Fears and Concerns of Individuals Contemplating Esthetic Restorative Dentistry
Arthur A. Weiner, DMD; Paul C. Stark, MS, ScD; Joan LaSalvia, DDS; Matthew Navidomskis, DMD; and Gerard Kugel, DMD, MS, PhD
Abstract
Questionnaires that focus on the fear of dental treatment typically include a narrow list of previous treatment-related factors. By omitting items concerned with psychologic, emotional, and interpersonal traits that impact treatment, practitioners often fail to gain additional valuable information on related anxiety issues. This study was undertaken to identify previously unrecognized or poorly discussed sources of fear and anxiety in patients seeking esthetic dental treatment. The Esthetic Clinic at Tufts University School of Dental Medicine recruited 62 participants who were asked to score their level of anxieties and concerns based on 24 different items on a 0 to 5 Likert scale. In addition, age, gender, and type of procedure in consideration were the only other variables recorded. The item that elicited the highest level of anxiety was “not feeling happy with my new smile.” Thirty-eight respondents (61.3%) said they feel “markedly anxious”or “severely anxious” or answered “avoid completely.” Concerns “that the outcome might look false and unnatural” or “that the dentist might not redo it if I am not satisfied with the outcome” both received 37 out of 62 (59.7%) similar responses. These results suggest obstacles to treatment exist not only in areas typically investigated but also in factors rarely discussed during the patient-practitioner encounter. The practitioner needs to consider a broader range of issues when addressing the patient’s concerns.
Most dental practitioners know patients generally have anxiety associated with dental treatment. The sources vary, including fear of the drill and dental injection, prior trauma,1-4 and past experiences.
Throughout the years, numerous studies have investigated the phenomena associated with fear, anxiety, and avoidance of care.5-7 Some research has attempted to compare levels of patient satisfaction associated with different treatment interventions, whereas others have examined dentists’ attitudes and behaviors.8-11 In addition to exploring patients’ fears and dislike of dentistry, other clinicians have evaluated and devised various behavioral modalities, attempting to find efficient techniques that might reduce or ameliorate fear.12-16 However, due to the multiplicity of physical, psychological, and emotional factors that contribute to an individual’s make-up and can act as barriers to care,7 it has become increasingly difficult to use a single-study questionnaire to evaluate the totality of factors. As a result, it is possible that the practitioner will be missing integral information due to the omission of questions or the patient’s embarrassment in responding to sensitive questions.
Recent years have brought great advances both in techniques and materials, especially in esthetic restorative dentistry.18-22 An increasing number of individuals are seeking this type of dentistry not only because of increased oral and dentition needs but also to satisfy their personal, psychological, and emotional goals. Many techniques, especially those associated with veneers, require little tooth preparation and therefore result in minimal discomfort. However, dental practitioners often have encountered patient reluctance and stress23,24 when attempting to incorporate these cosmetic procedures into treatment plans. This may be attributed to the lack of information obtained during initial patient interviews or the self-reported initial questionnaires that practitioners frequently use. Recently, when taking patients’ histories in the Esthetic Clinic of Tufts University School of Dental Medicine (TUSDM), it was noted that despite a lack of fear of dental treatment, some patients were reluctant to consent to this type of advanced cosmetic dentistry in their treatment plans. Efforts to determine if any prior negative trauma, experiences, or practitioner attitudes were influencing these avoidance tendencies produced little information. Other factors not associated with treatment might be responsible, such as personality traits, emotional or compulsive disorders, history of abuse, and other issues representing situations that may not be obvious but impact opinions on treatment more than actual past treatment-related experiences.
Objective
This study was undertaken to identify previously unrecognized sources of fear and anxiety in patients seeking esthetic dental treatment. Those factors that previous studies have determined to be treatment barriers, such as prior trauma and fear of the needle and the sound of the drill, were purposely omitted from the questionnaire in an attempt to prevent these known variables from overshadowing other contributors to the avoidance of dental care. It was also of interest to ascertain whether age, gender, and type of procedure were related to the response.
Materials and Methods
Initially, 25 patients from the TUSDM esthetic clinic in Boston, Massachusetts were asked to state their primary concerns associated with esthetic dental treatment in an open-ended question format. In addition, faculty members from the esthetics clinic provided questions that they thought were particularly relevant. After eliminating redundancies and topics that have well-established links to fears and concerns, 24 questions remained. These items were aggregated to comprise the Dental Esthetic Anxiety Questionnaire (DEAQ), with each item being scored on a 0 to 5 Likert scale: 0 = “not at all anxious” and 5= “avoid completely.” All participants gave written informed consent, were told of the purpose and goals, and assured anonymity. This project was approved by the Tufts University Health Sciences Campus Institutional Review Board.
