Incorporating Orthodontics into Restorative Treatment to Improve Long-Term Prognosis
Ronald G. Wilkins, DDS
Abstract
Interdisciplinary treatment that incorporated orthodontics with restorative dentistry was used in this complex case to achieve major esthetic changes for a 45-year-old female patient, whose primary concern was the worn appearance of her teeth. The planning and sequential treatment of the case was facilitated using a system of diagnosis, risk assessment, and risk management. By employing orthodontics in the treatment plan, the number of restorations was kept to a minimum, thereby reducing the biomechanical risk to the dentition.
The importance of using a systematic approach to diagnosis, risk assessment, and risk management is critical when analyzing a restorative case.1 This approach can be instrumental in developing a treatment plan that serves to lower or manage risk and improve prognosis.2 The case presented here demonstrates how a complex set of problems can be treated in a straightforward
manner to achieve a satisfactory result.
Background
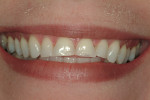
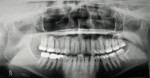
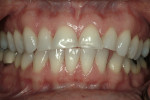
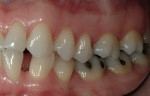
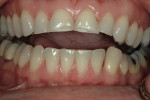
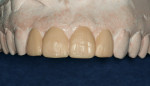
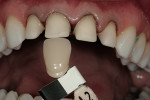
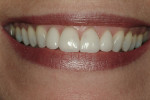
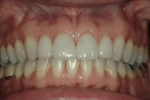
At the time the patient initially presented for treatment, she was a 45-year-old paralegal whose main concern was the worn appearance of her teeth. Her anterior teeth were also becoming sensitive to temperature change (Figure 1 and Figure 2). She stated her concern most succinctly: "I want my smile back" (Figure 3).
Medical History
The patient reported to be in good health and her medical history was non-contributory.
Dental History
The patient had regular dental care for the previous 20 years. She was aware of changes to her anterior teeth, which had gradually become shorter and more sensitive over the past several years.
Diagnostic Findings, Risk Assessment, and Prognosis
Periodontal: The patient presented with 1 mm to 2 mm of bone loss in the mandibular right molar area. She had 1 mm to 2 mm of attachment loss with facial recession in the mandibular anteriors and the maxillary bicuspids. There was no mobility of any teeth. The bone level had been stable for several years. These factors placed her in the American Academy of Periodontology (AAP) Class II category (Figure 4).
Risk: Low
Prognosis: Good
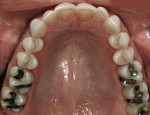
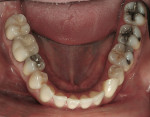
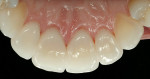
Biomechanical: The patient had several direct restorations in the posterior quadrants that were of acceptable condition. There were two porcelain-fused-to-metal crowns on tooth Nos. 30 and 31. Clinical and radiographic examination revealed no carious lesions. The lingual surfaces of the maxillary incisors exhibited severe erosion (Figure 5 and Figure 6). The etiology of the erosion appeared to be perimyelosis,3,4 a condition defined as the tongue posturing and rubbing on the lingual surfaces of the maxillary anterior teeth. The rubbing, combined with acid, causes the erosion. The source of the acid in this case was somewhat unclear. It appeared to be dietary in nature; however, the acid component may have come from sources present in the past that were no longer influencing the patient's system at the time of diagnosis. There was no history of eating disorders or gastroesophageal reflux disease (GERD). The tongue position can be seen between tooth Nos. 22 and 23 in Figure 7.
Risk: Moderate
Prognosis: Fair
Functional: There were no signs of temporomandibular dysfunction, nor was there any history of clenching or bruxism. With the exception of the maxillary anterior teeth, there were no signs of attrition, occlusal dysfunction, or a constricted chewing pattern. The patient was diagnosed with acceptable function. However, the patient had a secondary risk factor involving the perimyelosis.
Risk: Low
Prognosis: Good
Dentofacial: Dentofacial analysis revealed the patient's desire to lighten the tooth color. There was also a need to alter the maxillary incisal edge position. The maxillary and mandibular occlusal planes were not level in the face (Figure 7). The diastema between tooth Nos. 22 and 23 was of particular concern to the patient (Figure 8). She also presented a high lip dynamic in the maxillary arch and medium to high in the mandibular arch. There was a horizontal gingival asymmetry between tooth Nos. 8 and 9.
