A High-Tech Approach to Managing Periodontal Disease: Case Reports
John McAllister, DDS
Some 5% to 20% of any population has severe, generalized periodontitis, although mild-to-moderate periodontitis affects most adults.1 Statistics indicate that only 3% of those given a diagnosis of these diseases are being treated annually. The Laser Assisted New Attachment Procedure™ (LANAP™, Millennium Dental Technologies, Inc, Cerritos, CA) has been shown to be a clinically effective method in treating early, moderate-to-severe periodontal disease.2-5 LANAP is a laser-based procedure developed by Robert H. Gregg, II, DDS, and Delwin McCarthy, DDS, of Millennium Dental Technologies, Inc.6 This article presents cases that demonstrate how LANAP can provide clinical outcomes superior to invasive surgical procedures.
The indications for LANAP are the same as for standard periodontal therapies and include probing depths ≥ 4 mm with hemorrhage following probing, infection in the surrounding gingival tissue (erythema and edema), visible tooth mobility, radiographic evidence of bone loss, and positive laboratory tests for periodontal pathogens. Patients who decline to cooperate seem to be the only contraindication to performing LANAP.
An 8-year retrospective study of LANAP2 demonstrated consistent mean pocket depth reduction (40%) and improved bone density (38%). The study measured bone density changes with Emago® diagnostic software (Oral Diagnostic Systems, The Netherlands) and found 100% of cases showed a density increase. LANAP also was shown to be effective in reducing pocket depth without gingival recession over a 6-month period.
In the most recent peer-reviewed human histologic study comparing LANAP using the PerioLase® MVP-7 (Millennium Dental Technologies, Inc) with scaling and root planing (SRP) without using a laser, 12 teeth were removed in bloc and studied histologically. Results demonstrated 100% frequency of cementum-mediated new attachment to the root surface in the absence of long junctional epithelium in the LANAP group. In the SRP group, 0% had this finding, though 100% of the SRP subjects had long junctional epithelium.3
The cases presented show the LANAP protocol using the PerioLase MVP-7 (Figure 1), which can provide predictable results.
Case 1
An 85-year-old woman presented with a report by a periodontist who previously had evaluated her. The report noted that tooth No. 31 had a severe bony defect affecting the mesial aspect and a furcation. The tooth had a questionable short-term prognosis. The patient’s chief concern was a desire to avoid additional extractions and periodontal surgery. The patient’s medical history was unremarkable.
Oral hygiene was fair; dental radiographs revealed moderate-to-severe horizontal and vertical bony defects throughout the dentition. Periodontal charting around 28 teeth (168 sites) demonstrated generalized moderate-to-deep pockets up to 11 mm. Forty-nine sites probed ≤ 3 mm (30% normal) and nine sites probed ≥ 8 mm. An 11-mm defect was located on the mesial-lingual aspect of tooth No. 31 (Figure 2). A diagnosis of generalized moderate-to-advanced periodontitis was confirmed, and LANAP was scheduled for the patient.
The upper and lower left quadrants were treated first. The PerioLase LANAP protocol was followed. Troughing around each tooth was done at 150 milliseconds, 20 Hz, 3 Watts. Hemostasis was accomplished with 650 milliseconds, 20 Hz, 3 Watts; total joules used were 2139. The patient had the right quadrants treated the following week with a total of 2905 J. The patient tolerated the procedure well, with no complications or adverse effects. She was asked the following week to rate the experience on a scale of 1 to 10, with 10 being the worst pain she had ever had. She rated her pain as 0 (no pain).
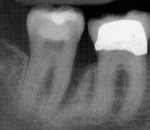
A comparison of the pre- and 3-month posttreatment radiographs of the bone surrounding tooth No. 31 showed strong evidence of bone fill mesially (Figure 3). The probing depths 23-months posttreatment (Figure 4) demonstrated the effectiveness of the procedure. Her bleeding score was reduced from 55.3% to 11%, a 44% improvement.
