Dental Root Resorption: A Review of the Literature and a Proposed New Classification
Robert J. Kanas, DDS; and Scott J. Kanas
Abstract
Objective This article reviews the dental literature pertaining to dental root resorption and proposes a classification system designed to facilitate communication of precise information for each type.
Design: A systematic review of the literature using PubMed was performed and supplemented with manual reviews of bibliographies from textbooks.
Results: A classification system was developed using etiology and morphologic characteristics of dental root resorption. Various types of dental root resorption were identified. The different forms were organized into dental and non-dental origins and further divided between internal and external resorption along etiologic and morphologic characteristics.
Conclusions: The classification of dental root resorption proposed may assist dentists in the formulation of a differential diagnosis and management of root resorption.
Root resorption in deciduous teeth is a normal physiologic response, resulting in exfoliation of the deciduous teeth with replacement by the permanent dentition. However, the process of root resorption in the permanent dentition has a pathologic basis. Types of root resorption in permanent teeth may be broadly classified into internal and external resorption. Internal eruption has its origins in the dental pulp whereas external resorption begins in the periodontal ligament (PDL). Internal resorption is relatively rare and occurs as a result of trauma or caries-related inflammation of the pulp. External root resorption has various causes, including: 1) infective/inflammatory conditions; 2) traumatic injuries; 3) pressure/mechanical stimulation; 4) neoplastic conditions; 5) systemic disorders; and 6) idiopathic.1,2 Various classification systems of root resorption have been proposed.1,3-6 These systems have used different terms and categories to describe dental root resorption. This article reviews the dental literature pertaining to dental root resorption and introduces a classification system that can communicate precise clinical information to the treating dentist. The article will clarify some of the terminology that previous systems have used.
Past Classification Schemes
A PubMed search combined with manual searches of bibliographies from textbooks was performed. The identified articles were not subjected to any definitive data analyses or meta-analysis. Table 1, Table 2, Table 3, Table 4 and Table 5 present known classification schemes that have been referenced in the past 40 years.1,3-6 Despite changes in terminology and the addition and deletion of some entities from one system to the next, each one has commonalities.
Classification of root resorption involves the categorization of different types on the basis of designated morphologic characteristics, as well as etiologic factors, for predicting potential biologic behavior so that appropriate treatment may be delivered. Unlike most disease processes that have a specific principal pathologic basis that make them identifiable, root resorption represents a radiographic sign of varied disease processes. Therefore, root resorption is a pathologic indicator of an underlying process rather than a specific disease entity.
Table 6 depicts the proposed classification system described in this article. The authors refer to it as "The Etiologic and Morphologic Basis of Root Resorption in Permanent Teeth." It broadly classifies root resorption into either dental or non-dental origins and then further into internal or external resorption. Unlike previous classification systems, this new version separates dental-related root resorption from those that have medical-associated origins. Furthermore, trauma-related root resorption, pressure root resorption, and idiopathic root resorption are further subdivided along etiologic and morphologic characteristics to assist clinicians in deciding the appropriate treatment options. Like most other classification systems, this system will be modified as a better understanding of how the biology of the pulpal and periodontal ligament cells interacts with osseous cellular structures and functions. Terminology in the new version varies somewhat from previous classification systems. The terms external surface resorption and transient apical resorption denote normal physiologic root responses of permanent teeth. The authors prefer the term physiologic apical resorption. It is not to be confused with transient apical breakdown (TAB), which represents an early stage of apical external resorption associated with trauma or pressure from orthodontics to the teeth.
A distinct pattern of external resorption, periapical replacement resorption (PARR) is characterized by replacement of the resorbing root with normal-appearing trabeculated bone.7 This process has also been referred to as apical replacement resorption or external apical replacement resorption. The authors prefer the term PARR.
Unlike PARR, other pathologic entities causing root resorption destroy both bone and tooth, causing cavitation.8 The ability of a disease entity to resorb bone may also lend itself to tooth resorption. Root resorption does not necessarily denote an aggressive pathologic process but rather suggests a destructive process capable of resorbing bone and tooth. Nevertheless, some aggressive disease processes, such as osteosarcoma and chondrosarcoma, cause root resorption.
Root Resorption from Dental Origins—Internal Resorption
Infective/Inflammatory/Trauma
Internal resorption is less common than external; however, it is related to either trauma or caries with bacterial extension to the pulp. Although two distinct morphologic patterns have been described, both share common etiologic factors and, therefore, are thought to originate from similar pathogenesis with different morphologic characteristics.
Radial pulp enlargement resorption—Previous terms include inflammatory internal resorption, intraradicular resorption, or pink tooth of Mummery.9 In this form, the resorbed dentin is replaced by granulation tissue and appears as an intrapulpal radiolucency.
Chronic inflammation of the dental pulp either from trauma, bacteria entering the pulpal tissue from dentinal tubules, or cracks in the cervical root is the suggested causal factor.10,11 Infrequently, internal resorption has been associated with orthodontic or periodontal therapies. It may occur anywhere along the root canal system but is more common in the cervical region of the pulp chamber.
