Interdisciplinary Treatment of an End-to-End Occlusion Due to Congenitally Missing Maxillary Lateral Incisors
Odontogenic aplasia, or the congenital absence of permanent teeth, is relatively common. When the missing teeth include the maxillary lateral incisors, treatment considerations must reconcile both esthetic and functional objectives. In developing dentition, erupting adjacent teeth can drift from their intended positions into the edentulous space created by the congenitally missing tooth. When this movement happens (eg, cuspids shifting more mesially than normal), esthetic and functional problems occur. A restorative solution for missing maxillary lateral incisors subsequent to the loss of the maxillary incisor spaces is presented while highlighting the use of a leucite-reinforced material. This approach allowed for a minimal preparation design and conservation of tooth structure, providing an optimal bond.
Analytic determination of the proper treatment is an important step in any dental therapy. One such con dition, congenitally missing maxillary lateral incisors, requires practitioners to choose from an array of treatment options to obtain optimal results. Proper retainment of the missing tooth space with subsequent restorative treatment is considered possible in some cases.1 This solution can be achieved conservatively using a bonded bridge or an implant and crown.1
When spaces between dentition are closed through orthodontics or natural forces following tooth loss, the resultant mesial drift of the maxillary dentition can create inappropriate esthetics.2 This drift may also produce future functional occlusion issues.3,4 The smile presentation can appear improper due to inconsistent tooth morphology.5For example, differences between a lateral incisor and cuspid include significantly different crown dimensions, contours, incisal embrasures, and periodontal relationships.5
When the maxillary cuspids migrate mesially, interaction with the mandibular cuspids for appropriate anterior guidance is lost.6 Destructive wear of other anterior teeth occurs as the teeth assume additional responsibility.6 The shorter maxillary arch circumference, due to the missing teeth, can result in an interarch discrepancy, compromising the occlusal relationship.7,8 A size mismatch between the maxillary and mandibular arches can place opposing dentition in functional paths, also causing destructive wear.7,8 The clinician should treat the condition when the patient is a young adult because treatment options are time-sensitive.9
Sometimes an ideal resolution, such as re-establishing lost space with an implant or prosthodontic solution, is impossible.9 Therefore, alternative restorative choices must be considered. In such cases, the restorative material must allow conservation of tooth structure.10 One such option enables recapturing of the tooth’s natural biomimetic characteristics, while still providing optimal bonding.10
Case Report
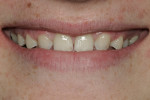
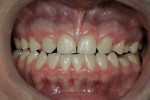
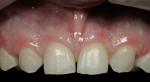
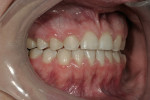
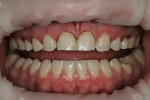
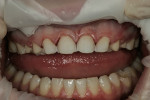
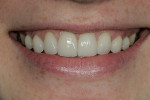
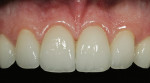
A 17-year-old female with a noncontributory medical history presented with congenitally missing maxillary lateral incisors (Figure 1, Figure 2, Figure 3 ). The patient was starting college in a year and wanted an attractive smile. Previous orthodontic care had aligned the remaining maxillary dentition mesially, in an attempt to eliminate the space created by the missing incisors. The resultant constriction of the maxillary arch circumference and end-to-end occlusal relationship left the patient disappointed with the esthetics.
