Combination Syndrome Symptomatology and Treatment
Abstract
Combination syndrome (CS) is one of the most fascinating oral conditions yet is poorly understood and underappreciated in the literature and clinical practice. This article reviews the most important literature on this subject and analyzes the etiology, symptomatology, diagnosis, and current therapeutic modalities for treatment in an attempt to better understand CS. The syndrome represents an example of a complex pathologic condition of the entire stomatognathic system with a multitude of hard-tissue, soft-tissue, and occlusal changes. These changes, initiated by a certain sequence of events, beginning with a prolonged period of tooth loss, can lead to severe bone atrophy in different regions of the jaws, loss of masticatory function, and the need for complex treatment. Implant rehabilitation of these patients in a preventative approach with cooperation of the entire dental team is emphasized.
Kelly proposed the name combination syndrome (CS) in his original article1 published in 1972 in the Journal of Prosthetic Dentistry. In 2003, this article was reprinted as a classic in the same journal.2 Although some of the symptoms were known previously, Kelly had proposed a new condition by connecting the variety of known characteristic symptoms into one syndrome.
“The Glossary of Prosthodontic Terms”3 defines CS as “the characteristic features that occur when an edentulous maxilla is opposed by natural mandibular anterior teeth, including loss of bone from the anterior portion of the maxillary ridge, overgrowth of the tuberosities, papillary hyperplasia of the hard palate’s mucosa, extrusion of the lower anterior teeth, and loss of alveolar bone and ridge height beneath the posterior mandibular removable dental prosthesis bases—also called anterior hyperfunction syndrome.”
It also is in the “Glossary of Implant Terms”4 as “a condition caused by the presence of lower anterior teeth and an absence of the posteriors, resulting in significant maxillary anterior alveolar resorption.” This oral condition is viewed as a rarely occurring syndrome with most signs and symptoms appearing in approximately 24% of the population wearing a maxillary complete denture as opposed to a bilateral-distal extension partial denture.5 The CS literature is full of controversy regarding this condition, including uncertainty in regard to identifying it as a medical syndrome.6
There are few studies of long-term results and the association with implant and prosthetic characteristics, patients’ medical conditions, and implant survival outcomes in partially edentulous patients missing posterior teeth.7 Classification of CS in a variety of partially edentulous cases recently has been proposed.8 Based on a literature reviewwea and the author’s experience, this article discusses the symptoms in the order of their typical clinical appearance and conventional and implant treatment for this condition.
Symptomatology
Development of CS stems from traumatic occlusion. The most common initiating scenario involves complete loss of teeth in the maxilla and partial loss of teeth in the mandible, with preserved anterior teeth causing a deficiency of masticatory function. Presence of complete maxillary and partial class I mandibular removable dentures only partially buffers a significant reduction of occlusal function. Loss of function in skeletal bones leads to nonuse atrophy of supporting bone and attached muscles, and jaws are no exception to this rule. For patients with CS, loss of posterior teeth and deficiency in mastication eventually lead to alveolar bone resorption in the posterior quadrants of the jaws. Further, the posterior mandible is more likely than the posterior maxilla to experience pronounced atrophy after tooth loss. This atrophy pattern occurs not only because of loss of function but also resorptive changes from denture wear9-14 and the age-related decrease of blood supply (poor perfusion) found in the posterior mandible and ramus.15
As patients with complete maxillary denture and bilateral distal-extension mandibular removable partial dentures progressively lose bone in the posterior mandible, the lower denture bases gradually sink and a posterior open bite develops. When patients’ complete maxillary and partial mandibular dentures are adjusted routinely, the development of the posterior open bite is less severe.1 When patients do not return for follow-up care and/or the mandibular removable partial denture is not well designed, relined, or maintained, a lack of posterior occlusal contacts causes an eventual and progressive shift of masticatory function to anterior segments of jaws.5
Subsequently, two important CS features usually develop. The first is hypertrophy of the anterior mandible with anterior hyperfunction. Anterior teeth are not designed for heavy occlusal load. Posterior reduction of function (posterior hypofunction) leads to anterior increase in function and subsequently hypertrophy of anterior mandibular bone to accommodate it. Anterior mandibular teeth take over function of mastication of practically the entire mandibular dentition. An adverse chronic pressure originating from the lower anterior teeth is directed toward the anterior portion of the unsupported maxillary denture. This repetitive force inevitably causes considerable resorption of the premaxillary alveolar bone. Heavy function, unusual in the anterior regions of the jaws, is known in the CS literature as anterior hyperfunction,16,17 which explains the other commonly used term for the syndrome, anterior hyperfunction syndrome.6,8,16,17
As both anterior maxillary atrophy and anterior mandibular hypertrophy develop, the entire anterior jaw complex progressively rotates clockwise (autorotation), leading to eventual unesthetic submergence of maxillary anterior denture teeth underneath the upper lip and abnormal exposure of mandibular anterior natural teeth from and above the vermilion border of the lower lip. Chronic occlusal trauma from the incisal edges of mandibular anterior teeth also often causes “flabby” and “fibrous” soft-tissue changes of the anterior palate, commonly described in the literature as papillary hyperplasia.1,5,6 The hyperplastic tissues in the region can be extensive and may compromise support and retention of a complete maxillary denture.
