Treatment of Traumatic Dental Intrusion by Surgical Repositioning: Clinical Case Report
Célia T.M.H. Saito, DDS, MS, PhD; Eloá R. Luvizuto, DDS, MS, PhD; Cláudia Letícia Vendrame dos Santos, DDS, MS, PhD; Carolina Lunardelli Trevisan, DDS, MS; Sônia Regina Panzarini, DDS, MS, PhD; Celso Koogi Sonoda, DDS, MS, PhD; and Wilson Roberto Poi, DDS, MS, PhD
Abstract
The prevalence of dental trauma and its consequences are challenging. This article presents a clinical case of a 9-year-old female who was in a bicycling accident and had a dental intrusion of the left maxillary lateral incisor with extensive dislocation. In the emergency department, surgical repositioning of the intruded tooth and a splinting with steel wire and composite resin was performed and the soft-tissue lesions were sutured. Two weeks after the first visit, pulp necrosis was found and endodontic treatment of the intruded tooth was started with a calcium hydroxide dressing. Despite the traumatic nature of the dental injury, the result of treatment was favorable. After 3 years of follow-up, repair of the resorptions and no signs of ankylosis of the teeth involved were evident. Considering the patient's age and the extent of intrusion, it was concluded that surgical repositioning associated with adequate endodontic therapy was an effective alternative treatment for this case.
Intrusion is the axial dislocation of a tooth into the alveolar bone.1 In the literature, it is described as a rare dental injury, affecting 0.5% to 2% of injuries in permanent teeth. Typically, the tooth involved appears to have had extensive crushing of the periodontal ligament and alveolar bone, as well as a rupture of the pulp neurovascular supply.2 These events are strongly correlated to the extent of the trauma and the degree of root and bone tissue development.2,3 Crushing of the periodontal ligament may result in a loss of gingival insertion and both root and alveolar bone resorptions. While the neurovascular supply may be partially interrupted, in most cases it is completely interrupted, which causes pulp necrosis, and the chances of revascularization are similar to those in the case of tooth avulsion. Should revascularization occur in a tooth with incomplete root formation, the condition could progress to alter the original root shape.1
With regard to the type of treatment, spontaneous re-eruption appears to present less chance of additional risks and more favorable healing. Normally, this treatment is indicated for cases of teeth with incomplete root formation, but it can also be indicated in some cases of teeth with complete root formation.3 Orthodontic repositioning could be indicated for repositioning most teeth with intrusive luxation; however, this requires caution with respect to the direction of traction. Surgical repositioning is indicated for teeth with complete root formation and total intrusion and for cases of multiple intrusions, especially with labial displacement and intrusions of the central incisors with complete intrusion and penetration into the nasal cavity.3
This article presents a clinical case of dental intrusion with extensive dislocation in the anterior maxillary region, treated by surgical repositioning.
Case Report
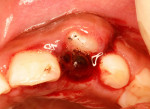
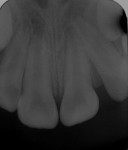
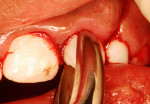
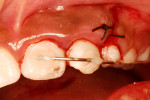
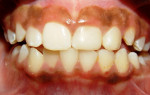
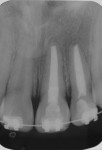
A 9-year-old female who was involved in a bicycling accident presented to the Department of Surgery and Integrated Clinic at São Paulo State University in Araçatuba, Brazil for treatment of a dental injury. At the initial visit, during extraoral examination, a lacerated wound with contusions and edema of the upper lip were found. On intraoral examination, there was evidence of gingival lacerations in the mesial region of the primary upper left canine and an intrusion completely covering the crown of tooth No. 10. A crack in the enamel of tooth No. 9 (Figure 1 and Figure 2) was also observed. Emergency treatment provided 12 hours after the trauma consisted of surgical repositioning of the intruded tooth (Figure 3) and a splinting with steel wire and composite resin, in addition to suturing the intraoral soft-tissue lesions with silk thread 5-0 (Figure 4 and Figure 5). As medication therapy, an antibiotic (amoxicillin 250 mg, every 8 hours for 7 days) and an analgesic (acetaminophen 100 mg, every 8 hours while pain persisted) were prescribed.
