Evaluating Extraction Sockets in the Esthetic Zone for Immediate Implant Placement
Cyril I. Evian, DMD; Jonathan A. Waasdorp, DMD, MS; Maki Ishii, DMD; Martine Mandracchia, DDS; Farshid Sanavi, DMD, PhD; and Edwin S. Rosenberg, DMD
Abstract
With the increasing demands of patients and the profession to maximize esthetic outcomes and minimize the number of procedures, clinicians must consider the use of immediate placement of implants into extraction sockets. Despite atraumatic extraction techniques, many cases present with a non-intact extraction socket, with bone deficiency in the coronal or apical aspect of the socket. In cases of immediate placement, an intact socket and guided bone regeneration procedures are often prerequisites to a successful esthetic outcome. In most cases, these grafting techniques can be performed at the time of immediate placement. Certain cases, however, have undergone such extensive bone and soft-tissue destruction that implants cannot be placed immediately and hard- and/or soft-tissue augmentation is required prior to implant placement. This article describes a classification system that considers both hard- and soft-tissue defects and the morphology of the extraction socket for immediate implant placement. Recommendations are made concerning the surgical technique required to treat the hard- and soft-tissue defects based on the socket morphology.
With the advancement of dental implant knowledge and technology, the protocol for implant placement has evolved significantly from the original Bränemark recommendations. Successful osseointegration and restoration of the dentition has become very predictable, yet challenges remain in many cases. Inadequate bone availability for implant placement and optimal esthetic outcomes are common issues facing clinicians. Numerous animal1 and human2-5 studies document progressive alveolar bone resorption after tooth extraction, with most resorption occurring in the first year. Successful implant therapy still can be attained in a resorbed ridge through a wide range of treatment options, including block grafts, guided bone regeneration, and placement of narrower width or shorter length implants. Scientific evidence has shown success with these treatments;6-12 however, these options can increase expense and treatment time. Immediate placement of implants, when properly planned and executed, can offer many advantages such as the following:13-16
- Reduced treatment time
- Reduced number of procedures
- Preservation of width and height of the alveolar bone
- Soft-tissue preservation
- Achievement of ideal implant location, provided that the extracted tooth has a desirable position and alignment
Although evidence suggests socket preservation may decrease this postextraction resorption,17-19 opinions conflict as to whether alveolar bone can be preserved with immediate implant placement.20-22 In a beagle dog study, Araújo and Lindhe23 showed similar coronoapical bone height is lost between an immediately placed implant and a naturally healed socket. They concluded implant placement cannot prevent the loss of bundle bone because of its lack of blood supply. In a human study, Covani et al24 compared changes in buccolingual ridge width of immediate and delayed implants at the time of placement and second-stage surgery. On average, 1.07 mm more width was maintained by immediate placement rather than delayed (6 to 8 weeks). A systematic review demonstrated similar survival to delayed implants, with the advantages of possible preservation of alveolar bone, increased patient satisfaction, and improved esthetics;14 more research is required in this area.
A controversial factor commonly known as the "critical gap" is another issue in immediate implant placement. Although evidence from animal studies25 shows decreased bone-to-implant contact with greater implant-to-socket distance without the use of an osteoconductive matrix, sufficient clinical integration and survival occurs. Although this "critical gap" is usually considered to be an average of 1 mm to 2 mm,25,26 other factors such as the thickness of the buccal plate, surface of the implant,27 and depth of defect28 must be considered. Ultimately, the decision to graft is largely based upon clinical experience, as patients with thick bony biotypes will achieve clinical bone fill of larger gaps without placement of graft materials. When larger defects are present at the time of immediate placement, successful simultaneous guided bone regenerative techniques using various graft materials and membranes have been documented.29,30 In addition, success with simultaneous soft-tissue grafting to increase biotype thickness and improve esthetics has been shown.31,32
Clinical reports have demonstrated improved esthetic results can be attained when the architecture of the soft tissue and extraction socket is maintained.33 Methodology includes avoiding disruption of the marginal tissue and using a gingival healing device to support the soft tissue at the time of immediate placement. Marginal tissue integrity can be maintained during the procedure by flapless surgery or an apical access incision.34 Gingival healing devices include healing abutments, custom healing abutments, or provisional restorations. These devices are placed on the implant during immediate placement.
