meier product limit estimation and corresponding 95% confidence intervals (CIs) for the mean survival estimate. Inferential statistical analyses (Mann-Whitney U) of the marginal bone resorption were performed for the 1-year and 5-year evaluations to test the hypothesis of equality of mean ranks of the marginal bone resorption between axial implants and tilted implants (α = .05).
Results
One implant (position 24) was lost in one patient after 56 months of follow-up, rendering a survival rate of 97.1% and 98.8% at 8 years (Kaplan-Meier), using the patient and implant as units of analysis, respectively (Table 2). The lost implant showed signs of severe bone loss and was removed, followed by the curettage of the implant site, disconnection of the prosthesis, and placement of a removable prosthesis for 6 months (after this healing period an implant would be inserted in the same site). The mean implant survival estimate was 97.1 months (95% CI: 93.3 months to 100.8 months [the maximum registered follow-up for an implant was 99 months]). A total of two unaccounted implants were registered belonging to one patient who deceased 4 months after implant insertion due to causes unrelated to the treatment. No dropouts occurred during the follow-up of this study.
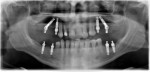
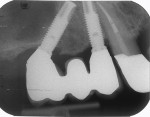
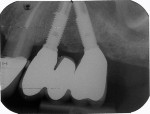
Seventy-seven implant radiographs (91% at patient level) were readable for marginal bone level at 1 year, while 17 implant radiographs (100% at patient level) were readable at the 5-year follow-up. The marginal bone resorption for the implants was 1.05 mm (standard deviation [SD] = 0.65 mm) at 1 year of function, with a distribution for the axial and tilted implants of 1.08 mm (SD = 0.65 mm) and 0.92 mm (SD = 0.49 mm), respectively. At 5 years of function, the marginal bone resorption for the implants was 1.47 mm (SD = 0.37 mm), with a distribution for the axial and tilted implants of 1.64 mm (SD = 0.63 mm) and 1.25 mm (SD = 0.29 mm), respectively. Representative radiographs at 5-year follow-ups are presented in Figure 7 and Figure 8. The frequencies of marginal bone resorption are presented in Table 3 and in Figure 9 and Figure 10.Three implants in three patients presented bone resorption exceeding 2 mm at the 1-year follow-up, with two of them being an outlier value (Figure 9). One implant in one patient presented with bone resorption exceeding 2.5 mm at the 5-year follow-up, representing an outlier value (Figure 10). The difference in marginal bone resorption between axial and tilted implants was not significant at the 1-year (P = 0.107) and 5-year (P = 0.211) evaluations.
Two bridges (provisionals) fractured in two patients: One with recurrent fractures at 10 days, 1 month, and 2 months postsurgically; and another at 6 months postsurgically. One abutment screw loosening occurred in one patient at 4 months follow-up. In all three situations, the patients were heavy bruxers presenting wear patterns in the opposing dentition. The situations were resolved by repairing the prosthesis, adjusting the occlusion, and manufacturing an occlusal nightguard. No further mechanical complications were registered.
Two patients presented peri-implant pathology in one implant each, with presence of suppuration, peri-implant pockets, and bleeding on probing at 11 months and 4 years of function. The first patient was referred for surgical intervention to successfully resolve the problem, while the second patient's problem was resolved through nonsurgical treatment (scaling and irrigation with chlorhexidine).50 No further biological complications were registered.
No functional or esthetic complications were registered during the follow-up of this study.
Discussion of Results
The choice of study parameters was based on the theoretical analysis of biomechanics and load distribution using axial and tilted implants to provide prosthetic support. The hypothesis to test was that immediate placement and function of two implants (one anterior axial implant and one posterior implant tilted distally) for partial rehabilitation of the posterior maxilla was possible with the same level of success as for partial rehabilitations in other areas using immediate function implants. The 1-year and 5-year survival rates compare favorably to data of partial edentulous rehabilitations in the maxilla using implants in immediate function47 and support the research hypothesis.
