Restoring Esthetics and Function in an Edentulous Patient with Ectodermal Dysplasia
Key Take-Aways
- Mondial® Denture Teeth demonstrate life-like opalescence and possess the strength required for implant-supported dentures.
- These teeth feature high abrasion resistance, biocompatibility, plaque resistance, and color stability.
- CAD/CAM fabrication of Mondial denture teeth ensures harmonious tooth set-up and reproducible articulation.
- Mondial teeth enable accurate intercuspal relationships, excellent anatomical shape, and physiological function.
Historically, most dentists accepted denture esthetics as less than ideal and incapable of appearing as lifelike as fixed esthetic dentistry. As part of the general practice, denture design and tooth mold selection often were delegated to the laboratory technician. Removable dentures typically were considered necessary for patients who, for the most part, became edentulous through neglect—periodontal disease and rampant caries resulted from the neglect, causing tooth loss. However, conditions do rarely occur—such as ectodermal dysplasia (ED)—over which the patient has no control and for which denture prostheses are required.1
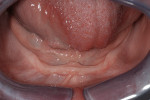
ED is a multifactoral hereditary disorder; its main dental manifestation is hypodontia of varying severity.1,2 Reduced vertical dimension, peg-shaped laterals, and poorly developed alveolar ridges are among the symptoms reported in ED1-3 (Figure 1 and Figure 2). Cosmetic restorative dental treatment is almost always necessary, and children may need dentures at an early age. Multiple denture replacements often are needed throughout development, and dental implants may be an option in adolescence.3-7 Because dental treatment is complex, a multidisciplinary approach is ideal.6
With the continued success of implant dentistry along with patients having increased knowledge about dental esthetics, edentulous or partially edentulous individuals, including those with ED, are desiring superior levels of esthetics and durability in removable and implant-supported prosthetics.8 Manufacturers have responded by introducing denture teeth capable of withstanding implant forces and that also resemble the characteristics of a natural smile.9,10
An adolescent man with ED was treated with implant-supported dentures created using denture teeth made from a highly cross-linked, tough, elastic matrix (NanoPearls, Mondial® Denture Teeth, Heraeus Kulzer, www.heraeus-dental-us.com). These teeth were selected because they demonstrate the life-like opalescence, high abrasion resistance, biocompatibility, plaque resistance, color stability, and strength required for implant-supported dentures.11,12
Case Presentation
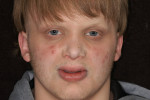
A 17-year-old patient presented with ED that significantly affected his dentition. The mid-portion of the lower third of his face was considerably underdeveloped. The width of the mouth (ie, commissure to commissure) was diminished and characterized by severe lip constriction. This disproportion was partly attributed to edentulism and diminished alveolar process, with the lips continuing to become constricted from no intraoral resistance or support. The upper arch was also edentulous, with diminished alveolar process.
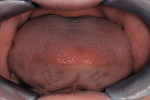
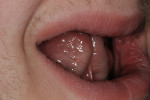
The patient also presented with macroglossia resulting from diminished alveolar growth and dental development, and from using his tongue as the primary means for mastication by pressing food against the palate (Figure 3). Use of his lips in mastication added to their profound constricture (Figure 4).
Treatment Considerations
The challenges that this extreme ED case presented required collaboration among dental specialties. Taking a traditional denture design and retention approach was questionable due to the underdeveloped maxillary and mandibular alveolar processes. Achieving predictable retention necessitated an implant-supported prosthesis; however, no appreciable osseous tissue was available to engage an implant. Complex augmentation procedures were required to enhance the proposed recipient sites. Because the patient never had a functional dentition, occlusion and esthetics also were considerations.
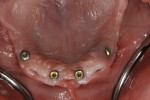
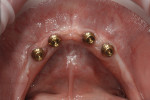
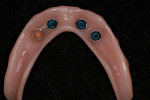
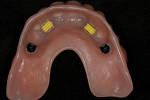
The dental implant surgical procedures were performed in three treatment phases. Initially, four Straumann (www.straumann.us) tissue-level implants were placed in the mandibular arch, followed by the second phase of care, which utilized Regenaform® (RTI Biologics, Inc., www.rtix.com) to augment the maxilla for increased buccal-lingual width and, 6 months later, the placement of four Straumann bone-level dental implants (Figure 5 and Figure 6).
Esthetic and Functional Denture Design
Proper harmony and balance between a person’s smile and facial design incorporates tooth size, shape, shade, and position, as well as the visual impact that their inter-relationship has on the patient’s appearance. The nanofillers in the selected Mondial denture teeth create life-like optical characteristics, such as depth, vital color, and natural light dynamics. The labial, buccal, and occlusal surfaces enhance esthetics, and the tooth layers match the Vitapan Classical shade system (Vident, www.vident.com) and improve opalescence.
Because the patient had never had teeth, a computer-generated cosmetic image (Envision A Smile, www.envisionasmile.com) served as an anatomically correct visual reference to determine what could be accomplished (Figure 7 and Figure 8). Once established, traditional removable denture design methods were implemented.
Maxillary and mandibular arch impressions were taken, and a starting vertical dimension was determined by taking a jaw relation and using a position marked on the patient’s nose and chin.13 Additionally, proper tooth molds were selected based on the patient’s extraoral features and the computer-generated images.
