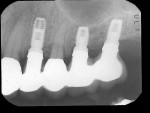
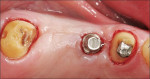
Connecting Teeth to Implants: A Critical Review of the Literature and Presentation of Practical Guidelines
Gary Greenstein, DDS, MS; John Cavallaro, DDS; Richard Smith, DDS; and Dennis Tarnow, DDS
Abstract
Historically, connecting a tooth to an implant to function as an abutment to replace a missing tooth was discouraged. It was believed differences in mobility patterns of a tooth and an implant would result in the prosthesis being cantilevered off the implant, thereby stressing the implant. Several papers concluded increased stress caused technical and biologic complications, which led to a decreased survival rate for a tooth-implant supported prosthesis (TISP) when compared with an implant-only supported prosthesis (ISP). However, problems attributed to TISPs may have been overstated. This paper reviews animal studies and human clinical trials that monitored successful use of TISPs. In addition, numerous issues are addressed that question the data, which have been interpreted to indicate that a tooth should not be connected to an implant. Recommendations are made to facilitate attaining high success rates with TISPs.
Pvariety of prosthetic techniques can be used to re store the dentition subsequent to loss of teeth. The method of rehabilitation depends on the num ber, arrangement, and status of residual teeth (eg, peri odontal health, remaining tooth structure); cost; patient de sires; and adequacy of the bone to support dental im plants. Historically, it was believed if a tooth and an implant were used as abutments in the same prosthesis, the implant would be subjected to an increased bending moment because of differences in their mobility patterns. This increased stress could lead to a decreased success rate for a tooth-implant supported prosthesis (TISP) compared with implant-only supported prosthesis (ISP).1-7 However, potential problems associated with TISPs may have been overstated. There fore, this article assesses the literature to determine if evidence-based decisions could be made concerning the utility of connecting teeth to dental implants.
Advantages and Potential Problems Associated with Connecting Teeth to Dental Implants
Broadening treatment possibilities is the main advantage in constructing a TISP (Figure 1). Other reasons a TISP may be advantageous are listed in Table 1. In contrast, some factors suggest it may be prudent to avoid a TISP. For example, a tooth with a healthy ligament can move 200 µm in response to a 0.1 N force, but an implant is displaced < 10 µm.8 This movement is primarily due to bone flexure.9 Therefore, if a three-unit TISP is functioning, differences in mobility patterns between a tooth and an implant could result in the tooth being depressed into the socket, which might cause the prosthesis to be cantilevered off the im plant.10 Theoretically, this could increase stress on the im plant and lead to both technical and biologic complications (Table 2).1,2,5,7 However, the precise biomechanical impact due to dissimilarity in mobility patterns remains controversial.11 In this regard, despite a 10-fold greater axial and transverse mobility of teeth compared to implants, mitigating factors may accommodate a TISP. For instance, bone has some natural elasticity12 and some resiliency is in components of implant assemblies.13-15 Also, a cushion effect may be provided by the cement layer within the prosthesis,16 and there may be force deflection in the suprastructure of the prosthesis.13,14 In addition, several studies indicated teeth in a TISP share the occlusal load and all the forces are not transferred to the implant.13,14 Therefore, to determine the utility of connecting teeth to implants, the data must be evaluated from different perspectives: theoretical concerns, technical and physiologic problems, and func tionality of TISPs over time.
Theoretical Complications Associated with a TISP
The concept that occlusal forces on a TISP result in the pros thesis being cantilevered off the implant was derived from finite elemental analysis and photoelastic stress studies.17,18 Finite element analysis (FEA) is a computerized-simulation technique used in engineering to assess stresses and strains on solid objects. It employs a numerical approximation of physical properties that can be modeled. However, extrapolating information from FEA studies to humans with re spect to stress distribution is difficult because many as sumptions are needed concerning biologic factors, such as bone properties, response to applied mechanical force, and stress distribution after force transmission.19-21 Furthermore, as will be discussed in this article, clinical trials that assessed po tential problems associated with TISPs did not usually dem onstrate the extent of problems predicted by FEA.
Technical Problems Related to TISPs
Technical complications include mechanical damage to the teeth or implants, implant components, and suprastructures (Table 2). It was assumed that a rigid connection be tween an implant and a natural tooth would result in additional strain on the implant because the tooth could move in function. Therefore, the use of nonrigid connector or telescopic crowns was advocated to reduce the bending mo ments on the implant.22-35 However, this could result in oth er problems, namely tooth intrusion.
Intrusion of Teeth
When implants were connected to natural teeth to support a fixed partial denture, the incidence of tooth intrusion va r ied (movement of a tooth out of its crown in an apical di rection) (Figure 2).1,5,7,31,34-42 Surveys indicated intrusion occurred, on average, in 3% to 5.2% of the cases.1,29,32 An assessment by Reider and Parel29 found 50% of intrusions happened in individuals with parafunctional habits, specifically bruxism. They also noted it usually occurred in pa tients with non rigid semi-precision attachments.
