Oral Factitious Injury in a Child with Kabuki Syndrome
Rose Wadenya, DMD, MS; Andres Pinto, DMD, MPH; and Rochelle Lindemeyer, DMD
Abstract: Factitious injury or self-injurious behavior is a common manifestation in children affected by neurologic, developmental, or psychiatric disease. The nature and presentation of this behavior in the oral cavity varies among diagnoses and may be missed easily. This report describes the presence of self-injurious behavior in a child with Kabuki syndrome who presented to a pediatric dentistry referral practice for evaluation of gingival bleeding, and provides a brief overview of the known etiology and management of this challenging condition. Clinicians should be aware of the possibility of self-injurious behavior when treating children who have Kabuki syndrome.
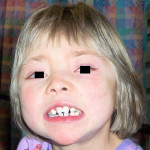
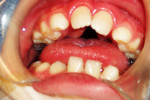
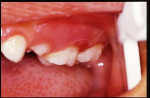
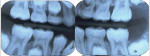
Kabuki syndrome is a rare, multiple congenital anomaly/mental retardation syndrome first described in 1981.1 This syndrome was reported initially in Japanese children but may occur in many ethnic groups. The most striking aspects of the disorder are the unique facial features, including long palpebral fissures, arched eyebrows, short columnella, and prominent ears (Figure 1). Other findings include microcephaly, hypotonia, seizures, hearing loss, ptosis, strabismus, congenital heart defects, renal anomalies, growth hormone deficiency, skeletal abnormalities, and immune deficiency. Dental and craniofacial findings include a trapezoid-shaped philtrum, cleft palate or cleft lip/palate, lip pits, hypodontia, microdontia, a small dental arch, maxillary recession, and midfacial hypoplasia (Figure 2 and Figure 3). Mental retardation is a cardinal manifestation of the disorder. Approximately 300 cases have been reported in the literature. No standard testing is available for this syndrome, and the diagnosis is made from phenotypic characteristics.2 This article, to the authors; knowledge, is the first report of oral self-injurious behavior in a child with Kabuki syndrome.
Case Report
An 11-year-old Middle Eastern male presented to the Children’s Hospital of Philadelphia complaining of gingival bleeding from the left side of his mouth. A detailed review of his medical history revealed that he received a diagnosis of Kabuki syndrome at 1 year of age. Chromosomal analysis showed the normal male karyotype 46, XY. Other findings at that time included bilateral kidney hypoplasia, beta thalassemia trait, retinal colobomas, ventricular septal defect, which closed on its own at 2 years of age, mild scoliosis, and submucous cleft palate. At 3 years of age, the patient also received a diagnosis of autism and developmental delay. At presentation, he exhibited characteristic facial features of the syndrome: arched eyebrows that were sparse on the lateral third, long palpebral fissures, eversion of lateral third of the lower eyelids, large prominent ears, broad nose with a depressed nasal tip, and scoliosis. He also had a low-tone subluxed left hip and was receiving care from specialists at the children’s hospital.
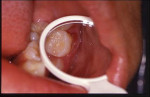
The intraoral examination revealed moderate bleeding of the maxillary left gingiva surrounding a primary second molar (Figure 4, 5, 6). The periodontal examination revealed normal osseous and gingival anatomy with minimal recession in the distal of the tooth. After careful observation and additional parent questioning, it was apparent that the child favored the left maxillary area when introducing his fingers into the mouth and that the gingival bleeding was aggravated by the finger habit. The remaining mixed dentition was normal.
The parents were encouraged to monitor the patient closely and dissuade him from putting his fingers in the mouth. The need for meticulous oral hygiene with a soft toothbrush (three times per day) was reinforced. A 2-week follow-up visit revealed healthy soft tissue around the affected tooth, which exfoliated approximately 4 weeks later.
Discussion
The presence of self-injurious behavior involving the oral soft or hard tissues is documented in the dental literature involving children and adults.3-7 A plethora of diseases are linked to the appearance of this behavior, and psychiatric abnormalities, such as depression, social stress, and low esteem, often are present.8 In addition, eating disorders and suicidal behaviors are common in adolescents, who are subject to intense peer pressure.9
One form of self-injurious behavior that reflects destruction of one’s body without suicidal intent is termed nonsuicidal self-injury (NSSI).10 NSSI may produce factitial sequelae, affecting the hands, head, and neck. This type of self-injurious behavior can be attributed to functional and biologic causes. A recent study in preadolescent girls reported a close association between internal distress (peer victimization) and the onset of self-injury for social reinforcement. It is worth noting that half of the girls interviewed in this small study admitted to a recent NSSI.11 Another population-based Canadian survey reported that 20% of 568 youngsters interviewed admitted to some form of self-injurious behavior, with 56% not receiving professional help for this behavior.12 NSSI often occurs in the oral cavity as repetitive movements that cause tissue damage and is seen in normal or mentally impaired individuals. This behavior has been reported in mental retardation, autism, cerebral palsy, Lesch-Nyhan syndrome, Cornelia de Lange syndrome, Tourette and Rett syndromes, hereditary sensory and autonomic neuropathy, familial dysautonomia, and Chiari type II malformations.4-7 Similarly, patients who have sustained severe traumatic brain injury or are comatose may develop neuropathologic chewing that can result in self-inflicted injury.3 An altered sensitivity to pain predisposes these patients to extensive oral self-inflicted ulcerations, leading to loss of permanent dentition and mucosal scarring that affects masticatory function.