The Mondial denture teeth molds selected for this case are based on the Magister/Orthognath molds used successfully worldwide for 40 years. With CAD/CAM technology, sets of teeth can be created with the identical shape for all tooth sizes. There also are no frictional surfaces that resist function, so accuracy is ensured.
This information was sent to the laboratory, where the impressions were boxed and poured, trimmed appropriately, and stabilized record bases with wax rims were fabricated. The record bases and wax rims were tried-in to ensure proper fit and comfort.14,15 Necessary adjustments were made, and a bite registration material was applied between the indexed wax rims. The properly oriented casts were returned to the laboratory for setting the teeth.
CAD/CAM fabrication of the Mondial denture teeth ensures harmonious tooth set-up and reproducible articulation for precisely defined centric relationships and improved function. Overall, Mondial teeth enable accurate intercuspal relationships, superior anatomical shape, and physiological function.
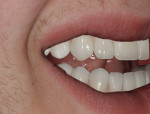
The casts were mounted on an articulator, and the six anterior upper and lower teeth were set in the wax rims and returned to the office for try-in and esthetic and functional evaluation (Figure 9). Close attention was given to the revealing of tooth length during animated gestures, as well as in the repose position. The incisal edge was placed in the ideal position, just touching the inner vermillion border of the lower lip. Esthetic guidelines were followed as they would be for upper/lower veneer smile design cases.
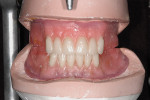
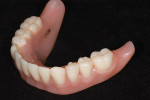
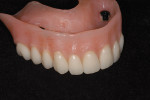
Once approved, the laboratory added the upper and lower posterior teeth for try-in, after which the overdentures were processed on the final cast and returned for delivery (Figure 10, Figure 11, Figure 12, Figure 13 and Figure 14).
Conclusion
Ectodermal dysplasia dramatically impacted this patient’s facial esthetics and oral function. When he presented, his motivation for treatment was esthetics, a challenging proposition considering no reference point existed from which to begin. Creating a perspective from which he and the dental team could consider the esthetic possibilities first required a proper and sound functional scheme as the basis for an implant-supported prosthesis created using Mondial denture teeth (Figure 15). Ultimately, all parameters for treating the case successfully were addressed, although questions remain given the nature of ED.
Disclosure
Dr. Kirtley has received an honorarium from Heraeus Kulzer, LLC.
References
1. Bidra AS, Martin JW, Feldman E. Complete denture prosthodontics in children with ectodermal dysplasia: review of principles and techniques. Compend Contin Educ Dent. 2010;31(6):426-433.
2. Ziada H, Holland T. Ectodermal dysplasia: a case report. J Ir Dent Assoc. 1997;43(4):127-129.
3. Becktor KB, Becktor JP, Keller EE. Growth analysis of a patient with ectodermal dysplasia treated with endosseous implants: a case report. Int J Oral Maxillofac Implants. 2001;16(6):864-874.
4. Oczakir C, Balmer S, Mericske-Stern R. Implant-prosthodontic treatment for special care patients: a case series study. Int J Prosthodont. 2005;18(5):383-389.
5. Kramer FJ, Baethge C, Tschernitschek H. Implants in children with ectodermal dysplasia: a case report and literature review. Clin Oral Implants Res. 2007;18(1):140-146.
6. Bergendal T, Eckerdal O, Hallonsten AL, et al. Osseointegrated implants in the oral habilitation of a boy with ectodermal dysplasia: a case report. Int Dent J. 1991;41(3):149-156.
7. Sweeney IP, Ferguson JW, Heggie AA, Lucas JO. Treatment outcomes for adolescent ectodermal dysplasia patients treated with dental implants. Int J Paediatr Dent. 2005;15(4):241-248.
8. DiMatteo A. Dentures & implants: bringing them together for a winning combination. Inside Dentistry. 2009;5(1):96-104.
9. Henry K. Q&A on the future of implants. Dent Equip Mater. September/October 2006.
10. Rossein KD. Alternative treatment plans: implant-supported mandibular dentures. Inside Dentistry. 2006;2(6):42-43.
11. Hahnel S, Rosentritt M, Bürgers R, Handel G. Adhesion of Streptococcus mutans NCTC 10449 to artificial teeth: an in vitro study. J Prosthet Dent. 2008;100(4):309-315.
12. Assunção WG, Barão VA, Pita MS, Goiato MC. Effect of polymerization methods and thermal cycling on color stability of acrylic resin denture teeth. J Prosthet Dent. 2009;102(6):385-392.
13. Lytle RB. Vertical relation of occlusion by the patient’s neuromuscular perception. J Prosthet Dent. 1964;14(1):12-21.
14. Shor A, Goto Y, Shor K. Mandibular two-implant-retained overdenture: prosthetic design and fabrication protocol. Compend Contin Educ Dent. 2007;28(2):80-88.
15. Vogel R. Clinical technique to simplify overdenture success. Implant Realities. 2006;1:19-20.
About the Author
George E. Kirtley, DDS
Private Practice
Indianapolis, Indiana
Accredited member of both the American Academy of Cosmetic Dentistry and the British Academy of Cosmetic Dentistry