The marginal bone resorption values were distributed within the accepted standards for implant rehabilitations.47,51 At the 1-year follow-up, three implants in three patients (one on each patient) presented more than 2 mm of marginal bone resorption. One of the implants represented the implant failure that was accounted for in the survival analysis and later removed. For the remaining two implants, given the absence of wear patterns or peri-implant pathology, a possible explanation may be the fact that both patients had a history of periodontal pathology, and one patient was a heavy smoker (40 cigarettes/day), which in association to the position of the implants (posterior region of the maxilla) may have contributed to this outlier value for marginal bone resorption.50 At the 5-year follow-up, one implant in one patient presented more than 2.5 mm of marginal bone resorption. This was due to an episode of peri-implant pathology that occurred because of infection at 4 years of follow-up. The implant was inserted next to a tooth that after 2 years developed an aggressive episode of periodontitis with loss of supporting bone (thereby affecting the adjacent implant). The difference in marginal bone resorption values between axial and tilted implants was not significant at 1 year (P = 0.107) and 5 years of function (P = 0.211).
Mechanical complications occurred in three patients in the first 6 months of function. The main cause for these complications may be related to occlusal overload due to the fact that the patients were heavy bruxers. Once the occlusion was adjusted and a nightguard was manufactured no further mechanical complications occurred in the follow-up of the study, including after the insertion of the definitive prostheses in all patients. Biological complications occurred in two patients in whom the implants were placed in a periodontal compromised area, a fact that may have contributed to these incidences.50
The discussion of the biomechanical aspect comprises several issues. The nature of this concept, thought to rehabilitate partial edentulism in the posterior maxilla, implied a careful planning so that it could provide a functional prosthetic support in areas submitted to high occlusal loads. The concept design was aimed at avoiding several factors such as a straight implant alignment, suboptimal implant size, or the use of cantilevers in order to decrease the potential bending forces of the implants.
In terms of mechanical strength, the low marginal bone resorption registered in this study allowed for the implants to be positioned above the threshold for increased risk of incidence of implant fractures. In this study, the mean marginal bone resorption was below 1.5 mm, which meant that the exposure of the implant section was located before the implants' second thread in the apical direction. This way, the implants were not exposed below the area of two to three threads (the area of engagement of the abutment screw), which would have made them more prone to increased probability of implant fracture due to bending overload.11
The issue of implant load is also an important biomechanical aspect to consider. The results obtained in this study also reflected the effect of parafunctional habits, as these were the main causes for the incidence of mechanical complications, namely bridge fractures. The remedies implemented were enough to resolve the complications, but parafunctional habits remain an important consideration in treatment planning, with the objective of diagnosing potential heavy bruxers prior to the prosthetic rehabilitation. The fact that no mechanical complications occurred after the insertion of the metal-ceramic bridges may also be related to the influence of the prosthetic material on implant loading,31 but this issue was not addressed in this study.
The presence of cantilevers magnifies vertical and lateral forces generated at the occlusal contact, which can translate clinically into mechanical complications and bone loss. The results of this study also support these findings, as the partial rehabilitations comprised support at both ends of the bridge without the use of cantilevers, which translated clinically into good outcomes.
The use of implant tilting is one of the most important aspects of this concept, as it provided greater posterior support and enabled insertion of longer implants with potential for enhanced primary anchorage, a fundamental issue in immediate function. No differences were observed in the outcome of these implants when compared with axial implants, as the hypothesis of equality of mean ranks for the marginal bone resorption was not rejected at the 1- and 5-year evaluations.
The limitations of the study include: only one clinic was involved; only one operator was involved; small sample size; and lack of a control group. The extrapolation of results from this clinical study to the general population should be made with caution, as the analysis is limited to the middle-aged partial edentulous population (around 56 years of age) with the variable "age" normally distributed. Long-term randomized clinical trials should be conducted to measure the effect of this type of rehabilitation in its full length.