Many authors reported that stress-breaking connectors were associated with more intrusion than rigid connections.1,5,34 Intrusion of teeth associated with nonrigid semi-precision attachments usually contained the female portion of the keyway in the natural tooth.29,43,44 Others reported no intrusion of teeth associated with rigid connectors.1,5,7,37,39,45-50 Rigid connection designs include soldered connectors, set screw connectors, and coping-sleeve methods.43 However, intrusion occurred in some patients with rigid connectors if telescopic crowns were used on abutment teeth.29,33,35,41 Several investigators also demonstrated when rigid connectors were used, results did not differ if restorations were screw- or cement-retained.35,48,51
In conclusion, the potential for intrusion of an abutment tooth cannot be ignored; however, it should not be a deterrent from connecting teeth to implants. This dilemma can be avoided by proper patient selection (avoidance of those with bruxism), use of rigid connectors, avoidance of placing copings on teeth used as abutments, proper abutment pre paration (parallel walls) to maximize retention and resistance form, and permanent cementation.52
Other Technical Complications Related to TISPs
The technical problems listed in Table 2 are dependent on bridge configurations and dimensions, tooth abutment preparation, employed cements, opposing dentition, kinds of screws used, types of implants, etc. Therefore, data from one study cannot be extrapolated with specificity to other patient populations or implant systems. However, trends can be observed; therefore, data from the literature are presented to provide an overview of reported complications.
Several studies noted more technical problems associated with TISPs than ISPs. For example, Naert et al5,6 monitored 140 ISPs and 140 TISPs (1 to 15 years) and concluded an ISP is preferable because of an increased number of technical problems associated with a TISP. The complication rate for a TISP was 5% to 10%. The incidences of some problems included periapical lesions (3.5%), tooth fracture (0.6%), extraction because of caries or periodontitis (1%), crown cement failure (8%), and framework fracture in three patients. In contrast, only two abutment screws fractured in the ISP group. However, these data can be mis leading because some ISPs had multiple implants providing additional overall support for the prosthesis compared with the TISPs.
Brägger et al7 reported that after 5 years, TISPs did not have a higher risk of technical or biologic complications compared with ISPs. However, after 10 years, TISPs had more failures than ISPs. In general, after a 10-year monitoring period, 11 out of 22 TISPs (50%) remained free of any technical and biologic complications, whereas 18 out of 33 ISPs (54.5%) had no technical or biologic problems.53 In contrast, other investigators reported only minor technical complications associated with TISPs34,36,39,52 or no differences when ISPs and TSPs were compared intraindividually.38,47,49 In this regard, Lang et al1 determined in their meta-analysis that most of the technical complications associated with TISPs (Table 2) occurred when there was a nonrigid connection between abutment teeth. They also concluded screw-retained restorations needed more maintenance than cemented crowns.
In summary, the literature indicates use of rigid connections between teeth and implants in a TISP usually reduces mechanical complications to a level that appears to be com parable with problems associated with an ISP. However, it needs to be noted that studies were conducted for various lengths of time (Table 3,5,7,31,34-38,44,47,49,51-63 Table 4,1,64,65 and Table 55,7,35,36,38,46,49,53,55,57,66,67) and many papers did not provide long-term follow-up on technical complications.
Biologic Complications Associated with TISP
Bone Loss
The amount of bone loss around abutments is often used as a critical determinant to evaluate the durability of TISPs and ISPs. To assess the prevalence of this occurrence, issues need to be discussed from four different points of view: con ceptual effect of occlusal load on bone loss, usual amount of osseous resorption around freestanding implants, bone loss around implants in an ISP, and bone loss around natural tooth abutments in a TISP.
Theoretical Concept: Occlusion Related to Bone Loss
The influence of occlusal forces on peri-implant bone was reviewed by Isidor.68 He concluded the literature had conflicting information as to whether overloading an implant can lead to implant failure, which can consist of progressive bone loss or total deosseointegration. It was also noted that animal studies have shown occlusal load may contribute to complete loss of osseointegration69 or marginal bone loss.70 However, in hu man clinical investigations, de spite many authors referring to occlusal trauma as a cause for implant loss,3,11,50,67,71,72 others indicated this relationship has not been clearly demonstrated.2,68,73-76 A review by Vidyasagar and Apse77 reached the same conclusion as Isidor. Therefore, it can be summarized that in some situations, occlusal forces may affect the bone around implants; however, numerous confounding variables (eg, density of bone, strength of loading force) make it difficult to delineate the circumstances when this occurs.
Clinical Trials Assessing Bone Loss around Freestanding Implants
Studies noted the mean bone loss around freestanding dental implants ranged from 0.14 mm to 1.6 mm (mean 0.93 mm) during the first year and subsequently 0 mm to 0.2 mm annually (mean 0.1 mm).49,50,59,71,72 Therefore, the question is whether stress placed on an implant connected to a tooth would result in more bone resorption than is ex pected normally around a freestanding implant.
Clinical Trials Assessing Bone Loss around TISP
Bone loss that occurred around the implants incorporated in to a TISP was discussed by Naert et al.6 They reported more bone resorption around rigid than around nonrigid connectors. However, the total additional bone loss (0.7 mm) oc curred over 15 years. This amount of bone loss is within the acceptable standards established by Albrektsson et al.78 Their criteria was < 1.5-mm bone loss the first year after implant insertion followed by < 0.2-mm per year in subsequent years. Kind berg et al36 also observed minor bone loss around abutment teeth and implants after 1 year, with a few exceptions.