The study coordinator provided each patient with the questionnaire and remained with the respondent to answer any questions that arose. Age and gender were recorded, as well as the type of procedure being considered: implants, porcelain veneers, anterior crowns and bridges, and dentures.
Sample Size Calculation
With a sample size of 50, the authors expected a 95% confidence that the width of the interval will be no more than 0.13 (nQuery Advisor® 7.0, Statistical Solutions, https://www.statsol.ie). As a result, the enrollment of 62 patients allowed for a 20% attrition rate.
Statistical Analysis
For each of the 24 questions, the percentage of answers for each of the six choices was reported. The six-level Likert scale was also dichotomized (“not at all anxious,” “a little anxious,” and “moderately anxious” vs “markedly anxious,” “severely anxious,” and “avoid completely”) for further analysis. The associations between age and procedure and the scores from the 24 questions were compared using Fisher’s exact tests. Spearman rank correlation was used to explore the relationship between participant’s age and score. All P values < .05 were considered statistically significant. Analyses were performed using SAS® 9.2 software (SAS, https://www.sas.com).
Results
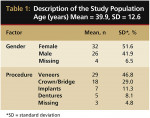
The mean (standard deviation) age was 39.9 (12.6) years. There were 32 women (51.6%) and 26 men (41.9%) (four people did not answer the question regarding gender). A total of 29 (46.8%) had been scheduled to receive veneer restorations, while 18 (29%) were to receive anterior crowns and bridges, 7 (11.3%) would receive implants, and 5 (8.1%) were contemplating obtaining dentures (3 people did not answer the question regarding the type of restoration contemplated) (Table 1).
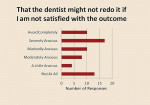
The item that elicited the highest level of anxiety pertained to “not feeling happy with my new smile.” Of the 62 respondents, 38 (61.3%) answered the question representing levels of concern: “markedly anxious,” “severely anxious” or “avoid completely” (Figure 1). Concerns that “the outcome might look false and unnatural” (Figure 2) and “the dentist might not redo it if I am not satisfied with the outcome” (Figure 3) both received 37 out of 62 (59.7%) responses: “markedly anxious,” “severely anxious,” or “avoid completely.” Concern that “the cosmetic dentistry cost will be more than I can afford” (Figure 4) was the next highest, with 35 out of 62 (56.5%) responding with “markedly anxious,” “severely anxious,” or “avoid completely.” The answers to the question about whether “the outcome might not be as hoped” (Figure 5) were “markedly anxious,” “severely anxious,” or “avoid completely” 54.8% of the time (34 out of 62). Please see Table 2 for complete breakdown.
The response pattern to most questions did not differ by age, gender, or type of procedure. However, women were much more likely than men to be concerned that “the outcome may look false and unnatural.” Of the 32 women, 25 (78.1%) answered with “markedly anxious,” “severely anxious,” or “avoid completely” as compared to the 26 men, of whom only 10 (38.5%) selected one of those three answers (P = .0425). Age was only associated with the concern “that my family and friends might not like my new smile.” There was a statistically significant negative association, suggesting that with increased age, the level of concern decreases (r = - 0.295, P = .021). The only item that demonstrated different responses by procedure was being anxious “thinking about the degree of discomfort associated with these procedures.” Patients with dentures were more likely to select the answer “avoid completely” (P = .0033).
Discussion
The advent of behavioral science and its marked and increasing emphasis in the curriculum of dental schools has led to greater observation and collection of information by practitioners, researchers, and students regarding patient behaviors in the dental environment. Numerous investigations1-7 demonstrate the multiplicity of variants that can trigger some form of anxiety and concern. The longer these feelings, thoughts, concerns, and emotions persist unexplained or ignored, the greater the chance of developing an emotional response that leads to negative behavior. Failure to collect all the information that makes an individual decide to enter into a particular situation may ultimately play a role in furthering and/or worsening already present negative thoughts and emotions. The responsibility for proper assessment and use of this acquired information or lack thereof depends directly on a practitioner’s acumen and willingness to take a thorough history of the patient’s physical and emotional health.14
Prior studies1-4,8,17 have demonstrated that various factors cause fear and treatment avoidance. These include prior trauma, patient satisfaction or dissatisfaction with treatment, practitioner/patient relationships, and personal reasons, as well as physical, psychological, and emotional disorders. Numerous studies have focused on all of the above; however, little attention has been directed toward those that include social, family, personal feelings affected by personality, embarrassment, guilt, concern about another’s opinion, practitioners’ reluctance to fully discuss treatment outcomes or listen to patients about goals and needs, and the negative effects on treatment. Seeking information concerning these factors is often either overlooked in the history taking or purposely not included in self-reporting patient questionnaires because some might consider these issues too sensitive to discuss and not pertinent to contemplated treatment.