The importance of interdisciplinary care in the treatment of adult patients is unquestionable, providing patients with further treatment possibilities.52 Interdisciplinary care was linked to the excellent outcome achieved in the rehabilitations in this study. To achieve success, it was necessary to join the efforts of an implantologist (implant placement for rehabilitation of the partially edentulous maxillae), a prosthodontist (fixed prosthetic implant-supported rehabilitation), a general practitioner, and a dental hygienist. The interdisciplinary approach to oral healthcare is linked to stronger patient participation in the treatment protocol, which leads to an optimal treatment outcome and patient satisfaction.53 The interdisciplinary work in this study allowed for a reduction in rehabilitation treatment steps, a procedure described in the literature.54
Despite the specific conditions of this type of rehabilitation, the importance of the general practitioner should be emphasized. Typically the first to make contact with the patient, the general practitioner possesses a degree of knowledge that correlates significantly with the outcome of the rehabilitation. A well-informed dentist is better able to advise patients by proposing alternative treatment plans with the paFtients' best interests in mind. In the presented cases, the general practitioner acted in two different pathways: as the coordinator of the treatment plan, responsible for the patients' referral; and as the intermediary, facilitating communication between the different specialties.
Disclosure
Dr. Maló currently serves as a consultant for Nobel Biocare AB.
References
1. Regev E, Smith RA, Perrot DH, Pogrel MA. Maxillary sinus complications related to endosseous implants. Int J Oral Maxillofac Implants. 1995;10(4):451-461.
2. Jensen OT, Shoulman LB, Block MS, Iacono VJ. Report of the Sinus Consensus Conference of 1996. Int J Oral Maxillofac Implants. 1998;13(suppl):11-45.
3. Maló P, de Araújo Nobre M, Rangert B. Short implants placed one-stage in maxillae and mandibles: a retrospective clinical study with 1 to 9 years of follow-up. Clin Implant Dent Relat Res. 2007;9(1):15-21.
4. Friberg B, Jemt T, Lekholm U. Early failures in 4,641 consecutively placed Brånemark dental implants: a study from stage 1 surgery to the connection of completed prostheses. Int J Oral Maxillofac Implants. 1991;6(2):142-146.
5. Lekholm U. The Brånemark implant technique: A standardized procedure under continuous development. In: Laney WR, Tolman DE, eds. Tissue Integration in Oral, Orthopedic, and Maxillofacial Reconstruction. Chicago, IL: Quintessence Publishing; 1992:194-199.
6. Rangert B, Sennerby L, Nilson H. Load factor analysis for implants in the resorbed posterior maxilla. In: Jensen OT, ed. The Sinus Bone Graft. Chicago, IL: Quintessence Publishing; 1999:167-177.
7. Piattelli A, Piattelli M, Scarano A, Montesani L. Light and scanning electron microscopic report of four fractured implants. Int J Oral Maxillofac Implants. 1998;13(4):561-564.
8. Swanberg DF, Henry MD. Avoiding implant overload. Implant Soc. 1995;6(1):12-14.
9. Rangert B, Jemt T, Jörneus L. Forces and moments on Brånemark implants. Int J Oral Maxillofac Implants. 1989;4(3):241-247.
10. Rangert B. Mechanical and biomechanical guidelines for the use of Brånemark System—clinical studies. Aust Prosthodont J. 1993;7(suppl):45-49.
11. Rangert B, Krogh PH, Langer B, Van Roekel N. Bending overload and implant fracture: a retrospective clinical analysis. Int J Oral Maxillofac Implants. 1995;10(3):326-334.
12. Rilo B, da Silva JL, Mora MJ, Santana U. Guidelines for occlusion strategy in implant-borne prostheses. A review. Int Dent J. 2008;58(3):139-145.
13. Rangert BR, Sullivan RM, Jemt TM. Load factor control for implants in the posterior partially edentulous segment. Int J Oral Maxillofac Implants. 1997;12(3):360-370.
14. Purton DG, Carter GM, Hunter KM. Success and failure in partial edentulism treated with implant-supported bridges. N Z Dent J. 1994;90(401):98-102.
15. Morgan MJ, James DF, Pilliar RM. Fractures of the fixture component of an osseointegrated implant. Int J Oral Maxillofac Implants. 1993;8(4):409-414.