The second important symptom in CS cases is posterior maxillary hypertrophy and enlargement of maxillary tuberosities. In his original article,1 Kelly suggested its origin from a “negative pressure” from underneath the denture related to presence of a posterior palatal seal. Today, it is attributed to a slow resorption of posterior mandibular bone, with reduction of alveolar ridge height and progressive sinkage (down migration) of the mandibular partial denture. The ensuing chronic posterior open bite seems to be responsible for hypertrophy of posterior maxillary alveolar bone with tuberosities in an attempt to preserve the vertical occlusal functional relationship. If the posterior maxilla has a remaining tooth or teeth, this bone hypertrophy usually occurs at the same time as tooth/teeth super-eruption. In most clinical cases with a lack of opposing dentition, both the teeth and underlying bone react simultaneously: teeth super-erupt and bone develops hypertrophy. In patients with CS, this phenomenon is unique and can occur in both the anterior and posterior regions of the jaws. In anterior segments of the jaws, lack of maxillary teeth (especially in the presence of anterior hyperfunction) leads to extrusion of mandibular teeth with simultaneous mandibular alveolar hypertrophy. In posterior segments of the jaws, an opposite process develops. A non-use atrophy of the mandibular edentulous bone with increasing posterior open bite is responsible for hypertrophy of posterior maxillary alveolar bone and super-eruption of teeth, if present.
Wolff’s law can give the best explanation for bone remodeling changes that occur in CS. It states that “bone, either normal or abnormal, will develop the structure most suited to resist those forces acting on it.”18 In other words, bone is deposited and resorbed in accordance with the stresses placed upon it. Recent experimental research has indicated that bone resorption is a pressure-regulated phenomenon.19 Both bone atrophy and hypertrophy are opposite processes of the bone remodeling process, and their development in the stomatognathic system appears to be proportional to a degree of occlusal stress.
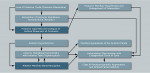
Resorption of both anterior maxillary and posterior mandibular edentulous alveolar ridges leads to a progressive collapse of the vertical dimension of occlusion (anterior and posterior vertical occlusal heights). The mandible moves forward, causing a relative (pseudo) mandibular prognathism. An overprojected and up-rotated chin point and a collapsed lower facial height are associated with the altered facial esthetics seen in advanced CS cases. In some patients, not all symptoms are present or obvious. Two symptoms that are consistently present and distinguish CS cases from all other dental conditions are resorption of anterior maxilla and posterior open bite (loss of posterior occlusion). Figure 1 demonstrates the 10 most common CS symptoms and their interrelationships.
Treatment Options
Because of the complexities of CS, a team of dental professionals should be involved in the treatment process of patients with this oral condition. Kelly1 emphasized prevention as the best possible treatment. He stated that the clinician should do everything possible to prevent the unfavorable combination of removable dental prostheses that include a complete maxillary denture and distal extension mandibular partial denture. Frequent relining of ill-fitting dentures slows down but does not stop the development of CS.
If conventional denture treatment is the only one selected by the patient, CS symptoms can be postponed through the use of a properly designed class I mandibular removable partial denture with equal redistribution of occlusal stresses over the hard and soft tissues of the entire dentition that maintains posterior function with maximal support and stability from the retromolar pads and buccal shelves.20,21 A meticulous follow-up care and maintenance protocol is important.
Jameson and others16,17,22,23 noticed avoidance of anterior hyperfunction should be the main emphasis of treatment directed at improving stability of removable dentures. Jameson advocated “linear occlusion,” or the occlusal arrangement of artificial teeth, as viewed in the horizontal plane, with a straight, long, narrow occlusal table of the mandibular posterior artificial teeth. He also stressed the importance of reducing the anterior incisal length for protrusive clearance. Although this prosthetic technique could improve the stability of dentures, it does not address endosseous bone loading (EBL) and prevention of bone resorption. Directing treatment toward the retention of lower posterior teeth “as abutments by means of endodontic and periodontic techniques” was emphasized by both Kelly1 and Jameson.16,17,22 Mandibular overdentures retained on natural posterior roots with stud-type abutments can allow preservation of posterior alveolar bone and occlusion. This treatment approach does not stop bone resorption completely because the denture bases remain supported by mucosal tissues. In addition, in many cases, it is not possible to keep anterior incisor teeth or posterior roots because of the severity of their endodontic and/or periodontal conditions.