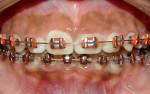
Two weeks after the first visit, pulp necrosis was diagnosed and endodontic therapy of intruded tooth No. 10 was instituted with a dressing of calcium hydroxide and splint removal. The dressing was changed after 15 days. During clinical and radiographic examinations at 45 days, the patient showed a fracture of tooth No. 9 where the original enamel crack was observed. Pulp necrosis of tooth No. 9 was detected, with the presence of a periapical radiolucent area and resorption on the lateral distal surface of the root. Therefore, it was necessary to bond the crown fragment, perform a pulpectomy, and fill the root canal of tooth No. 9 with a calcium hydroxide dressing to control the resorption process. After 1 month of using the calcium hydroxide dressing, the filling of the root canals of teeth Nos. 9 and 10 was performed. In addition, yearly clinical and radiographic examinations were performed to evaluate the treatment results (Figure 6 and Figure 7). After 3 years of follow-up, the teeth presented no signs of root resorption and the treatment was shown to be satisfactory. Furthermore, orthodontic treatment was initiated (Figure 8 and Figure 9).
Discussion
Dental trauma occurs more frequently in children and adolescents, as shown in the literature worldwide.4-8 Moreover, the maxillary anterior teeth are those most involved.4,9 Falls, collisions with other persons and objects, sports, traffic accidents, and violence are the main etiologic factors.4,10-13 Studies that specifically evaluated tooth intrusion have shown evidence of greater frequency of involvement of a single dental element, with dislocation of 1 mm to 8 mm in most cases and the most affected age bracket from 6 to 12 years.14
Among the treatment options to achieve repositioning of an intruded tooth, spontaneous eruption is mentioned as presenting the best prognosis. However, its indication is restricted to cases of teeth with incomplete root formation, some cases of minor displacement of teeth with complete root formation, and orthodontic repositioning—the technique most often indicated for most intruded teeth.3 In the present clinical case, the degree of intrusion with complete coverage of the crown and professional experience contributed to the choice of surgical repositioning, in agreement with Andreasen et al.3
Pulp necrosis was evident and consequently treated. In a study by Andreasen et al,2 140 intruded teeth were examined, and 124 cases of pulp necrosis were verified in which the teeth with incomplete root formation had pulp necrosis diagnosed in longer periods of observation. The other 16 cases that presented with pulp vitality were subsequently shown to have had obliterated root canals. The severity of periodontal ligament trauma in cases of intrusion can be verified by the high rate of progressive, inflammatory resorption and ankylosis.
Frequently, intruded lateral incisors present a high rate of defects in the marginal periodontium. This occurrence seems to be linked to the fact that these teeth are more commonly involved in multiple intrusions.2 In the present clinical case, the lateral incisor was the only intruded tooth, which contributed to a smaller loss of marginal periodontium. Nevertheless, it was not the only tooth affected by the trauma; the central incisor showed a coronal fracture as a direct result of the trauma and probably as an indirect effect of the bone tissue being crushed on its distal face, caused by the displacement of the lateral incisor.
Conclusion
The case reported herein showed satisfactory apical and periodontal healing, which reinforces the efficacy of treating severely intruded permanent teeth by surgical repositioning combined with adequate root canal therapy.