Risk: High
Prognosis: Poor
Treatment Goals
- Whiten the patient's teeth.
- Lengthen the maxillary incisors 2 mm to 3 mm. The maxillary anterior teeth needed to be positioned labially to allow for restorative material.
- Level the occlusal planes to make them congruent with the esthetic plane (Figure 9).
- Close the diastema between tooth Nos. 22 and 23.
- Improve gingival symmetry between tooth Nos. 8 and 9.
- Restore the maxillary incisors with materials that harmonize with the natural dentition.
Treatment Plan
After establishing a diagnosis and considering the patient's level of risk in each diagnostic area, a treatment plan was developed that served to decrease the risk and improve the long-term prognosis.5,6 The key element in minimizing long-term risk and improving prognosis was incorporating orthodontics into the treatment plan. By ideally positioning the teeth within the framework of the face and the intra- and inter-arch relationships, the amount of restorative dentistry could be kept to a minimum. Keeping the number of restorations to a minimum reduces the biomechanical risk to the dentition.
Phase I: Orthodontics
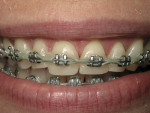
Treatment began with orthodontics for the purpose of leveling and aligning the occlusal planes, closing the diastema, and positioning the anterior teeth for proper restoration. Near the end of the orthodontic phase, transitional composite bonding was placed to restore proper length and contour to the maxillary incisors. This served as an aid in guiding the final orthodontic detailing (Figure 10).
Phase II: Retention
A 6-month retention phase followed the active orthodontic phase. The patient appreciated the improved esthetics that the transitional bonding provided throughout this period (Figure 11). During this time the patient whitened her teeth using 15% carbamide peroxide in bleach trays. Near the end of the retention phase, a Kois deprogrammer was used to ensure the occlusion had equal bilateral contacts on the posterior teeth. Very little adjustment was needed to achieve this occlusion.
Phase III: Restorative
The restorative phase involved the placement of bonded porcelain crowns on the maxillary incisors. This restoration design was chosen to optimize esthetics.7 A diagnostic wax-up was done to develop ideal contours and facilitate production of the provisional crowns (Figure 12). The preparations were of minimal reduction on the labial surfaces, and there was almost no preparation necessary on the lingual surfaces (Figure 13 and Figure 14). Even though most of the enamel had been eroded on the lingual aspects of the incisors, there was a rim of enamel remaining that facilitated bonding. Enamel bonding circumferentially served to increase retention and reduce microleakage (Figure 15).
Conclusion
This article illustrates the use of interdisciplinary treatment (orthodontics and a minimal amount of restorative dentistry) to achieve major esthetic changes (Figure 16 and Figure 17). Using a system of diagnosis, risk assessment, and risk management facilitated the planning and sequential treatment of this complex case. The case proceeded smoothly to a satisfactory result largely as a result of a solid, systematic, and detailed treatment plan (Figures 18).
Acknowledgment
The orthodontic treatment was performed by Rand Bennett, DDS, MS, Salt Lake City, Utah. The crowns were constructed by LeBeau Dental Laboratory, Renton, Wash.
References
1. Kois JC. Diagnostically driven interdisciplinary treatment planning. In: Cohen M, ed. Interdisciplinary Treatment Planning: Principles, Design, Implementation. 1st ed. Chicago IL: Quintessence Publishing; 2008.
2. Bakeman EM. Kois JC. Maximizing esthetics/minimizing risk: the line of predictable success. Inside Dentistry. 2005:1(1):16-24.
3. Imfeld T. Dental erosion. Definition, classification and links. Eur J Oral Sci. 1996;104(2 pt 2):151-155.
4. Bartlett D. Etiology and prevention of acid erosion. Compen Contin Educ Dent. 2009;30(9):616-620.
5. Kois JC. New Challenges in Treatment Planning: Shifting the Paradigm Toward Risk and Perceived Value. Part 1. Journal of Cosmetic Dentistry. 2011;26(4):63-69.
6. Kois JC. New Challenges in Treatment Planning: Incorporating the Fundamentals of Patient Risk Management. Part 2. Journal of Cosmetic Dentistry. 2011;27(1):110-123.
7. Kois JC, McGowan S. Diagnostically generated anterior tooth preparation for adhesively retained porcelain restorations: rationale and technique. Esthetic Technique. 2001;1(2):187-193.
About the Author
Ronald G. Wilkins, DDS
Private Practice,
Salt Lake City, Utah