To aid the practitioner in diagnosis and preoperative treatment planning, several classifications of extraction sockets have been published by Salama and Salama,35 Caplanis et al,36 and Elian et al.12 The Salama classification separates sockets by degree of defect severity, while Elian describes a combination of hard- and soft-tissue defects. This article describes a classification system, through case reports, that considers both the hard- and soft-tissue status and the morphology of the extraction socket for purposes of immediate implant placement. Recommendations are made concerning the surgical technique required for each type of socket classification along with clinical examples. This will assist with surgical treatment planning for immediate dental implant placement.
Classification of Extraction Sockets for Immediate Implant Placement
When possible, tooth extraction should be performed atraumatically without facial flap elevation. If papilla reflection or vertical-releasing incisions are used, the same principles are followed. After tooth extraction, the hard and soft tissues of the bony socket are evaluated. A small curette or probe is used to determine its bony integrity. Based on the hard- and soft-tissue topography, extraction sockets can be classified as follows:
- Type I: The bony socket is intact, and the soft-tissue form is undisturbed.
- Type II: The bony socket is intact in the coronal aspect of the socket, but a fenestration is present in the apical area. The soft tissue remains intact and undisturbed.
- Type III: Bone loss is present in the coronal aspect of the socket. The soft tissue remains intact and undisturbed.
- Type IV: Bony defects exist in conjunction with soft-tissue deformity. Often, the severity of this defect precludes implant placement.
Recommended surgical and prosthetic approaches to treat the above situations with immediately placed implants are as follows.
Type I
Immediate dental implant placement without incisions or flaps is recommended. The healing abutment or soft-tissue retention device should be fitted at the time of implant placement. This does not mean the implant is immediately loaded or temporized, yet evidence suggests this is a viable treatment option.37,38 The healing abutment may be positioned at or just above the gingival margin.
Type II
No incision or flap should be used in the coronal aspect of the gingival site. Immediate implant placement is performed; the healing device is used to retain the gingival form. An apicoectomy approach is employed to repair the apical bony defect.34
Type III
Coronal full-thickness incisions at the gingival margin and flaps are required to repair the bony defect via bone regeneration techniques. A soft-tissue retention device may be used to help retain the soft-tissue form at the time of immediate placement. Pre-implant orthodontic extrusion may be considered prior to extraction and immediate placement.
Type IV
If the clinician deems it appropriate to immediately place an implant after extraction, incisions and flaps are necessary because soft and hard tissues require repair. Bone augmentation is necessary at the time of implant placement. Soft-tissue augmentation, such as a subepithelial connective tissue graft, may be performed during implant placement or at a later date (ie, Stage II).
Additional Considerations
Considerations also include orthodontic extrusion or soft-tissue augmentation prior to the implant procedure, if applicable. The gingival soft-tissue retention device is generally not used at this time but may be considered. If the surgeon is unable to attain primary stability, implant placement is delayed until the site has adequately healed. If at any stage of the aforementioned conditions primary stability cannot be achieved, site preservation/development for future implant placement is necessary.
Case Reports
The preoperative treatment in all of the following cases included thorough medical, dental, and periodontal evaluations. All medical needs, including diabetic and hypertensive control, were addressed prior to surgical intervention. None of the patients in these cases smoked. Dental and implant therapy was performed according to accepted professional protocol. Patients were given an antibiotic regimen 2 days prior to the surgical implant procedure, and they continued this regimen for 5 days postoperatively. All patients rinsed with chlorhexidine 0.12% for 1 minute prior to surgery. The surgical procedures were performed under local anesthesia, and all patients received an analgesic for 5 to 7 days postoperatively and were supervised at 1 week, 1 month, and periodically until the final prosthesis was constructed.
