Implant-Assisted Overdenture: A Case Report
Doug McMaster, DDS
Abstract
A patient's extreme susceptibility to periodontal disease, likely exacerbated by a history of smoking, resulted in severe periodontal breakdown. Employing a systematic approach that identified both patient risk and prognosis using data gathered during the patient examination, a treatment plan was developed that included extraction of structurally compromised teeth and the use of implant-assisted complete overdentures. This treatment approach accomplished a reduction of biomechanical, periodontal, and dentofacial risk, as well as an increase in functional harmony.
Dental patients may undergo many years of fine restorative dentistry, comply with preventive care recommendations, and yet still lose their teeth because even the best dentistry and patient cooperation can be undermined by host susceptibility.1 The Kois Center philosophy embraces a systematic approach that identifies both patient risk and prognosis using data gathered during the patient examination. This approach addresses host susceptibility in the development of a treatment plan that lowers the patient's risk for future dental disease.
This case documents a dental outcome that many consider a failure for either the patient or the clinician: the loss of all teeth. However, by using these systematic principles, a treatment plan was developed that lowered the patient's risk of future dental problems and provided a significant improvement in his quality of life.
Clinical Case Overview
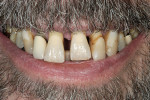
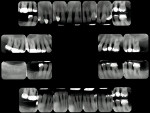
Patient History and Chief Complaint: A 53-year-old man presented with chief concerns regarding the appearance, sensitivity, and mobility of his teeth (Figure 1). He responded positively on the dental questionnaire for bleeding gums, sore teeth, sensitivity to temperature, unpleasant taste or odor in mouth, clenching of teeth, and lost teeth.
The patient reported that he had seen at least three dentists in the previous 4 years at his current dental office and had been receiving periodontal maintenance appointments every 3 months. His most recent full-mouth radiographs were 1 year old, and he had been previously told by his periodontist that he needed full dentures, with or without implants.
He disliked the appearance of the gum tissue at the necks of the teeth, and he wanted crowns, if possible, as alternatives to a “full plate.” An avid scuba diver, the patient was afraid he would lose his dentures while diving. He was also concerned that dentures would alter his sense of taste.
The patient’s medical review revealed a history of tonsillectomy, appendectomy, and pleural effusion. He had recently quit smoking and was currently taking vitamins and dietary supplements, with no contraindications to proceeding with dental treatment.
Diagnostic Findings
Periodontal: The examination revealed generalized probing depths between 5 mm and 9 mm, with generalized bleeding and localized sites of suppuration. The combination of recession and probing depths resulted in a generalized 8 mm to 12 mm of attachment loss. Radiographs revealed severe horizontal bone loss, multiple vertical osseous defects, and the appearance of possible apical periodontal communication. Approximately half of the teeth exhibited Class 1 mobility, with the remaining teeth Class 2 or 3. All molars demonstrated at least one furcation invasion of grade 1 with multiple grade 2 and 3 involvements. The diagnosis was type AAP IV, advanced periodontitis.
Risk: High
Prognosis: Hopeless
Biomechanical: Upon clinical examination, several teeth had acceptable small direct restorations. Tooth Nos. 2 through 5, 7, 12 through 14, 19, and 29 had either large direct restorations or full-coverage crowns, indicating structurally compromised teeth. Active caries was not noted. Pulpal involvement was visible on tooth No. 19.
Risk: Moderate
Prognosis: Fair
Functional: The patient reported a tendency at times to clench his teeth. Examination revealed tenderness of the masticatory musculature and temporomandibular joint (TMJ) crepitus. Minimal attrition was present on all anterior teeth. Anterior teeth were in contact and the maxillary anterior teeth were splayed and mobile. The patient’s history of squeezing, along with the observation of crepitus and muscle tenderness, contributed to the diagnosis of occlusal dysfunction.
Risk: Moderate
Prognosis: Fair
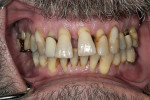
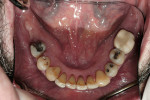
Dentofacial: The following observations were evident upon examination: high maxillary lip dynamics, with 3 mm to 4 mm of incisor display at rest. In a full smile, the free gingival margins were not visible due to recession, but 2 mm to 4 mm of root structure was visible beyond the anatomical cemento-enamel junction (CEJ) of all upper teeth (Figure 2). Soft-tissue scalloping was close to normal but appeared unattractive due to the large amount of recession and loss of papillae. Horizontal asymmetry was noted in the lower anterior region (Figure 3).