As a result, this study was undertaken to determine if any of the items or situations presented by the DEAQ demonstrated significant levels of anxiety and concern among the participants and therefore warrant inclusion by dental practitioners at all levels in the armamentarium of history taking when patients are contemplating esthetic dentistry and other treatments. The DEAQ was constructed to incorporate many of these interpersonal emotions and factors that often cause an individual to deliberate and hesitate. Each item was constructed in simple terms so as not to evoke a strong negative feeling of intrusion into personal spaces. Many times, these emotions are hidden but exert a high degree of anxiety that actually overshadows any existing fear or anxiety regarding actual treatment. These factors, often considered insignificant, may act as the real obstacle to treatment because of a failure to recognize and designate any importance. In 2007, Goldstein24 studied attitudes and problems confronted by both patients and esthetic dentists that contributed to concerns, anxiety, and reluctance to consent to treatment. The most common factors were botched dentistry; overtreatment; high cost; unrealistic expectations; not knowing a patient’s true expectations; the media’s distorted images of beauty; failure to fully explain treatment and material limitations; and not fully understanding or listening to the goals, needs, and personality of the patient.
This study identified five factors that caused most of the respondents to answer: “markedly anxious,” “severely anxious,” or “avoid completely.” They were pertaining to possibly “not feeling happy with my new smile;” “the outcome might look false and unnatural;” “the dentist might not redo it if I am not satisfied with the outcome;” “the cosmetic dentistry cost will be more than I can afford;” and “the outcome might not be as hoped.”
Women were more likely than men to answer “markedly anxious,” “severely anxious,” or “completely avoid” when being concerned that “the outcome may look false and unnatural.” In addition, the younger patients were more likely to be concerned “that family and friends might not like new smile.” The data seem to indicate that a link does exist in a patient’s mind concerning situations and feelings that ought to be part of initial discussions and explanations, rather than ignored due to factors, such as embarrassment, fear of confronting a patient’s prior experiences, misconceptions, or a rush to initiate treatment. These factors, not fear of treatment, may be the actual barriers to complete optimal dental care.
Conclusions
All dental practices may have patients who experience fear and anxiety regarding actual and contemplated dental treatment. Much of these feelings may be caused by various individual factors that have been investigated and validated by numerous studies. This study, conducted at the TUSDM, has demonstrated barriers to treatment exist not only in those areas already abundantly investigated but also in emotional factors, situations, relationships, and personal feelings not often discussed during the patient-practitioner encounter. The failure to involve these in any initial discussion may be due to the patient fearing a practitioner’s response or concern that asking such questions might indicate a lack of mutual trust. The practitioner might believe that such personal concerns as to cost, opinions of the patient’s social contacts and family, or the patient’s final cosmetic goals are not as important as what the practitioner thinks he or she can accomplish. Experience has shown that even the smallest and seemingly most unimportant factor or emotion left unexplained and unattended can become a major obstacle to treatment compliance, as much as a prior trauma or past negative event. More detailed studies, combined with continual education at all levels of the dental profession, will shed greater light on this phase of behavioral patient management, aiding in reducing and ameliorating the anxiety and concern associated with dental treatment.
Clinical Implications
This study suggests there may be factors previously unrecognized that cause patients’ fear and anxiety and result in the delay or avoidance of esthetic dentistry. Practitioners should be keenly attuned with the patient and willing to explore the totality of information that is motivating the patient, including all physical, psychological, and emotional considerations, both past and present.
References
1. Weiner AA. The basic principles of fear, anxiety and phobias as they relate to the dental visit. Quintessence Int Dent Dig. 1980; 11:119-123.
2. Forgione AG, Clark RE. Comments on an empirical study of the causes of dental fear. J Dent Res. 1974;53(2):496-499.
3. Milgrom P, Coldwell SE, Getz T, et al. Four dimensions of fear of dental injections. J Am Dent Assoc. 1997;128(6):756-766.