Akça et al54 conducted a study to evaluate the findings by Naert et al.6 They concluded a rigid connection did not jeopardize the marginal bone levels around dental implants and the bone re mained stable after 2 years of function.54 Similarly, Hosny et al38 determined the amounts of marginal bone loss around freestanding and tooth-connected implants did not differ significantly. They reported 1 mm of bone loss in the first 3 to 6 months after abutment connection and then 0.015 mm annually for 14 years. Stable bone levels around the im plants suggest excessive loads to the implants did not occur when they were connected to teeth. Gunne et al49 and Lindh et al34 also reported bone resorption around implants incorporated in a TISP was similar to bone loss adjacent to im plants in an ISP when assessed within the same individual.
In another study, Block et al35 reported no difference in the amount of bone loss around implants that employed a rig id or nonrigid connection. They noted teeth around a rigid connection tended to lose more bone; however, the amount of bone resorption was within the criteria defined as success by Albrektsson et al.78 Other investigators also did not re port any bone resorption after construction of a TISP.39,52,55
In conclusion, the amount of bone degradation around dental im plants used as abutments after teeth and implants are con nected is usually within a range of acceptable bone loss for freestanding implants. Therefore, these data indicate that bone resorption around a TISP is not excessive.
Endodontics
The literature contains limited and conflicting data that addresses inclusion of abutment teeth with endodontic therapy in a TISP; therefore, no conclusions can be drawn regarding the affect of root canal therapy on survivability of a TISP.34,35,53 Furthermore, with respect to survival of endodontically treated teeth, it should also be noted that other clinical factors that may influence their retention were not recorded: amounts of remaining tooth structure or the presence of a reinforcing ferrule around the endodontically treated teeth.79
Animal and Human Clinical trials Assessing the Utility of TISPs
Several lines of evidence can be assessed to help evaluate the predictability of employing a TISP. Animal studies provide histologic data that are difficult to obtain in humans, and clinical trials supply comparisons of efficacy of TISP and ISP over a prolonged period.
Based on animal studies80-83 that provided histologic evidence, the following conclusions can be drawn: teeth connected to implants in a TISP did not usually undergo periodontal ligament atrophy,82 bone around teeth was able to remodel under stress caused by the bridgework,81 a TISP usually functioned as well as a bridge supported by natural teeth, and, if rigid connections are used, these constructions functioned successfully.80,83 However, these re sults need to be interpreted with regard to the length of the observation periods, which were relatively short.
Human Clinical Trials: Evidence Supporting Use of Connecting Implants to Teeth
A high level of evidence supporting the use of TISPs is de rived from investigations that assessed their functionality for many years. In this regard, numerous studies indicated implants can be splinted to teeth and function successfully (Table 3). Different types of studies have been conducted: a limited number of clinical trials compared same-sized TISP and ISP intraindividually, comparisons of dissimilarly sized TISP and ISP intraindividually, comparisons of different-sized ISPs and TISPs in various patient populations, and case reports assessing various combinations of im plants and teeth. In addition, a meta-analysis can summarize trends demonstrated by similar studies employing comparable treatment methods.
Meta-analyses in the Literature Assessing Success of Fixed Prostheses
Systematic reviews addressed the survivability of prostheses supported by teeth alone,64 implants alone,65 and TISPs1 (Table 4). Comparison of results with respect to implant and prostheses survivability indicate for the first 5 years, no disadvantage is associated with fabricating a TISP (Table 5). Yet, by the tenth year, a TISP has a reduced survival rate when compared with an ISP or a tooth-supported prosthesis (Table 5). However, careful inspection of the data used in the meta-analysis to assess TISPs after 10 years reveals many shortcomings of the analysis.1 Specifically, the analysis included only three studies (60 patients) because of its ex clusion criteria.1 Furthermore, these data are based on prostheses supported by the following implant systems that are not used anymore or their surfaces have been improved: 22 prostheses with ITI implants (placed before 1990, thus the titanium plasma spray surface is outdated), 23 cases with machined-surfaced implants, and 15 prostheses using Bio ceram® sapphire implants (Kyocera Corporation, Kyoto, Japan). Therefore, with regard to bone loss, prosthesis failure, or implant survivability, the data used in the metaanalysis may not be relevant to contemporary implants with better surfaces, such as textured. Furthermore, im proved technologies with respect to casting, porcelain ma terials, etc, may enhance prosthesis survivability.
Other issues also remain unresolved. For instance, Lang et al1 performed a meta-analysis to specifically determine the survivability of TISPs. They found the survival rate was similar after 5 years for an ISP and a TISP, but a TISP had a reduced survival rate between the fifth and tenth years (Table 5). However, after 10 years, Lang et al1 did not find a significant difference in the failure rates of abutment teeth or implants in the TISP group (respectively, 5 out of 47, 10.6%, vs 7 out of 45, 15.6%). Thus, they concluded some thing other than loss of abutment teeth contributes to the additional loss of prostheses in the TISP group. However, they could not identify a reason.