Internal resorption is active only in teeth where part of the pulp remains vital.6 Therefore, pulp tests may be variable, either exhibiting a positive pulp test if the coronal pulp is vital while the apical pulp becomes necrotic, or a nonresponsive pulp test if the coronal pulp becomes necrotic while the apical pulp is vital. When extensive coronal resorption occurs, the crown may be pink and is referred to as the pink tooth of Mummery.
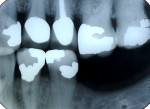
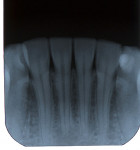
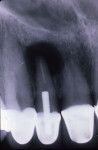
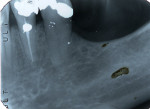
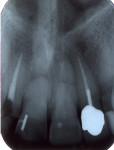
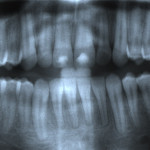
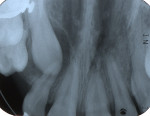
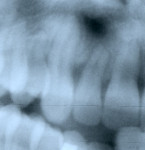
Radial pulp enlargement internal resorption is usually asymptomatic and discovered through a routine radiographic examination. The original tapered outline of the canal is lost, and a symmetrical, well-defined, balloon-like radiolucency within the dilated root canal is observed10 (Figure 1). If the resorption becomes progressive, it will eventually perforate the lateral root surface and may appear similar to external cervical resorption. However, this clinical dilemma may be resolved with the following approach. First, internal root resorption appears as a well-defined radiolucency of the root canal space in contrast to an ill-defined radiolucency of the canal space in external cervical resorption (Figure 2 and Figure 3). Secondly, the mesial-buccal-distal (MBD) rule may be employed whereby two radiographs are taken—one perpendicular to the root and the other at a mesial angle.12 Internal resorption lesions will not shift no matter how severe an angle at which the radiograph is taken, whereas external cervical resorption will shift from its superimposed position over the root canal space and usually extend to the root surface (Figure 2 and Figure 3).
Conventional root canal therapy should be instituted as soon as the diagnosis of internal resorption has been established.5 Delay or failure to treat this type of resorption may lead to eventual extension to the PDL. To correct the perforation, this would require an additional surgery, such as crown lengthening or root extrusion with orthodontic appliances.5
Metaplastic (replacement) pulp resorption—Previous terms include root canal replacement resorption and metaplastic resorption. The etiology, clinical features, and treatment options for metaplastic internal resorption are equivalent to radial pulp enlargement resorption. The distinguishing feature of this type of internal resorption is partial replacement of the enlarged root canal space with radiopaque material, giving the appearance of partial canal obliteration.6 The radiodense material appears less dense than the surrounding dentin, and the internal resorption looks less defined than that observed in radial pulp enlargement resorption. Histologic studies of internal resorption demonstrate replacement of normal pulp tissue by a periodontal-like connective tissue with both osteogenic and resorptive potential.13
External Resorption
Physiologic apical resorption—External surface resorption, transient apical resorption, and transient root resorption are terms previously used to describe normal physiologic response of the root surface to physiologic stimuli of the masticatory system, such as chewing pressure and muscle forces on the teeth.6,14,15 It is found in most teeth, is part of the repair process to the cementum and PDL space, is self-limiting, and is normally not detected clinically or radiographically.16,17 It must be distinguished from transient apical breakdown (TAB), which is usually associated with a history of trauma or orthodontic therapy.18
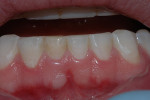
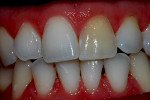
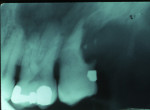
No significant clinical signs are detectable. Pulp vitality tests should be responsive. A history of trauma or color change in a tooth or teeth should signal the possibility of TAB (Figure 4 and Figure 5). This is usually not visible on radiographs because of its small size. Use of radiographic magnification may aid in identifying this type of resorption in most teeth.17 It is characterized by small saucer-shaped excavations at the apices or along the lateral surface of the roots. When observed at the apex of teeth, the problem must be distinguished from TAB or apical inflammatory external resorption. No treatment is indicated because the process is self-limiting.
Infective/inflammatory resorption—Apical inflammatory resorption originates from a necrotic pulp with periapical periodontitis, whereas cervical inflammatory resorption has been associated with bacterial extension into the PDL near the cervical one third of the root.1,6
Apical (pulp) inflammatory resorption—The terms external inflammatory root resorption, inflammatory resorption, periapical inflammation resorption, and apical inflammatory resorption are used to describe this common form of external resorption.1,6,19 Most teeth with apical periodontitis or apical cyst will exhibit some degree of external resorption at the apex of the involved tooth.20
Apical inflammatory resorption results from either caries extending to the pulp, traumatic intrusive luxation, or avulsion with re-implantation resulting in necrosis of the root canal system and development of periapical periodontitis/cyst.2
The process is normally asymptomatic, and the apical periodontitis is normally of long duration. Pulp tests should be nonresponsive, and the affected tooth may exhibit pain on percussion. A draining fistula may be observed near the adjacent tooth. Previous conventional root canal therapy may have been performed on some teeth without resolution of the external resorption. Extensive resorption may lead to mobility of the affected tooth or teeth.