4. Corah NL. Development of a dental anxiety scale. J Dent Res. 1969;48(4):596.
5. Corah NL, Zielezny MA, O’Shea RM, et al. Development of an interval scale of anxiety. Anesth Prog. 1989;33(5):220-224.
6. Weiner AA. Dental anxiety: an efficient means of identification. J Mass Dent Soc. 1988;38(2):75-79.
7. Weiner AA, Sheehan DV. Differentiating anxiety-panic disorders from psychologic anxiety. Dent Clin North Am. 1988;32 (4):823-842.
8. Weiner AA, Weinstein PW. Dentists’ knowledge, attitudes, and assessment practices in relation to fearful patients: a pilot study. Gen Dent. 1995;43(2):164-168.
9. Tay KM, Winn W, Milgrom P, et al. Effects of instruction on dentists’ motivation to manage fearful patients. J Dent Educ. 1993;57(6):444-448.
10. Heaton LJ, Carlson CR, Smith TA, et al. Predicting anxiety during dental treatment using patients’ self-reports. Less is more. J Am Dent Assoc. 2007;138(2):188-194.
11. Smith TA, Heaton LJ. Fear of dental care: are we making any progress? J Am Dent Assoc. 2003;134(8):1101-1108.
12. Corah NL, O’Shea RM, Ayer WA. Dentists’ management of patients’ fear and anxiety. J Am Dent Assoc. 1985;110(5):734-736.
13. Weiner AA, Moore PA, Sheehan D. Current behavioral modes for reducing dental anxiety. Quintessence Int Dent Dig. 1982;13 (9):981-985.
14. Corah NL. Reduction of patient stress and the patient-dentist relationship. NY State Dent J. 1984;50(8):478-479.
15. Corah NL, O’Shea R, Bissell G, et al. The dentist-patient relationship: perceived dentist behaviors that reduce patient anxiety and increase satisfaction. J Am Dent Assoc. 1988;116(1):73-76.
16. Pawlicki RE. Psychological/behavioral techniques in managing pain and anxiety in the dental patient. Anesth Prog. 1991;38(4-5): 120-127.
17. Centore L, Reisner L, Pettengill C. Better understanding your patient from a psychological perspective: early identification of problem behaviors affecting the dental office. J Calif Dent Assoc. 2002;30(7):512-519.
18. Carlsson GE, Johansson A, Johansson AK, et al. Attitudes toward dental appearance in 50- and 60-year-old subjects living in Sweden. J Esthet Restor Dent. 2008;20(1):46- 55.
19. Jørnung J, Fardal Ø. Perceptions of patients’ smiles: a comparison of patients’ and dentists’ opinions. J Am Dent Assoc. 2007; 138(12):1544-1553.
20. Mack MR. Perspective of facial esthetics in dental treatment planning. J Prosthet Dent. 1996;75(2):169-176.
21. Gurel G. The science and art of porcelain laminate veneers. Quintessence. 2003;7:246.
22. Papasotiriou OS, Nathanson D, Goldstein RE. Computer imaging versus conventional esthetic consultation: a prospective clinical study. J Esthet Dent. 2000;12(2):72-77.
23. Waliszewski M, Shor A, Brudvik J, et al. A survey of edentulous patient preference among different denture esthetic groups. J Esthet Rest Dent. 2006;18(6):352-369.
24. Goldstein RE. Attitudes and problems faced by both patients and dentists in esthetic dentistry today: an AAED membership survey. J Esthet Rest Dent. 2007;19(3):164-170.
About the Authors
Arthur A. Weiner, DMD
Professor
Department of General and Behavioral Dentistry
Tufts University School of Dental Medicine
Boston, Massachusetts
Paul C. Stark, MS, ScD
Associate Professor
Department of Research Administration
Director of Advanced and Graduate Studies
Tufts University School of Dental Medicine
Boston, Massachusetts
Joan LaSalvia, DDS
Assistant Professor
Department of Prosthodontics and Operative Dentistry
Division of Operative and Esthetic Dentistry
Tufts University School of Dental Medicine
Boston, Massachusetts
Matthew Navidomskis, DMD
Research Assistant
Tufts University School of Dental Medicine
Boston, Massachusetts
Gerard Kugel, DMD, MS, PhD
Professor
Department of Research Administration
Associate Dean for Research
Tufts University School of Dental Medicine
Boston, Massachusetts