Smile Designing for the Malcontent Patient
Ronald LuBovich Sr, DDS, MSD, FIDS, FICOI
Abstract
Patients and dentists may have conflicting opinions regarding the definition of an esthetically pleasing smile. Every dentist is likely to encounter malcontent patients who may have difficulty communicating their esthetic desires for smiles and may even refuse to pay for successful treatment outcomes that they misperceive as failures. Learning how to work with such patients is essential. Part of achieving patient satisfaction is encouraging their participation in designing their smile. With the use of a crown-bridge-veneer pattern, tried-on prepared teeth, or implants, an exacting acrylic wax smile is designed. This pattern is used to analytically and objectively design porcelain contours for the finished smile design. This technique works well for veneers, full crowns, or bridges.
The clinician who restores anterior maxillary teeth experiences routine challenges, such as: A) midline positioning; B) the length and width of the central incisors; C) the incisal plane and orientation to the interpupillary line; and D) the patient’s sex and opinion of what makes a beautiful smile.
Every dentist is likely to see a malcontent patient. This article defines such patients as those who dislike any upper anterior maxillary crowns fabricated by previous dentists. One type of malcontent patient knows what he or she wants but is unable to communicate this. However, they do not blame others for their unhappiness. The problem is treatable, and these patients need to be trained to speak in helpful and descriptive terms. They can usually be taught to communicate adequately so that a wonderful smile design can be made. A practitioner should be wary of patients who blame others for their unhappiness. Their problems may not be treatable and inevitably they are unhappy with any and all services provided, even if they never pay for the service. Some use their complaints to avoid paying for dental services, despite successful treatment outcomes. The goal is to first determine, with a thorough diagnosis, history, and examination, if their problems are treatable or whether the patient should be referred to another dentist. Demanding and analytical characteristics in a patient who knows what kind of smile he or she desires does not necessarily preclude dental treatment. Lefer et al1 suggest there are psychological benefits in enabling patients to participate in designing their dental appearance rather than the dentist taking an authoritarian role: “Patient involvement will determine esthetic preference and affect success.” Brigante2suggests patient-assisted esthetics is critical for successful outcomes. In this author’s opinion, this was true in 1981 and remains so today. It is true for all areas of prosthodontics, both removable and fixed.
Anterior maxillary smile designing is always a challenge. Occasionally, smile designing is a frustrating experience, with considerable trial and error. The principles of esthetics must be considered when smile designing a 1x6 anterior maxillary set of crowns, veneers, or bridges. The principles of esthetics vary between dentists. However, there are basic tenets of dental esthetics that are beneficially performed when creating smile designs. Since Wright’s paper in 1878, numerous authors have referenced principles in denture esthetics.3 Initial theories have been proven to be scientifically unfounded.4 Denture esthetics provided the basics of esthetics that is now practiced in all areas of prosthodontics. Later references for dental esthetics have many areas of agreement, and the most popular of those principles, as they relate to success in esthetics, are briefly reviewed in this article.
The cosmetic dentist knows the importance of the following:
1. The plane of the incisal edges and interpupillary line.
2. The midline and its position and angle is critical in anterior maxillary smile (designing).
3. The size of the two central incisors is usually one-sixteenth the width of the bizygomatic distance. DENTSPLY International (https://www.dentsply.com) developed a device called the tooth indicator to measure this distance and indicate the proportionately correct width of the central incisors).
4. Central incisors should be identical,5-9 in length, width, and shape, including line-angle prominences; laymen prefer square and ovoid shapes and relate tapering-form teeth as aged.10
5. The smile and lip contours shapes also contribute to smile designing.
6. Positive, straight, or reverse smile lines are good alternatives, depending on a patient’s preference. A positive smile is most popular and youthful in appearance;11 flat or straight smile lines are more aged and rugged appearing, and reverse smile lines appear more esthetic when the upper anterior teeth are longer from gingival to their incisal edges. Dong et al12 wrote, “The amount of maxillary incisal exposure decreases with age, accompanied by an increase of mandibular incisal exposure.”
7. Rotating a lateral incisor on the narrow side of the face is needed occasionally.
8. When upper anterior pontics are esthetically too long, the use of pink or dark melanin gingival porcelain is often beneficial in implant anterior maxillary esthetics.
9. Contours and tooth length vary for males and females. Laymen, according to Marunick et al,13 found “preferences for square teeth for males and ovoid teeth for females support the dentogenic concept.”5-9
Cosmetic dentists have historically used many different techniques to guide the smile designing of upper anterior teeth. Many methods and guidelines are available to aid the cosmetic dentist in communicating esthetic needs to the dental technician. There are some recent references and guidelines for anterior esthetics. Naylor14 suggests the use of a grid analysis system as an aid to such treatment planning for the maxillary anterior teeth. Kleeberger15 recommends the use of a stick bite to provide more information to the laboratory technician. The stick bite is aligned perpendicular to the long axis of the face. This provides the technician more information about the needed midline, the axes, and incisal plane of the finished crowns or bridges.