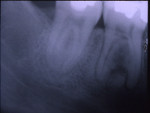
Radiographically, the PDL space widens and loss of the surrounding lamina dura occurs. The apical root surface becomes irregular and ragged at either the mesial or distal surfaces. As the apical periodontitis becomes more progressive, the apical root resorption becomes extensive, causing shortening of the apical one third of the involved root or roots (Figure 6 and Figure 7)
The source of the inflammation must be identified and, if possible, removed. Conventional root canal therapy with intracanal canal calcium hydroxide dressings and apical radicular surgery to remove the inflammation and restore the open apex are accepted treatment protocols.21 In some cases, the apical external resorption may not resolve and the tooth may need to be extracted.22
Cervical (periodontal) inflammatory resorption—Invasive cervical resorption, extracanal invasive resorption, cervical root resorption, and cervical inflammatory resorption are terms used to describe this form of external resorption.23-27 Although the exact etiology has not been established, the authors grouped this condition with inflammatory resorptive conditions. Cervical lesions may develop above the crestal bone (supraosseous) or below the crestal bone (intraosseous).26
Factors implicated in cervical inflammatory resorption include bacteria from periodontal disease, periodontal treatment, trauma, intracoronal bleaching, orthodontics, bruxism, developmental tooth defects, or idiopathic causes.23-30 The exact pathogenesis is not known. However, the process originates in the periodontium or PDL in contrast to apical inflammatory resorption, which originates in a necrotic pulp.
The problem is usually asymptomatic and discovered on routine radiographs. The process may appear similar to tooth decay, especially in a supraosseous position in the root. The teeth usually are responsive to pulp tests unless the process begins to involve the pulp.
Cervical inflammatory resorption appears as a moth-eaten, irregular radiolucency superimposed over a root canal in the cervical one third with extension to the surface or PDL (Figure 2 and Figure 3) The lesion may be supraosseous or intraosseous.26 Additional radiographs should be taken at different angles using the MBD rule to differentiate it from internal root resorption, as discussed previously12.
The extent of the resorption and accessibility to instrumentation must be identified. Supraosseous lesions may be removed with a large slow-speed round bur with application of trichloracetic acid to the root surface and restored with glass ionomer cement or amalgam without a surgical flap procedure.31 Intraosseous lesions require a surgical flap procedure to access the lesion or forced eruption with orthodontic appliances prior to restoration (Figure 8). Restoration is performed similarly to that of supraosseous lesions (Figure 9). Conventional root canal therapy may be required if the resorption extends near or to the pulpal tissues.
Trauma (avulsed/luxated/fracture)—The most common cause of external resorption is trauma to a tooth. Depending on the type of injury, severity of the injury, and maturity of the root and pulp, different types of external root resorption may be observed.18,32
TAB—Transient apical breakdown (TAB) is a temporary process in which the apex of a tooth displays radiographic evidence of resorption.18 However, the injured periapical root and bone returns to a normal state following repair, which may take up to 1 year after the traumatic event. Yet this process may invariably be followed by mild apical resorption with apical pulp obliteration.18
TAB is related to the type of injury and stage of root development. It usually results from moderate injuries to a tooth from extrusion or lateral luxation in mature teeth with developed roots and closed apices. It is rare after a slight injury and absent after a severe injury (intrusive luxation).18 TAB may be observed during orthodontic treatment or occlusal trauma.
The affected tooth may undergo some color change and have varied results from pulp tests (Figure 4). The color change and pulp tests usually return to normal after 1 year. TAB is distinguished from apical physiologic resorption by history, color change, and pulp vitality tests.
Initially, widening of the apical PDL space is observed radiographically and may be followed by apical surface resorption and blunting of the apex (Figure 5). Pulp obliteration mainly in the apical root may ensue.18 Conversely, after widening of the PDL space, the TAB may return to normal with little evidence of root resorption and changes in the PDL space.33,34
TAB is important to identify because no definitive treatment except periodic recall is necessary.
Periapical replacement resorption (PARR) with ankylosis—Apical replacement resorption, external replacement resorption, and replacement resorption with ankylosis are previous terms used.2,6,7,33
PARR with ankylosis is a common sequella from severe trauma to a tooth, such as intrusive luxation or avulsion with re-implantation. Immature root and pulp formation is a risk factor to the development of this type of resorption.18,33 This is a continuous process whereby the tooth is gradually resorbed and replaced by bone as a result of severe damage or loss of the PDL. In avulsion, damage and drying of the PDL is thought to be the origins of this type of resorption.35 PARR without ankylosis may be observed in orthodontic treated teeth or appear less often as idiopathic apical external resorption.