Risk: High
Prognosis: Poor
Medical: There were no contraindications to dental treatment at this time. Had his smoking habit been current, this could be considered a slight increased risk factor for dental implants.2-4
Risk: Low
Prognosis: Good
Treatment Goals
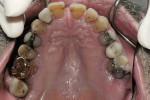
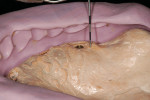
The risk management considerations and treatment plan were developed using a systematic approach. The treatment would reduce the biomechanical risk by removing the structurally compromised teeth (Figure 4 and Figure 5), as well as reduce the functional risk by creating an occlusion in harmony with the joints. Additionally, treatment would reduce the periodontal risk by removing hopeless, periodontally involved teeth (Figure 6) and improve esthetics by raising the occlusal plane 3 mm to minimize root and gingival display.5-8
Additionally, treatment goals addressed two specific patient demands: the restorative result would be stable enough to hold a scuba regulator, and an exposed palate would be incorporated to prevent taste alteration.9-13
Treatment Plan
The treatment plan consisted of consultation with the periodontist to identify the best implant sites and fabrication of an immediate transitional denture. A surgical guide would also be fabricated, and all teeth would be extracted, followed by delivery of the immediate denture. It was determined the best locations for the greatest length of implants would be in positions of tooth Nos. 6, 8, 11, 13, 19, 22, 27, and 30, with ultimate delivery of implant-assisted complete overdentures.
Treatment Phase
During consultation with the periodontist, it was determined that no teeth could be retained. Potential implant sites were identified using radiographs and study models.
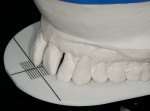
The immediate transitional denture was designed (Figure 7). The facial surface of tooth No. 9 was in the desired horizontal position and, when shortened by 3 mm, was in the desired vertical position. The modified tooth No. 9 then became the “go by” tooth, establishing the incisal edge position. Instructions were given to the dental laboratory to raise the remaining upper teeth, keeping them level with the shortened position of tooth No. 9, completing the occlusal plane. The lower anterior teeth were shortened 2 mm on the diagnostic cast establishing the lower incisal edge position, and the laboratory was instructed to close the occlusal vertical dimension as necessary to regain anterior contact with the desired upper arch.
The immediate transitional denture was used as a surgical guide during tooth extraction and placement of the implants. Holes were placed in the denture acrylic through the occlusal or lingual to tooth Nos. 6, 8, 11, 13, 19, 22, 27, and 30. The transitional denture was used as the actual surgical guide to minimize costs and allow immediate scheduling. The teeth were extracted, necessary bone grafting was accomplished, implants were placed, and the transitional denture was inserted. Several relines of the transitional denture were necessary throughout the following months to accommodate soft-tissue healing and close the holes made for the surgical guide; this did not compromise patient comfort or fit. Shortly after placing the transitional denture, the patient could detect a reduction of taste perception, particularly of chocolate.
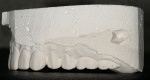
The transitional denture came extremely close to achieving the goals of raising the occlusal plane for esthetics and palatal repositioning of the upper incisors (Figure 8). The attempt to raise the occlusal plane esthetically resulted in the transitional denture occlusal plane being superior to the acrylic overlying the maxillary tuberosity (Figure 9). During the integration period the patient was able to successfully scuba dive with the transitional denture resting on the healing screws.
Upon integration of the implants, new dentures were fabricated. Fixture level impressions were taken using an open-tray technique. Prior to the wax try-in, the transitional denture was modified to close the diastema between tooth Nos. 8 and 9, allowing the patient and his family to decide if they wanted to maintain the diastema in the final denture. The patient elected to close the diastema in the final denture. The final occlusal plane was established, with the result being slightly lower than the transitional denture.
Once the wax try-in was accepted by the patient, silicone matrices were made of the upper and lower try-in set-ups. These matrices, or guides, fit onto the master models containing the fixture analogs and captured the entire facial and a portion of the occlusal surfaces of the teeth.
The silicone matrices were used to design the bar and attachment location on the master model so that adequate thickness of the denture framework and acrylic could be created. The design included a split frame bar for the mandibular arch in order to reduce the effect of mandibular flexure.14-17 Due to the severity of the periodontal disease, a large amount of tissue shrinkage was expected and did occur. There was adequate interocclusal space to create the bar assembly (Figure 10), and attachments were chosen, keeping height to a minimum. The space available for bar placement could easily be seen with the silicone matrix guide positioned on the master cast, and the laboratory fabricated the bar with attachments. The lower arch had 3 mm more space available than the upper arch as a result of raising the occlusal plane and changing the occlusal vertical dimension. Clips were used to provide both tripod stabilization and potential alternative retention in the event that implant fixtures were compromised in the future.
The bar and attachments were tried in, verified for passivity, and the wax try-in dentures were placed in the mouth, onto the bar and attachment assemblies, to confirm achievement of esthetic and functional goals.
The dentures were processed and then reinserted on the frameworks and attachments intraorally (Figure 11, Figure 12 and Figure 13). A bite registration was taken with an anterior deprogramming stop, and the case was remounted for occlusal refinement.