When maximal esthetics and patient participation in the smile design process is needed, this author recommends the use of a wax pattern smile design. This smile design facilitates the tooth preparations. Then the pattern is developed with the patient, who can communicate his or her needs to the cosmetic dentist or dental technician. Patient participation is important to acquire his or her esthetic preferences and affect a successful outcome.1,2,10,13 The dentist or technician should be a facilitator, not an authoritarian.1 This can entail describing the differences between a rugged, angular, and masculine appearance and softer, more rounded feminine appearance. Patients should be encouraged to bring photographs, pictures from magazines, and their own drawings. Every effort to devote attention to their needs and desires should be performed.
Case Report 1
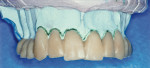
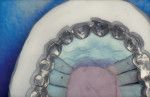
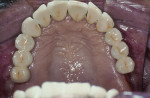
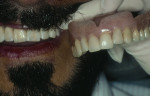
A 45-year-old male in good health presented with a chief complaint: “I did not like my smile as it was being performed in several other dental offices.” He had seen three dentists who considered him a malcontented patient. This patient presented with a history of implants placed in the posterior upper maxilla. Thereafter, the patient returned to the restorative dentist with a request to make his implant bridge similar to his old upper denture. He had worn an upper denture for more than 20 years. After working with the restorative dentist for several appointments, the patient became unsatisfied with the lack of progress and refused to pay for previous bridges. He tried two more dentists but was still unhappy. Then, for his upper implant-supported bridge, he was referred to the author’s office. The patient was a graphic designer, and he had brought small drawings of how he wanted his upper anterior bridge to appear. He brought his old denture, with teeth set as he wanted. An impression was made of the old upper denture to make a smile design cast (Figure 1). After custom implant posts were made, impressioned, and mounted on a fully adjustable Denar® articulator, (Whip Mix, https://www.whipmix.com), the smile design pattern was started (Figure 2). The irregular mal-aligned appearance of the old denture was imitated in the complete upper full-contour white wax pattern and tried in on the custom implant posts. Patient compliance was good in the creation of his wax pattern. He had specific needs and requests, and his desires were carefully evaluated to determine what he meant by each request. It is this author’s goal to listen to patients, decipher their concerns, and then make the bridge design according to the patient’s desires. After the pattern was finished in one appointment, the patient was provided with consent forms to finish the bridgework. When the author reviewed the importance of making final decisions about length, width, and inclinations of the teeth and read the consent form to the patient, the patient decided he would like to consider this pattern and examine it during another appointment. The patient was then seen on two subsequent appointments before he was happy with the pattern. Minimal changes were made during each appointment, but they were important for him before he would sign the consent to finish the bridgework. He then provided written consent to finish the upper metal-porcelain bridge. Two polyvinyl impressions of the facials of the wax pattern were then made. One was cut in the middle third; both were used to design the metal frame of the planned finished bridge. Figure 3 demonstrates how the internal frame was designed to complement the facial and lingual design of the mal-aligned overlapped teeth. The metal frame was designed to duplicate the proposed design of the finished porcelain bridge (Figure 4). He requested a natural color; internal opaque modifiers were used. Body and enamel porcelains were also modified to create more depth and color on line angles and more chroma at the middle incisal edges. The bridge was then delivered. The patient wanted minimal changes; the bridge was colored and glazed. He was satisfied with his special smile design pattern (Figure 5 and Figure 6). However, he called the author a week later and said he was unhappy. After making an appointment to determine why, he related the following chief complaint: “When I look at my smile from across the room, it appears my bridges’ front teeth are too short by 2 mm.” The author reminded the patient that the bridge was designed to a special pattern made on three appointments according to his smile design requests. The patient said, “I understand. You have been wonderful in helping design my smile, and I know that a new bridge will need to be made. I do not mind paying for another bridge to be made.” The author then modified the original wax pattern, tried it on his implant posts, made the changes requested, and then fabricated the second metal-ceramic fixed partial denture. The second maxillary bridge was delivered, and he was again happy. There were minimal differences in bridge Nos. 1 to 2. No appreciable difference was shown in photographs. He did not want the author to photograph his complete face. It is the author’s opinion that if the wax pattern were not made and consents were not made, this patient would always be unhappy with his smile. He would have continued being a problem with other dentists in regard to the making and remaking of his maxillary implant-supported fixed partial denture. The patient has had many years of successful smiling and function with his implant-supported bridge. This bridge is fully functional without any porcelain damage more than 20 years later (Figure 6). All implants are healthy.