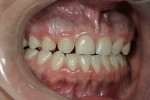
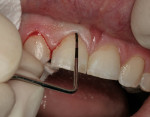
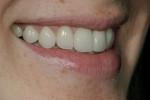
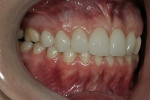
A clinical examination revealed that the end-to-end occlusal relationship was causing significant enamel loss from insufficient anterior guidance in lateral functional movements (Figure 4 and Figure 5).7,8 This loss was caused by mesial migration of the maxillary cuspids.6 The risk of incurring further wear to these teeth over time was great, and the oral health ramifications of nontreatment were unacceptable.7, 9
Clinical Discussion and Treatment Plan
Because the patient’s root morphology was compromised and exhibited foreshortening, any extensive orthodontic plan was quickly eliminated from consideration.5 After discussing the case, the orthodontist and dentist determined that a risk-free, limited orthodontic protocol was the best option.11,12 This plan entailed the creation of a more natural horizontal relationship between the maxillary and mandibular arches by bringing the mandibular incisors back and flaring the maxillary anteriors facially.13 Then, the interproximal spaces would be filled by conservatively prepared porcelain veneers.13
The increased circumference of the upper arch, with decreased circumference of the mandibular arch, would also provide room for natural height and width ratios, a proportionate balance of the maxillary incisors, and elimination of the crossbite of teeth Nos. 6 to 27. The orthodontic treatment would be 12 months (Figure 6).11,12 The procedure would then be completed to an esthetic and functional finish using indirect porcelain restorations (Figure 7).13
Laboratory Discussion
When considering a restorative material, the technician should think from the “outside in.” Whether dentine, porcelain, or composite, any optically dense material must be covered by a minimum of 0.5 mm of translucent enamel material and provide a color depth.14 If little-to-no enamel reduction has occurred, a technician needs only to replace the missing enamel, allowing the colors and effects of the natural tooth to be expressed.14 Feldspathic veneers are the obvious choice in these cases because the ceramist has the greatest ability to vary the amount of filtering, or expression, of the underlying color and character.15
However, the greater the tooth reduction, the more difficult it is to make a restoration appear natural.15 If teeth are overprepared, all internal structures and characteristics must be layered in ceramic, prior to layering the enamel.14This requires greater skill and knowledge but allows for the utmost number of options when choosing restorative materials.15 Any system with dentine and enamel materials, such as IPS e.max® (Ivoclar Vivadent, https://www.ivoclarvivadent.com), porcelain fused to metal, or high-strength ceramics (LAVA®, 3M ESPE, https://www.3mespe.com), will suffice.15
Product Description
Conservative preparation of teeth for restorations should be the goal of all dentistry. Three-quarter crowns and veneers, with finishing lines in enamel, are functionally equal to crowns but allow for conservation of tooth structure.14,15 In cases that require greater than 0.5 mm of restorative material, a hybrid material that combines the optics of dentine and enamel is the obvious choice.14,15 Leucite-reinforced glass-ceramic restorations show a low clinical failure rate and excellent esthetics, even beyond 11 years.15
IPS Empress® Esthetic (Ivoclar Vivadent) is a leucite-reinforced, pressable ceramic that fits the functional and esthetic requirements of restorative cases.15 While a feldspathic option was considered in this case, the functional changes to the patient’s occlusal scheme necessitated the use of a high-strength material.14,15 The color, clarity, strength, and leucite distribution of IPS Empress Esthetic contributed to improved strength and superior optical properties compared with other materials used for metal-free restorations.15 Leucite-reinforced restorative materials, such as IPS Empress Esthetic, allow practitioners to create pressed and layered restorations that mimic the beauty of natural dentition, while still enabling conservation of the tooth structure.14,15
Pressable ceramics also have the advantage of being the most predictable material for managing interdental spaces—when tissue is blunted or tissue and tooth morphologies are dissimilar.14,15 In this case, the IPS Empress Esthetic ingot ETC-0 provided a natural blend of translucency and color filtering, creating a slightly brighter esthetic result.14,15
The challenge presented by pressable ceramics, however, is in disguising the interface between the more optically dense ingot material and the translucent enamel veneering materials.14,15 The typical approach has been to “cut in” internal incisal structures by shaping the pressed restoration during cutback for veneering enamel. Layering this area with transparent material alone can result in a manufactured-looking incisal zone.14,15 IPS Empress Esthetic was chosen for its combination of enhanced strength and complementary veneering ceramics, which allowed management of the transitional incisal zone.14,15
Restorative Treatment
The treatment plan involved minimally prepared, additive leucite-reinforced porcelain restorations. This restoration would apply to eight teeth, ranging from a veneer for tooth No. 4 to a full crown for the microdontic tooth No. 13.