Studies Addressing Survivability of Prostheses
Controlled Clinical Trials:Intraindividual Studies
Gunne et al conducted a randomized, controlled study that compared the use of TISPs vs ISPs (N = 10, 20 prostheses).49 They assessed contralateral three-unit constructions for 10 years; one mandibular posterior side received a three-unit TISP and the other side had a three-unit ISP. They reported that TISPs did not result in increased technical or biologic problems. No statistically significant differences were found with regard to implant failure rate or bone loss. The total marginal bone loss for TISP and ISP was 0.5 mm and 0.6 mm to 0.7 mm, respectively. Implants that were 7-mm long were as effective as 10-mm implants, and most of the ISPs were cantilevered bridges. The opposing dentition was a denture. This was a small study and lacked adequate power to find small differences between the test and control groups.1 Data related to this one cohort of patients were published at three different times: 3 years,63 5 years,46 and 10 years.49
Block et al35 placed 60 TISPs contralaterally in 30 pa tients and compared rigid with nonrigid connections. Af ter 5 years, no significant difference in crestal bone levels on the implants were noted with either type of connection and most patients were treated successfully with both kinds. However, the two groups had a high incidence of intrusion because of the use of temporary cementation. In addition, patients with nonrigid connections needed more maintenance visits. The high incidence of tooth intrusion and ad ditional visits for maintenance led to the authors suggesting that other treatment methods that do not connect teeth to implants may be needed. However, they mentioned a conventionally cemented prosthesis with an extremely retentive preparation may have overcome the high incidence of intrusion that they experienced.
Hosny et al38 monitored different combinations of abutment teeth: single tooth and single implant, multiple teeth connected to an implant, and multiple implants connected to a tooth. A total of 18 patients received either TISPs (test group) or ISPs (control group), each within the same jaw. No prostheses demonstrated adverse results. The cases (12 maxillary and six mandibular prostheses) were monitored 1 to 14 years. No implants were lost, and no differences in marginal bone loss were observed between the treatment groups.
Lindh et al47 conducted a 2-year follow-up of various max illary prostheses (N = 26 patients). One side received an ISP and the other a TISP. Different prostheses sizes were fabricated depending on patients’ needs. The researchers found no difference in the failure rate of implants (88% cumulative survival rate) with different prosthetic designs and no additional bone loss with the TISP.
Controlled Clinical Trial: Different Patient Populations Were Compared
Brägger et al7 for a 4- to 5-year period monitored two pa tient groups: 40 ISPs and 18 TISPs. Loss of prostheses occurred at the same rate in both groups (each group lost one prosthesis). Survivability after 5 years was 97.5% (ISP) vs 95% (TISP). However, after 10 years, the survivability of the prostheses was significantly better with an ISP (93.9%, 31 out of 33) than a TISP (68.2%, 15 out of 22).53 The main reason for the difference between 5 and 10 years was because of loss of crown retention on teeth, which led to car ies and subsequent failure of four abutments, resulting in loss of four prostheses. The 10-year follow-up included only 22 prostheses, thus a small number of lost abutments (four carious teeth) translated into a large percentage of failed prostheses. Furthermore, most of the lost tooth abutments were nonvital teeth restored with a cast post and core.
Naert et al5 also monitored patients with ISPs (140 pros theses, 123 patients) and TISPs (140 prostheses, 123 pa tients). The loading time for TISP was 1.5 years to 15 years (mean 6.5 years) and ISP was 1.3 years to 14.5 years (mean 6.2 years). The cumulative success rates of the implants for ISPs and TISPs were 98.5% and 95%, respectively. There were no significant differences with regard to loss of im plants even though more implants were lost with TISP (10 out of 339 TISPs vs one out of 329 ISPs). With regard to the cumulative success rate of the prostheses, no statistically significant differences between ISP (98.4 %) vs TISP (94.9%) were noted.
Nickenig et al48 compared rigid (n = 56) and nonrigid connections (n = 28) in various sizes of TISPs (84 prostheses, 83 patients), which were in service 2.2 years to 8.3 years (mean 4.73 years). Brånemark System® (Bio-Dent Labora tories, Ontario, Canada) and Straumann (Andover, MA) implants were used. After 5 years, 8% of the abutment teeth needed a therapeutic measure, eg, periodontal therapy (5%) or restoration (2.5%). However, the researchers found an increased incidence of technical problems was usu ally associated with nonrigid connections. Among the TISPs with rigid connections, only three out of 56 prostheses had technical problems. The authors concluded TISPs with rigid connection provided a high success rate.
Case Reports
In 1997, Gross and Laufer45 addressed splinting implants to natural teeth in a review paper and concluded this should be approached cautiously. However, they noted if the teeth were well supported, immobile, and positioned close to the implant, a TISP was not destructive. They reported root in trusion was a problem when nonrigid connectors were used and cited numerous studies that monitored patients with successful TISPs.24,44,62,67 Table 3 includes an additional 11 studies addressing successful splinting of teeth to im plants not mentioned by Gross and Laufer45 or published after their review.24,31,36,37,39,47,51,52,54,58,60
Conclusion
Despite the fact that the potential mobility between a tooth and an implant are different and the precise etiology of tooth intrusion is unknown, it is reasonable to rigidly connect a tooth to an implant. This is particularly true if the anatomy dictates that placement of an additional implant(s) is contraindicated or if there are economic concerns. This deduction is based on almost every study that addressed this issue and found the survival rates were similar when TISPs and ISPs were compared. At present, there are no large long-term studies that assessed textured surface im plants as an integral part of a TISP.