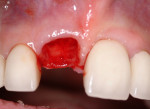
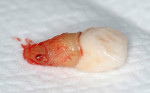
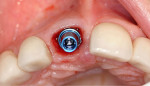
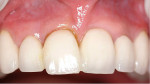
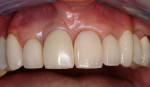
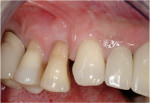
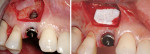
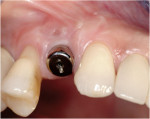
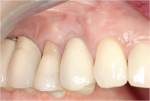
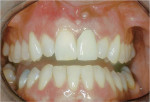
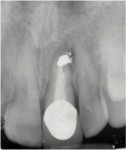
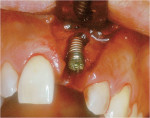
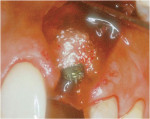
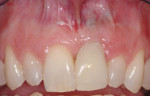
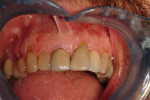
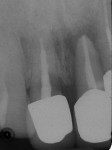
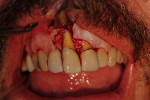
These cases illustrate the decision-making process for the surgical technique during immediate dental implant placement, depending on the socket morphology classification. Case 1 demonstrates a Type I socket morphology in which the bony socket is intact and the soft-tissue form is undisturbed (Figure 1, Figure 2, Figure 3, Figure 4, Figure 5, Figure 6 and Figure 7). Case 2 illustrates a Type II socket in which the bony socket is intact in the coronal aspect of the socket but fenestration is present in the apical area (Figure 8, Figure 9, Figure 10 and Figure 11). Case 3 was classified as a Type III socket. This type of case has bone loss in the coronal aspect of the socket (, Figure 12, Figure 13, Figure 14, Figure 15, Figure 16 and through Figure 17). The soft tissue remains intact and undisturbed. In Case 4, a Type IV socket is a combination of bone and soft-tissue defect (Figure 18, Figure 19 and Figure 20).
Discussion
It is imperative for the clinician to determine the prognosis of an immediate-implant–placement case and warn the patient that implant placement may not be possible if pre-implant grafting is necessary for predictable success. Minimal trauma to the bone and soft tissue must be exercised during extraction. Careful evaluation of the socket after extraction and osteotomy preparation should be performed to determine the bone's integrity. This is especially important in the apical region where fenestration of the bone is common. Failure to recognize this can lead to retrograde peri-implantitis. The bone level must be determined in relation to the soft-tissue height. The implant should be placed at the bone level or below the bone crest. With the advent of wider, tapered implants, the gap between the implant and socket can be minimized. Implants should be placed toward the palatal aspect of the socket to minimize encroachment of the implant and subgingival device on the facial tissues. The device must not cause distention of the soft tissues, as recession will occur. The soft-tissue retention device in the form of a healing cap, abutment, or provisional abutment should be fitted onto the implant to mimic the supraosseous root form. A provisional restoration may be used as part of the soft-tissue retention device. The implant may or may not be loaded, depending on whether the clinician deems it appropriate.
Conclusion
When the clinician considers immediate placement of an implant in an extraction socket to be appropriate, careful evaluation of the hard- and soft-tissue integrity must be made. Each extraction socket type as described in the classification system presented in this article requires different surgical techniques. Pre- and post-implant therapy, such as orthodontic extrusion or soft-tissue augmentation, also may be considered for successful integration and esthetic outcome of the case. The use of a gingival retention device is critical to maintain the form of the soft tissue and should be used with discretion whenever possible.
References
1. Araújo MG, Sukekava F, Wennström JL, Lindhe J. Tissue modeling following implant placement in fresh extraction sockets. Clin Oral Implants Res. 2006;17(6):615-624.