16. Capodiferro S, Favia G, Scivetti M, et al. Clinical management and microscopic characterisation of fatigue-induced failure of a dental implant. Case report. Head Face Med. 2006;22:18.
17. Piattelli A, Scarano A, Piattelli M, et al. Hollow implants retrieved for fracture: a light and scanning electron microscope analysis of 4 cases. J Periodontol.1998;69(2):185-189.
18. Isidor F. Loss of osseointegration caused by occlusal load of oral implants. A clinical and radiographic study in monkeys. Clin Oral Implants Res. 1996;7(2):143-152.
19. Isidor F. Histological evaluation of peri-implant bone at implants subjected to occlusal overload or plaque accumulation. Clin Oral Implants Res. 1997;8(1):1-9.
20. Alexander H, Ricci JL, Hrico GJ. Mechanical basis for bone retention around dental implants. J Biomed Mater Res B Appl Biomater. 2009;88(2):306-311.
21. van Steenberghe D, Naert I, Jacobs R, Quirynen M. Influence of inflammatory reactions vs. occlusal loading on peri-implant marginal bone level. Adv Dent Res. 1999;13:130-135.
22. Quirynen M, Naert I, van Steenberghe D. Fixture design and overload influence marginal bone loss and implant success in the Brånemark system. Clin Oral Implants Res. 1992;3(3):104-111.
23. Tawil G. Peri-implant bone loss caused by occlusal overload: repair of the peri-implant defect following correction of the traumatic occlusion. A case report. Int J Oral Maxillofac Implants. 2008;23(1):153-157.
24. Misch CE, Suzuki JB, Misch-Dietsh FM, Bidez MW. A positive correlation between occlusal trauma and peri-implant bone loss: literature support. Implant Dent. 2005;14(2):108-116.
25. Uribe R, Peñarrocha M, Sanchis JM, García O. Marginal peri-implantitis due to occlusal overload. A case report. Med Oral. 2004;9(2):159-162.
26. Khraisat A, Abu-Hammad O, Al-Kayed AM, Dar-Odeh N. Stability of the implant/abutment joint in a single-tooth external-hexagon implant system: clinical and mechanical review. Clin Implant Dent Relat Res. 2004;6(4):222-229.
27. Brunski JB. In vivo bone response to biomechanical loading at the bone/dental-implant interface. Adv Dent Res. 1999;13:99-119.
28. English CE. Biomechanical concerns with fixed partial dentures involving implants. Implant Dent. 1993;2(4):221-242.
29. McAlarney ME, Stavropoulos DN. Theoretical cantilever lengths versus clinical variables in fifty-five clinical cases. J Prosthet Dent. 2000;83(3):332-343.
30. Shackelton JL, Carr L, Slabbert JC, Becker PJ. Survival of fixed implant-supported prostheses related to cantilever lengths. J Prosthet Dent. 1994;71(1):23-26.
31. Duyck J, Van Oosterwyck H, Vanden Sloten J, et al. Magnitude and distribution of occlusal forces on oral implants supporting fixed prostheses. An in vivo study. Clin Oral Implants Res. 2000;11(5):465-475.
32. Haraldson T, Zarb G. A 10-year follow-up study of the masticatory system after treatment with osseointegrated implant bridges. Scand J Dent Res. 1988;96(3):243-252.
33. Shalak R. Biomechanical considerations in osseointegrated prostheses. J Prosthet Dent. 1983;49(6):843-848.
34. Glantz PO, Rangert B, Svensson A, et al. On clinical loading of osseointegrated implants. A methodological and clinical study. Clin Oral Implants Res. 1993;4(2):99-105.
35. Benzing UR, Gall H, Weber H. Biomechanical aspects of two different implant-prosthetic concepts for edentulous maxillae. Int J Oral Maxillofac Implants. 1995;10(2):188-198.
36. Pattersson EA, Burguete RL, Thoi MH, Johns RB. Distribution of load in an oral prosthesis system: an in vitro study. Int J Oral Maxillofac Implants. 1995;10(5):552-560.