A history of severe trauma will be elicited from the patient to the involved tooth that will usually demonstrate color change (Figure 10 through Figure 12). Pulp tests will be nonresponsive. In many cases, conventional root canal therapy may have been performed. The teeth are usually asymptomatic.
PARR with ankylosis is characterized by shortening of the apical portion of the root with replacement by normal-appearing trabeculated bone (Figure 10 and Figure 11).2,7 The apical root becomes blunted but maintains a relatively smooth contour. The entire root canal system is obliterated, and the PDL space is obscured or lacking. Infrequently, horizontal root fractures may be observed in the involved tooth or adjacent teeth (Figure 10).
It is important to recognize PARR with ankylosis because the prognosis is questionable. There is little definitive treatment. At the time of avulsion, the tooth must be transported in a proper medium, such as Hank's Balanced Salt Solution, to prevent drying and damage to the PDL before re-implantation.36 This process usually progresses until significant loss of the root structure occurs. The teeth may eventually become mobile, making extraction necessary.
Infective/inflammatory resorption—Trauma with resultant pulpal necrosis or damage to the root surface is the most common cause of inflammatory apical or cervical resorption, respectively.2,6,32 Bacteria and their byproducts and breakdown products from the root canal system enter the dentinal tubules of the root, stimulating inflammation in the adjacent periodontal tissues. This leads to progressive external root resorption. Either apical inflammatory resorption or cervical inflammatory resorption may develop. The clinical, radiographic, and treatment options are identical to infective/inflammatory external resorption already discussed.
Pressure resorption—There are three categories of pressure resorption: orthodontic, impacted teeth, and occlusal forces.
Orthodontic: External root resorption associated with orthodontic treatment is frequent and unpredictable. Orthodontic studies demonstrate between 19% and 31% of anterior teeth show some evidence of root resorption.7 Endodontically treated teeth demonstrate no greater resorption than vital teeth when subjected to orthodontic forces.37 The anterior maxillary incisors, especially lateral incisors, were reported to be the most frequently involved teeth, followed by lower incisors and then maxillary premolars. Adults experience more resorption posttreatment than children do. Other risk factors associated with resorption include root morphology, such as dilacerated or pointed roots, or bicuspid extraction therapy with significant overjet correction.38-40 Recently, a genetic predisposition to external apical root resorption in some patients receiving orthodontic treatment has been demonstrated.41,42 Two morphologic types of external root resorption have been identified: TAB and PARR without ankylosis.
TAB is frequently observed during orthodontic treatment and looks similar to trauma-related TAB (Figure 13). However, these changes are transient and eventually disappear posttreatment. Unlike trauma-related TAB, pulp obliteration is not observed. Mild residual apical root resorption may be observed in affected teeth. Clinical history would differentiate between trauma and orthodontic-related TAB. Once identified, no treatment is indicated.
PARR without ankylosis is commonly reported in the literature associated with orthodontic treatment. It looks similar to trauma-related PARR, aside from the development of ankylosis and pulp obliteration7 (Figure 14). The PDL space is usually visible around the entire root surface except for the most apical area, which may be ill-defined. It usually involves the anterior maxillary teeth and lower incisors. Generally, the root loss is not clinically significant unless it occurs prior to treatment in patients with short roots. Pretreatment consultation and informed consent is recommended.
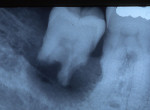
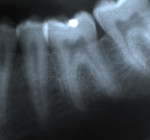
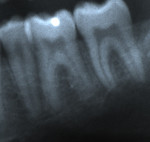
Impacted teeth: The most common sites of impaction-related external resorption are the distal roots of the second molars and apical roots of the maxillary lateral incisors (Figure 15, Figure 16 and Figure 17). Both originate in impacted teeth that necessarily do not resorb themselves; impacted third molars and impacted maxillary cuspids exert pressure against the adjacent roots, respectively.1,2,43-45 Radiographs reveal irregular, scalloped borders to the affected root surface. Often, there is superimposition of the impacted crown over the root surface, and evaluation of the root resorption may be difficult to analyze. To prevent this type of resorption, impacted third molars should be routinely removed and impacted cuspids should be treated orthodontically at an early age. The resorption is irreversible; if the case is severe, extraction of the resorbed tooth may be necessary.
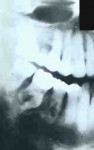
Occlusal forces: Excessive occlusal forces can result in dystrophic changes in the PDL, alveolar bone, and pulp, leading to periapical inflammation, external root resorption, and bone sclerosis.5,46,47 Widening of the PDL space or TAB-like changes may occur.47 The radiopaque thickening of the apical alveolar bone secondary to occlusal forces is termed bone sclerosis. Pulp test findings are variable and inconclusive. The lower molars are frequently involved. Radiographs show dense radiopaque bone at the apex of the affected tooth with mild blunting of the root apex. Sometimes, superimposition of sclerotic bone hinders evaluation of the root resorption. Occlusion-related resorption must be distinguished from condensing osteitis, idiopathic bone sclerosis, and localized idiopathic apical root resorption (Figure 18 and Figure 19). Conventional root canal therapy in teeth exhibiting irreversible pulpitis or pulp necrosis combined with occlusal evaluation is recommended.48
Idiopathic—Idiopathic external root resorption is infrequent and may appear in localized or multiple forms.49 It must be distinguished from systemic diseases that may cause external root resorption. The mechanism is unknown, but other causes of root resorption mentioned in this article have been implicated.