The literature supports the idea that a rigid connection between a tooth and an implant usually precludes intrusion of teeth. The following guidelines can help prevent intrusion of teeth (items 1 to 9) and enhance patient care when contemplating fabricating a TISP.
- Select healthy teeth—periodontally stable and in dense bone.
- Rigidly connect the tooth and implant (no stress breakers), employ large solder joints to enhance rigidity (Figure 3), or use one-piece castings.
- Avoid telescopic crowns (no copings) (Figure 4a and Figure 4b).
- Provide retention form with minimal taper of axial walls on abutment teeth. Enhance resistance form with boxes and retention grooves if the clinical crown is not long (Figure 5).
- Parallel the implant abutment to the preparation of the tooth and use a rigid connection.
- Use permanent cementation (no screw retention or tem porary cementation).
- The bridge span should be short. Preferably, place one pontic between two abutments. However, with additional tooth or implant support or cross-arch stabilization, additional pontics can be used.
- Occlusal forces should be meticulously directed to the opposing arch (Figure 6).
- In general, do not use TISPs in patients with parafunctional habits. If they are treated with TISPs, overengineer the case by maximizing the number of implants and splinting.
- Cantilever extensions should be used cautiously; however, they may be employed when tooth or implant support is adequate, eg, cantilever-implant-implant-pontic-tooth-tooth (Figure 7).
- TISPs in patients with uncontrolled caries should be avoided; ISPs are preferred (Figure 8).
- Pulpless teeth with extensive missing coronal tooth structure or root canal anatomy that is inadequate to predictably retain a core or post and core should not be used in a TISP.
- High-risk TISPs (eg, multiple adjacent pontics, double cantilevered pontics) or prostheses with minimal abutment support should be expected to have a higher failure rate even though these treatment plans may benefit certain patients (Figure 9 and Figure 10).
- In the esthetic zone, if a papilla or papillae is crucial for esthetics or function (eg, phonetics), consider us ing natural teeth (TISPs) because the supracrestal gingival fibers associated with healthy teeth will provide interproximal soft-tissue support (Figure 11).
- If appropriate case selection principles are applied (eg, minimal caries rate, good root anatomy, minimal tooth mobility, adequate retention and resistance form, rigid prosthesis design, adequate overall abutment support for the prosthesis), then combining implants and natural teeth may permit segmentation of a prosthesis into smaller sections, which may provide an alternate treatment plan to a large one-piece bridge.
References
1. Lang N, Pjetursson B, Tan K, et al. A systematic review of the survival and complication rates of fixed partial dentures (FPDs) after an observation period of at least 5 years. II. Combined tooth-implant-supported FPDs. Clin Oral Implants Res. 2004;15(6): 643-653.
2. Lang NP, Wilson TG, Corbet EF. Biological complications with dental implants: their prevention, diagnosis and treatment. Clin Oral Implants Res. 2000;11(suppl 1):146-155.
3. Naert IE, Quirynen M, van Steenberghe D, et al. A six-year pros thodontic study of 509 consecutively inserted implants for the treatment of partial edentulism. J Prosthet Dent. 1992;67(2):236-245.
4. Naert I, Koutsikakis G, Duyck J, et al. Biologic outcome of single-implant restorations as tooth replacements: a long-term follow-up study. Clin Implant Dent Relat Res. 2000;2(4):209-218.
5. Naert IE, Duyck JA, Hosny MM, et al. Freestanding and tooth-implant connected prostheses in the treatment of partially edentulous patients. Part I: an up to 15-years clinical evaluation. Clin Oral Implants Res. 2001;12(3): 237-244.
6. Naert IE, Duyck JA, Mahmoud M, et al. Freestanding and tooth-implant connected prostheses in the treatment of partially edentulous patients. Part II: an up to 15-years radiographic evaluation. Clin Oral Implants Res. 2001;12(3):245-251.
7. Brägger U, Aeschlimann S, Bürgin W, et al. Biological and technical complications and failures with fixed partial dentures (FPD) on implants and teeth after four to five years of function. Clin Oral Implants Res. 2001;12(1):26-34.
8. Cohen SR, Orenstein JH. The use of attachments in combination implant and natural-tooth fixed partial dentures: a technical report. Int J Oral Maxillofac Implants. 1994;9(2):230-234.
9. Brunski JB. Biomaterials and biomechanics in dental implant design. Int J Oral Maxillofac Implants. 1988;3(2):85-97.
10. Renouard F, Rangert B. Risk Factors in Implant Dentistry: Simplified Clinical Analysis for Predictable Treatment. 1st ed. Han over Park, IL: Quintessence Publishing Co. Inc.; 1999:43.
11. Kim Y, Oh TJ, Misch CE, et al. Occlusal considerations in im plant therapy: clinical guidelines with biomechanical rationale. Clin Oral Implants Res. 2005;16(1):26-35.