37. Tashkandi EA, Lang BR, Edge MJ. Analysis of strain at selected bone sites of a cantilevered implant-supported prosthesis. J Prosthet Dent. 1996;76(2):158-164.
38. Assif D, Marshak B, Horowitz A. Analysis of load transfer and stress distribution by an implant-supported fixed partial denture. J Prosthet Dent. 1996;75(3):285-291.
39. Rangert B, Sullivan R. Biomechanical principles: preventing prosthetic overload induced by bending. Nobelpharma News. 1993;7(3):4-5.
40. Krekmanov L, Kahn M, Rangert B, Lindstrom H. Tilting of posterior mandibular and maxillary implants for improved prosthesis support. Int J Oral Maxillofac Implants. 2000;15(3):405-414.
41. Fortin Y, Sullivan RM, Rangert B. The Marius implant bridge: surgical and prosthetic rehabilitation for the completely edentulous upper jaw with moderate to severe resorption: a 5-year retrospective clinical study. Clin Implant Dent Relat Res. 2002;4(2):69-77.
42. Maló P, Rangert B, Nobre M. All-on-4 immediate-function concept with Brånemark System implants for completely edentulous maxillae: A 1-year retrospective clinical study. Clin Implant Dent Relat Res. 2005;7(suppl 1):S88-S94.
43. Balleri P, Ferrari M, Veltri M. One-year outcome of implants strategically placed in the retrocanine bone triangle. Clin Implant Dent Relat Res. 2010;12(4):324-330.
44. Aparicio C, Perales P, Rangert B. Tilted implants as an alternative to maxillary sinus grafting: a clinical, radiologic, and periotest study. Clin Implant Dent Relat Res. 2001;3(1):39-49.
45. Calandriello R, Tomatis M. Simplified treatment of the atrophic posterior maxilla via immediate/early function and tilted implants: A prospective 1-year clinical study. Clin Implant Dent Relat Res. 2005;7(suppl 1):S1-S12.
46. Maló P, Rangert B, Nobre M. All-on-4 immediate-function concept with Brånemark System implants for completely edentulous mandibles: A retrospective clinical study. Clin Implant Dent Relat Res. 2003;5(suppl 1):S2-S9.
47. Maló P, Rangert B, Dvärsäter L. Immediate function of Brånemark implants in the esthetic zone: A retrospective clinical study with 6 months to 4 years of follow-up. Clin Implant Dent Relat Res. 2000;2(3):138-146.
48. Maló P, Nobre Mde A, Petersson U, Wigren S. A pilot study of complete edentulous rehabilitation with immediate function using a new implant design: case series. Clin Implant Dent Relat Res. 2006;8(4):223-232.
49. Albrektsson T, Dahl E, Enbom L, et al. Osseointegrated oral implants. A Swedish multicenter study of 8139 consecutively inserted Nobelpharma implants. J Periodontol.1988;59(5):287-296.
50. De Araújo Nobre M, Capelas C, Alves A, et al. Non-surgical treatment of peri-implant pathology. Int J Dent Hyg. 2006;4(2):84-90.
51. Malo P, De Araújo Nobre M, Rangert B. Implants placed in immediate function in periodontally compromised sites: a five-year retrospective and one-year prospective study. J Prosthet Dent. 2007;97(6 suppl):S86-S95.
52. Akin-Nergiz N, Nergiz I, Schmage P. Interdisciplinary concepts in treating adult patients. J Orofac Orthop. 1997;58(6):340-351.
53. Vandamme K, Opdebeeck H, Naert I. Pathways in multidisciplinary oral health care as a tool to improve clinical performance. Int J Prosthodont. 2006;19(3):227-235.
54. Lai YL, Chou IC, Liaw YC, et al. Triple immediate therapy (ridge expansion, soft tissue augmentation, and provisional restoration) of maxillary anterior single implant. J Periodontol.2007;78(7):1348-1353.
About the Authors
Paulo Maló, DDS, PhD
Surgery and Prosthetic Department
Maló Clinic
Lisbon, Portugal
Miguel de Araújo Nobre, RDH
Clinical Research Department
Maló Clinic
Lisbon, Portugal