Case 2
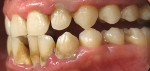
A 58-year-old woman presented with a treatment plan for periodontal osseous surgery and removal of her lower front teeth. The patient had an uneventful medical history. Dental examination and history revealed that the patient never had any restorative dentistry. Full-mouth radiographs demonstrated generalized vertical bony defects limited to the anterior segment. Periodontal charting indicated probing depths of 9 mm on 11 sites, with depth at 32 sites between 5 mm and 8 mm. Only 50 sites probed normally (3 mm); total: 28 teeth, 168 probing sites. The diagnosis of type IV or advanced periodontal disease and primary occlusal trauma was recorded (Figure 5). Upper left and lower left quadrants were treated with LANAP. Right quadrants were treated 8 days later.
Troughing around the tooth was performed with a PerioLase MVP-7 using a “short pulse,” which has a duration of 150 milliseconds. Pulse energy was set to 100 mJ and repetition rate was 20 Hz, giving an average power of 3.8 W. The parameters for hemostasis or “long pulse” used to finish the procedure were 550-millisecond duration, 180 mJ, 20 Hz, also providing an average power of 3.8 W.
An advantage of this laser system is the readout of total energy delivered during the procedure. This value is essential in determining the “light dose.” To compute the light dose, the total energy delivered is divided by the sum of the depths of all pockets, which, in this case, was 15.2 J/mm pocket depth.
The condition of the periodontal tissues 1-week posttreatment was unremarkable in the appearance of healing. No evidence of further recession was noted. The patient reported a 2 on the previously described 1-to-10 pain scale.
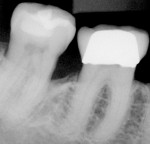
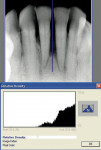
The patient dutifully attended periodontal maintenance appointments at consistent 3-month intervals. A comparison of the pretreatment and 3-month posttreatment radiographs of the bone surrounding teeth Nos. 24 and 25 shows strong evidence of increased bone density (Figure 6). The density profiles clearly demonstrate this increase (Figure 7 and Figure 8).
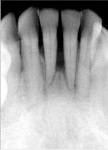
A follow-up examination was performed at 14-months posttreatment. Slight staining, light calculus, and healthy-appearing gingiva were noted. The probing depths recorded at this examination provided a quantitative index of the efficacy of LANAP (Figure 9). The 11 deep pockets (≥ 9 mm) that represented an advanced stage of periodontitis responded favorably to therapy. These pockets were reduced by an average of 6 mm from a median probing depth of 9 mm pretreatment to a median probing depth of 3 mm at 14 months posttreatment. With all pockets ≥ 4 mm, 112 sites before treatment, only three sites had a 4-mm pocket after treatment. All other sites were ≤ 3 mm. Bleeding was 77% before LANAP and 4% after LANAP, a 73% improvement.
Case 3
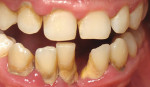
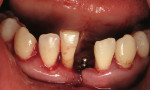
A 39-year-old man presented for full-mouth radiographic examination and a second-opinion consultation on treatment planning. His primary concern was the scheduled removal of the lower anterior teeth (Nos. 23, 25, and 26) for the following week. The patient’s previous dentist had informed him that the teeth were hopelessly pathologic and could not be saved. The patient’s medical history revealed nothing remarkable. His dental history showed no previous dental treatment and a missing tooth No. 24 (Figure 10 and Figure 11). Full-mouth radiographs demonstrated generalized vertical bony defects throughout his mouth.
The radiograph of teeth Nos. 23, 25, and 26 indicated deep vertical and three-wall defects. Clinical examination revealed his teeth to have a class III mobility (apically mobile). The patient reported that palpation of any area around the teeth was tender-to-very painful.
One week later periodontal charting following local anesthesia demonstrated bony defects and periodontal pockets up to 12 mm. The probing depths of 186 sites around 31 teeth showed a median probing depth of 6.4 mm. Of greatest concern were 44 pockets ≥ 8 mm.