The need for a stronger material to fill the incisal embrasures was the main reason IPS Empress Esthetic was chosen.15 Due to the morphologic changes with increased crown length (Figure 8 and Figure 9) and additional bulk in the incisal embrasures, the leucite-reinforced material provided increased strength compared to feldspathic glass.14,15
Another benefit of the leucite material was the ability to keep the restoration thickness minimal (Figure 10).14,15 This prevented preparing the tooth past the dentoenamel junction, leaving nearly 100% of the enamel surface to bond the restoration (Figure 11 and Figure 12).14,15
Conclusion
The authors advocate the use of leucite-reinforced porcelain when adding facial contours because it allows for sufficient restoration thickness without the need to prepare through the enamel.15 This “additive technique” takes advantage of the increased tensile strength of the leucite-reinforced hybrid.15 In the case presented here, because the shapes of the teeth were changing from cuspids to laterals and first bicuspid to a larger cuspid, a thicker layer of porcelain was needed to fill the incisal embrasures (Figure 13, Figure 14, Figure 15).14 Therefore, a stronger and more translucent material was employed.
As mentioned, dental teams are presented with myriad choices of restorative materials and CAD/CAM options have complicated the landscape further. While material decisions are always important, proposed changes to a patient’s habitual occlusion make these choices even more crucial. Esthetics, while still the driving force behind cases involving restorations in the anterior segment, must be considered in combination with resistance to impact because patients may not be accustomed to their new functional movements (Figure 16, Figure 17, Figure 18).
Acknowledgment
The authors thank Ross L. Crist, DDS, MS, for expertly completing the interdisciplinary orthodontic care, which helped accomplish the case objectives.
References
1. Laing E, Cunningham SJ, Jones S, et al. Psychosocial impact of hypodontia in children. Am J Orthod Dentofacial Orthop. 2010;137(1):35-41.
2. Heij DG, Opdebeeck H, van Steenberghe D, et al. Facial development, continuous tooth eruption, and mesial drift as compromising factors for implant placement. Int J Oral Maxillofac Implants. 2006;21(6):867-878.
3. van Beek H. Dissertations 25 years later. 1. Mesial drift of teeth by occlusal forces. Ned Tijdschr Tandheelkd. 2004;111(2):48-51.
4. van Beek H, Fidler VJ. An experimental study of the effect of functional occlusion on mesial tooth migration in macaque monkeys. Arch Oral Biol. 1977;22(4):269-271.
5. Townsend G, Harris EF, Lesot H, et al. Morphogenetic fields within the human dentition: a new, clinically relevant synthesis of an old concept. Arch Oral Biol. 2009;54(suppl 1):S34-S44.
6. Sayin MO, Türkkahraman H. Effects of lower primary canine extraction on the mandibular dentition. Angle Orthod. 2006;76(1):31-35.
7. Chen LL, Xu TM, Jiang JH, et al. Longitudinal changes in mandibular arch posterior space in adolescents with normal occlusion. Am J Orthod Dentofacial Orthop. 2010;137(2):187-193.
8. Tsai HH, Tan CT. Positional changes of the upper canine and posterior teeth, hard palate, and sinus floor from primary to permanent dentition. J Dent Child (Chic). 2004;71(1):48-53.
9. Strong SM. Replacement of congenitally missing lateral incisors with implant crowns. Gen Dent. 2008;56(6):516-519.
10. Cerutti A, Barabanti N. New resin composites used to restore both anterior and posterior teeth. Br Dent J. 2005;198(7):447.
11. Vitályos G, Török J, Hegedus C. The role of preprosthetic orthodontics in the interdisciplinary management of congenitally missing maxillary lateral incisors: case report. Fogorv Sz. 2005;98(6):223-228.
12. Kokich VG. Maxillary lateral incisor implants: planning with the aid of orthodontics. J Oral Maxillofac Surg. 2004;62(9 suppl 2):48-56.
13. Hohlt WF, Hovijitra S. Management of anterior spacing with orthodontics and prosthodontics. J Indiana Dent Assoc. 1999;78(3):18-23.
14. Chun YH, Raffelt C, Pfeiffer H, et al. Restoring strength of incisors with veneers and full ceramic crowns. J Adhes Dent. 2010;12(1):45-54.
15. Fradeani M, Redemagni M. An 11-year clinical evaluation of leucite-reinforced glass-ceramic crowns: a retrospective study. Quintessence Int. 2002;33(7):503-510.
About the Authors
Michael R. Sesemann, DDS
Private Practice
Omaha, Nebraska
Bradford Patrick, BSc
Owner
Patrick Dental Studio
Bend, Oregon