12. Smith JW, Walmsley R. Factors affecting the elasticity of bone. J Anat. 1959;93: 503-523.
13. Rangert B, Gunne J, Sullivan DY. Mechanical aspects of a Brånemark implant connected to a natural tooth: an in vitro study. Int J Oral Maxillofac Implants. 1991;6(2):177-186.
14. Rangert B, Gunne J, Glantz PO, et al. Vertical load distribution on a three-unit prosthesis supported by a natural tooth and a single Brånemark implant. An in vivo study. Clin Oral Implants Res. 1995;6(1):40-46.
15. McGlumphy EA, Campagni WV, Peterson LJ. A comparison of the stress transfer characteristics of a dental implant with a rigid or a resilient internal element. J Prosthet Dent. 1989;62(5): 586-593.
16. Pietrabissa R, Gionso L, Quaglini V, et al. An in vitro study on compensation of mismatch of screw versus cement-retained implant supported fixed prostheses. Clin Oral Implants Res. 2000;11(5):448-457.
17. Menicucci G, Mossolov A, Mozzati M, et al. Tooth-implant connection: some biomechanical aspects based on finite element analyses. Clin Oral Implants Res. 2002;13(3): 334-341.
18. Nishimura RD, Ochiai KT, Caputo AA, et al. Photoelastic stress analysis of load transfer to implants and natural teeth comparing rigid and semirigid connectors. J Prosthet Dent. 1996;81(6):696-703.
19. Geng JP, Tan KB, Liu GR. Application of finite element ana lysis in implant dentistry: a review of the literature. J Prosthet Dent. 2001;85(6): 585-598.
20. Lin CL, Chang SH, Wang JC, et al. Mechanical interactions of an implant/tooth-supported system under different periodontal supports and number of splinted teeth with rigid and non-rigid connections. J Dent. 2006;34(9):682-691.
21. Misch CM, Ismail YH. Finite element stress analysis of tooth-to-implant fixed partial denture designs. J Prosthodont. 1993;2(2): 83-92.
22. Sullivan, DY. Prosthetic considerations for the utilization of osseointegrated fixtures in the partially edentulous arch. Int J Oral Maxillofac Implants. 1986;1(1):39-45.
23. Ericsson I, Lekholm U, Brånemark PI, et al. A clinical evaluation of fixed bridge restorations supported by the combination of teeth and osseointegrated titanium implants. J Clin Periodontol. 1986;13(4):307-312.
24. Kirsch A, Mentag PJ. The MZ endosseous two phase implant system: 4 complete oral rehabilitation treatment concept. J Oral Implant. 1986;12:576-589.
25. Kay H. Free standing vs. implant-tooth-interconnected res torations: understanding the prosthodontic perspective. Int J Periodont Rest Dent. 1993;13:47-68.
26. Lill W, Matejka M, Rambousek K, et al. The ability of currently available stress-breaking elements for osseointegrated im plants to imitate natural tooth mobility. Int J Oral Maxillofac Implants. 1988;3(4):281-286.
27. Richter EJ. Basic biomechanics of dental implants in prosthetic dentistry. J Prosthet Dent. 1989;61(5):602-609.
28. Becker CM, Kaiser DA, Jones JD. Guidelines for splinting im plants. J Prosthet Dent. 2000;84(2):210-214.
29. Reider CE, Parel SM. A survey of natural tooth abutment in trusion with implant-connected fixed partial dentures. Int J Peri odontics Restorative Dent. 1993;12(4):335-347.
30. English CE. Root intrusion in tooth-implant combination cases. Implant Dent. 1993;2(2): 79-85.
31. Cordaro L, Ercoli C, Rossini C, et al. Retrospective evaluation of complete-arch fixed partial dentures connecting teeth and implant abutments in patients with normal and reduced periodontal support. J Prosthet Dent. 2005;94(4)313-320.
32. Garcia LT, Oesterle LJ. Natural tooth intrusion phenomenon with implants: a survey. Int J Oral Maxillofac Implants. 1998;13(2):227-231.
33. Cho GC, Chee WW. Apparent intrusion of natural teeth under an implant-supported prosthesis: a clinical report. J Prosthet Dent. 1992;68(1): 3-5.
34. Lindh T, Dahlgren S, Gunnarsson K, et al. Tooth-implant sup ported fixed prostheses: a retrospective multicenter study. Int J Prosthodont. 2001;14(4): 321-328.
35. Block MS, Lirette D, Gardiner D, et al. Prospective evaluation of implants connected to teeth. Int J Oral Maxillofac Implants. 2002;17(4):473-487.
36. Kindberg H, Gunne J, Kronström M. Tooth- and implant-sup ported prostheses: a retrospective clinical follow-up up to 8 years. Int J Prosthodont. 2001;14(6): 575-581.
37. Fugazzotto PA, Kirsch A, Ackermann KL, et al. Implant/tooth-connected restorations utilizing screw-fixed attachments: a sur vey of 3,096 sites in function for 3 to 14 years. Int J Oral Maxillofac Implants. 1999;14(6):819-823.
38. Hosny M, Duyck J, van Steenberghe D, et al. Within-subject comparison between connected and nonconnected tooth-to-implant fixed partial prostheses: up to 14-year follow-up study. Int J Prosthodont. 2000;13(4):340-346.