2. Pietrokovski J, Massler M. Alveolar ridge resorption following tooth extraction. J Prosthet Dent. 1967;17(1):21-27.
3. Atwood DA. Bone loss of edentulous alveolar ridges. J Periodontol. 1979;50(4 spec no):11-21.
4. Carlsson GE, Persson G. Morphologic changes of the mandible after total extraction and wearing of dentures. Sven Tandlak Tidskr. 1970;63(3):219-232.
5. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent. 2003;23(4):313-323.
6. von Arx T, Buser D. Horizontal ridge augmentation using autogenous block grafts and the guided bone regeneration technique with collagen membranes: a clinical study with 42 patients. Clin Oral Implants Res. 2006;17(4):359-366.
7. Pikos MA. Block autografts for localized ridge augmentation: Part I. The posterior maxilla. Implant Dent. 1999;8(3):279-285.
8. das Neves FD, Fones D, Bernardes SR, et al. Short implants—an analysis of longitudinal studies. Int J Oral Maxillofac Implants. 2006;21(1):86-93.
9. Buser D, Dula K, Hess D, et al. Localized ridge augmentation with autografts and barrier membranes. Periodontol 2000. 1999;19:151-163.
10. Buser D, Dula K, Lang NP, Nyman S. Long-term stability of osseointegrated implants in bone regenerated with the membrane technique. 5-year results of a prospective study with 12 implants. Clin Oral Implants Res. 1996;7(2):175-183.
11. Shatkin TE, Shatkin S, Oppenheimer BD, Oppenheimer AJ. Mini dental implants for long-term fixed and removable prosthetics: a retrospective analysis of 2514 implants placed over a five-year period. Compend Contin Educ Dent. 2007;28(2):92-101.
12. Elian N, Cho SC, Froum S, et al. A simplified socket classification and repair technique. Pract Proced Aesthet Dent. 2007;19(2):99-106.
13. Chen ST, Wilson TG Jr, Hammerle CH. Immediate or early placement of implants following tooth extraction: review of biologic basis, clinical procedures, and outcomes. Int J Oral Maxillofac Implants. 2004;19(suppl):12-25.
14. Esposito MA, Koukoulopoulou A, Coulthard P, Worthington HV. Interventions for replacing missing teeth: dental implants in fresh extraction sockets (immediate, immediate-delayed and delayed implants). Cochrane Database Syst Rev. 2006;(4):CD005968.
15. Schwartz-Arad D, Laviv A, Levin L. Survival of immediately provisionalized dental implants placed immediately into fresh extraction sockets. J Periodontol. 2007;78(2):219-223.
16. Schwartz-Arad D, Yaniv Y, Levin L, Kaffe I. A radiographic evaluation of cervical bone loss associated with immediate and delayed implants placed for fixed restorations in edentulous jaws. J Periodontol. 2004;75(5):652-657.
17. Irinakis T, Tabesh M. Preserving the socket dimensions with bone grafting in single sites: an esthetic surgical approach when planning delayed implant placement. J Oral Implantol. 2007;33(3):156-163.
18. Araújo MG, Lindhe J. Ridge preservation with the use of Bio-Oss collagen: a 6-month study in the dog. Clin Oral Implants Res. 2009;20(5):433-440.
19. Nevins M, Camelo M, De Paoli S, et al. A study of the fate of the buccal wall of extraction sockets of teeth with prominent roots. Int J Periodontics Restorative Dent. 2006;26(1):19-29.
20. Froum SJ. Immediate placement of implants into extraction sockets: rationale, outcomes, technique. Alpha Omegan. 2005;98(2):20-35.
21. Paolantonio M, Dolci M, Scarano A, et al. Immediate implantation in fresh extraction sockets. A controlled clinical and histological study in man. J Periodontol. 2001;72(11):1560-1571.
22. Botticelli D, Berglundh T, Lindhe J. Hard-tissue alterations following immediate implant placement in extraction sites. J Clin Periodontol. 2004;31(10):820-828.
23. Araújo MG, Sukekava F, Wennström JL, Lindhe J. Ridge alterations following implant placement in fresh extraction sockets: an experimental study in the dog. J Clin Periodontol. 2005;32(6):645-652.