About the Authors
Célia T.M.H. Saito, DDS, MS, PhD
Department of Integrated Clinic and Surgery
UNESP – São Paulo State University
Araçatuba, Brazil
Eloá R. Luvizuto, DDS, MS, PhD
Department of Integrated Clinic and Surgery
UNESP – São Paulo State University
Araçatuba, Brazil
Cláudia Letícia Vendrame dos Santos, DDS, MS, PhD
Department of Integrated Clinic and Surgery
UNESP – São Paulo State University
Araçatuba, Brazil
Carolina Lunardelli Trevisan, DDS, MS
Department of Integrated Clinic and Surgery
UNESP – São Paulo State University
Araçatuba, Brazil
Sônia Regina Panzarini, DDS, MS, PhD
Doctor Assistant Professor of the Department of Integrated Clinic and Surgery
UNESP – São Paulo State University
Araçatuba, Brazil
Celso Koogi Sonoda, DDS, MS, PhD
Doctor Assistant Professor of the Department of Integrated Clinic and Surgery
UNESP – São Paulo State University
Araçatuba, Brazil
Wilson Roberto Poi, DDS, MS, PhD
Doctor Assistant Professor of the Department of Integrated Clinic and Surgery-
UNESP – São Paulo State University
Araçatuba, Brazil
References
1. Andreasen JO, Andreasen FM. Texto e Atlas Colorido de Traumatismo Dental. Porto Alegre: Artmed Editora; 2001:151-180.
2. Andreasen JO, Bakland LK, Andreasen FM. Traumatic intrusion of permanent teeth. Part 2. A clinical study of the effect of preinjury and injury factors, such as sex, age, stage of root development, tooth location, and extent of injury including number of intruded teeth on 140 intruded permanent teeth. Dent Traumatol. 2006;22(2):90-98.
3. Andreasen JO, Bakland LK, Andreasen FM. Traumatic intrusion of permanent teeth. Part 3. A clinical study of the effect of treatment variables such as treatment delay, method of repositioning, type of splint, length of splinting and antibiotics on 140 teeth. Dent Traumatol. 2006;22(2):99-111.
4. Calişkan MK, Türkün M. Clinical investigation of traumatic injuries of permanent incisors in Izmir, Turkey. Endod Dent Traumatol. 1995;11(5):210-213.
5. Mestrinho HD, Bezerra AC, Carvalho JC. Traumatic dental injuries in Brazilian pre-school children. Braz Dent J. 1998;9(2):101-104.
6. Schatz JP, Joho JP. A retrospective study of dento-alveolar injuries. Endod Dent Traumatol. 1994;10(1):11-14.
7. Da Silva AC, Passeri LA, Mazzonetto R, et al. Incidence of dental trauma associated with facial trauma in Brazil: a 1-year evaluation. Dent Traumatol. 2004;20(1):6-11.
8. Zerman N, Cavalleri G. Traumatic injuries to permanent incisors. Endod Dent Traumatol. 1993;9(2):61-64.
9. Sae-Lim V, Hon TH, Wing YK. Traumatic dental injuries at the Accident and Emergency Department of Singapore General Hospital. Endod Dent Traumatol. 1995;11(1):32-36.
10. Altay N, Güngör HC. A retrospective study of dento-alveolar injuries of children in Ankara, Turkey. Dent Traumatol. 2001;17(5):201-204.
11. Cardoso M, de Carvalho Rocha MJ. Traumatized primary teeth in children assisted at the Federal University of Santa Catarina, Brazil. Dent Traumatol. 2002;18(3):129-133.
12. Flanders RA, Bhat M. The incidence of orofacial injuries in sports: a pilot study in Illinois. J Am Dent Assoc. 1995;126(4):491-496.
13. Marcenes W, al Beiruti N, Tayfour D, Issa S. Epidemiology of traumatic injuries to the permanent incisors of 9-12-year-old schoolchildren in Damascus, Syria. Endod Dent Traumatol. 1999;15(3):117-123.
14. Andreasen JO, Bakland LK, Matras RC, Andreasen FM. Traumatic intrusion of permanent teeth. Part 1. An epidemiological study of 216 intruded permanent teeth. Dent Traumatol. 2006;22(2):83-89.