39. Palmer RM, Howe LC, Palmer PJ. A prospective 3-year study of fixed bridges linking Astra Tech ST implants to natural teeth. Clin Oral Implants Res. 2005;16(3): 302-307.
40. Pesun IJ. Intrusion of teeth in the combination implant-to-natural-tooth fixed partial denture: a review of the theories. J Prosthodont. 1997;6(4):268-277.
41. Sheets CG, Earthman JC. Natural tooth intrusion and reversal in implant-assisted prosthesis: evidence of and a hypothesis for the occurrence. J Prosthet Dent. 1993;70(6):513-520.
42. Sheets CG, Earthman JC. Tooth intrusion in implant-assisted prosthesis. J Prosthet Dent. 1997;77(1):39-45.
43. Schlumberger TL, Bowley JF, Maze GI. Intrusion phenomenon in combination tooth-implant restorations: a review of the literature. J Prosthet Dent. 1998;80(2): 199-203.
44. Ericsson I, Lekholm U, Brånemark PI, et al. A clinical evaluation of fixed-bridge restorations supported by the combination of teeth and osseointegrated titanium implants. J Clin Periodontol. 1986;13(4):307-312.
45. Gross M, Laufer BZ. Splinting osseointegrated implants and natural teeth in rehabilitation of partially edentulous patients. Part I: laboratory and clinical studies. J Oral Rehabil. 1997;24(11): 863-870.
46. Olsson M, Gunne J, Astrand P, et al. Bridges supported by free-standing implants versus bridges supported by tooth and im plants. A five-year prospective study. Clin Oral Implants Res. 1995;6(2):114-121.
47. Lindh T, Bäck T, Nyström E, et al. Implant versus tooth-implant supported prostheses in the posterior maxilla: a 2-year report. Clin Oral Implants Res. 2001;12(5): 441-449.
48. Nickenig HJ, Schäfer C, Spiekermann H. Survival and complication rates of combined tooth-implant-supported fixed partial dentures. Clin Oral Implants Res. 2006;17(5):506-511.
49. Gunne J, Astrand P, Lindh T, et al. Tooth-implant and implant supported fixed partial dentures: a 10-year report. Int J Pros tho dont. 1999;12(3):216-221.
50. Quirynen M, Naert I, van Steenberghe D, et al. Periodontal as pects of osseointegrated fixtures supporting a partial bridge. An up to 6-years retrospective study. J Clin Periodontol. 1992;19(2): 118-126.
51. Tangerud T, Grønningsaeter AG, Taylor A. Fixed partial dentures supported by natural teeth and Brånemark system im plants: a 3-year report. Int J Oral Maxillofac Implants. 2002;17(2):212-219.
52. Clarke DF, Chen ST, Dickinson AJ. The use of a dental im plant as an abutment in three unit implant-tooth supported fixed partial denture: a case report and 32 month follow-up. Aust Dent J. 2006;51(3): 263-267.
53. Brägger U, Karoussis I, Persson R, et al. Technical and biological complications/failures with single crowns and fixed partial dentures on implants: a 10-year prospective cohort study. Clin Oral Implants Res. 2005;16(3): 326-334.
54. Akça K, Uysal S, Cehreli MC. Implant-tooth-supported fixed partial prostheses: correlations between in vivo occlusal bite forces and marginal bone reactions. Clin Oral Implants Res. 2006;17(3): 331-336.
55. Fartash B, Arvidson K. Long-term evaluation of single crystal sapphire implants as abutments in fixed prosthodontics. Clin Oral Implants Res. 1997;8(1): 58-67.
56. Jemt T, Lekholm U. Oral implant treatment in posterior partially edentulous jaws: a 5-year follow-up report. Int J Oral Maxillofac Implants. 1993;8(6): 635-640.
57. Koth DL, McKinney RV, Steflik DE, et al. Clinical and statistical analyses of human clinical trials with the single crystal aluminum oxide endosteal dental implant: five-year results. J Prosthet Dent. 1988;60(2): 226-234.
58. Kronström M, Trulsson M, Söderfeldt B. Patient evaluation of treatment with fixed prostheses supported by implants or a combination of teeth and implants. J Prosthodont. 2004;13(3): 160-165.
59. Pylant T, Triplett RG, Key MC, et al. A retrospective evaluation of endosseous titanium implants in the partially edentulous patient. Int J Oral Maxillofac Implants. 1992;7(2):195-202.
60. Romeo E, Lops D, Margutti E, et al. Long-term survival and success of oral implants in the treatment of full and partial arches: a 7-year prospective study with the ITI dental implant system. Int J Oral Maxillofac Implants. 2004;19(2): 247-259.
61. Steflik DE, Koth DL, Robinson FG, et al. Prospective investigation of the single-crystal sapphire endosteal dental im plant in humans: ten-year results. J Oral Implantol. 1995;21(1):8-18.
62. van Steenberghe D. A retrospective multicenter evaluation of the survival rate of osseointegrated fixtures supporting fixed partial prostheses in the treatment of partial edentulism. J Pros thet Dent. 1989;61(2):217-223.