24. Covani U, Bortolaia C, Barone A, Sbordone L. Bucco-lingual crestal bone changes after immediate and delayed implant placement. J Periodontol. 2004;75(12):1605-1612.
25. Akimoto K, Becker W, Persson R, et al. Evaluation of titanium implants placed into simulated extraction sockets: a study in dogs. Int J Oral Maxillofac Implants. 1999;14(3):351-360.
26. Botticelli D, Berglundh T, Buser D, Lindhe J. The jumping distance revisited: An experimental study in the dog. Clin Oral Implants Res. 2003;14(1):35-42.
27. Persson LG, Berglundh T, Lindhe J, Sennerby L. Re-osseointegration after treatment of peri-implantitis at different implant surfaces. An experimental study in the dog. Clin Oral Implants Res. 2001;12(6):595-603.
28. Yoon HC, Choi JY, Jung UW, et al. Effects of different depths of gap on healing of surgically created coronal defects around implants in dogs: a pilot study. J Periodontol. 2008;79(2):355-361.
29. Covani U, Cornelini R, Barone A. Buccal bone augmentation around immediate implants with and without flap elevation: a modified approach. Int J Oral Maxillofac Implants. 2008;23(5):841-846.
30. Fugazzotto PA, Shanaman R, Manos T, Shectman R. Guided bone regeneration around titanium implants: report of the treatment of 1,503 sites with clinical reentries. Int J Periodontics Restorative Dent. 1997;17(3):292-299.
31. Bianchi AE, Sanfilippo F. Single-tooth replacement by immediate implant and connective tissue graft: a 1-9-year clinical evaluation. Clin Oral Implants Res. 2004;15(3):269-277.
32. Fowler EB, Breault LG, Rebitski G. Ridge preservation utilizing an acellular dermal allograft and demineralized freeze-dried bone allograft: Part II. Immediate endosseous implant placement. J Periodontol. 2000;71(8):1360-1364.
33. Wheeler SL, Vogel RE, Casellini R. Tissue preservation and maintenance of optimum esthetics: a clinical report. Int J Oral Maxillofac Implants. 2000;15(2):265-271.
34. Evian CI, Al-Momani A, Rosenberg ES, Sanavi F. Therapeutic management for immediate implant placement in sites with periapical deficiencies where coronal bone is present: technique and case report. Int J Oral Maxillofac Implants. 2006;21(3):476-480.
35. Salama H, Salama M. The role of orthodontic extrusive remodeling in the enhancement of soft and hard tissue profiles prior to implant placement: a systematic approach to the management of extraction site defects. Int J Periodontics Restorative Dent. 1993;13(4):312-333.
36. Caplanis N, Lozada JL, Kan JY. Extraction defect assessment, classification, and management. J Calif Dent Assoc. 2005;33(11):853-863.
37. Avvanzo P, Ciavarella D, Avvanzo A, et al. Immediate placement and temporization of implants: three- to five-year retrospective results. J Oral Implantol. 2009;35(3):136-142.
38. Crespi R, Capparé P, Gherlone E, Romanos GE. Immediate versus delayed loading of dental implants placed in fresh extraction sockets in the maxillary esthetic zone: a clinical comparative study. Int J Oral Maxillofac Implants. 2008;23(4):753-758.
About the Authors
Cyril I. Evian, DMD Clinical Professor, University of Maryland
College Park, Maryland
Clinical Associate Professor
New York University
New York, New York
Jonathan A. Waasdorp, DMD, MS Private Practice
King of Prussia, Pennsylvania
Maki Ishii, DMD Private Practice
Elkins Park, Pennsylvania
Martine Mandracchia, DDS Clinical Associate Professor
New York University
New York, New York
Farshid Sanavi, DMD, PhD Private Practice
Elkins Park, Pennsylvania
Edwin S. Rosenberg, DMD Clinical Associate Professor
New York University
New York, New York