Case Report 2
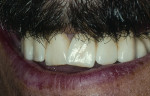
A 35-year-old female presented to the author’s clinic with her chief complaint: “I am not happy with my new crowns.” She recently had three sets of new crowns made for the upper anterior maxillary teeth. Figure 7 represents the appearance of her new upper anterior crowns. She had the following chief complaints: 1) “These crowns look like they should be in a man’s mouth;” 2) “They do not look like my previously made old crowns, which I liked;” 3) “The middle line of the upper two front teeth do not align with my face;” 4) “The two front teeth are not similar in their shapes;” and 5) “I hate these crowns.”
During the clinical examination, the author agreed with the patient’s chief complaints. Her crowns were masculine in appearance and angular.
Another patient had told her that the author makes wax patterns of crowns before making crowns. She asked to participate in the making of her smile design wax pattern. The pattern (Figure 8) was prepared and tried on the prepared maxillary teeth. Patient compliance was good in the smile design pattern. In two appointments, the size and length of the two front teeth were resolved. When she was happy, she signed the consent to finish bridgework crowns (Figure 9).
The patient wanted bright white crowns. She planned to bleach and perhaps crown the lower teeth. All upper anterior crowns were performed with a special formula to create a bleached white appearance. She loves her new crowns and has had years of success with smiling and function with her crowns, which are functioning and very cosmetic 20 years later (Figure 10).
Conclusion
There are various methods of making crowns that suit a patient’s smile design needs. This article presents one method of communicating the exact design patients want or need in the making of “their smile, their way.” Certainly, this plan will not succeed if the technician is not provided with a wax pattern. The author has found that many technicians stack bridgework and crowns upside down. More successful smiles result when technicians hold master casts in the same way patients present to them (right side up). When technicians stack them upside down, patients then have difficulty relating the smile design when seated in front of the clinician. The axial line angles of each crown or bridge unit needs to be drawn on the art form of the cast. This is another aid for the ceramist in stacking-stamping porcelain, which is similar to that described by LuBovich.16 The silicone or polyvinyl index can also be used to stamp out contours in porcelain during stacking. The ability of the designer ceramist will also make a difference in the final results. The wax pattern is an aid and can be more exact than any other technique, provided the wax pattern fits the dies well without rocking. Like appropriate treatment planning, this wax pattern performs like a plan. Like all cosmetic dentists know, a plan is needed. Without it, the dentist should prepare for failure.
References
1. Lefer L, Pleasure MA, Rosenthal L. Psychiatric approach to the denture patient. J Psychosoma Res.1962;6:199-207.
2. Brigante RF. Patient-assisted esthetics. J Prosthet Dent. 1981; 46(1):14-20.
3. Wright JW. A consideration of temperament in relation to teeth. Dental Cosmos. 1884;26:113.
4. Williams JL. The temperamental selection of artificial teeth: a fallacy. Dent Dig. 1914;20:243-305.
5. Frush JP, Fisher RD. How dentogenic restorations interpret the sex factor. J Prosthet Dent. 1956;6:160-172.
6. Frush JP, Fisher RD. How dentogenic restorations interpret the personality factor. J Prosthet Dent. 1956;6:441-449.
7. Frush JP, Fisher RD. The age factor in dentogenics. J Prosthet Dent. 1957;7:5-13.
8. Frush JP, Fisher RD. The dynesthetic interpretation of the dentogenic concept. J Prosthet Dent. 1958;8:558-581.
9. Frush JP, Fisher RD. Dentogenetics: its practical application. J Prosthet Dent. 1959;9:914-921.
10. Brisman AS. Esthetics: a comparison of dentists’ and patients’ concepts. J Am Dent Assoc. 1980:100(3):345-352.
11. Tjan AH, Miller GD, The JG. Some esthetic factors in a smile. J Prosthet Dent. 1984;51(1):24-28.
12. Dong JK, Jin TH, Cho HW, et al. The esthetics of the smile: a review of some recent studies. Int J Prosthodont. 1999;12(1):9-19.
13. Marunick MT, Chamberlain BB, Robinson CA. Denture aesthetics: an evaluation of laymen’s preferences. J Oral Rehabil. 1983;10:399-406.
14. Naylor CK. Esthetic treatment planning: the grid analysis system. J Esthet Restor Dent. 2002;14(2):76-84.
15. Kleeberger BT. Restoring the worn anterior dentition for function and esthetics. Journal of Cosmetic Dentistry. 2007;23(2):83-92.
16. LuBovich RP, Sanders HA Jr. The use of a silicone index to apply and contour porcelain on occlusal surfaces of ceramometal restorations. J Prosthet Dent. 1981;45(4):392-394.
About the Author
Ronald LuBovich Sr, DDS, MSD, FIDS, FICOI
Private Practice
Nashville, Tennessee