63. Astrand P, Borg K, Gunne J, et al. Combination of natural teeth and osseointegrated implants as prosthesis abutments: a 2-year longitudinal study. Int J Oral Maxillofac Implants. 1991;6(3): 305-312.
64. Tan K, Pjetursson BE, Lang NP, et al. A systematic review of the survival and complication rates of fixed partial dentures (FPDs) after an observation period of at least 5 years. Clin Oral Implants Res. 2004;15(6): 654-666.
65. Pjetursson BE, Tan K, Lang NP, et al. A systematic review of the survival and complication rates of fixed partial dentures (FPDs) after an observation period of at least 5 years. Clin Oral Implants Res. 2004;15(6):667-676.
66. Mau J, Behneke A, Behneke N, et al. Randomized multicenter comparison of two coatings of intramobile cylinder implants in 313 partially edentulous mandibles followed up for 5 years. Clin Oral Implants Res. 2002;13(5): 477-487.
67. Jemt T, Lekholm U, Adell R. Osseointegrated implants in the treatment of partially edentulous patients: a preliminary study on 876 consecutively placed fixtures. Int J Oral Maxillofac Im plants. 1989;4(3): 211-217.
68. Isidor F. Influence of forces on peri-implant bone. Clin Oral Implants Res. 2006;17(suppl 2): 8-18.
69. Isidor F. Loss of osseointegration caused by occlusal load of oral implants. A clinical and radiographic study in monkeys. Clin Oral Implants Res. 1996;7(2): 143-152.
70. Miyata T, Kobayashi Y, Araki H, et al. The influence of controlled occlusal overload on peri-implant tissue. Part 3: a histologic study in monkeys. Int J Oral Maxillofac Implants. 2002;15(3):425-431.
71. Esposito M, Hirsch JM, Lekholm U, et al. Biological factors contributing to failures of osseointegrated oral implants. (I). Success criteria and epidemiology. Eur J Oral Sci. 1998;106(1):527-551.
72. Esposito M, Hirsch JM, Lekholm U, et al. Biological factors contributing to failures of osseointegrated oral implants. (II). Etiopathogenesis. Eur J Oral Sci. 1998;106(3):721-764.
73. Engel E, Gomez-Roman G, Axmann-Krcmar D. Effect of oc clusal wear on bone loss and Periotest value of dental implants. Int J Prosthodont. 2001;14(5): 444-450.
74. Wennerberg A, Carlsson GE, Jemt T. Influence of occlusal factors on treatment outcome: a study of 109 consecutive pa tients with mandibular implant-supported fixed prostheses opposing maxillary complete dentures. Int J Prosthodont. 2001;14(6):550-555.
75. Lindquist LW, Carlsson GE, Jemt T. A prospective 15-year follow-up study of mandibular fixed prostheses supported by os seointegrated implants. Clinical results and marginal bone loss. Clin Oral Implants Res. 1996;7(4): 329-336.
76. Lindquist LW, Carlsson GE, Jemt T. Association between mar ginal bone loss around osseointegrated mandibular implants and smoking habits: a 10-year follow-up study. J Dent Res. 1997;76(10):1667-1674.
77. Vidyasagar L, Apse P. Biological response to dental implant loading/overloading. Implant overloading: empiricism or science? Stomatologija. 2003;5: 83-89.
78. Albrektsson T, Zarb G, Worthington P, et al. The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants. 1986;1(1):11-25.
79. Sorensen JA, Martinoff JT. Clinically significant factors in dowel design. J Prosthet Dent. 1984;52(1): 28-35.
80. Akagawa Y, Hosokawa R, Sato Y, Kamayama K. Comparison between freestanding and tooth-connected partially stabilized zirconia implants after two years’ function in monkeys: a clinical and histological study. J Prosthetic Dent. 1998;80:551-558.
81. Pesun IJ, Steflik DE, Parr GR, et al. Histologic evaluation of the periodontium of abutment teeth in combination implant/tooth fixed partial denture. Int J Oral Maxillofac Implants. 1999;14(3):342-350.
82. Biancu S, Ericsson I, Lindhe J. The periodontal ligament of teeth connected to osseointegrated implants. An experimental study in the beagle dog. J Clin Periodontol. 1995(5);22:362-370.
83. O’Leary TJ, Dykema RW, Kafrawy AH. Splinting osseointegrated fixtures to teeth with normal periodontium. In: Laney WR, Tolman DE, eds. Tissue Integration in Oral, Orthopedic and Maxillofacial Reconstruction. Hanover Park, IL: Quintessence Publishing Co. Inc.; 1990;48-57.
About the Authors
Gary Greenstein, DDS, MS
Associate Professor
Department of Periodontology and Implant Dentistry
New York University College of Dentistry
New York, New York
Private Practice
Freehold, New Jersey
John Cavallaro, DDS
Associate Professor
Department of Periodontology and Implant Dentistry
New York University College of Dentistry
New York, New York
Private Practice
Brooklyn, New York
Richard Smith, DDS
Associate Professor
Department of Periodontology and Implant Dentistry
New York University College of Dentistry
New York, New York
Private Practice
New York, New York
Dennis Tarnow, DDS
Professor
Department of Periodontology and Implant Dentistry
New York University College of Dentistry
New York, New York
Private Practice
New York, New York