Localized and multiple apical idiopathic resorption have a similar radiographic morphology—PARR without ankylosis—and, therefore, will be discussed together (Figure 18 and Figure 19). The localized form occurs in one to three posterior teeth whereas the multiple form may begin in the molars and bicuspids and eventually involve most of the dentition in a symmetrical pattern.7,49-56 Both forms occur at a young age; however, in the multiple type, the process progresses with age and may lead to the loss of multiple teeth, whereas the localized form appears self-limiting. In both forms, males are reported at a greater frequency than females. Both types are detected on routine radiographs, but the localized form may be more common. Patients sometimes complain of cold sensitivity in the affected teeth. Pulp test findings are responsive. The localized form should be monitored. The multiple form has no definitive treatment, and eventual loss of multiple teeth is likely.
Multiple cervical idiopathic resorption is rare and also must be distinguished from systemic diseases that may cause external resorption. It differs in many ways from the multiple apical form.57-59 The problem occurs in females more often than in males, is progressive, and exhibits multiple moth-eaten cervical cavitations in contrast to PARR in the apical form. Similar treatments are employed as mentioned in the "inflammatory cervical resorption" section; however, the speed and pattern of progression are difficult to predict.
Surgical—Bone grafts of alveolar clefts—In a patient with cleft lip and palate, the standard treatment protocol has been the use of autogenous bone grafting with cancellous iliac bone to the alveolar cleft followed by orthodontic therapy.60,61 External root resorption has been observed as a complication in a small percentage of adjacent teeth receiving the grafts.62 Surgical trauma and drying of the PDL during surgery along with bacterial infection and orthodontic forces are possible etiologic factors. Performing the grafts before the eruption of the cuspids and at an earlier age between 9 and 11 years has shown to reduce the risk of root resorption.
Root Resorption from Non-Dental Origins
Separating root resorption of non-dental origins from that of dental origins is important because the treatment of non-dental types will usually require medical therapy while those of dental origins will necessitate traditional dental therapy.
Internal Resorption
Herpes zoster infection—Herpes zoster is a secondary, reactivation infection caused by the varicella-zoster virus.63 The distribution is usually along the sensory ganglion and epithelial surface innervated by that nerve (dermatome). Herpes zoster may impact the trigeminal nerve, and, consequently, dental structures may be adversely affected. Oral lesions are distributed unilaterally along the side of the infected sensory ganglion. Oral complications may include multiple unilateral mucosal ulcers and a papillovesicular facial skin eruption, osteonecrosis of the jaws, severe periodontitis, tooth exfoliation, and scarring of the facial skin.64,65 Rarely, prodromal odontalgia with pulpitis and devitalization of the teeth has been reported together with both internal and external root resorption.66,67 Herpes zoster infection, therefore, should be considered when unexplained odontalgias and root resorption occur in multiple adjacent teeth on one side of the dental arch.
The pattern of root resorption is usually near the cervical area and involves the pulp with extension to the PDL, which is why this type of resorption is difficult to differentiate between internal and external. The authors included it under "internal resorption" because conventional root canal therapy is indicated in the devitalized pulps of affected teeth. Periodontal flap surgery may be required in cases of cervical root perforation requiring repair. Antiviral medication may be needed to control further outbreaks and postherpetic neuralgia.
External Resorption
Neoplasia and cysts of the jaws—Various odontogenic and non-odontogenic cysts and tumors of the jaws may produce different patterns of external root resorption that are not of dental origins.1-4,7,9,68-70 Differentiating these types of lesions from those originating from dental sources is important for avoiding unnecessary dental therapy or delays in appropriate medical treatments.
A short list of cysts and tumors causing external root resorption includes odontogenic keratocyst, lateral periodontal cyst, ameloblastoma, giant cell reparative granuloma, ossifying fibroma, cementoblastoma, osteoblastoma, osteosarcoma, and chondrosarcoma (Figure 20). Pulp tests of adjacent teeth are usually responsive. However, if the neoplastic process involves the neurovascular bundle supplying the tooth, the pulp test findings may be variable or nonresponsive. If a jaw lesion with associated root resorption is considered to be of neoplastic or cystic origins, a biopsy of the lesion is essential to arrive at a definitive diagnosis to render proper treatment prior to any dental therapy.
Systemic disorders—Although systemic disorders causing root resorption are rare, they should be considered in the differential diagnosis of external root resorption (Figure 21 and Figure 22). Frequently, blood chemistry tests, urine analysis, endocrine/hormone tests, biopsies, and genetic/molecular gene studies may aid in the diagnosis.