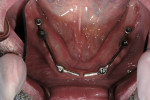
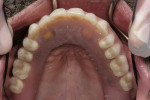
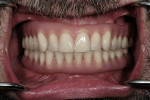
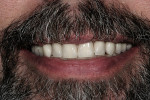
The bars were torqued onto the implants, and the dentures were delivered to the patient (Figure 14, Figure 15 and Figure 16).
Conclusion
Recognizing risks that may cause a dental restoration or treatment to fail earlier than anticipated can be quite valuable. The patient in this case had received acceptable restorative dentistry. Both the patient and his periodontal providers made diligent efforts to treat and maintain his periodontal health. However, the patient’s extreme susceptibility to periodontal disease, likely exacerbated by a history of smoking, resulted in such severe periodontal breakdown that he was uncomfortable with and embarrassed by his mouth. Neither more, nor better, treatment would have prevented ultimate tooth loss.
Acknowledging the patient’s significant susceptibility to periodontal disease and designing the treatment plan to reduce or manage risk served to increase long-term prognosis. Extracting all of the teeth accomplished a reduction of biomechanical and periodontal risk. The implant-supported denture was designed to be in functional harmony, and dentofacial risk was managed by vertically positioning the denture teeth more ideally within the framework of the lips and face. A systematic review of risk and prognosis laid the foundation for a treatment plan that provided significant improvement in the patient’s quality of life and lessened risk of future dental problems.
Acknowledgment
Implant placement, bone grafting, removal of existing teeth, and delivery of the immediate denture were performed by Brien Harvey, DDS, MS, Tucson, Arizona. The bar and attachments were fabricated by Dental Prosthetics, Tucson, Arizona, and the dentures were constructed by Eastside Dental Services, Tucson, Arizona.
References
1. Burt B. Position paper: epidemiology of periodontal diseases. J Periodontol. 2005;76(8):1406-1419.
2. Kumar A, Jaffin RA, Berman C. The effect of smoking on achieving osseointegration of surface-modified implants: a clinical report. Int J Oral Maxillofac Implants. 2002;17(6):816-819.
3. DeLuca S, Habsha E, Zarb GA. The effect of smoking on osseointegrated dental implants. Part I: implant survival. Int J Prosthodont. 2006;19(5):491-498.
4. Schwartz-Arad D, Samet N, Samet N, Mamlider A. Smoking and complications of endosseous dental implants. J Periodontol. 2002;73(2):153-157.
5. Kokich VO Jr, Kiyak HA, Shapiro PA. Comparing the perception of dentists and lay people to altered dental esthetics. J Esthet Dent. 1999;11(6):311-324.
6. Vig RG, Brundo GC. The kinetics of anterior tooth display. J Prosthet Dent. 1978;39(5):502-504.
7. Tjan AH, Miller GD, The JG. Some esthetic factors in a smile. J Prosthet Dent. 1984:51(1):24-28.
8. Spear F. Too much tooth, not enough tooth: making decisions about anterior tooth position. J Am Dent Assoc. 2010;141(1):93-96.
9. Kapur KK, Soman SD. Masticatory performance and efficiency in denture wearers. 1964. J Prosthet Dent. 2006;95(6):407-411.
10. Siadat H, Alikhasi M, Mirfazaelian A, et al. Patient satisfaction with implant-retained mandibular overdentures: a retrospective study. Clin Implant Dent Relat Res. 2008:10(2):93-98.
11. Gibbs CH, Mahan PE, Mauderli A, et al. Limits of human bite strength. J Prosthet Dent. 1986;56(2):226-229.
12. Awad MA, Lund JP, Dufresne E, Feine JS. Comparing the efficacy of mandibular implant-retained overdentures and conventional dentures among middle-aged edentulous patients: satisfaction and functional assessment. Int J Prosthodont. 2003;16(2):117-122.
13. Allen PF, McMillan AS. A review of the functional and psychosocial outcomes of edentulousness treated with complete replacement dentures. J Can Dent Assoc. 2003:69(10):662.
14. Zarone F, Apicella A, Nicolais L, et al. Mandibular flexure and stress build-up in mandibular full-arch fixed prostheses supported by osseointegrated implants. Clin Oral Implants Res. 2003;14(1):103-114.
15. Paez CY, Barco T, Roushdy S, Andres C. Split-frame implant prosthesis designed to compensate for mandibular flexure: a clinical report. J Prosthet Dent. 2003;89(4):341-343.
16. Misch CE, ed. Diagnostic casts, preimplant prosthodontics, treatment prostheses, and surgical templates. In: Contemporary Implant Dentistry. 2nd ed. St Louis, MO: Mosby; 1999:135-149.
17. Misch CE, ed. Mandibular full-arch implant fixed prosthetic options. In: Dental Implant Prosthetics. St Louis, MO: Elsevier Mosby; 2005:252-264.
About the Author
Doug McMaster, DDS
Private Practice
Tucson, Arizona