For some patients, mandibular anterior teeth can be treated with root canal therapy and have their clinical crowns shortened to place opposing maxillary incisors in a proper position. In advanced conditions of super-eruption, they need to be removed with vertical reduction of hypertrophic alveolar bone (alveoloplasty). A variety of surgical procedures may be needed, including excision of hyperplastic tissue from the anterior palate, reduction of hypertrophic bone of maxillary tuberosities and anterior mandible (alveolectomy), correction of premaxillary bone atrophy with bone grafting, subantral augmentation (sinus lift), and extraction of super-erupted (extruded) teeth. Occlusal considerations with correction of the occlusal plane always should be a part of the comprehensive treatment for CS.
Both implant-retained and implant-supported prostheses have become increasingly popular in the past 30 years and have been proven to be a successful prosthetic rehabilitation for partially and completely edentulous maxilla and mandible.24-26 Implant-anchored prostheses have no inherent mobility associated with traditional root overdentures. These prostheses also demonstrate tremendous retention, improved stability, and ensure the endosseous bone loading that is so important for bone preservation.Implant-borne prostheses provide system rigidity with solid posterior contacts and preserved posterior occlusion, an imperative factor in CS cases.
At the same time, it is well documented in the literature27-32 that full mandibular implant-retained or supported prostheses based on four to six anteriorly placed implants against a complete maxillary denture provoke an extensive resorption of premaxillary bone that is comparable with resorption afflicted from natural mandibular anterior teeth. The cause is similar—anterior traumatic occlusion. Therefore, implant treatment of both the mandibular and maxillary arches needs to be considered to control CS-associated bone loss. By reinforcing the maxilla with implants, a compatible pair of implant-supported upper and lower prostheses can function in unison for an extended period.
Full-arch maxillary and mandibular reconstruction with endosseous dental implants (with or without previous alveolar bone grafting) should aim to develop a stable posterior occlusion, prevent anterior hyperfunction, and, hopefully, achieve an even distribution of masticatory force over the entire dentition. These conditions can provide long-lasting stability for patients with CS. Many standard prosthetic principles of treatment are applicable in CS cases, including protective occlusal scheme, cross-arch stabilization, appropriate anterior-posterior (A-P) implant spread, thoughtful prosthetic design with adequate metal support of acrylic portion and cleansable features of prostheses, and adequate esthetics and phonetics.
Conclusion
CS cases demonstrate bone remodeling changes that include atrophy and hypertrophy in certain regions of the jaws. Chronic occlusal pressure (overload) eventually leads to bone resorption in the anterior maxillary zone (premaxilla). In reverse, lack of function and loss of occlusion over time tend to promote super-eruptive forces from the opposing dentition, leading to bone hypertrophy that is usually present in regions of anterior mandible and posterior maxilla, including maxillary tuberosities. Loss of posterior occlusion (posterior open bite) and anterior maxillary bone resorption are the defining symptoms of CS.
Although a traditional prosthetic approach with a complete maxillary denture and a bilateral-distal extension mandibular partial denture remains in use, osseointegrated implant-retained and especially implant-supported prosthetic treatment has become the mainstream approach for patients with CS. Implant rehabilitation techniques applied for CS patients are directed toward the prevention of EBL and bone preservation, reversal of anterior occlusal trauma (anterior hyperfunction), and reestablishment of posterior occlusion. Complex CS cases often necessitate an interdisciplinary approach to care. Further prospective and retrospective studies are necessary to challenge and expand our current knowledge of CS, emphasize its prevention, and improve treatment protocols for this fascinating and complex dental condition.
References
1. Kelly E. Changes caused by a mandibular removable partial denture opposing a maxillary complete denture. J Prosthet Dent. 1972;27(2):140-150.
2. Kelly E. Changes caused by a mandibular removable partial denture opposing a maxillary complete denture. J Prosthet Dent. 2003;90(3):213-219.
3. The glossary of prosthodontic terms. J Prosthet Dent. 2005;94(1):10-92.
4. Oral implantology. Glossary of implant terms. J Oral Implantol. 2007;(suppl 1):2-14.
5. Shen K, Gongloff RK. Prevalence of the “combination syndrome” among denture patients. J Prosthet Dent. 1989;62(6): 642-644.