Many systemic abnormalities have been implicated. Collectively, they include hormonal imbalances,71 Paget's disease of bone,72,73 hyperparathyroidism,74 Gaucher's disease,7 hypophosphatasia,75 Papillon-Lefèvre syndrome,76 hemifacial atrophy,77 renal and liver diseases,78,79 focal dermal hypoplasia (Goltz syndrome),80 familial expansile osteolysis,81 and osteogenesis imperfecta.82 These diseases should be excluded in cases of multiple idiopathic apical or cervical resorptions.
Conclusion
A systematic review of the dental literature pertaining to dental root resorption was performed, and a classification system based on the etiologic and morphologic features of each type of resorption was proposed. This system should aid the dentist in determining a differential diagnosis when managing dental root resorption.
Acknowledgments
The authors would like to thank the librarians, Marilyn Dow, Beverly Reppart, Jessica Grimes, and Cynthia Mulenga, at the University of Detroit Mercy School of Dentistry for their advice and assistance in retrieving the numerous articles used in this review. The first author would also like to thank Dr. Jerald Jensen and Dr. Al Abrams for their mentorship.
References
1. Bakland LK. Root Resorption. Dent Clin North Am. 1992;36(2):491-507.
2. Fuss Z, Tsesis I, Lin S. Root resorption—diagnosis, classification and treatment choices based on stimulation factors. Dent Traumatol. 2003;19(4):175-182.
3. Pindborg JJ, ed. Pathology of the Dental Hard Tissues. Copenhagen, Denmark: Munksgaard; 1970:338.
4. Shafer WG, Hine JK, Levy BM. A Textbook of Oral Pathology. 4th ed. Philadelphia, PA: WB Saunders; 1983:328-332.
5. Benenati FW. Root resorption: types and treatment. Gen Dent. 1997;45(1):42-45.
6. Ne RF, Witherspoon DE, Gutmann JL. Tooth resorption. Quintessence Int. 1999;30(1):9-25.
7. Bender IB, Byers MR, Mori K. Periapical replacement resorption of permanent, vital, endodontically treated incisors after orthodontic movement: report of two cases. J Endod. 1997;23(12):768-773.
8. Gunraj MN. Dental root resorption. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1999;88(6):647-653.
9. Neville BW, Damm DD, Allen CM, Bouquot J. Oral and Maxillofacial Pathology. 3rd ed. St. Louis, MO: Saunders Elsevier; 2009:65-70.
10. Rabinowitch BZ. Internal resorption. Oral Surg Oral Med Oral Pathol. 1957;10(2):193-206.
11. Walton RE, Leonard LA. Cracked tooth: an etiology for "idiopathic" internal resorption? J Endod. 1986;12(4):167-169.
12. Gartner AH, Mack T, Somerlott RG, Walsh LC. Differential diagnosis of internal and external root resorption. J Endod. 1976;2(11):329-334.
13. Wedenberg C, Zetterqvist L. Internal resorption in human teeth—a histological, scanning electron microscopic, and enzyme histochemical study. J Endod. 1987;13(6):255-259.
14. Trope M. Clinical management of the avulsed tooth. Dent Clin North Am. 1995;39(1):93-111.
15. Heithersay GS. Management of tooth resorption. Aust Dent J. 2007;52(1 suppl):S105-S121.
16. Henry JL, Weinmann JP. The pattern of resorption and repair of human cementum. J Am Dent Assoc. 1951;42(3):270-290.
17. Massler M, Malone AJ. Root resorption in human permanent teeth: a roentographic study. Am J Orthod. 1954;40(8):619-633.
18. Andreasen FM. Transient apical breakdown and its relation to color and sensibility changes after luxation injuries to teeth. Endod Dent Traumatol. 1986;2(1):9-19.
19. Goultschin J, Nitzan D, Azaz B. Root resorption. Review and discussion. Oral Surg Oral Med Oral Pathol. 1982;54(5):586-590.
20. Malueg LA, Wilcox LR, Johnson W. Examination of external apical root resorption with scanning electron microscopy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1996;82(1):89-93.
21. Tronstad L. Recent development in endodontic research. Scand J Dent Res. 1992;100(1):52-59.
22. Nair PN. On the causes of persistent apical periodontitis: a review. Int Endod J. 2006;39(4):249-281.
23. Gulsahi A, Gulsahi K, Ungor M. Invasive cervical resorption: clinical and radiological diagnosis and treatment of 3 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;103(3):e65-e72.
24. Frank AL. Extracanal invasive resorption: an update. Compend Contin Educ Dent. 1995;16(3):250-266.
25. Mock ES, Wolff GK, Galvan DA. Rapidly progressing extracanal invasive resorption. Gen Dent. 1997;45(1):66-67.
26. Benenati FW. Extracanal invasive root resorption: a perplexing oddity. Gen Dent. 2002;50(1):70-71.
27. Bergmans L, Van Cleynenbreugel J, Verbeken E, et al. Cervical external root resorption in vital teeth. J Clin Periodontol. 2002;29(6):580-585.