The etiology of self-injurious behavior is linked to an abnormal balance of neurotransmitters.13 Abnormal levels of endorphins and enkephalins, endogenous opiates linked to self-satisfaction and well-being are found in the cerebrospinal fluid of some patients. These individuals engage in repetitive behavior to fulfill the need for production of these molecules. Dopaminergic dysfunction is described in some subgroups, and dopamine agonistic drugs have induced similar behaviors experimentally. Serotonin dysfunction is documented in children exhibiting self-injurious behavior with agitation. Often, these children are affected by increased stress and compulsive-obsessive disorders that set forth the injurious behavior.
Biologic and environmental determinants play an important role in the development of self-injury in genetically and psychologically susceptible children. Common triggers in this category include allergic reactions, constipation, otitis media, and other painful conditions that present the child with an unfamiliar pattern of events, leading to the behavior.14,15 The nonverbal child in the presence of frustration, stress, or attention-seeking may become involved in self-injurious behavior.
From an oral perspective, the severity of self-injurious behavior differs among conditions such as neurologic trauma, developmental delay, or syndromic diagnosis, and psychiatric diagnoses that may have this behavior as an outcome.
Management
The management of oral self-injury has been limited to nonpharmacologic interventions, ranging from behavior modification to placement of intraoral appliances intended to protect and isolate the soft tissues. These appliances can be hard-made from acrylic or may be made of soft material, depending on the nature of the injury. Other interventions include occlusal adjustment of protruding or sharp dental anatomy to limit the amount of damage and pharmacotherapy, which is used in patients with autism, mental retardation and syndromic disease.15 In most instances, a combination of psychosocial, cognitive, and pharmacologic interventions is necessary to control the behavior successfully.15,16
Conclusion
These authors believe this article is the first report of oral self-injury in a child with Kabuki syndrome. Dentists must be able to recognize behavior patterns of oral self-injury in this population and the triggering events that may lead to a new onset or change in behavior pattern. Many of these children may have intraoral sources of discomfort or pain, unrelated to neurologic or biochemical central nervous system abnormalities that precipitate the aberrant behavior. A team approach with close collaboration with the child’s physicians enhances the efficacy of dental, behavioral, and pharmacologic therapy in circumstances in which the self-injurious behavior requires more than physical interventions to manage. The case described in this report is mild in severity and presumably linked to the discomfort associated with the mixed dentition, as the self-injury resolved solely with simple behavioral intervention.
References
1. Adam M, Hudgins L. Kabuki syndrome: a review. Clin Genet. 2005;67(3):209-219.
2. Johnson G, Mayhew JF. Anesthesia for a child with kabuki syndrome. Pediatr Anesth. 2007;17(9):900-901.
3. Kobayashi T, Ghanem H, Umezawa K, et al. Treatment of self-inflicted oral trauma in a comatose patient: a case report. J Can Dent Assoc. 2005;71(9):661-664.
4. Nurko C, Errington BD, Ben Taylor W, et al. Lip biting in a patient with chiari type II malformation: case report. Pediatr Dent. 1999;21(3):209-212.
5. Lucavechi T, Barbería E, Maroto M, et al. Self-injurious behavior in a patient with mental retardation: review of the literature and a case report. Quintessence Int. 2007;38(7):e393-e398.
6. Medina AC, Sogbe R, Gómez-Rey AM, et al. Factitial oral lesions in an autistic paediatric patient. Int J Paediatr Dent. 2003;13(2):130-137.
7. Erdem TL, Ozcan I, Ilgüy D, et al. Hereditary sensory and autonomic neuropathy: review and a case report with dental implications. J Oral Rehabil. 2000;27(2):180-183.
8. Williams KA, Bydalek KA. Adolescent self-mutilation: diagnosis and treatment. J Psychosoc Nurs Ment Health Serv. 2007;45(12):19-23.
9. Ahrén-Moonga J, Holmgren S, von Knorring L, et al. Personality traits and self-injurious behaviour in patients with eating disorders. Eur Eat Disord Rev. 2008;16(4):268-275.
10. Prinstein MJ. Introduction to the special section on suicide and nonsuicidal self-injury: a review of unique challenges and important directions for self-injury science. J Consult Clin Psychol. 2008;76(1):1-8.
11. Hilt LM, Cha CB, Nolen-Hoeksema S. Nonsuicidal self-injury in young adolescent girls: moderators of the distress-function relationship. J Consult Clin Psychol. 2008;76(1):63-71.
12. Nixon MK, Cloutier P, Jansson SM. Nonsuicidal self-harm in youth: a population-based survey. CMAJ. 2008;178(3):306-312.
13. King BH. Pharmacological treatment of mood disturbances, aggression, and self-injury in persons with pervasive developmental disorders. J Autism Dev Disord. 2000;30(5):439-445.
14. Russell PS. Self-injurious behavior to the lower extremities among children with atypical development: a diagnostic and treatment algorithm. Int J Low Extrem Wounds. 2006;5(1):10-17.
15. Symons FJ, Thompson A, Rodriguez MC. Self-injurious behavior and the efficacy of naltrexone treatment: a quantitative synthesis. Ment Retard Dev Disabil Res Rev. 2004;10(3):193-200.
16. Richman DM. Early intervention and prevention of self-injurious behaviour exhibited by young children with developmental disabilities. J Intellect Disabil Res. 2008;52(Pt 1):3-17.
About the Authors
Rose Wadenya, DMD, MS
Assistant Professor
Pediatric Dentistry
The Children’s Hospital of Philadelphia
Philadelphia, Pennsylvania
Andres Pinto, DMD, MPH
Assistant Professor
Oral Medicine and University Associate
The Children’s Hospital of Philadelphia
Philadelphia, Pennsylvania
Rochelle Lindemeyer, DMD
Assistant Professor and Residency Program Director
The Children’s Hospital of Philadelphia
Philadelphia, Pennsylvania