The PerioLase MVP-7 was used on the “short pulse” for troughing for 150 milliseconds and the “long pulse” for finishing for 550 milliseconds. The “light dose” was 16.3 J/mm-pocket depth. Frenectomy and placement of an Imtec MDI® Sendax implant (IMTEC®, Ardmore, OK) was splinted to the mobile lower anteriors during the surgical procedure (Figure 12, Figure 13, Figure 14, Figure 15).
Discussion
These three cases demonstrate and support the efficacy of LANAP using the PerioLase MVP-7. The results are consistent with past case studies and university research using the pulsed Nd:YAG laser as a legitimate and effective modality for the treatment of moderate-to-severe adult periodontitis in a general dental practice.2,3,7-9 These cases also are consistent with the studies previously reported using the LANAP procedure.2,6 All three cases show dramatic radiographic bone regeneration following LANAP.
These cases appear consistent with histological results of new cementum-mediated attachment to the root surface in the absence of long junctional epithelium as proof of principle.3 In the cases treated in the author’s office, consistent clinical results have been obtained using the LANAP protocol and the PerioLase MVP-7. As of this writing, the three cases presented continue to exhibit stable and healthy periodontum at routine maintenance visits.
Conclusion
As a clinician, it is rewarding to be able to offer a service that reverses the primary cause of tooth loss with little-to-no posttreatment discomfort. In the author’s opinion, LANAP appears to provide a minimally invasive alternative that may be preferable to traditional periodontal surgical techniques and provides excellent, predictable results with significant new attachment, cementum, and bone regeneration. Regeneration of lost periodontal tissues is being reported consistently among PerioLase users. Today more than 600 dentists have adopted the protocol; this represents less than 1% of US dentists who provide this service, even though US Food and Drug Administration clearance occurred more than 4 years ago, noting the “new cementum mediated attachment to the root surface in the absence of long junctional epithelium.”
General dentists should consider using this modality for their patients who require surgical intervention of their periodontal disease. This is because it is minimally invasive, provides predictable results, causes minor postoperative pain, and increases treatment acceptance compared with conventional periodontal surgery.
References
1. Burt B; Research, Science and Therapy Committee of the American Academy of Periodontology. Position paper: epidemiology of periodontal diseases. J Periodontol. 2005;76(8): 1406-1419.
2. Harris DM, Gregg RH 2nd, McCarthy DK, et al. Laser assisted new attachment procedure in private practice. Gen Dent. 2004;52(5): 396-403.
3. Yukna RA, Carr RL, Evans GH. Histologic evaluation of an Nd:YAG laser-assisted new attachment procedure in humans. Int J Periodontics Restorative Dent. 2007;27(6):577-587.
4. Gunsolly JC, Elswick RK, Davenport JM. Equivalence and superiority testing in regeneration clinical trials. J Periodontol. 1998;69(5):521-527.
5. White JM, Goodis HE, Rose CL. Use of pulsed ND:YAG laser for intraoral soft tissue surgery. Lasers Surg Med. 1991;11(5): 455-461.
6. Summary for safety and effectiveness information Periolase dental laser system (501[K] No. K030290). US Food and Drug Administration Center for Devices and Radiological Health Web site. https://www.fda.gov/cdrh/pdf3/k030290.pdf. Accessed May 20, 2008.
7. Gregg RH, McCarthy DK. Laser ENAP for periodontal bone regeneration. Dent Today. 1998;17(5): 88-91.
8. Long CA. New attachment procedure using the pulsed Nd:YAG. Dent Today. 2008;27(2): 166-171.
9. Piñero J. Nd:YAG-assisted periodontal curettage to prevent bacteremia before cardiovascular surgery. Dent Today. 1998;17(3):84-87.
About the Author
John McAllister, DDS
Private Practice
Downey, California
Clinical Instructor
Institute for Advanced Laser Dentistry
Cerritos, California