28. Harrington GW, Natkin E. External resorption associated with bleaching of pulpless teeth. J Endod. 1979;5(11):344-348.
29. Madison S, Walton R. Cervical root resorption following bleaching of endodontically treated teeth. J Endod. 1990;16(12):570-574.
30. Rodriguez-Pato RB. Root resorption in chronic periodontitis: a morphometrical study. J Periodontol. 2004;75(7):1027-1032.
31. Heithersay GS. Treatment of invasive cervical resorption: an analysis of results using topical application of trichloracetic acid, curettage, and restoration. Quintessence Int. 1999;30(2):96-110.
32. Andreasen JO, Bakland LK, Andreasen FM. Traumatic intrusion of permanent teeth. Part 2. A clinical study of the effect of preinjury and injury factors, such as sex, age, stage of root development, tooth location, and extent of injury including number of intruded teeth on 140 intruded permanent teeth. Dent Traumatol. 2006;22(2):90-98.
33. Andreasen FM. Transient root resorption after dental trauma: the clinician's dilemma. J Esthet Restor Dent. 2003;15(2):80-92.
34. Boyd KS. Transient apical breakdown following subluxation injury: a case report. Endod Dent Traumatol. 1995;11(1):37-40.
35. Lindskog S, Pierce AM, Blomlof L, Hammarstrom L. The role of the necrotic periodontal membrane in cementum resorption and ankylosis. Endod Dent Traumatol. 1985;1(3):96-101.
36. Krasner P. Advances in the treatment of avulsed teeth. Dent Today. 2003;22(8):84-87.
37. Mattison GD, Delivanis HP, Delivanis PD, Johns PI. Orthodontic root resorption of vital and endodontically treated teeth. J Endod. 1984;10(8):354-358.
38. Sameshima GT, Sinclair PM. Predicting and preventing root resorption: Part I. Diagnostic factors. Am J Orthod Dentofacial Orthop. 2001;119(5):505-510.
39. Sameshima GT, Sinclair PM. Predicting and preventing root resorption: Part II. Treatment factors. Am J Orthod Dentofacial Orthop. 2001;119(5):511-515.
40. Kaley J, Phillips C. Factors related to root resorption in edgewise practice. Angle Orthod. 1991;61(2):125-132.
41. Al-Qawasmi RA, Hartsfield JK Jr, Everett ET, et al. Genetic predisposition to external apical root resorption. Am J Orthod Dentofacial Orthop. 2003;123(3):242-252.
42. Al-Qawasmi RA, Hartsfield JK Jr, Everett ET, et al. Genetic predisposition to external apical root resorption in orthodontic patients: linkage of chromosome-18 marker. J Dent Res. 2003;82(5):356-360.
43. Henefer EP. Root resorption by an impacted tooth. Oral Surg Oral Med Oral Pathol. 1968;26(5):658.
44. Romero CJ. Root resorption of second molar related to impacted 3rd molar. Oral Surg Oral Med Oral Pathol. 1971;32(3):502.
45. Yamaoka M, Furusawa K, Ikeda M, Hasegawa T. Root resorption of mandibular second molar teeth associated with the presence of the third molars. Aust Dent J. 1999;44(2):112-116.
46. Yusof WZ, Ghazali MN. Multiple external root resorption. J Am Dent Assoc. 1989;118(4):453-455.
47. Neff P. Trauma from occlusion. Restorative concerns. Dent Clin North Am. 1995;39(2):335-354.
48. Rawlinson A. Treatment of root and alveolar bone resorption associated with bruxism. Br Dent J. 1991;170(12):445-447.
49. Soğur E, Soğur HD, Baksi Akdeniz BG, Sen BH. Idiopathic root resorption of the entire permanent dentition: systematic review and report of a case. Dent Traumatol. 2008;24(4):490-495.
50. Williams CG. Suspected idiopathic external resorption of a mandibular molar. Br Dent J. 1983;155(6):193-195.
51. Soni NN, LaVelle WE. Idiopathic root resorption. Report of a case. Oral Surg Oral Med Oral Pathol. 1970;29(3):387-389.
52. Rivera EM, Walton RE. Extensive idiopathic apical root resorption. A case report. Oral Surg Oral Med Oral Pathol. 1994;78(5):673-677.
53. McMullin A, Fleming PS, DiBiase AT. Idiopathic generalized apical root resorption: a report of three cases. Int J Paediatr Dent. 2008;18(4):312-316.
54. Cholia SS, Wilson PH, Makdissi J. Multiple idiopathic external apical root resorption: report of four cases. Dentomaxillofac Radiol. 2005;34(4):240-246.
55. Schätzle M, Tanner SD, Bosshardt DD. Progressive, generalized, apical idiopathic root resorption and hypercementosis. J Periodontol. 2005;76(11):2002-2011.