6. Palmqvist S, Carlsson GE, Owall B. The combination syndrome: a literature review. J Prosthetic Dent. 2003;90(3):270-275.
7. Attard NJ, Zarb GA. Implant prosthodontic management of partially edentulous patients missing posterior teeth: the Toronto experience. J Prosthet Dent. 2003;89(4):352-359.
8. Tolstunov L. Combination syndrome: classification and case report. J Oral Implantol. 2007;33(3):139-151.
9. Carlsson GE. Clinical morbidity and sequelae of treatment with complete dentures. J Prosthet Dent. 1998;79(1):17-23.
10. Atwood DA. Reduction of residual ridges: a major oral disease entity. J Prosthet Dent. 1971;26(3):266-279.
11. Tallgren A. The continuing reduction of residual alveolar ridges in complete denture wearers: a mixed-longitudinal study covering 25 years. J Prosthet Dent. 1972;27(2):120-132.
12. Bergman B, Carlsson GE. Clinical long-term study of complete denture wearers. J Prosthet Dent. 1985;53(1):56-61.
13. Campbell RL. A comparative study of the resorption of the alveolar ridges in denture-wearers and non denture-wearers. J Am Dent Assoc. 1960;60:143-153.
14. Józefowicz W. The influence of wearing dentures on residual ridges: a comparative study. J Prosthet Dent. 1970;24(2):137-144.
15. Tolstunov L. Implant zones of the jaws: implant location and related success rate. J Oral Implantol. 2007;33(4):211-220.
16. Jameson WS. Various clinical situations and their influence on linear occlusion in treating combination syndrome: a discussion of treatment options. Gen Dent. 2003;51:443-447.
17. Jameson WS. Combining fixed and removable restorations with linear occlusion in treating combination syndrome: a discussion of treatment options. Gen Dent. 2003;51(5):443-447.
18. Glossary of Implant Dentistry. Upper Montclair, NJ: International Congress of Oral Implantologists; 2004.
19. Carlsson GE. Responses of jawbone to pressure. Gerodontology. 2004;21(2):65-70.
20. Saunders TR, Gillis RE Jr, Desjardins RP. The maxillary complete denture opposing the mandibular bilateral distal-extension partial denture: treatment considerations. J Prosthet Dent. 1979;41(2):124-128.
21. Langer Y, Laufer B, Cardash HS. Modalities of treatment for the combination syndrome. J Prosthodont. 1995;4(2):76-82.
22. Jameson WS. The use of linear occlusion to treat a patient with combination syndrome: a clinical report. J Prosthet Dent. 2001;85(1):15-19.
23. Frush JP. Linear occlusion. Ill Dent J. 1966;35(12):788-794.
24. Adell R, Eriksson B, Lekholm U, et al. A long-term follow-up study of osseointegrated implants in the treatment of totally edentulous jaws. Int J Oral Maxillofac Implants. 1990;5(4):347-358.
25. Jemt T, Lekholm U, Adell R. Osseointegration in the treatment of partially edentulous patients: a preliminary study of 876 consecutively placed fixtures. Int J Oral Maxillofac Implants. 1989;4(3):211-215.
26. Zarb G, Attard N. Implant management of posterior partial edentulism. Int J Prosthodont. 2007;20:371-373.
27. Kreisler M, Behneke N, Behneke A, et al. Residual ridge resorption in the edentulous maxilla in patients with implant-supported mandibular overdentures: an 8-year retrospective study. Int J Prosthodont. 2003;16(3):295-300.
28. Lechner SK, Mammen A. Combination syndrome in relation to osseointegrated implant-supported overdentures: a survey. Int J Prosthodont. 1996;9(1):58-64.
29. Barber HD, Scott RF, Maxson BB, et al. Evaluation of anterior maxillary alveolar ridge resorption when opposed by the transmandibular implant. J Oral Maxillofac Surg. 1990;48(12):1283-1287.
30. Narhi TO, Geertman ME, Hevinga M, et al. Changes in the edentulous maxilla in persons wearing implant-retained mandibular overdentures. J Prosthet Dent. 2000;84(1):43-49.
31. Thiel CP, Evans DB, Burnett RR. Combination syndrome associated with a mandibular implant-supported overdenture: a clinical report. J Prosthet Dent. 1996;75(2):107-113.
32. Cabianca M. Combination syndrome: treatment with dental implants. Implant Dent. 2003;12(4):300-305.
About the Author
Len Tolstunov, DDS, DMD
Private Practice, Oral and Maxillofacial Surgery
San Francisco, California
Assistant Clinical Professor
Department of Oral and Maxillofacial Surgery
University of the Pacific School of Dentistry
San Francisco, California