56. Brooks JK. Multiple idiopathic apical external root resorption. Gen Dent. 1986;34(5):385-386.
57. Moody GH, Muir KF. Multiple idiopathic root resorption. A case report and discussion of pathogenesis. J Clin Periodontol. 1991;18(8):577-580.
58. Liang H, Burkes EJ, Frederiksen NL. Mutiple idiopathic cervical root resorption: systematic review and report of four cases. Dentomaxillofac Radiol. 2003;32(3):150-155.
59. Iwamatsu-Kobayashi Y, Satoh-Kuriwada S, Yamamoto T, et al. A case of multiple idiopathic external root resorption: a 6-year follow-up study. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005;100(6):772-779.
60. Abyholm FE, Bergland O, Semb G. Secondary bone grafting of alveolar clefts. A surgical/orthodontic treatment enabling a non-prosthodontic rehabilitation in cleft lip and palate patients. Scand Plast Reconstr Surg. 1981;15(2):127-140.
61. Enemark H, Krantz-Simonsen E, Schramm JE. Secondary bone grafting in unilateral cleft lip palate patients: indications and treatment procedures. Int J Oral Surg. 1985;14(1):2-10.
62. Gerner NW, Hurlen B, Bergland O, et al. External root resorption in patients with secondary bone-grafting of alveolar clefts. Endod Dent Traumatol. 1986;2(6):263-266.
63. Solomon CS, Coffiner MO, Chalfin HE. Herpes zoster revisited: implicated in root resorption. J Endod. 1986;12(5):210-213.
64. Ramchandani PL, Mellor TK. Herpes zoster associated with tooth resorption and periapical lesions. Br J Oral Maxillofac Surg. 2007;45(1):71-73.
65. Wright WE, Davis ML, Geffen DB, et al. Alveolar bone necrosis and tooth loss. a rare complication associated with herpes zoster infection of the fifth cranial nerve. Oral Surg Oral Med Oral Pathol. 1983;56(1):39-46.
66. Goon WW, Jacobsen PL. Prodromal odontalgia and multiple devitalized teeth caused by a herpes zoster infection of the trigeminal nerve: report of case. J Am Dent Assoc. 1988;116(6):500-504.
67. Gregory WB Jr, Brooks LE, Penick EC. Herpes zoster associated with pulpless teeth. J Endod. 1975;1(1):32-35.
68. Kolas S, Cavalaris CJ, Finch RR. Radiographic patterns of resorption seen in some gnathodental hard-tissue disturbances. Dent Clin North Am. 1968:589-611.
69. Hutchison IL, Hopper C, Coonar HS. Neoplasia masquerading as periapical infection. Br Dent J. 1990;168(7):288-294.
70. Gahan R, Rout J, Webster K. Case report: oral manifestations and radiographic features of osteosarcoma. Dent Update. 2007;34(1):52-54.
71. George DI Jr, Miller RL. Idiopathic resorption of teeth. A report of three cases. Am J Orthod. 1986;89(1):13-20.
72. Smith BJ, Eveson JW. Paget's disease of bone with particular reference to dentistry. J Oral Pathol. 1981;10(4):233-247.
73. Barnett F, Elfenbein L. Paget's disease of the mandible—a review and report of a case. Endod Dent Traumatol. 1985;1(1):39-42.
74. Belanger GK, Coke JM. Idiopathic external root resorption of the entire dentition: report of a case. ASDC J Dent Child. 1985;52(5):359-363.
75. Newman WG. Possible etiologic factors in external root resorption. Am J Orthod. 1975;67(5):522-539.
76. Rüdiger S, Berglundh T. Root resorption and signs of repair in Papillon-Lefèvre syndrome. A case study. Acta Odontol Scand. 1999;57(4):221-224.
77. Fayad S, Steffensen B. Root resorption in a patient with hemifacial atrophy. J Endod. 1994;20(6):299-303.
78. Moskow BS. Periodontal manifestations of hyperoxaluria and oxalosis. J Periodontol. 1989;60(5):271-278.
79. Pankhurst CL, Eley BM, Moniz C. Multiple idiopathic external root resorption. A case report. Oral Surg Oral Med Oral Pathol. 1988;65(6):754-756.
80. Baxter AM, Shaw MJ, Warren K. Dental and oral lesions in two patients with focal dermal hypoplasia (Goltz syndrome). Br Dent J. 2000;189(10):550-553.
81. Mitchell CA, Kennedy JG, Owens PD. Dental histology in familial expansile osteolysis. J Oral Pathol Med. 1990;19(2):65-70.
82. Thoma KH, Sosman MC, Bennett GA. An unusual case of hereditary fibrous osteodysplasia (fragilitas ossium) with replacement of dentin by osteocementum. Am J Orthod Oral Surg. 1941;29(1):C1-C30.
About the Authors
Robert J. Kanas, DDS
Staff Dentist, Crittenton Medical Center
Rochester Hills, Michigan
Private Practice
Lakeville, Michigan
Scott J. Kanas
Predoctorate Student, Biochemistry, University of Detroit Mercy
Detroit, Michigan